Articles
- Page Path
- HOME > Endocrinol Metab > Volume 37(2); 2022 > Article
-
Original ArticleAdrenal Gland Outcome-Based Decision-Making Algorithm for Treating Patients with Primary Aldosteronism
-
Jung Hee Kim1
 , Chang Ho Ahn2, Su Jin Kim3, Kyu Eun Lee3, Jong Woo Kim4, Hyun-Ki Yoon5, Yu-Mi Lee6, Tae-Yon Sung6, Sang Wan Kim7, Chan Soo Shin1, Jung-Min Koh8, Seung Hun Lee8
, Chang Ho Ahn2, Su Jin Kim3, Kyu Eun Lee3, Jong Woo Kim4, Hyun-Ki Yoon5, Yu-Mi Lee6, Tae-Yon Sung6, Sang Wan Kim7, Chan Soo Shin1, Jung-Min Koh8, Seung Hun Lee8
-
Endocrinology and Metabolism 2022;37(2):369-382.
DOI: https://doi.org/10.3803/EnM.2022.1391
Published online: April 14, 2022
1Department of Internal Medicine, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Korea
2Department of Internal Medicine, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Korea
3Department of Surgery, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Korea
4Department of Radiology, Chung-Ang University Health Care System Hyundae Hospital, Namyangju, Korea
5Department of Radiology and Research Institute of Radiology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
6Department of Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
7Department of Internal Medicine, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul National University College of Medicine, Seoul, Korea
8Division of Endocrinology and Metabolism, Department of Medicine, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- Corresponding author: Seung Hun Lee. Division of Endocrinology and Metabolism, Department of Medicine, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul 05505, Korea Tel: +82-2-3010-5666, Fax: +82-2-3010-6962, E-mail: hun0108@amc.seoul.kr
Copyright © 2022 Korean Endocrine Society
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Background
- Optimal management of primary aldosteronism (PA) is crucial due to the increased risk of cardiovascular and cerebrovascular diseases. Adrenal venous sampling (AVS) is the gold standard method for determining subtype but is technically challenging and invasive. Some PA patients do not benefit clinically from surgery. We sought to develop an algorithm to improve decision-making before engaging in AVS and surgery in clinical practice.
-
Methods
- We conducted the ongoing Korean Primary Aldosteronism Study at two tertiary centers. Study A involved PA patients with successful catheterization and a unilateral nodule on computed tomography and aimed to predict unilateral aldosterone-producing adenoma (n=367). Study B involved similar patients who underwent adrenalectomy and aimed to predict postoperative outcome (n=330). In study A, we implemented important feature selection using the least absolute shrinkage and selection operator regression.
-
Results
- We developed a unilateral PA prediction model using logistic regression analysis: lowest serum potassium level ≤3.4 mEq/L, aldosterone-to-renin ratio ≥150, plasma aldosterone concentration ≥30 ng/mL, and body mass index <25 kg/m2 (area under the curve, 0.819; 95% confidence interval, 0.774 to 0.865; sensitivity, 97.6%; specificity, 25.5%). In study B, we identified female, hypertension duration <5 years, anti-hypertension medication <2.5 daily defined dose, and the absence of coronary artery disease as predictors of clinical success, using stepwise logistic regression models (sensitivity, 94.2%; specificity, 49.3%). We validated our algorithm in the independent validation dataset (n=53).
-
Conclusion
- We propose this new outcome-driven diagnostic algorithm, simultaneously considering unilateral aldosterone excess and clinical surgical benefits in PA patients.
- Primary aldosteronism (PA) is the most common type of endocrine hypertension (HTN), and affects 5% to 10% of hypertensive subjects [1,2]. Subjects with PA have increased cardiovascular and cerebrovascular risks compared with those with essential HTN [3]. Therefore, PA management aims to reduce the cardiovascular disease risk by improving blood pressure (BP) and normalizing potassium levels, thereby lowering mortality.
- However, there are two significant points to consider in this respect. The first is whether adrenal venous sampling (AVS) should be implemented. AVS is the gold standard for subtyping PA but is invasive, technically challenging, and has limited availability [1,4]. Therefore, several researchers have suggested clinical predictors of a unilateral aldosterone excess, such as serum potassium levels, estimated glomerular filtration rate (eGFR), plasma aldosterone concentration (PAC), aldosterone-to-renin ratio (ARR) before/after confirmatory tests, and computed tomography (CT) findings [5-8]. If CT shows normal adrenal glands or bilateral lesions, AVS should be performed in patients who are willing to undergo surgery. However, in cases with a unilateral lesion on CT, AVS may be avoided if the lesion can accurately predict unilateral aldosterone excess. Thus, while previous reports have included CT findings as predictors, we have reconsidered whether AVS needs to be performed when unilateral adrenal nodules were already observed on CT.
- Second, it needs to be considered whether surgery improves a clinical outcome in all patients with unilateral aldosterone excess. Although surgery is the mainstay treatment in patients with unilateral aldosterone excess, complete clinical success in terms of clinical outcome occurs only in 37% of patients with unilateral aldosterone excess [9]. Thus, confirmation of unilateral aldosterone excess does not guarantee surgical remission. Zarnegar et al. [10] developed the aldosterone resolution score (ARS), which is based on female sex, shorter HTN duration, lower number of antihypertensive medications, and low body mass index (BMI). The ARS was validated in several studies but was not useful in a French cohort [11-13]. Recently, the Primary Aldosteronism Surgical Outcome (PASO) score was developed by an international group, which additionally includes adrenal nodule size and target organ damage [14]. A Japanese group also suggested using the absence of diabetes mellitus (DM) as another predictor of clinical benefit [15]. However, the definition of surgical outcome was not consistent across studies.
- Hitherto, no algorithm has considered both unilateral aldosterone excess and surgical benefit for deciding on surgery in PA patients. Moreover, a single algorithm is not sufficient to decide on surgical intervention. Herein, we sought to combine predictors of unilateral aldosterone excess with the clinical benefits of surgery in PA patients into an algorithm that can improve decision-making before embarking on invasive procedures and surgery in clinical practice.
INTRODUCTION
- Study population
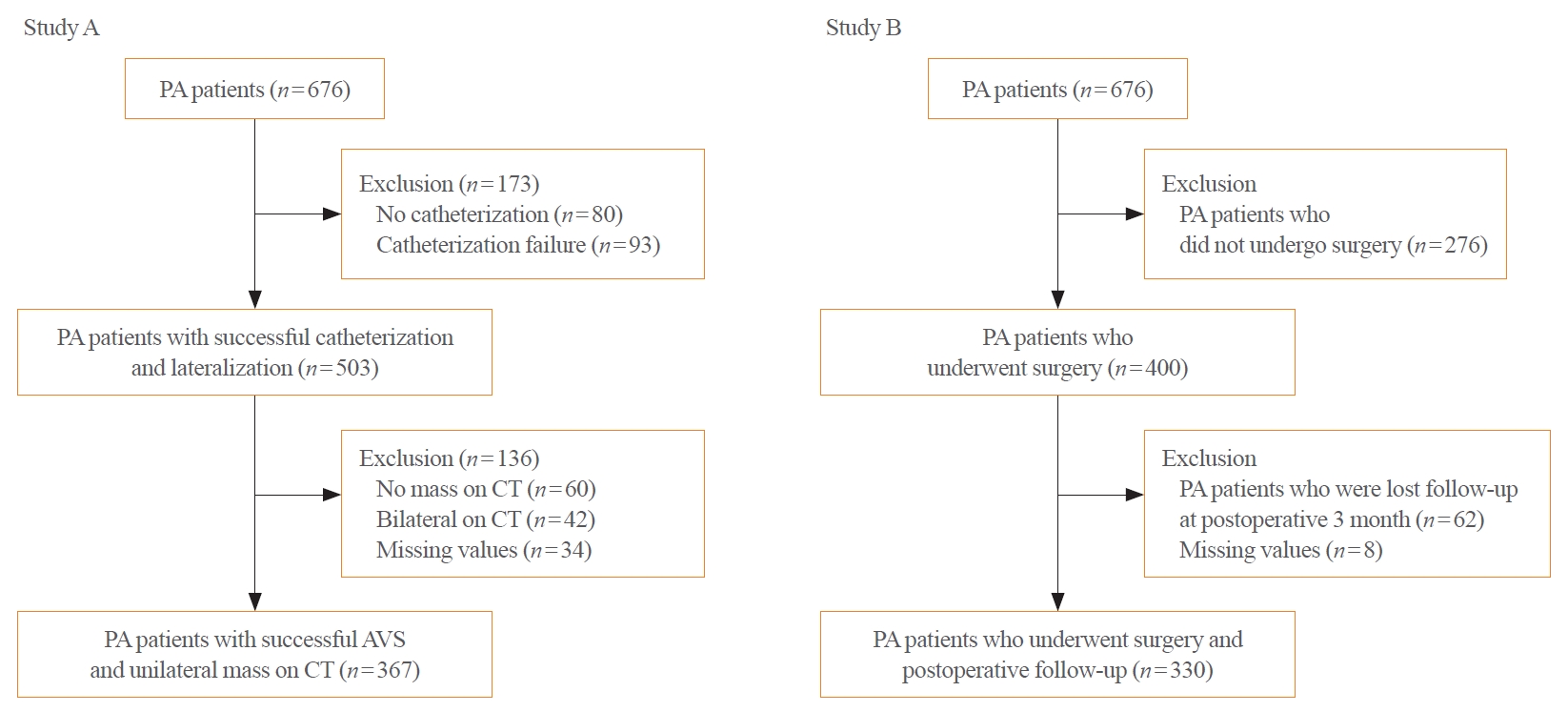
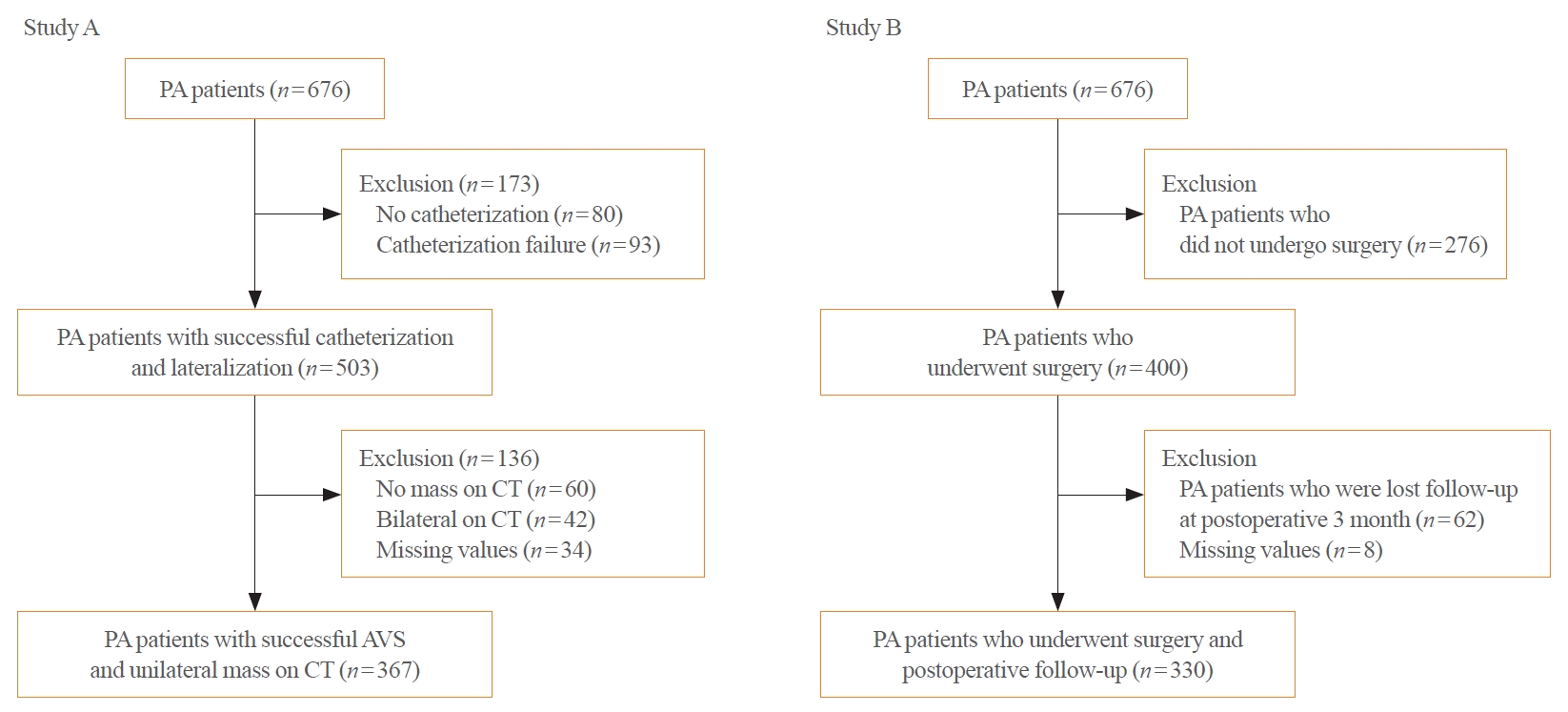
- The Korean Primary Aldosteronism Study is an ongoing cohort study of PA. In this retrospective cohort study, 676 PA patients were enrolled from Seoul National University Hospital from 2000 to 2018 (SNUH, n=363) and Asan Medical Center from 2007 to 2016 (AMC, n=313). Among 676 PA patients from the two centers, Study A was conducted in PA patients with successful catheterization and a unilateral adrenal nodule on CT (n=367) (Fig. 1). The study A cohort was randomly divided into a training dataset (n=257), to develop a lateralization predictive model, and a test dataset (n=110), to validate the model. Patients in Study B were also recruited from the original population of 676 PA patients. Study B was performed in PA patients who underwent adrenalectomy, completed a 3-month postoperative follow-up, and had postoperative clinical outcomes (n=330) (Fig. 1). Among a total of 676 PA patients, 239 patients were included in both Study A and B. The final algorithm was applied to the independent validation dataset derived from Seoul National University Bundang Hospital (n=53). The validation set consisted of PA patients with a unilateral adrenal nodule who underwent adrenalectomy and followed-up after surgery at 3 months from 2010 to 2020 at Seoul National University Bundang Hospital.
- Data collection
- We collected the following data from electronic medical records: age, sex, BMI, BP, family history of HTN, diagnosis and duration of HTN, number of antihypertensive medications, DM, dyslipidemia, coronary artery disease (CAD), atrial fibrillation, cerebrovascular disease (CVD), obstructive sleep apnea (OSA), and hypertensive retinopathy.
- HTN was defined as systolic blood pressure (SBP) ≥140 and/or diastolic blood pressure (DBP) ≥90 mm Hg, or current use of antihypertensive medication. Antihypertensive medications were shown as a defined daily dose (DDD), which is the assumed average maintenance dose per day, according to the World Health Organization anatomical therapeutic chemical (ATC)/DDD index 2019. DM was defined by fasting plasma glucose level ≥7.0 mmol/L (126 mg/dL), glycated hemoglobin ≥6.5%, or current use of oral antidiabetic drugs or insulin. Patients taking lipid-lowering agents or with an abnormal lipid panel (total cholesterol ≥240 mg/dL, low-density lipoprotein cholesterol ≥160 mg/dL, triglyceride ≥200 mg/dL, and high-density lipoprotein cholesterol <40 mg/dL) were considered to have dyslipidemia.
- CAD was defined as a history of percutaneous coronary intervention, coronary artery bypass surgery, or unstable angina noted on their medical records. CVDs were indicated by doctor-diagnosed ischemic or hemorrhage stroke. The presence of atrial fibrillation, OSA, and hypertensive retinopathy was retrieved from the medical records.
- Laboratory measurements
- PAC was measured by radioimmunoassay (RIA) using the SPAC-S Aldosterone kit (TFB Inc., Tokyo, Japan). Plasma renin activity (PRA) was measured by RIA using Renin RIA beads (TFB Inc., at SNUH before 2011) or a PRA RIA kit (TFB Inc., at SNUH after 2011 and at AMC). Intra- and inter-assay coefficients of variation for each assay were 10% and 5%, respectively. PAC and PRA measured at baseline were used as variables. Serum potassium levels, creatinine levels, and eGFR (calculated using the Modification of Diet in Renal Disease equation) were also retrieved from the medical records.
- Diagnosis of PA
- PA was confirmed using a saline infusion test (SIT) in patients with an ARR of ≥20 and a PAC of >15 ng/dL [1]. PAC >10 ng/dL SIT confirmed the diagnosis of PA, whereas PAC after SIT <5 ng/dL excluded the diagnosis PA [1]. The SIT was repeated if PAC of 5 to 10 ng/dL after SIT. We discontinued diuretics and mineralocorticoid receptor antagonists for ≥6 weeks and beta-adrenergic receptor blockers for ≥2 weeks before confirmatory testing. Calcium channel or alpha-adrenergic receptor blockers were preferred for BP control; however, if BP was persistently elevated more than 140/90 mm Hg, angiotensin II receptor blockers or angiotensin-converting enzyme inhibitors were added.
- CT and AVS
- A unilateral adrenal nodule on CT was defined as a nodule measuring ≥7 mm in diameter, and a normal contralateral adrenal gland [16]. Thin-slice (1 to 3-mm-thick) CT was performed for all patients, and findings were evaluated by radiologists. AVS was performed sequentially under adrenocorticotropic hormone stimulation [1,4]. Successful catheterization was defined as a selectivity index (the ratio of cortisol levels in the adrenal vein to those in the inferior vena cava) of ≥3. The lateralization index (LI) was calculated by dividing the aldosterone-to-cortisol ratio of the dominant adrenal vein by that of the non-dominant vein. Unilateral aldosterone excess was defined as an LI of >4, while bilateral aldosterone excess was defined as an LI of <3. Concordance between the side of the adrenal nodule on CT imaging and the side of aldosterone excess on AVS was evaluated.
- Definition of clinical outcomes
- We assessed postoperative outcomes at 3 months post-surgery, according to the BP outcome published by the PASO study group [9]. Complete clinical success was defined as SBP <140 and DBP <90 mm Hg without antihypertensive medication. Partial clinical success was defined by a decrease in the number of antihypertensive medications, an SBP of >20 mm Hg, or a DBP of >10 mm Hg, with the same dose of antihypertensive medications. Alternatively, clinical success was considered absent.
- Statistical analyses
- Categorical variables are expressed as numbers (%) and were compared using the chi-square test. Continuous variables were compared using the Mann-Whitney U test for non-normally distributed variables or Student’s t test for normally distributed variables, and are expressed as medians (interquartile ranges).
- All statistical analyses were performed using R version 3.6.2 (Foundation for Statistical Computing, Vienna, Austria), and the criteria for statistical significance was P<0.05 for two-tailed tests.
- For variable selection, we applied the L1 penalized, least absolute shrinkage and selection operator (LASSO) regression to minimize potential collinearity and over-fitting of variables. We augmented 10-fold cross-validation and selected the value of the penalty parameter (λ) as 1 standard error estimate to show the highest accuracy. The R package “glmnet” was used for LASSO regression. Subsequently, the selected variables were incorporated into stepwise logistic regression models. The area under the curve (AUC), with a 95% confidence interval (CI) and cutoff points, of selected variables were analyzed using the R package “OptimalCutpoints.”
- Ethical considerations
- The studies involving human participants were reviewed and approved by the Institutional Review Board of SNUH (no. H-1801-010-911) and AMC (no. 2016-0254). The need for obtaining informed consent was waived due to the retrospective study design.
METHODS
- Study A: development of the Primary Aldosteronism Predicting Subtype score
- Among 367 PA patients with a unilateral adrenal nodule on CT, 243 (66.2%) revealed concordant unilateral excess and 19 (5.2%) revealed discordant unilateral excess in AVS (Table 1, Study A cohort). The concordant group was younger (P=0.005), had lower BMI (P<0.001), and higher DBP (P=0.041) than the discordant group. The prevalence and duration of HTN, and the dose of anti-hypertensive medications were similar, and there were no differences in the prevalence of comorbidities, including DM, CAD, atrial fibrillation, CVD, OSA, and retinopathy, between the two groups. Serum creatinine level and eGFR was also similar. The concordant group displayed lower serum potassium levels (P<0.001) and PRA (P<0.001), but higher PAC (P<0.001) and ARR (P<0.001) than the discordant group. The concordant group had a larger tumor size than the discordant group (P=0.010). In the discordant group, contralateral lateralization on AVS was present in 15.3% (19/124).
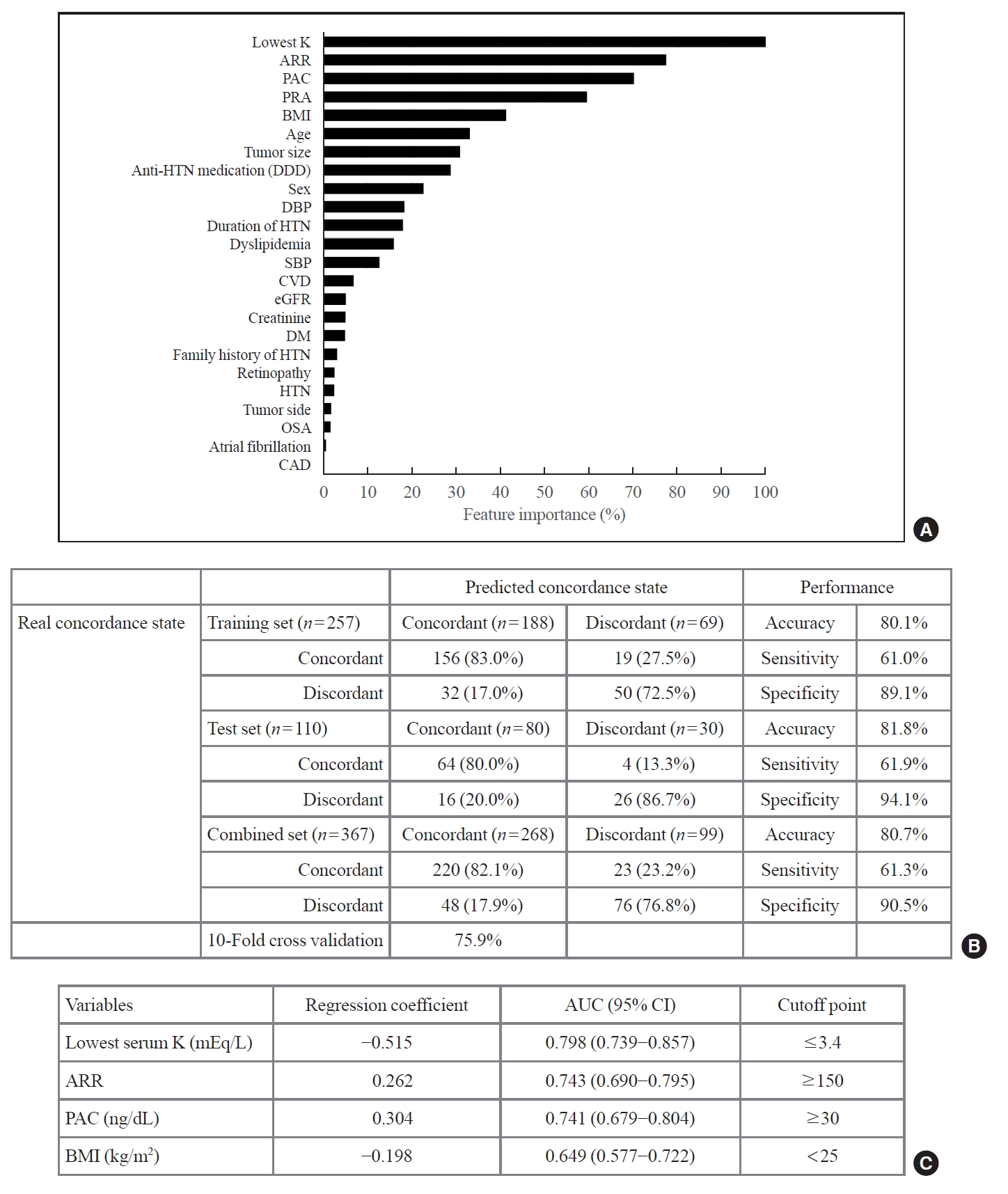
- We selected all variables in the training set to predict the concordance on AVS using the LASSO regression models (n=257) (Fig. 2). The final values used for the model were cost=0.5, and epsilon=0.001. Accuracy was used to select the optimal model, using the largest value. The confusion matrix for the training, test, and combined sets is shown in Fig. 2A. In the training set (n=257), 206 patients (accuracy, 80.1%) were correctly classified, with a sensitivity and specificity of 61.0% and 89.1%, respectively. To circumvent overfitting bias and assess generalizability, the LASSO model was validated by a 10-fold cross-validation algorithm, and the accuracy was 75.9%. In the test set, 90 of 110 patients were correctly classified (accuracy, 81.8%) (Fig. 2B). Based on the feature importance, the lowest serum potassium level, ARR, PAC, and BMI were incorporated into the final model (Fig. 2C). The cutoff point of each variable was identified in the training set, and lowest serum potassium level ≤3.4 mEq/L, ARR ≥150, PAC ≥30 ng/mL, and BMI <25 kg/m2 were identified as significant predictors of aldosterone-producing adenoma on CT.
- We performed logistic regression analysis using the above-mentioned four variables in the combined set (n=367). The odds ratios in the multivariate logistic regression models were 4.38 for lowest serum potassium level ≤3.4 mEq/L, 2.94 for ARR ≥150, 2.42 for PAC ≥30 ng/mL, and 1.89 for BMI <25 kg/m2. Accordingly, a point was assigned for each variable, and the scoring system with a total score of 10 points (the Primary Aldosteronism Predicting Subtype [PAPS] score) was developed (Table 2).
- The developed PAPS score in the training set was validated in the test set. Receiver operating characteristic (ROC) curve analysis yielded an AUC of 0.819 (95% CI, 0.774 to 0.865) (Fig. 3A). The cutoff point of PAPS score with the highest sensitivity was 10, which could avoid misclassified adrenalectomy. In the test set, a PAPS score 10 identified concordance between CT imaging and AVS findings in 20 of 23 (sensitivity, 92.9%) with an accuracy of 61.1% (Fig. 3B). A PAPS score 10 identified concordance between CT imaging and AVS findings in 62 of 65 (sensitivity, 97.6%) with an accuracy of 61.6% in the combined set. In the combined set, a PAPS score 0 identified discordance between CT imaging and AVS findings in 38 of 48 (79.2%).
- Study B: development of the Primary Aldosteronism Predicting Surgical Outcome score
- Another decision-making point revolves around whether adrenalectomy can improve the clinical outcome of unilateral PA patients. To address this, we investigated predictors for clinical success in adrenalectomized PA patients (Study B). In PA patients with unilateral adrenalectomy (n=400), 330 patients were followed-up at 3-month postoperatively. Among them, complete and partial clinical success was achieved in 191 and 103 patients (57.8% and 31.2%, respectively). Table 3 demonstrates the clinical characteristics of PA patients according to clinical success after adrenalectomy. Patients with complete clinical success were younger (P<0.001), more frequently female (P<0.001), and had lower BMI (P<0.001). Patients with complete clinical success exhibited milder HTN than those with partial or absent clinical success: lower SBP (P=0.006), shorter duration of HTN (P<0.001), and used a lower dose of antihypertensive medications (P<0.001). Moreover, the prevalence of DM, dyslipidemia, and CAD was lower in patients with complete clinical success (P=0.003). Patients with complete clinical success had lower serum creatinine levels (P=0.008), with glomerular hyperfiltration. However, there was no difference in serum potassium level, PAC, or ARR.
- We constructed stepwise logistic regression models in the training set (n=227) using all variables (Tables 4-6). In the multivariate models, four variables remained as significant predictors of complete clinical success after adrenalectomy. In the final model, female sex, HTN duration, antihypertensive medications, and CAD were included (Table 4). Next, we identified the cutoff point of continuous variables as duration of HTN <5 years and anti-HTN medication <2.5 DDD. Accordingly, a point was assigned for each variable, and a scoring system with a total score of 10 points (the Primary Aldosteronism Predicting Surgical Outcome [PAPSO] score) was developed (Table 5). In the confusion matrix using the combined set (n=370), a PAPSO score 10 identified complete clinical success in 56 of 64 (sensitivity, 94.9%) with an accuracy of 56.7% (Table 6), whereas a PAPSO score <4 identified absence of complete clinical success in 62 of 77 (specificity, 92.2%) with an accuracy of 70.6% (Table 6).
- Clinical decision-making algorithm for PA patients with a unilateral adrenal nodule
- Collectively, we suggested a clinical decision-making algorithm for PA patients with a unilateral adrenal nodule on CT (Fig. 4). First, if PA patients with PAPS score of 10 have a lowest serum potassium level ≤3.4 mEq/L, ARR ≥150, PAC ≥30 ng/mL, and BMI <25 kg/m2, AVS can be avoided, and adrenalectomy can be performed directly (17.7% in our cohort). On the other hand, if the PA patients with PAPS score of 0 do not satisfy any of the above four criteria, the probability for bilateral secretion was very high, and medical therapy can commence (13.1% in our cohort). Second, those with PAPS score 1 to 9 who satisfied any of the four criteria can be reassessed based on female sex, HTN duration <5 years, antihypertensive medications <2.5 DDD, and the absence of CAD. If they satisfied the criteria with PAPSO scores <4, postoperative clinical improvement was less likely (complete success rate, 18.6%), and medical therapy can be recommended, without AVS. However, if they meet the criteria with PAPSO scores ≥4, AVS may be required for surgery.
- Validation of our clinical decision-making algorithms in the independent validation set
- We further validated our algorithm in the independent validation set (n=53). Clinical characteristics of study subjects in the validation dataset were shown in Table 7. Compared with PA patients who satisfied the inclusion criteria of both Study A and B as the development set (n=239), clinical characteristics except ARR were not different between the validation set and development set. A PAPS score 10 identified concordances between CT imaging and AVS findings in 12 of 12 (sensitivity, 100.0%), whereas a PAPS score 0 identified discordance between CT imaging and AVS findings in 1 of 2 (50.0%) (Table 8). In PA patients with PAPS scores ranging from 1 to 9 points (n=35, 66.0%), a PAPSO score <4 identified absence of complete clinical success in 9 of 11 (specificity, 81.8%).
RESULTS
- In the present study, we developed a new outcome-driven diagnostic algorithm for AVS and surgery in PA patients that incorporated which patients would benefit from the surgery. We predicted that surgery without AVS can be performed in non-obese patients with a unilateral adrenal nodule, hypokalemia, ARR ≥ 150, and PAC ≥30 ng/mL, with a sensitivity of 97.6%. For the remaining patients, the algorithm indicates that female patients with an HTN duration <5 years, antihypertensive medications <2.5 DDD, and without CAD may benefit from adrenalectomy, with a sensitivity of 94.2%.
- Previous reports have suggested clinical prediction scores for circumventing invasive AVS in unilateral aldosterone excess [5-7,14,17]. Firstly, Kupers et al. [5] developed a clinical prediction score, including typical Conn’s adenoma (≥8 mm on CT), hypokalemia, and glomerular hyperfiltration (eGFR >100 mL/min/1.73 m2). This scoring system exhibited a specificity of 100%, and 30% of PA patients could undergo surgery without AVS directly. However, this score showed very low sensitivity (46% to 64%) and specificity (53% to 85%) in other validated studies [7,18,19]. Therefore, Kuper’s prediction score was considered as a complementary tool for AVS. Subsequently, to improve the accuracy of clinical prediction scores, the extent of aldosterone excess, as indicated by PAC and the ARR, was incorporated into the scoring system in other studies [6,8,17,20,21]. However, those studies were limited by the small number of enrolled patients, data from confirmation testing, and lack of internal and external validation. The scoring system suggested by Kamemura et al. [22] was developed based on 200 patients but only applied to patients with no adrenal nodule on CT. Kobayashi et al. [23] also developed a score for bilateral PA based on 1,290 patients, which was validated in 646 patients, and reported a positive-predictive value of 93.5%. However, their scoring system can be applied to few patients, because they assumed no adrenal nodule on CT. Recently, Burrello et al. [8] combined PAC at screening and after a SIT, serum potassium level, the presence of an adrenal nodule, the largest nodule size, and unilateral adrenal nodule as predictive variables using a machine learning algorithm and an external validation set. However, PAC at screening and after SIT were collinear, and the three imaging variables were redundant. In our study, we incorporated PAC at screening instead of post-SIT PAC. We assumed a unilateral adrenal nodule because CT imaging is easily performed, and the lack of tumor or bilateral lesions on CT require AVS to decide on surgery. Furthermore, in the present study, nodule size was not a strong predictor among the 32 variables, although the nodule size differed between the two groups.
- In our cohort, 57.8% (191/330) of subjects achieved HTN resolution, and 31.2% achieved HTN improvement after surgery. In previous studies, the proportion of patients with complete clinical success was 16% to 72% [10,24-27]. The discrepancy in clinical success rate can be attributed to different outcomes and study populations. In 2017, the PASO study group was defined, and the clinical outcome was standardized. They reported that 37% (range, 17 to 62) and 47% (range, 35 to 66) of patients achieved complete and partial clinical success, respectively [9]. We also followed the PASO criteria, and the clinical success rate was comparable to the PASO results.
- Several potential predictors of complete clinical success have been reported. First, the ARS included the number of antihypertensive medications, HTN duration, BMI, and female sex [10]. The ARS was validated in several studies, with an AUC of 0.71 to 0.84 [11-13]. Other groups also included these variables as outcome predictors [14,15]. The number of antihypertensive medications and the duration of HTN may reflect the absence of essential HTN or vascular damage caused by long-term aldosterone excess. These variables also remained strong predictors in our final models.
- Female sex was also a significant prognostic factor in our study. Although the mechanism was uncertain, estrogen may have a vasoprotective effect on salt-sensitive HTN as well as on heart and kidney diseases [28-30]. Barrett Mueller et al. [31] also demonstrated that estrogens suppress renin‒angiotensin‒aldosterone system activity, which attenuates the complication of aldosterone excess. High BMI may be associated with essential HTN as well as persistent HTN after adrenalectomy [32]. However, in our final model, the inclusion of the female sex abolished the effect of low BMI because female individuals may have a relatively lower BMI than male individuals.
- Morisaki et al. [15] newly identified DM as a predictive factor of the postoperative outcome. The presence of DM is strongly associated with the progression of essential HTN [33]. The prevalence of DM was also significantly higher in the partial/absent clinical success group in the present study. Nonetheless, DM was not selected as a significant variable in multivariate analysis. Instead, we identified the presence of CAD as a new predictor, which implicates target organ complications of long-term aldosterone excess. In this regard, Burrello et al. [14] also included left ventricular hypertrophy and microalbuminuria as target organ damage in the PASO score. However, they did not evaluate hypertensive retinopathy, chronic kidney disease, and peripheral artery disease as possible factors.
- There are several strengths in the present study. In real practice, subjects with a unilateral nodule are cases who require decision-making, including whether to perform AVS and surgery. In contrast to previous reports, we included subjects with unilateral nodules. For these patients, the question arises whether they should undergo AVS to ascertain whether they require surgery. We used a moderate sample size from two different centers. We included the ARR, without confirmatory data, which expands the usefulness of our algorithm. We emphasized the clinical decision algorithm instead of a simple scoring system. We simultaneously included the unilateral aldosterone excess and postoperative benefit for deciding on surgery in PA patients with a unilateral adrenal nodule. In terms of methodology, the machine learning algorithm, such as linear discriminant analysis or random forest analysis, was introduced in the PASO score [14]. Rather, we selected representative variables using the LASSO method, which shrinks the estimates of weaker factors toward zero and allows the strongest predictors alone to remain in the model. Additionally, we calculated the standardized potency of antihypertensive agents, expressed as DDD, instead of simply using the number of antihypertensive medications.
- The study had some limitations. It was a long-term retrospective cohort study, which may increase the risk of ascertainment bias. We did not assess biochemical success because biochemical data were not available for a considerable number of patients at the postoperative follow-up visit (144 of 330, 43.6%). Clinical outcome was assessed at the 3-month postoperative follow-up; thus, complete remission can be underestimated because the resolution of HTN may take up to 6 months after surgery. Unfortunately, our algorithm was not validated in another independent cohort. To compensate for these shortcomings, we conducted the study in subjects from two centers and randomly split these into the training and testing sets, and validated the algorithm’s accuracy in the testing set.
- Recent research reported on the expanding spectrum of PA [34]. A considerable number of patients present with bilateral, but asymmetrical aldosterone excess. Thus, simple dichotomization into unilateral and bilateral PA does not reflect the complexity of PA. Given the clinical spectrum of PA, we envisioned an outcome-based algorithm instead of dichotomized treatment. Our algorithm may help clinicians to decide to perform AVS or to undergo surgery in clinical practice.
DISCUSSION
-
CONFLICTS OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
Conception or design: J.H.K., S.H.L. Acquisition, analysis, or interpretation of data: J.H.K., C.H.A., S.J.K., K.E.L., J.W.K., H.K.Y., Y.M.L., T.Y.S., S.W.K., C.S.S., J.M.K., S.H.L. Drafting the work or revising: J.H.K. Final approval of the manuscript: J.H.K., C.H.A., S.J.K., K.E.L., J.W.K., H.K.Y., Y.M.L., T.Y.S., S.W.K., C.S.S., J.M.K., S.H.L.
Article information
-
Acknowledgements
- This study was funded by the Asan Institute for Life Sciences, Seoul, Republic of Korea (project no. 2019IP0862) and the National Research Foundation of Korea by the Ministry of Science, ICT, and Future Planning of Korea (NRF-2020R1C1-C1010723).


Values are expressed as median (interquartile ranges) or number (%). Data with non-normal distribution were analyzed using the Mann‒Whitney U test.
CT, computed tomography; AVS, adrenal venous sampling; BMI, body mass index; SBP, systolic blood pressure; DBP, diastolic blood pressure; HTN, hypertension; DDD, daily defined dose; DM, diabetes mellitus; CAD, coronary artery disease; CVD, cerebrovascular disease; OSA, obstructive sleep apnea; eGFR, estimated glomerular filtration rate; PAC, plasma aldosterone concentration; PRA, plasma renin activity; ARR, aldosterone-to-renin ratio.
a Five subjects among 372 primary aldosteronism patients with unilateral adrenal nodule on CT were excluded due to the missing variable values.
Values are expressed as median (interquartile ranges) or number (%). Data with non-normal distribution were analyzed using the Mann‒Whitney U test.
BMI, body mass index; SBP, systolic blood pressure; DBP, diastolic blood pressure; HTN, hypertension; DDD, daily defined dose; DM, diabetes mellitus; CAD, coronary artery disease; CVD, cerebrovascular disease; OSA, obstructive sleep apnea; eGFR, estimated glomerular filtration rate; PAC, plasma aldosterone concentration; PRA, plasma renin activity; ARR, aldosterone-to-renin ratio; CT, computed tomography.
The cutoff point of each variable was developed using the R package “OptimalCutpoints.” Univariate and multivariate logistic regression models were generated.
PAPSO score, Primary Aldosteronism Predicting Surgical Outcome score; OR, odds ratio; CI, confidence interval; HTN, hypertension; DDD, defined daily dose.
| Score | Value | Concordance | Complete clinical success |
|---|---|---|---|
| PAPS score=10 points | 16 (30.2) | 12 of 12a (100) | 11 of 16 (68.8) |
| PAPS score=0 points | 2 (3.8) | 1 of 2 (50.0) | 0 of 2 (0) |
| PAPS score=1‒9 points | 35 (66.0) | 16 of 35 (45.7) | |
| PAPSO score ≥4 points | 24 (45.3) | 14 of 24 (58.3) | |
| PAPSO score <4 points | 11 (20.7) | 2 of 11 (18.2) | |
| Total | 53 (100.0) | 27 of 53 (50.9) |
- 1. Funder JW, Carey RM, Mantero F, Murad MH, Reincke M, Shibata H, et al. The management of primary aldosteronism: case detection, diagnosis, and treatment: an Endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab 2016;101:1889–916.ArticlePubMed
- 2. Monticone S, Burrello J, Tizzani D, Bertello C, Viola A, Buffolo F, et al. Prevalence and clinical manifestations of primary aldosteronism encountered in primary care practice. J Am Coll Cardiol 2017;69:1811–20.ArticlePubMed
- 3. Monticone S, D’Ascenzo F, Moretti C, Williams TA, Veglio F, Gaita F, et al. Cardiovascular events and target organ damage in primary aldosteronism compared with essential hypertension: a systematic review and meta-analysis. Lancet Diabetes Endocrinol 2018;6:41–50.ArticlePubMed
- 4. Monticone S, Viola A, Rossato D, Veglio F, Reincke M, Gomez-Sanchez C, et al. Adrenal vein sampling in primary aldosteronism: towards a standardised protocol. Lancet Diabetes Endocrinol 2015;3:296–303.ArticlePubMed
- 5. Kupers EM, Amar L, Raynaud A, Plouin PF, Steichen O. A clinical prediction score to diagnose unilateral primary aldosteronism. J Clin Endocrinol Metab 2012;97:3530–7.ArticlePubMed
- 6. Nanba K, Tsuiki M, Nakao K, Nanba A, Usui T, Tagami T, et al. A subtype prediction score for primary aldosteronism. J Hum Hypertens 2014;28:716–20.ArticlePubMed
- 7. Zhang Y, Niu W, Zheng F, Zhang H, Zhou W, Shen Z, et al. Identifying unilateral disease in Chinese patients with primary aldosteronism by using a modified prediction score. J Hypertens 2017;35:2486–92.ArticlePubMedPMC
- 8. Burrello J, Burrello A, Pieroni J, Sconfienza E, Forestiero V, Rabbia P, et al. Development and validation of prediction models for subtype diagnosis of patients with primary aldosteronism. J Clin Endocrinol Metab 2020;105:dgaa379.ArticlePubMed
- 9. Williams TA, Lenders JW, Mulatero P, Burrello J, Rottenkolber M, Adolf C, et al. Outcomes after adrenalectomy for unilateral primary aldosteronism: an international consensus on outcome measures and analysis of remission rates in an international cohort. Lancet Diabetes Endocrinol 2017;5:689–99.ArticlePubMedPMC
- 10. Zarnegar R, Young WF Jr, Lee J, Sweet MP, Kebebew E, Farley DR, et al. The aldosteronoma resolution score: predicting complete resolution of hypertension after adrenalectomy for aldosteronoma. Ann Surg 2008;247:511–8.PubMed
- 11. Utsumi T, Kawamura K, Imamoto T, Kamiya N, Komiya A, Suzuki S, et al. High predictive accuracy of aldosteronoma resolution score in Japanese patients with aldosterone-producing adenoma. Surgery 2012;151:437–43.ArticlePubMed
- 12. Aronova A, Gordon BL, Finnerty BM, Zarnegar R, Fahey TJ 3rd. Aldosteronoma resolution score predicts long-term resolution of hypertension. Surgery 2014;156:1387–93.ArticlePubMed
- 13. Pasquier L, Kirouani M, Fanget F, Nomine C, Caillard C, Arnault V, et al. Assessment of the Aldosteronona resolution score as a predictive resolution score of hypertension after adrenalectomy for aldosteronoma in French patients. Langenbecks Arch Surg 2017;402:309–14.ArticlePubMed
- 14. Burrello J, Burrello A, Stowasser M, Nishikawa T, Quinkler M, Prejbisz A, et al. The primary aldosteronism surgical outcome score for the prediction of clinical outcomes after adrenalectomy for unilateral primary aldosteronism. Ann Surg 2020;272:1125–32.ArticlePubMed
- 15. Morisaki M, Kurihara I, Itoh H, Naruse M, Takeda Y, Katabami T, et al. Predictors of clinical success after surgery for primary aldosteronism in the Japanese Nationwide Cohort. J Endocr Soc 2019;3:2012–22.ArticlePubMedPMC
- 16. Vincent JM, Morrison ID, Armstrong P, Reznek RH. The size of normal adrenal glands on computed tomography. Clin Radiol 1994;49:453–5.ArticlePubMed
- 17. Leung HT, Woo YC, Fong CH, Tan KC, Lau EY, Chan KW, et al. A clinical prediction score using age at diagnosis and saline infusion test parameters can predict aldosterone-producing adenoma from idiopathic adrenal hyperplasia. J Endocrinol Invest 2020;43:347–55.ArticlePubMed
- 18. Riester A, Fischer E, Degenhart C, Reiser MF, Bidlingmaier M, Beuschlein F, et al. Age below 40 or a recently proposed clinical prediction score cannot bypass adrenal venous sampling in primary aldosteronism. J Clin Endocrinol Metab 2014;99:E1035–9.ArticlePubMed
- 19. Venos ES, So B, Dias VC, Harvey A, Pasieka JL, Kline GA. A clinical prediction score for diagnosing unilateral primary aldosteronism may not be generalizable. BMC Endocr Disord 2014;14:94.ArticlePubMedPMC
- 20. Kocjan T, Janez A, Stankovic M, Vidmar G, Jensterle M. A new clinical prediction criterion accurately determines a subset of patients with bilateral primary aldosteronism before adrenal venous sampling. Endocr Pract 2016;22:587–94.ArticlePubMed
- 21. Kobayashi H, Haketa A, Ueno T, Ikeda Y, Hatanaka Y, Tanaka S, et al. Scoring system for the diagnosis of bilateral primary aldosteronism in the outpatient setting before adrenal venous sampling. Clin Endocrinol (Oxf) 2017;86:467–72.ArticlePubMed
- 22. Kamemura K, Wada N, Ichijo T, Matsuda Y, Fujii Y, Kai T, et al. Significance of adrenal computed tomography in predicting laterality and indicating adrenal vein sampling in primary aldosteronism. J Hum Hypertens 2017;31:195–9.ArticlePubMed
- 23. Kobayashi H, Abe M, Soma M, Takeda Y, Kurihara I, Itoh H, et al. Development and validation of subtype prediction scores for the workup of primary aldosteronism. J Hypertens 2018;36:2269–76.ArticlePubMed
- 24. Lumachi F, Ermani M, Basso SM, Armanini D, Iacobone M, Favia G. Long-term results of adrenalectomy in patients with aldosterone-producing adenomas: multivariate analysis of factors affecting unresolved hypertension and review of the literature. Am Surg 2005;71:864–9.ArticlePubMed
- 25. Steichen O, Zinzindohoue F, Plouin PF, Amar L. Outcomes of adrenalectomy in patients with unilateral primary aldosteronism: a review. Horm Metab Res 2012;44:221–7.ArticlePubMed
- 26. Rossi GP, Cesari M, Cuspidi C, Maiolino G, Cicala MV, Bisogni V, et al. Long-term control of arterial hypertension and regression of left ventricular hypertrophy with treatment of primary aldosteronism. Hypertension 2013;62:62–9.ArticlePubMed
- 27. Muth A, Ragnarsson O, Johannsson G, Wangberg B. Systematic review of surgery and outcomes in patients with primary aldosteronism. Br J Surg 2015;102:307–17.ArticlePubMed
- 28. Manosroi W, Tan JW, Rariy CM, Sun B, Goodarzi MO, Saxena AR, et al. The association of estrogen receptor-β gene variation with salt-sensitive blood pressure. J Clin Endocrinol Metab 2017;102:4124–35.ArticlePubMedPMC
- 29. Mihailidou AS, Ashton AW. Cardiac effects of aldosterone: does gender matter? Steroids 2014;91:32–7.ArticlePubMed
- 30. Komukai K, Mochizuki S, Yoshimura M. Gender and the renin-angiotensin-aldosterone system. Fundam Clin Pharmacol 2010;24:687–98.ArticlePubMed
- 31. Barrett Mueller K, Lu Q, Mohammad NN, Luu V, McCurley A, Williams GH, et al. Estrogen receptor inhibits mineralocorticoid receptor transcriptional regulatory function. Endocrinology 2014;155:4461–72.ArticlePubMedPMC
- 32. Willett WC, Dietz WH, Colditz GA. Guidelines for healthy weight. N Engl J Med 1999;341:427–34.ArticlePubMed
- 33. Cruickshank K, Riste L, Anderson SG, Wright JS, Dunn G, Gosling RG. Aortic pulse-wave velocity and its relationship to mortality in diabetes and glucose intolerance: an integrated index of vascular function? Circulation 2002;106:2085–90.ArticlePubMed
- 34. Vaidya A, Mulatero P, Baudrand R, Adler GK. The expanding spectrum of primary aldosteronism: implications for diagnosis, pathogenesis, and treatment. Endocr Rev 2018;39:1057–88.ArticlePubMedPMC
References
Figure & Data
References
Citations

- Subtype-specific Body Composition and Metabolic Risk in Patients With Primary Aldosteronism
Seung Shin Park, Chang Ho Ahn, Sang Wan Kim, Ji Won Yoon, Jung Hee Kim
The Journal of Clinical Endocrinology & Metabolism.2024; 109(2): e788. CrossRef - Prognostic models to predict complete resolution of hypertension after adrenalectomy in primary aldosteronism: A systematic review and meta‐analysis
Luigi Marzano, Amir Kazory, Faeq Husain‐Syed, Claudio Ronco
Clinical Endocrinology.2023; 99(1): 17. CrossRef - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - Correlation of Histopathologic Subtypes of Primary Aldosteronism with Clinical Phenotypes and Postsurgical Outcomes
Chang Ho Ahn, You-Bin Lee, Jae Hyeon Kim, Young Lyun Oh, Jung Hee Kim, Kyeong Cheon Jung
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef

 KES
KES
 PubReader
PubReader ePub Link
ePub Link Cite
Cite