Search
- Page Path
- HOME > Search
Original Articles
- Clinical Study
- A Phase II Multi-Center, Non-Randomized, Parallel Group, Non-Inferiority Study to Compare the Efficacy of No Radioactive Iodine Remnant Ablation to Remnant Ablation Treatment in Low- to Intermediate-Risk of Papillary Thyroid Cancer: The MOREthyroid Trial Protocol
- Eun Kyung Lee, You Jin Lee, Young Joo Park, Jae Hoon Moon, Ka Hee Yi, Koon Soon Kim, Joo Hee Lee, Sun Wook Cho, Jungnam Joo, Yul Hwangbo, Sujeong Go, Do Joon Park
- Endocrinol Metab. 2020;35(3):571-577. Published online September 22, 2020
- DOI: https://doi.org/10.3803/EnM.2020.681
- 4,642 View
- 119 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Radioactive iodine (RAI) remnant ablation is recommended in patients with papillary thyroid cancer (PTC) and extrathyroidal extension or central lymph node metastasis. However, there exists little evidence about the necessity of remnant ablation in PTC patients with low- to intermediate-risk, those have been increasing in recent decades.
Methods
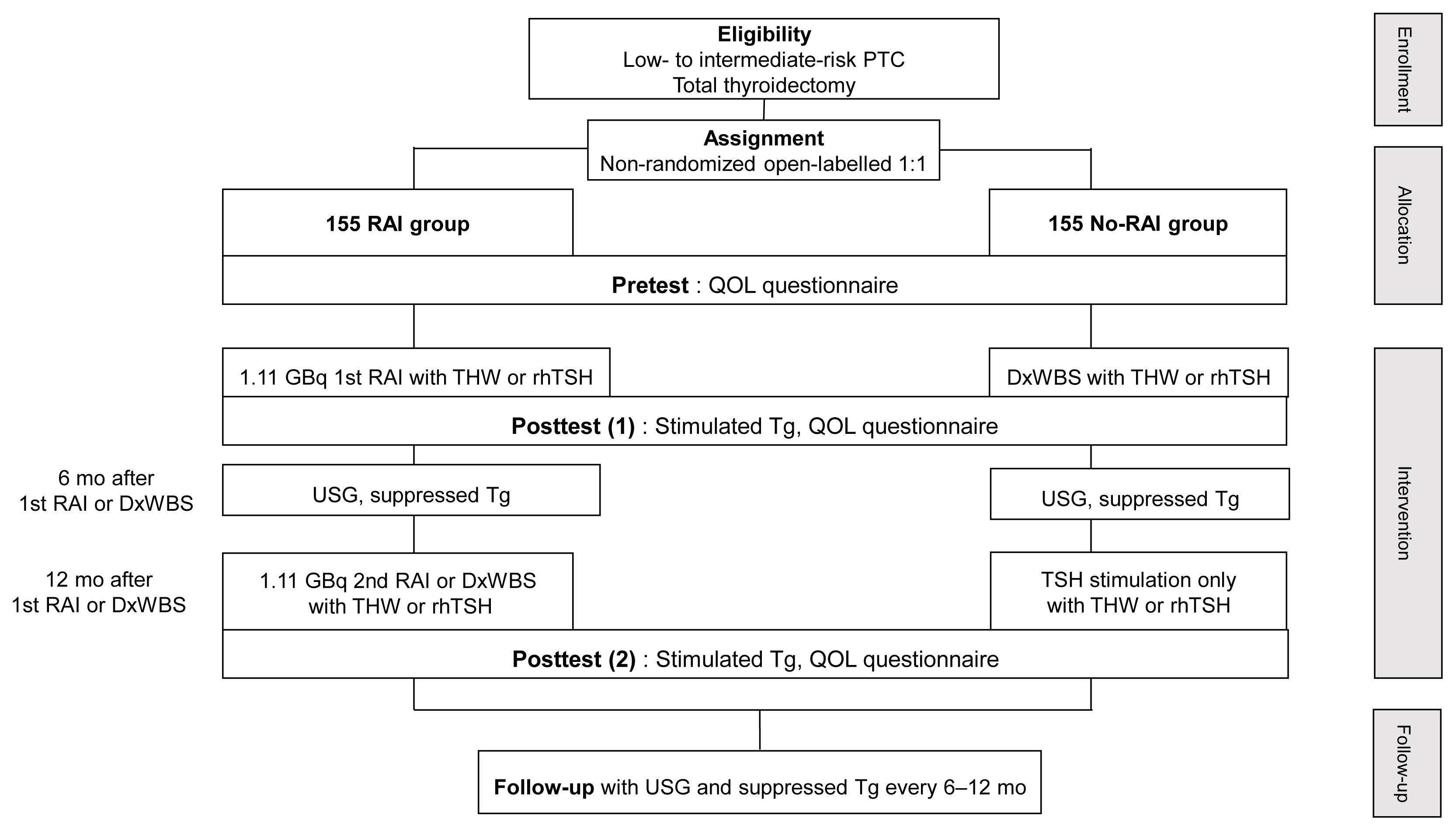
This multicenter, prospective, non-randomized, parallel group clinical trial will enroll 310 eligible patients with low- to intermediate-risk of thyroid cancer. Inclusion criteria are patients who recently underwent total thyroidectomy for PTC with 3 or less tumors of size 1≤ to ≤2 cm with no microscopic extension and N0/x, or size ≤2 cm with microscopic extension and/or N1a (number of lymph node ≤3, size of tumor foci ≤0.2 cm, and lymph node ratio <0.4). Patients choose to undergo RAI ablation (131I, dose 1.1 GBq) or diagnostic whole-body scan (DxWBS) (131I or 123I, dose 0.074 to 0.222 GBq), followed by subsequent measurement of stimulated thyroglobulin (sTg) within 1 year. Survey for quality of life (QOL) will be performed at baseline and at 1 year after follow-up. The total enrollment period is 5 years, and patients will be followed up for 1 year. The primary endpoint is the non-inferiority of surgery alone to surgery with ablation in terms of biochemical remission (BCR) rate (sTg ≤2 ng/mL) without evidence of structural recurrence. The secondary endpoint was the difference of QOL.
Conclusion
This study will evaluate whether surgery alone achieves similar BCR and improved QOL compared to RAI ablation in patients with low- to intermediate-risk PTC within 1 year.

- Clinical Study
- Apolipoprotein B Levels Predict Future Development of Hypertension Independent of Visceral Adiposity and Insulin Sensitivity
- Seung Jin Han, Wilfred Y. Fujimoto, Steven E. Kahn, Donna L. Leonetti, Edward J. Boyko
- Endocrinol Metab. 2020;35(2):351-358. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.351
- 5,813 View
- 130 Download
- 7 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
High plasma apolipoprotein B (apoB) levels have been shown to be associated with hypertension, central obesity, and insulin resistance in cross-sectional research. However, it is unclear whether apoB levels predict future hypertension independent of body composition and insulin sensitivity. Therefore, we prospectively investigated whether plasma apoB concentrations independently predicted the risk of hypertension in a cohort of Japanese Americans.
Methods
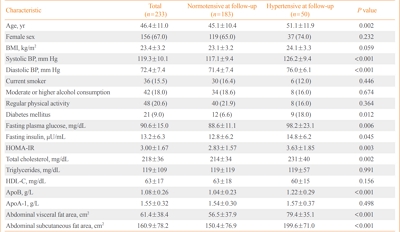
A total of 233 normotensive Japanese Americans (77 men, 156 women; mean age, 46.4±11.0 years) were followed over 10 years to monitor them for the development of hypertension. Fasting plasma concentrations of apoB, glucose, and insulin were measured at baseline. Insulin sensitivity was estimated using the homeostasis model assessment of insulin resistance (HOMA-IR). The abdominal visceral and subcutaneous fat areas were measured at baseline using computed tomography. Logistic regression analysis was used to estimate the association between apoB concentrations and the odds of incident hypertension.
Results
The 10-year cumulative incidence of hypertension was 21.5%. The baseline apoB level was found to be positively associated with the odds of incident hypertension over 10 years after adjustment for age, sex, body mass index, systolic blood pressure, abdominal visceral fat area, abdominal subcutaneous fat area, total plasma cholesterol concentration, diabetes status, and HOMA-IR at baseline (odds ratio and 95% confidence interval for a 1-standard deviation increase, 1.89 [1.06 to 3.37]; P=0.030).
Conclusion
Higher apoB concentrations predicted greater risks of future hypertension independent of abdominal visceral fat area and insulin sensitivity in Japanese Americans. -
Citations
Citations to this article as recorded by- Correlation between Central Obesity and Liver Function in Young Adults—A Cross-Sectional Study
John Alvin, Damodara Gowda KM
Journal of Health and Allied Sciences NU.2023; 13(02): 273. CrossRef - Serum amyloid A in children and adolescents: association with overweight and carotid intima-media thickness
Maria Vitória Mareschi Barbosa, João Carlos Pina Faria, Stephanie Ramos Coelho, Fernando Luiz Affonso Fonseca, Andrea Paula Kafejian Haddad, Fabíola Isabel Suano de Souza, Roseli Oselka Saccardo Sarni
einstein (São Paulo).2023;[Epub] CrossRef - The association of the apolipoprotein B/A1 ratio and the metabolic syndrome in children and adolescents: a systematic review and meta-analysis
Kayhan Dinpanah, Toba Kazemi, Sameep Shetty, Saeede Khosravi Bizhaem, Ali Fanoodi, Seyed Mohammad Riahi
Journal of Diabetes & Metabolic Disorders.2023;[Epub] CrossRef - Current Data and New Insights into the Genetic Factors of Atherogenic Dyslipidemia Associated with Metabolic Syndrome
Lăcramioara Ionela Butnariu, Eusebiu Vlad Gorduza, Elena Țarcă, Monica-Cristina Pânzaru, Setalia Popa, Simona Stoleriu, Vasile Valeriu Lupu, Ancuta Lupu, Elena Cojocaru, Laura Mihaela Trandafir, Ștefana Maria Moisă, Andreea Florea, Laura Stătescu, Minerva
Diagnostics.2023; 13(14): 2348. CrossRef - Sex-Based Differences and Risk Factors for Comorbid Nonalcoholic Fatty Liver Disease in Patients with Bipolar Disorder: A Cross-Sectional Retrospective Study
Ying Wang, Yiyi Liu, Xun Zhang, Qing Wu
Diabetes, Metabolic Syndrome and Obesity.2023; Volume 16: 3533. CrossRef - Apolipoprotein B Displays Superior Predictive Value Than Other Lipids for Long-Term Prognosis in Coronary Atherosclerosis Patients and Particular Subpopulations: A Retrospective Study
Chunyan Zhang, Jingwei Ni, Zhenyue Chen
Clinical Therapeutics.2022; 44(8): 1071. CrossRef - Genetics of Cholesterol-Related Genes in Metabolic Syndrome: A Review of Current Evidence
Sok Kuan Wong, Fitri Fareez Ramli, Adli Ali, Nurul ‘Izzah Ibrahim
Biomedicines.2022; 10(12): 3239. CrossRef
- Correlation between Central Obesity and Liver Function in Young Adults—A Cross-Sectional Study


 KES
KES

 First
First Prev
Prev



