Search
- Page Path
- HOME > Search
Review Articles
- Thyroid
- Management of Subclinical Hypothyroidism: A Focus on Proven Health Effects in the 2023 Korean Thyroid Association Guidelines
- Eu Jeong Ku, Won Sang Yoo, Hyun Kyung Chung
- Endocrinol Metab. 2023;38(4):381-391. Published online August 8, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1778
- 2,969 View
- 455 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
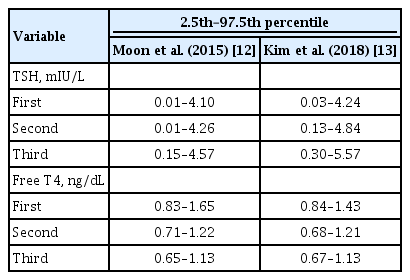
ePub - Subclinical hypothyroidism (SCH) is characterized by elevated thyroid-stimulating hormone (TSH) and normal free thyroxine levels. The Korean Thyroid Association recently issued a guideline for managing SCH, which emphasizes Korean-specific TSH diagnostic criteria and highlights the health benefits of levothyroxine (LT4) treatment. A serum TSH level of 6.8 mIU/L is presented as the reference value for diagnosing SCH. SCH can be classified as mild (TSH 6.8 to 10.0 mIU/L) or severe (TSH >10.0 mIU/L), and patients can be categorized as adults (age <70 years) or elderly (age ≥70 years), depending on the health effects of LT4 treatment. An initial increase in serum TSH levels should be reassessed with a subsequent measurement, including a thyroid peroxidase antibody test, preferably 2 to 3 months after the initial assessment. While LT4 treatment is not generally recommended for mild SCH in adults, it is necessary for severe SCH in patients with underlying coronary artery disease or heart failure and it may be considered for those with concurrent dyslipidemia. Conversely, LT4 treatment is generally not recommended for elderly patients, regardless of SCH severity. For those SCH patients who are prescribed LT4 treatment, the dosage should be personalized, and serum TSH levels should be regularly monitored to maintain the optimal LT4 regimen.
-
Citations
Citations to this article as recorded by- Clinical Implications of Different Thyroid-Stimulating Hormone (TSH) Reference Intervals between TSH Kits for the Management of Subclinical Hypothyroidism
Won Sang Yoo
Endocrinology and Metabolism.2024; 39(1): 188. CrossRef
- Clinical Implications of Different Thyroid-Stimulating Hormone (TSH) Reference Intervals between TSH Kits for the Management of Subclinical Hypothyroidism

- Thyroid
- Diagnosis and Management of Thyroid Disease during Pregnancy and Postpartum: 2023 Revised Korean Thyroid Association Guidelines
- Hwa Young Ahn, Ka Hee Yi
- Endocrinol Metab. 2023;38(3):289-294. Published online June 9, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1696
- 6,339 View
- 696 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Thyroid hormone plays a critical role in fetal growth and development, and thyroid dysfunction during pregnancy is associated with several adverse outcomes, such as miscarriage and preterm birth. In this review, we introduce and explain three major changes in the revised Korean Thyroid Association (KTA) guidelines for the diagnosis and management of thyroid disease during pregnancy: first, the normal range of thyroid-stimulating hormone (TSH) during pregnancy; second, the treatment of subclinical hypothyroidism; and third, the management of euthyroid pregnant women with positive thyroid autoantibodies. The revised KTA guidelines adopt 4.0 mIU/L as the upper limit of TSH in the first trimester. A TSH level between 4.0 and 10.0 mIU/L, combined with free thyroxine (T4) within the normal range, is defined as subclinical hypothyroidism, and a TSH level over 10 mIU/L is defined as overt hypothyroidism regardless of the free T4 level. Levothyroxine treatment is recommended when the TSH level is higher than 4 mIU/L in subclinical hypothyroidism, regardless of thyroid peroxidase antibody positivity. However, thyroid hormone therapy to prevent miscarriage is not recommended in thyroid autoantibody-positive women with normal thyroid function.
-
Citations
Citations to this article as recorded by- Use of thyroid hormones in hypothyroid and euthyroid patients: A survey of members of the Endocrine Society of Australia
Nicole Lafontaine, Suzanne J. Brown, Petros Perros, Enrico Papini, Endre V. Nagy, Roberto Attanasio, Laszlo Hegedüs, John P. Walsh
Clinical Endocrinology.2024; 100(5): 477. CrossRef - Management of Subclinical Hypothyroidism: A Focus on Proven Health Effects in the 2023 Korean Thyroid Association Guidelines
Eu Jeong Ku, Won Sang Yoo, Hyun Kyung Chung
Endocrinology and Metabolism.2023; 38(4): 381. CrossRef - Maternal isolated hypothyroxinemia in the first trimester is not associated with adverse pregnancy outcomes, except for macrosomia: a prospective cohort study in China
Jing Du, Linong Ji, Xiaomei Zhang, Ning Yuan, Jianbin Sun, Dan Zhao
Frontiers in Endocrinology.2023;[Epub] CrossRef
- Use of thyroid hormones in hypothyroid and euthyroid patients: A survey of members of the Endocrine Society of Australia

- Thyroid
- Thyroid Function across the Lifespan: Do Age-Related Changes Matter?
- John P. Walsh
- Endocrinol Metab. 2022;37(2):208-219. Published online April 14, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1463
- 5,922 View
- 332 Download
- 12 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
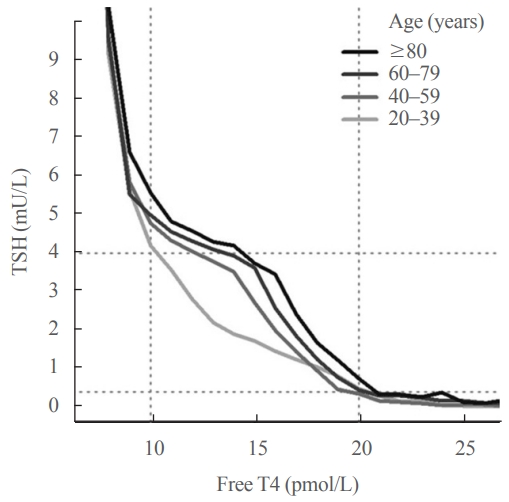
ePub - Circulating concentrations of thyrotropin (TSH) and thyroxine (T4) are tightly regulated. Each individual has setpoints for TSH and free T4 which are genetically determined, and subject to environmental and epigenetic influence. Pituitary-thyroid axis setpoints are probably established in utero, with maturation of thyroid function continuing until late gestation. From neonatal life (characterized by a surge of TSH and T4 secretion) through childhood and adolescence (when free triiodothyronine levels are higher than in adults), thyroid function tests display complex, dynamic patterns which are sexually dimorphic. In later life, TSH increases with age in healthy older adults without an accompanying fall in free T4, indicating alteration in TSH setpoint. In view of this, and evidence that mild subclinical hypothyroidism in older people has no health impact, a strong case can be made for implementation of age-related TSH reference ranges in adults, as is routine in children.
-
Citations
Citations to this article as recorded by- The ageing thyroid: implications for longevity and patient care
Diana van Heemst
Nature Reviews Endocrinology.2024; 20(1): 5. CrossRef - Incidence and Determinants of Spontaneous Normalization of Subclinical Hypothyroidism in Older Adults
Evie van der Spoel, Nicolien A van Vliet, Rosalinde K E Poortvliet, Robert S Du Puy, Wendy P J den Elzen, Terence J Quinn, David J Stott, Naveed Sattar, Patricia M Kearney, Manuel R Blum, Heba Alwan, Nicolas Rodondi, Tinh-Hai Collet, Rudi G J Westendorp,
The Journal of Clinical Endocrinology & Metabolism.2024; 109(3): e1167. CrossRef - Multi-trait analysis characterizes the genetics of thyroid function and identifies causal associations with clinical implications
Rosalie B. T. M. Sterenborg, Inga Steinbrenner, Yong Li, Melissa N. Bujnis, Tatsuhiko Naito, Eirini Marouli, Tessel E. Galesloot, Oladapo Babajide, Laura Andreasen, Arne Astrup, Bjørn Olav Åsvold, Stefania Bandinelli, Marian Beekman, John P. Beilby, Jette
Nature Communications.2024;[Epub] CrossRef - Evaluation of multiple organophosphate insecticide exposure in relation to altered thyroid hormones in NHANES 2007‐2008 adult population
Massira Ousseni Diawara, Songtao Li, Mingzhi Zhang, Francis Manyori Bigambo, Xu Yang, Xu Wang, Tianyu Dong, Di Wu, Chenghao Yan, Yankai Xia
Ecotoxicology and Environmental Safety.2024; 273: 116139. CrossRef - Thyroid-function reference ranges in the diagnosis of thyroid dysfunction in adults
Salman Razvi
Nature Reviews Endocrinology.2024; 20(5): 253. CrossRef - Association between exposure to chemical mixtures and epigenetic ageing biomarkers: Modifying effects of thyroid hormones and physical activity
Wanying Shi, Jianlong Fang, Huimin Ren, Peijie Sun, Juan Liu, Fuchang Deng, Shuyi Zhang, Qiong Wang, Jiaonan Wang, Shilu Tong, Song Tang, Xiaoming Shi
Journal of Hazardous Materials.2024; 469: 134009. CrossRef - DNA Methylation in Autoimmune Thyroid Disease
Nicole Lafontaine, Scott G Wilson, John P Walsh
The Journal of Clinical Endocrinology & Metabolism.2023; 108(3): 604. CrossRef - A Causality between Thyroid Function and Bone Mineral Density in Childhood: Abnormal Thyrotropin May Be Another Pediatric Predictor of Bone Fragility
Dongjin Lee, Moon Ahn
Metabolites.2023; 13(3): 372. CrossRef - Serum Lipidomic Analysis Reveals Biomarkers and Metabolic Pathways of Thyroid Dysfunction
Hua Dong, Wenjie Zhou, Xingxu Yan, Huan Zhao, Honggang Zhao, Yan Jiao, Guijiang Sun, Yubo Li, Zuncheng Zhang
ACS Omega.2023; 8(11): 10355. CrossRef - Developmental and environmental modulation of fecal thyroid hormone levels in wild Assamese macaques (Macaca assamensis)
Verena Behringer, Michael Heistermann, Suchinda Malaivijitnond, Oliver Schülke, Julia Ostner
American Journal of Primatology.2023;[Epub] CrossRef - Prevalence of Functional Alterations and the Effects of Thyroid
Autoimmunity on the Levels of TSH in an Urban Population of Colombia:
A Population-Based Study
Hernando Vargas-Uricoechea, Valentina Agredo-Delgado, Hernando David Vargas-Sierra, María V. Pinzón-Fernández
Endocrine, Metabolic & Immune Disorders - Drug Targets.2023; 23(6): 857. CrossRef - Genetic determinants of thyroid function in children
Tessa A Mulder, Purdey J Campbell, Peter N Taylor, Robin P Peeters, Scott G Wilson, Marco Medici, Colin Dayan, Vincent V W Jaddoe, John P Walsh, Nicholas G Martin, Henning Tiemeier, Tim I M Korevaar
European Journal of Endocrinology.2023; 189(2): 164. CrossRef - Relationship between Thyroid CT Density, Volume, and Future TSH Elevation: A 5-Year Follow-Up Study
Tomohiro Kikuchi, Shouhei Hanaoka, Takahiro Nakao, Yukihiro Nomura, Takeharu Yoshikawa, Md Ashraful Alam, Harushi Mori, Naoto Hayashi
Life.2023; 13(12): 2303. CrossRef - Thyroid Stimulating Hormone and Thyroid Hormones (Triiodothyronine and Thyroxine): An American Thyroid Association-Commissioned Review of Current Clinical and Laboratory Status
Katleen Van Uytfanghe, Joel Ehrenkranz, David Halsall, Kelly Hoff, Tze Ping Loh, Carole A. Spencer, Josef Köhrle
Thyroid®.2023; 33(9): 1013. CrossRef - Blood hormones and suicidal behaviour: A systematic review and meta-analysis
Xue-Lei Fu, Xia Li, Jia-Mei Ji, Hua Wu, Hong-Lin Chen
Neuroscience & Biobehavioral Reviews.2022; 139: 104725. CrossRef
- The ageing thyroid: implications for longevity and patient care

Original Articles
- Thyroid
- Developmental Hypothyroidism Influences the Development of the Entorhinal-Dentate Gyrus Pathway of Rat Offspring
- Ting Jin, Ranran Wang, Shiqiao Peng, Xin Liu, Hanyi Zhang, Xue He, Weiping Teng, Xiaochun Teng
- Endocrinol Metab. 2022;37(2):290-302. Published online April 8, 2022
- DOI: https://doi.org/10.3803/EnM.2021.1343
- 3,106 View
- 96 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Developmental hypothyroidism impairs learning and memory in offspring, which depend on extensive neuronal circuits in the entorhinal cortex, together with the hippocampus and neocortex. The entorhinal-dentate gyrus pathway is the main entrance of memory circuits. We investigated whether developmental hypothyroidism impaired the morphological development of the entorhinal-dentate gyrus pathway.
Methods
We examined the structure and function of the entorhinal-dentate gyrus pathway in response to developmental hypothyroidism induced using 2-mercapto-1-methylimidazole.
Results
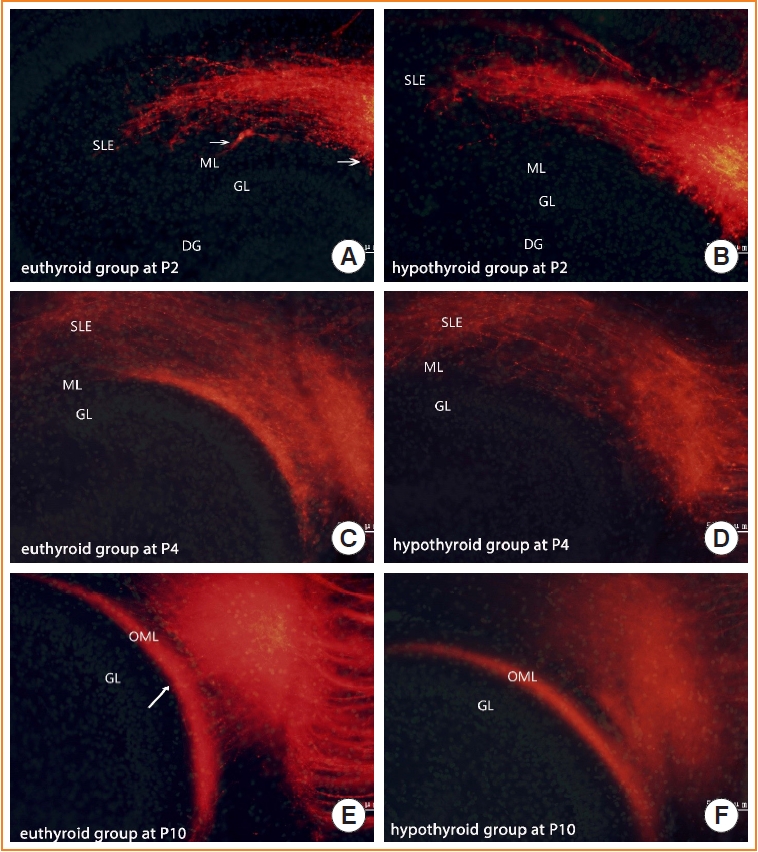
1,1´-Dioctadecyl-3,3,3´,3´-tetramethylindocarbocyanine perchlorate tract tracing indicated that entorhinal axons showed delayed growth in reaching the outer molecular layer of the dentate gyrus at postnatal days 2 and 4 in hypothyroid conditions. The proportion of fibers in the outer molecular layer was significantly smaller in the hypothyroid group than in the euthyroid group at postnatal day 4. At postnatal day 10, the pathway showed a layer-specific distribution in the outer molecular layer, similar to the euthyroid group. However, the projected area of entorhinal axons was smaller in the hypothyroid group than in the euthyroid group. An electrophysiological examination showed that hypothyroidism impaired the long-term potentiation of the perforant and the cornu ammonis 3–cornu ammonis 1 pathways. Many repulsive axon guidance molecules were involved in the formation of the entorhinaldentate gyrus pathway. The hypothyroid group had higher levels of erythropoietin-producing hepatocyte ligand A3 and semaphorin 3A than the euthyroid group.
Conclusion
We demonstrated that developmental hypothyroidism might influence the development of the entorhinal-dentate gyrus pathway, contributing to impaired long-term potentiation. These findings improve our understanding of neural mechanisms for memory function. -
Citations
Citations to this article as recorded by- Semaphorin 3A Increases in the Plasma of Women with Diminished Ovarian Reserve Who Respond Better to Controlled Ovarian Stimulation
Michela Palese, Gabriella Ferretti, Giuseppe Perruolo, Sara Serafini, Rossana Sirabella, Vincenzo Marrone, Martina De Rosa, Laura Sarno, Ida Strina, Carmela Matrone, Maurizio Guida
Life.2024; 14(3): 358. CrossRef
- Semaphorin 3A Increases in the Plasma of Women with Diminished Ovarian Reserve Who Respond Better to Controlled Ovarian Stimulation

- Thyroid
- Association between Thyroid Function and Heart Rate Monitored by Wearable Devices in Patients with Hypothyroidism
- Ki-Hun Kim, Juhui Lee, Chang Ho Ahn, Hyeong Won Yu, June Young Choi, Ho-Young Lee, Won Woo Lee, Jae Hoon Moon
- Endocrinol Metab. 2021;36(5):1121-1130. Published online October 21, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1216
- 5,370 View
- 155 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
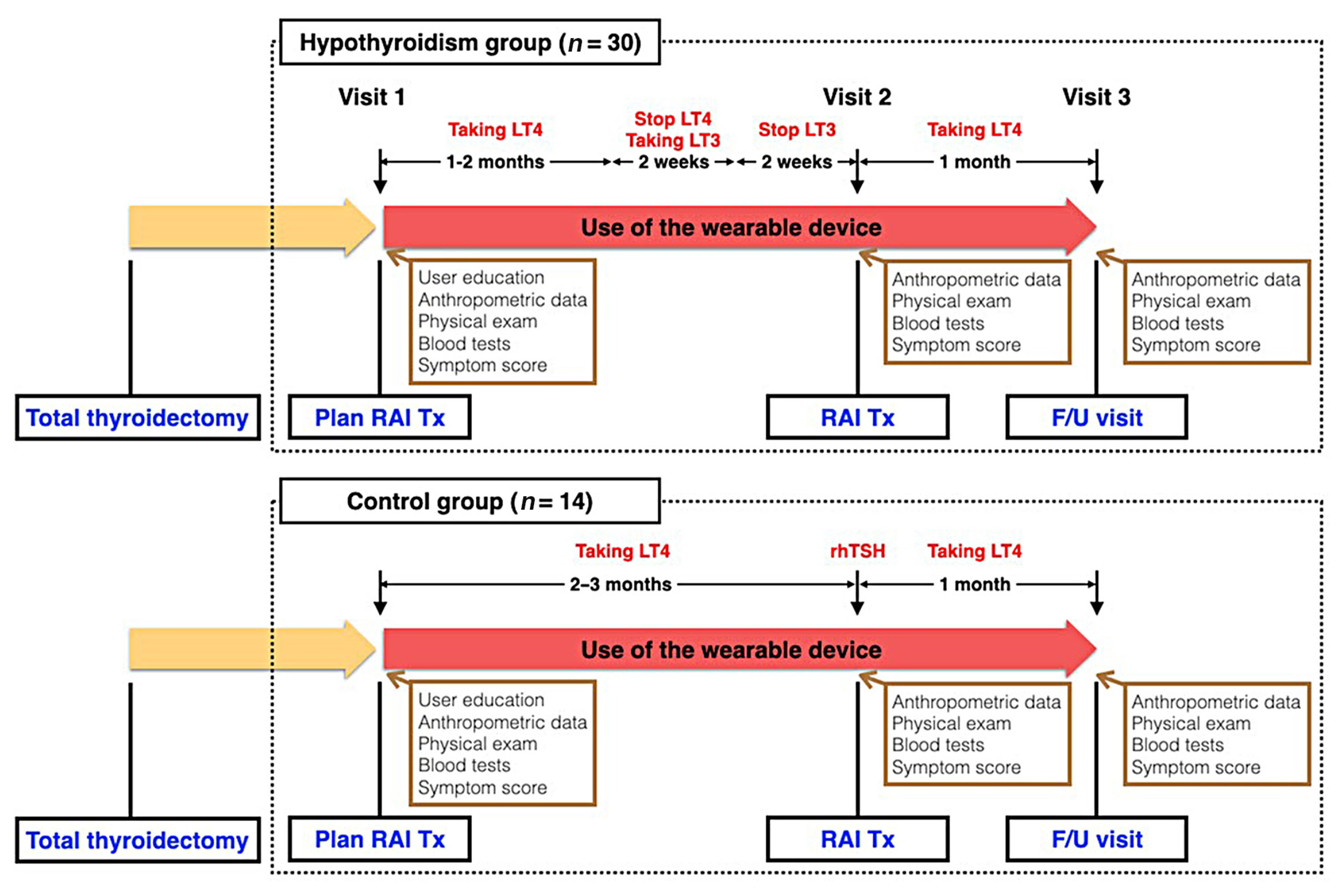
Heart rate (HR) monitored by a wearable device (WD) has demonstrated its clinical feasibility for thyrotoxicosis subjects. However, the association of HR monitored by wearables with hypothyroidism has not been examined. We assessed the association between serum thyroid hormone concentration and three WD-HR parameters in hypothyroid subjects.
Methods
Forty-four subjects scheduled for radioactive iodine therapy (RAI Tx) after thyroid cancer surgery were included. Thirty subjects were prepared for RAI Tx by thyroid hormone withdrawal (hypothyroidism group) and 14 subjects by recombinant human thyrotropin (control group). Three WD-HR parameters were calculated from the HR data collected during rest, during sleep, and from 2:00 AM to 6:00 AM, respectively. We analyzed the changes in conventionally measured resting HR (On-site rHR) and WDHR parameters relative to thyroid hormone levels.
Results
Serum free thyroxine (T4) levels, On-site rHR, and WD-HR parameters were lower in the hypothyroid group than in the control group at the time of RAI Tx. WD-HR parameters also reflected minute changes in free T4 levels. A decrease in On-site rHR and WD-HR parameters by one standard deviation (On-site rHR, approximately 12 bpm; WD-HR parameters, approximately 8 bpm) was associated with a 0.2 ng/dL decrease in free T4 levels (P<0.01) and a 2-fold increase of the odds ratio of hypothyroidism (P<0.01). WD-HR parameters displayed a better goodness-of-fit measure (lower quasi-information criterion value) than On-site rHR in predicting the hypothyroidism.
Conclusion
This study identified WD-HR parameters as informative and easy-to-measure biomarkers to predict hypothyroidism. -
Citations
Citations to this article as recorded by- Application of wearables for remote monitoring of oncology patients: A scoping review
Katharina Cloß, Marlo Verket, Dirk Müller-Wieland, Nikolaus Marx, Katharina Schuett, Edgar Jost, Martina Crysandt, Fabian Beier, Tim H Brümmendorf, Guido Kobbe, Julia Brandts, Malte Jacobsen
DIGITAL HEALTH.2024;[Epub] CrossRef - Thyroid hormone action during GABAergic neuron maturation: The quest for mechanisms
Sabine Richard, Juan Ren, Frédéric Flamant
Frontiers in Endocrinology.2023;[Epub] CrossRef - A machine learning-assisted system to predict thyrotoxicosis using patients’ heart rate monitoring data: a retrospective cohort study
Kyubo Shin, Jongchan Kim, Jaemin Park, Tae Jung Oh, Sung Hye Kong, Chang Ho Ahn, Joon Ho Moon, Min Joo Kim, Jae Hoon Moon
Scientific Reports.2023;[Epub] CrossRef
- Application of wearables for remote monitoring of oncology patients: A scoping review

- Thyroid
- The Positive Association between Subclinical Hypothyroidism and Newly-Diagnosed Hypertension Is More Explicit in Female Individuals Younger than 65
- Xichang Wang, Haoyu Wang, Li Yan, Lihui Yang, Yuanming Xue, Jing Yang, Yongli Yao, Xulei Tang, Nanwei Tong, Guixia Wang, Jinan Zhang, Youmin Wang, Jianming Ba, Bing Chen, Jianling Du, Lanjie He, Xiaoyang Lai, Yanbo Li, Zhaoli Yan, Eryuan Liao, Chao Liu, Libin Liu, Guijun Qin, Yingfen Qin, Huibiao Quan, Bingyin Shi, Hui Sun, Zhen Ye, Qiao Zhang, Lihui Zhang, Jun Zhu, Mei Zhu, Yongze Li, Weiping Teng, Zhongyan Shan
- Endocrinol Metab. 2021;36(4):778-789. Published online August 10, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1101
- 5,511 View
- 148 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Subclinical hypothyroidism (SCH) is the most common thyroid dysfunction, and its relationship with blood pressure (BP) has been controversial. The aim of the study was to analyze the association between SCH and newly-diagnosed hypertension.
Methods
Based on data from the Thyroid disease, Iodine nutrition and Diabetes Epidemiology (TIDE) study, 49,433 euthyroid individuals and 7,719 SCH patients aged ≥18 years were enrolled. Patients with a history of hypertension or thyroid disease were excluded. SCH was determined by manufacturer reference range. Overall hypertension and stage 1 and 2 hypertension were diagnosed according to the guidelines issued by the American College of Cardiology/American Heart Association in 2017.
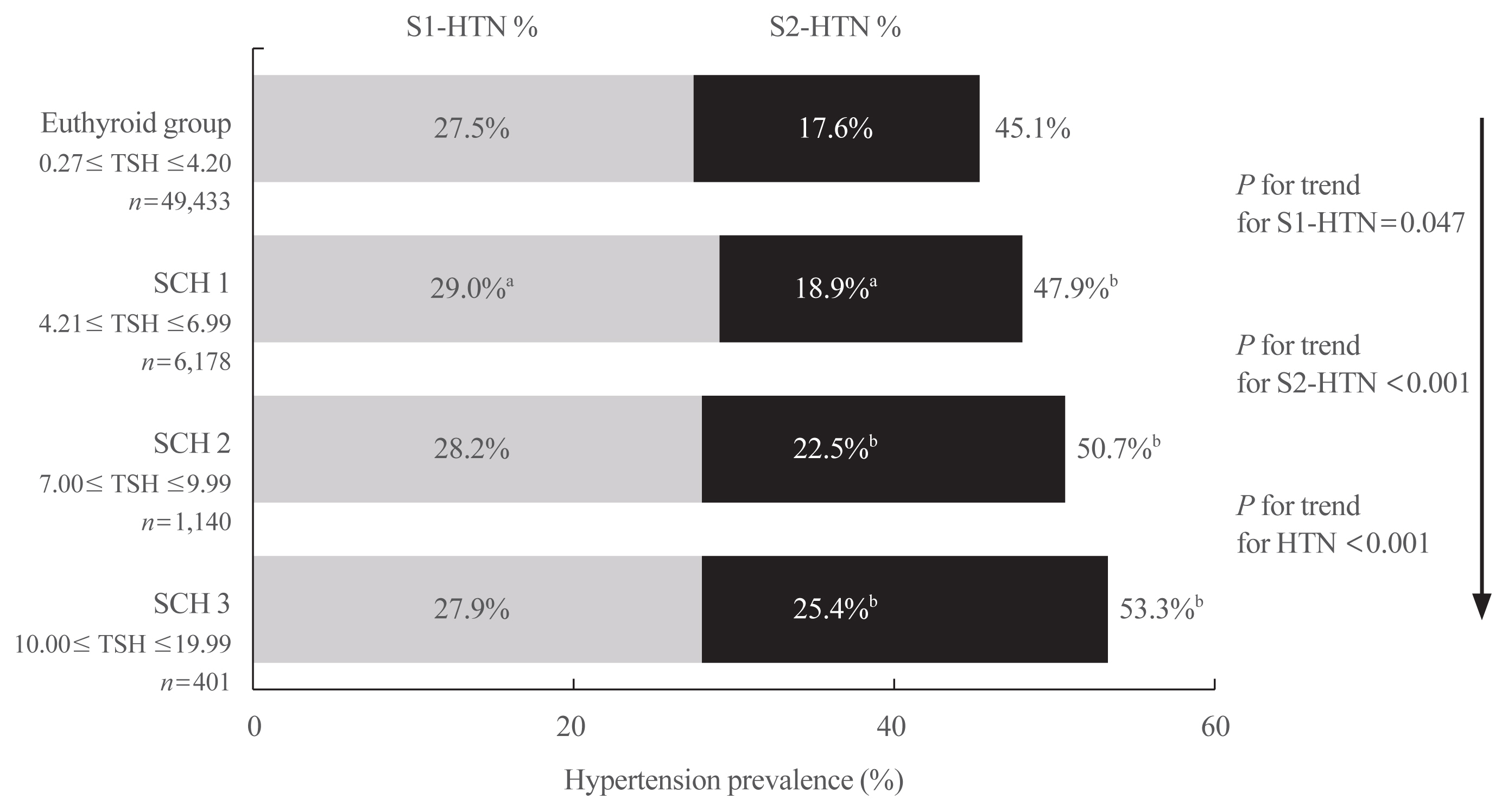
Results
The prevalence of overall hypertension (48.7%), including stage 1 (28.9%) and 2 (19.8%) hypertension, increased significantly in SCH patients compared with euthyroid subjects. With elevated serum thyroid stimulating hormone (TSH) level, the hypertension prevalence also increased significantly from the euthyroid to different SCH subgroups, which was more profound in females or subjects aged <65 years. The age- and sex-specific regression analysis further demonstrated the same trends in the general population and in the 1:1 propensity matched population. Similarly, several BP components (i.e., systolic, diastolic, and mean arterial BP) were positively associated with TSH elevation, and regression analysis also confirmed that all BP components were closely related with SCH in female subjects aged <65 years.
Conclusion
The prevalence of hypertension increases for patients with SCH. SCH tends to be associated with hypertension and BP components in females younger than 65 years. -
Citations
Citations to this article as recorded by- Systematic review and meta-analysis of levothyroxine effect on blood pressure in patients with subclinical hypothyroidism
Bahar Darouei, Reza Amani-Beni, Amir Parsa Abhari, Mohammad Fakhrolmobasheri, Davood Shafie, Maryam Heidarpour
Current Problems in Cardiology.2024; 49(2): 102204. CrossRef - Gender-Specific Associations Between Metabolic Disorders and Thyroid Nodules: A Cross-Sectional Population-Based Study from China
Fan Zhang, Di Teng, Nanwei Tong, Guixia Wang, Yongze Li, Xiaohui Yu, Zhongyan Shan, Weiping Teng
Thyroid.2022; 32(5): 571. CrossRef - Effect of Levothyroxine Supplementation on the Cardiac Morphology and Function in Patients With Subclinical Hypothyroidism: A Systematic Review and Meta-analysis
Xichang Wang, Haoyu Wang, Qiuxian Li, Ping Wang, Yumin Xing, Fan Zhang, Jiashu Li, Zhongyan Shan
The Journal of Clinical Endocrinology & Metabolism.2022; 107(9): 2674. CrossRef
- Systematic review and meta-analysis of levothyroxine effect on blood pressure in patients with subclinical hypothyroidism

Review Articles
- Thyroid
- Subclinical Hypothyroidism: Prevalence, Health Impact, and Treatment Landscape
- Won Sang Yoo, Hyun Kyung Chung
- Endocrinol Metab. 2021;36(3):500-513. Published online June 18, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1066
- 9,028 View
- 544 Download
- 16 Web of Science
- 19 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
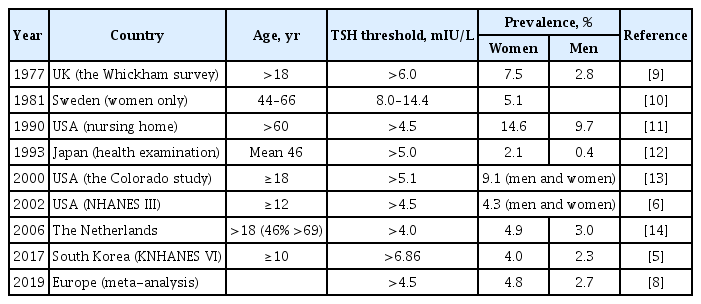
ePub - Subclinical hypothyroidism (sHypo) is defined as normal serum free thyroid hormone levels coexisting with elevated serum thyroid-stimulating hormone (TSH) levels. sHypo is a common condition observed in clinical practice with several unique features. Its diagnosis should be based on an understanding of geographic and demographic differences in biochemical criteria versus a global reference range for TSH that is based on the 95% confidence interval of a healthy population. During the differential diagnosis, it is important to remember that a considerable proportion of sHypo cases are transient and reversible in nature; the focus is better placed on persistent or progressive forms, which mainly result from chronic autoimmune thyroiditis. Despite significant evidence documenting the health impacts of sHypo, the effects of levothyroxine treatment (LT4-Tx) in patients with sHypo remains controversial, especially in patients with grade 1 sHypo and older adults. Existing evidence suggests that it is reasonable to refrain from immediate LT4-Tx in most patients if they are closely monitored, except in women who are pregnant or in progressive cases. Future research is needed to further characterize the risks and benefits of LT4-Tx in different patient cohorts.
-
Citations
Citations to this article as recorded by- THYROID FUNCTION ABNORMALITIES IN PATIENTS WITH CHOLELITHIASIS: A HOSPITAL-BASED CROSS-SECTIONAL STUDY
AVANISH KUMAR SAXENA, ANAM FATIMA, KUNDRAPU VEERA VENKATA SIVA, ANUSHKA PARIYA, VAYALAPALLI SYAMA CHINMAYI
Asian Journal of Pharmaceutical and Clinical Research.2024; : 138. CrossRef - Subclinical hypothyroidism and clinical outcomes after cardiac surgery: A systematic review and meta-analysis
Michele Dell’Aquila, Camilla S. Rossi, Tulio Caldonazo, Gianmarco Cancelli, Lamia Harik, Giovanni J. Soletti, Kevin R. An, Jordan Leith, Hristo Kirov, Mudathir Ibrahim, Michelle Demetres, Arnaldo Dimagli, Mohamed Rahouma, Mario Gaudino
JTCVS Open.2024;[Epub] CrossRef - The Relationship between Subclinical Hypothyroidism and Carotid Intima-Media Thickness as a Potential Marker of Cardiovascular Risk: A Systematic Review and a Meta-Analysis
Oana-Maria Isailă, Victor Eduard Stoian, Iuliu Fulga, Alin-Ionut Piraianu, Sorin Hostiuc
Journal of Cardiovascular Development and Disease.2024; 11(4): 98. CrossRef - Subclinical hypothyroidism, outcomes and management guidelines: a narrative review and update of recent literature
Bogumila Urgatz, Salman Razvi
Current Medical Research and Opinion.2023; 39(3): 351. CrossRef - Indicator of thyroid hormones in newborns from mothers with diffuse-endemic goiter
G. T. Makhkamova, Sh. T. Turdieva
Meditsinskiy sovet = Medical Council.2023; (1): 212. CrossRef - Diagnóstico y tratamiento del hipotiroidismo subclínico en adultos mayores
Debbie Noelia Tebanta Albán, Gabriel Aníbal Hugo Merino, María Valentina Muñoz Arteaga, Ariana Lisseth Vázquez López
Ciencia Digital.2023; 7(1): 6. CrossRef - 2023 Korean Thyroid Association Management Guidelines for Patients with Subclinical Hypothyroidism
Hyun Kyung Chung, Eu Jeong Ku, Won Sang Yoo, Yea Eun Kang, Kyeong Jin Kim, Bo Hyun Kim, Tae-Yong Kim, Young Joo Park, Chang Ho Ahn, Jee Hee Yoon, Eun Kyung Lee, Jong Min Lee, Eui Dal Jung, Jae Hoon Chung, Yun Jae Chung, Won Bae Kim, Ka Hee Yi, Ho-Cheol Ka
International Journal of Thyroidology.2023; 16(1): 32. CrossRef - Gut microbiota short-chain fatty acids and their impact on the host thyroid function and diseases
María José Mendoza-León, Ashutosh K. Mangalam, Alejandro Regaldiz, Enrique González-Madrid, Ma. Andreina Rangel-Ramírez, Oscar Álvarez-Mardonez, Omar P. Vallejos, Constanza Méndez, Susan M. Bueno, Felipe Melo-González, Yorley Duarte, Ma. Cecilia Opazo, Al
Frontiers in Endocrinology.2023;[Epub] CrossRef - Human amnion-derived mesenchymal stem cells improve subclinical hypothyroidism by immunocompetence mediating apoptosis inhibition on thyroid cells in aged mice
Chuyu Li, Qiang Rui, Xiaohan Dong, Song Ning, Jing Zhou, Huimin Wu, Chunyan Jiang, Yugui Cui, Jiayin Liu, Jun Jiang, Lianju Qin
Cell and Tissue Research.2023; 394(2): 309. CrossRef - Is Thyroid Dysfunction Associated with Unruptured Intracranial Aneurysms? A Population-Based, Nested Case–Control Study from Korea
Hyeree Park, Sun Wook Cho, Sung Ho Lee, Kangmin Kim, Hyun-Seung Kang, Jeong Eun Kim, Aesun Shin, Won-Sang Cho
Thyroid®.2023; 33(12): 1483. CrossRef - The Role of Global Longitudinal Strain in Subclinical Hypothyroid Patients With Heart Failure
Nismat Javed, Vibha Hayagreev, Angel DeLaCruz, Muhammad Saad, Amandeep Singh, Timothy Vittorio
Cureus.2023;[Epub] CrossRef - Association between shift work and the risk of hypothyroidism in adult male workers in Korea: a cohort study
Seonghyeon Kwon, Yesung Lee, Eunhye Seo, Daehoon Kim, Jaehong Lee, Youshik Jeong, Jihoon Kim, Jinsook Jeong, Woncheol Lee
Annals of Occupational and Environmental Medicine.2023;[Epub] CrossRef - Estimation of left ventricular functions in patients with subclinical hypothyroidism: a meta-analysis
Binyi Li, Yong Huang, Zheng Li
Frontiers in Endocrinology.2023;[Epub] CrossRef - Comparison of Five Different Criteria for Diagnosis of Subclinical Hypothyroidism in a Large-Scale Chinese Population
Yan-song Zheng, Sheng-yong Dong, Yan Gong, Jia-hong Wang, Fei Wang, Qiang Zeng
Frontiers in Endocrinology.2022;[Epub] CrossRef - Subclinical Hypothyroidism and Cognitive Impairment
Jung-Min Pyun, Young Ho Park, SangYun Kim
Journal of Alzheimer's Disease.2022; 88(2): 757. CrossRef - Effect of Levothyroxine Supplementation on the Cardiac Morphology and Function in Patients With Subclinical Hypothyroidism: A Systematic Review and Meta-analysis
Xichang Wang, Haoyu Wang, Qiuxian Li, Ping Wang, Yumin Xing, Fan Zhang, Jiashu Li, Zhongyan Shan
The Journal of Clinical Endocrinology & Metabolism.2022; 107(9): 2674. CrossRef - Natural history of subclinical hypothyroidism and prognostic factors for the development of overt hypothyroidism: Tehran Thyroid Study (TTS)
A. Amouzegar, M. Dehghani, H. Abdi, L. Mehran, S. Masoumi, F. Azizi
Journal of Endocrinological Investigation.2022; 45(12): 2353. CrossRef - Retrospective cohort analysis comparing changes in blood glucose level and body composition according to changes in thyroid‐stimulating hormone level
Hyunah Kim, Da Young Jung, Seung‐Hwan Lee, Jae‐Hyoung Cho, Hyeon Woo Yim, Hun‐Sung Kim
Journal of Diabetes.2022; 14(9): 620. CrossRef - Long working hours and the risk of hypothyroidism in healthy Korean workers: a cohort study
Yesung Lee, Woncheol Lee, Hyoung-Ryoul Kim
Epidemiology and Health.2022; 44: e2022104. CrossRef
- THYROID FUNCTION ABNORMALITIES IN PATIENTS WITH CHOLELITHIASIS: A HOSPITAL-BASED CROSS-SECTIONAL STUDY

- Miscellaneous
- Clinical Characteristics, Management, and Potential Biomarkers of Endocrine Dysfunction Induced by Immune Checkpoint Inhibitors
- Shintaro Iwama, Tomoko Kobayashi, Hiroshi Arima
- Endocrinol Metab. 2021;36(2):312-321. Published online April 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1007

- 5,404 View
- 265 Download
- 14 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Immune-related adverse events (irAEs) affecting the endocrine glands are among the most frequent irAEs induced by immune checkpoint inhibitors (ICIs) and include hypopituitarism, primary adrenal insufficiency, thyrotoxicosis, hypothyroidism, hypoparathyroidism, and type 1 diabetes mellitus. Since the incidence and clinical features of endocrine irAEs vary according to the ICI used, it is important to understand the characteristics of these irAEs and to manage each one appropriately. Since some endocrine irAEs, including adrenal crisis and diabetic ketoacidosis, are potentially life-threatening, predicting the risk of endocrine irAEs before their onset is critical. Several autoantibodies have been detected in patients who develop endocrine irAEs, among which anti-thyroid antibodies may be predictive biomarkers of thyroid dysfunction. In this review, we describe the clinical features of each endocrine irAE induced by ICIs and discuss their potential biomarkers, including autoantibodies.
-
Citations
Citations to this article as recorded by- Clinical characteristics and potential biomarkers of thyroid and pituitary immune-related adverse events
Tomoko Kobayashi, Shintaro Iwama, Hiroshi Arima
Endocrine Journal.2024; 71(1): 23. CrossRef - A case of rapidly progressive insulin-dependent diabetes mellitus without islet autoantibodies developed over two years after the first dose of nivolumab
Kota Nishihama, Yuko Okano, Chisa Inoue, Kanako Maki, Kazuhito Eguchi, Soichiro Tanaka, Atsuro Takeshita, Mei Uemura, Taro Yasuma, Toshinari Suzuki, Esteban C. Gabazza, Yutaka Yano
Diabetology International.2024;[Epub] CrossRef - Endocrinopathies associated with immune checkpoint inhibitor use
Anupam Kotwal, Randol Kennedy, Nupur Kikani, Sonali Thosani, Whitney Goldner, Afreen Shariff
Endocrine Practice.2024;[Epub] CrossRef - Recovery from insulin dependence in immune checkpoint inhibitor‐associated diabetes mellitus: A case report
Marie Okubo, Yuji Hataya, Kanta Fujimoto, Toshio Iwakura, Naoki Matsuoka
Journal of Diabetes Investigation.2023; 14(1): 147. CrossRef - Case Report: A Rising Cause of New-Onset Endocrinopathies After Immunotherapy
Charity Tan, Sarah Hendricks, Kristina Hernandez, Martha Benavides, Rupinderjit Samra
The Journal for Nurse Practitioners.2023; 19(5): 104582. CrossRef - Risk of Thyroid Dysfunction in PD-1 Blockade Is Stratified by the Pattern of TgAb and TPOAb Positivity at Baseline
Xin Zhou, Shintaro Iwama, Tomoko Kobayashi, Masahiko Ando, Hiroshi Arima
The Journal of Clinical Endocrinology & Metabolism.2023; 108(10): e1056. CrossRef - Severe thyrotoxicosis induced by tislelizumab: a case report and literature review
Liman Huo, Chao Wang, Haixia Ding, Xuelian Shi, Bin Shan, Ruoying Zhou, Ping Liang, Juan Hou
Frontiers in Oncology.2023;[Epub] CrossRef - Life-Threatening Endocrinological Immune-Related Adverse Events of Immune Checkpoint Inhibitor Therapy
Aleksandra Basek, Grzegorz K. Jakubiak, Grzegorz Cieślar, Agata Stanek
Cancers.2023; 15(24): 5786. CrossRef - Increased Risk of Thyroid Dysfunction by PD-1 and CTLA-4 Blockade in Patients Without Thyroid Autoantibodies at Baseline
Shintaro Iwama, Tomoko Kobayashi, Yoshinori Yasuda, Takayuki Okuji, Masaaki Ito, Masahiko Ando, Xin Zhou, Ayana Yamagami, Takeshi Onoue, Yohei Kawaguchi, Takashi Miyata, Mariko Sugiyama, Hiroshi Takagi, Daisuke Hagiwara, Hidetaka Suga, Ryoichi Banno, Tets
The Journal of Clinical Endocrinology & Metabolism.2022; 107(4): e1620. CrossRef - Biomarkers and risk factors for the early prediction of immune-related adverse events: a review
Ying Zhang, Xiaoling Zhang, Weiling Li, Yunyi Du, Wenqing Hu, Jun Zhao
Human Vaccines & Immunotherapeutics.2022;[Epub] CrossRef - Immune Checkpoint Inhibitors as a Threat to the Hypothalamus–Pituitary Axis: A Completed Puzzle
Agnese Barnabei, Andrea Corsello, Rosa Maria Paragliola, Giovanni Maria Iannantuono, Luca Falzone, Salvatore Maria Corsello, Francesco Torino
Cancers.2022; 14(4): 1057. CrossRef - Elevated TSH Level, TgAb, and Prior Use of Ramucirumab or TKIs as Risk Factors for Thyroid Dysfunction in PD-L1 Blockade
Tomoko Kobayashi, Shintaro Iwama, Ayana Yamagami, Yoshinori Yasuda, Takayuki Okuji, Masaaki Ito, Xin Zhou, Masahiko Ando, Takeshi Onoue, Takashi Miyata, Mariko Sugiyama, Daisuke Hagiwara, Hidetaka Suga, Ryoichi Banno, Tetsunari Hase, Masahiro Morise, Taka
The Journal of Clinical Endocrinology & Metabolism.2022; 107(10): e4115. CrossRef - Preconditioning of the immune system modulates the response of papillary thyroid cancer to immune checkpoint inhibitors
Fabiana Pani, Yoshinori Yasuda, Sylvie T Rousseau, Kevin C Bermea, Solmaz Roshanmehr, Rulin Wang, Srinivasan Yegnasubramanian, Patrizio Caturegli, Luigi Adamo
Journal for ImmunoTherapy of Cancer.2022; 10(12): e005538. CrossRef - Survival benefit of endocrine dysfunction following immune checkpoint inhibitors for nonthyroidal cancers
Anupam Kotwal, Mabel Ryder
Current Opinion in Endocrinology, Diabetes & Obesity.2021; 28(5): 517. CrossRef
- Clinical characteristics and potential biomarkers of thyroid and pituitary immune-related adverse events

Original Articles
- Clinical Study
- Characteristics of Immune-Related Thyroid Adverse Events in Patients Treated with PD-1/PD-L1 Inhibitors
- Jee Hee Yoon, A Ram Hong, Hee Kyung Kim, Ho-Cheol Kang
- Endocrinol Metab. 2021;36(2):413-423. Published online April 6, 2021
- DOI: https://doi.org/10.3803/EnM.2020.906

- 5,557 View
- 216 Download
- 22 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Thyroid immune-related adverse events (IRAEs) have been reported in patients treated with programmed cell death protein-1 (PD-1) and programmed cell death protein-ligand 1 (PD-L1) inhibitors. We investigated the incidence and clinical course of PD-1/PD-L1 inhibitor-induced thyroid IRAEs, and identified predictable clinical risk factors of thyroid IRAEs, in particular, overt hypothyroidism (OH).
Methods
We retrospectively reviewed the medical records of 325 cancer patients receiving PD-1/PD-L1 inhibitor in a tertiary referral center.
Results
A total of 50.5% (164/325) of patients experienced at least one abnormal thyroid function following PD-1/PD-L1 inhibitor. Eighty-four patients (51.2%) of them recovered to normal thyroid function during follow-up. In overall population, 25 patients (7.7%) required thyroid hormone replacement therapy due to PD-1/PD-L1 inhibitor-induced OH. Patients who progressed to OH showed significantly higher baseline thyroid stimulating hormone level and longer duration of PD-1/PD-L1 inhibitor therapy than those without thyroid dysfunction or OH (both P<0.001). Median time interval to the development of OH was 3 months after the therapy. OH was significantly associated with positive anti-thyroid peroxidase antibody at baseline and anti-thyroglobulin antibody during the therapy than those without thyroid dysfunction or OH (P=0.015 and P=0.005, respectively). We observed no patients with OH who were able to stop levothyroxine replacement after the cessation of PD-1/PD-L1 inhibitor therapy.
Conclusion
PD-1/PD-L1 inhibitor-induced thyroid dysfunctions are considerably reversible; however, OH is irreversible requiring levothyroxine replacement even after stopping the therapy. Positive thyroid autoantibodies may predict the progression to OH. -
Citations
Citations to this article as recorded by- Thyroid Dysfunction after Atezolizumab and Bevacizumab Is Associated with Favorable Outcomes in Hepatocellular Carcinoma
Young Shin Song, Hannah Yang, Beodeul Kang, Jaekyung Cheon, Ilhwan Kim, Hyeyeong Kim, Won Suk Lee, Yun Beom Sang, Sanghoon Jung, Ho Yeong Lim, Vincent E. Gaillard, Chan Kim, Hong Jae Chon
Liver Cancer.2024; 13(1): 89. CrossRef - Thyroid dysfunction (TD) induced by PD-1/PD-L1 inhibitors in advanced lung cancer
Yanling Wang, Xiaoxuan Yang, Jia Ma, Shenglan Chen, Ping Gong, Ping Dai
Heliyon.2024; 10(5): e27077. CrossRef - Non-Invasive Predictive Biomarkers for Immune-Related Adverse Events Due to Immune Checkpoint Inhibitors
Ben Ponvilawan, Abdul Wali Khan, Janakiraman Subramanian, Dhruv Bansal
Cancers.2024; 16(6): 1225. CrossRef - Implication of the Gut Microbiome and Microbial-Derived Metabolites in Immune-Related Adverse Events: Emergence of Novel Biomarkers for Cancer Immunotherapy
David Dora, Syeda Mahak Zahra Bokhari, Kenan Aloss, Peter Takacs, Juliane Zsuzsanna Desnoix, György Szklenárik, Patrick Deniz Hurley, Zoltan Lohinai
International Journal of Molecular Sciences.2023; 24(3): 2769. CrossRef - Immune checkpoint inhibitor-associated toxicity in advanced non-small cell lung cancer: An updated understanding of risk factors
Xiangxiao Hu, Lina Wang, Bin Shang, Junren Wang, Jian Sun, Bin Liang, Lili Su, Wenjie You, Shujuan Jiang
Frontiers in Immunology.2023;[Epub] CrossRef - Immune-related adverse events induced by programmed death protein-1 inhibitors from the perspective of lymphoma immunotherapy
Yong-Zhe Hou, Qin Zhang, Hai Bai, Tao Wu, Ya-Jie Chen
World Journal of Clinical Cases.2023; 11(7): 1458. CrossRef - Predictive Biomarkers for Checkpoint Inhibitor Immune-Related Adverse Events
Iñigo Les, Mireia Martínez, Inés Pérez-Francisco, María Cabero, Lucía Teijeira, Virginia Arrazubi, Nuria Torrego, Ana Campillo-Calatayud, Iñaki Elejalde, Grazyna Kochan, David Escors
Cancers.2023; 15(5): 1629. CrossRef - Immune-related thyroid dysfunctions during anti PD-1/PD-L1 inhibitors: new evidence from a single centre experience
Alice Nervo, Matteo Ferrari, Giovanni Gruosso, Enrica Migliore, Sara Basile, Valentina D’Angelo, Anna Roux, Alessandro Piovesan, Emanuela Arvat
Clinical and Experimental Medicine.2023; 23(8): 4817. CrossRef - RNA Sequencing Reveals Unique Transcriptomic Signatures of the Thyroid in a Murine Lung Cancer Model Treated with PD-1 and PD-L1 Antibodies
Rena Pollack, Joshua Stokar, Natan Lishinsky, Irina Gurt, Naomi Kaisar-Iluz, Merav E. Shaul, Zvi G. Fridlender, Rivka Dresner-Pollak
International Journal of Molecular Sciences.2023; 24(13): 10526. CrossRef - Immune‐related adverse events after immune check point inhibitors: Understanding the intersection with autoimmunity
Namrata Singh, Anne M. Hocking, Jane H. Buckner
Immunological Reviews.2023; 318(1): 81. CrossRef - Endocrine Side Effects in Patients Treated with Immune Checkpoint Inhibitors: A Narrative Review
Nicia I. Profili, Roberto Castelli, Antonio Gidaro, Alessandro Merella, Roberto Manetti, Giuseppe Palmieri, Margherita Maioli, Alessandro P. Delitala
Journal of Clinical Medicine.2023; 12(15): 5161. CrossRef - Incidence of Endocrine-Related Dysfunction in Patients Treated with New Immune Checkpoint Inhibitors: A Meta-Analysis and Comprehensive Review
Won Sang Yoo, Eu Jeong Ku, Eun Kyung Lee, Hwa Young Ahn
Endocrinology and Metabolism.2023; 38(6): 750. CrossRef - PD-1/PD-L1 Inhibitors in Patients With Preexisting Autoimmune Diseases
Ke Zhang, Xiangyi Kong, Yuan Li, Zhongzhao Wang, Lin Zhang, Lixue Xuan
Frontiers in Pharmacology.2022;[Epub] CrossRef - Association between the type of thyroid dysfunction induced by immune checkpoint inhibitors and prognosis in cancer patients
Han-sang Baek, Chaiho Jeong, Kabsoo Shin, Jaejun Lee, Heysun Suh, Dong-Jun Lim, Moo Il Kang, Jeonghoon Ha
BMC Endocrine Disorders.2022;[Epub] CrossRef - A Successful Case of Hepatocellular Carcinoma Treated with Atezolizumab Plus Bevacizumab with Multisystem Immune-related Adverse Events
Hidemi Hayashi, Koji Sawada, Takumu Hasebe, Shunsuke Nakajima, Jun Sawada, Yuri Takiyama, Yumi Takiyama, Toshikatsu Okumura, Mikihiro Fujiya
Internal Medicine.2022; 61(23): 3497. CrossRef - Immune Related Adverse Events of the Thyroid – A Narrative Review
Christopher A. Muir, Venessa H. M. Tsang, Alexander M. Menzies, Roderick J. Clifton-Bligh
Frontiers in Endocrinology.2022;[Epub] CrossRef - Thyroid-related adverse events induced by immune checkpoint inhibitors
Alexandra Chera, Andreea Lucia Stancu, Octavian Bucur
Frontiers in Endocrinology.2022;[Epub] CrossRef - Risk Factors and Biomarkers for Immune-Related Adverse Events: A Practical Guide to Identifying High-Risk Patients and Rechallenging Immune Checkpoint Inhibitors
Adithya Chennamadhavuni, Laith Abushahin, Ning Jin, Carolyn J. Presley, Ashish Manne
Frontiers in Immunology.2022;[Epub] CrossRef - Case 5: A 41-Year-Old Woman With Palpitation
Jiwon Yang, Kabsoo Shin, Jeongmin Lee, Jeonghoon Ha, Dong-Jun Lim, Han-Sang Baek
Journal of Korean Medical Science.2022;[Epub] CrossRef - Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim
Endocrinology and Metabolism.2022; 37(6): 839. CrossRef - Management of Endocrine and Metabolic Toxicities of Immune-Checkpoint Inhibitors: From Clinical Studies to a Real-Life Scenario
Calogera Claudia Spagnolo, Giuseppe Giuffrida, Salvatore Cannavò, Tindara Franchina, Nicola Silvestris, Rosaria Maddalena Ruggeri, Mariacarmela Santarpia
Cancers.2022; 15(1): 246. CrossRef - Antineoplastics
Reactions Weekly.2021; 1874(1): 31. CrossRef
- Thyroid Dysfunction after Atezolizumab and Bevacizumab Is Associated with Favorable Outcomes in Hepatocellular Carcinoma

- Clinical Study
- Subclinical Hypothyroidism Affects the Long-Term Outcomes of Patients Who Undergo Coronary Artery Bypass Grafting Surgery but Not Heart Valve Surgery
- Hana Kim, Sung Hye Kong, Jae Hoon Moon, Sang Yoon Kim, Kay-Hyun Park, Jun Sung Kim, Joong Haeng Choh, Young Joo Park, Cheong Lim
- Endocrinol Metab. 2020;35(2):308-318. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.308

- 6,460 View
- 151 Download
- 9 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
The aim of this study was to determine the associations between subclinical hypothyroidism (SCH) and long-term cardiovascular outcomes after coronary artery bypass grafting (CABG) or heart valve surgery (HVS).
Methods
We retrospectively reviewed and compared all-cause mortality, cardiovascular mortality, and cardiovascular events in 461 patients who underwent CABG and 104 patients who underwent HVS.
Results
During a mean±standard deviation follow-up duration of 7.6±3.8 years, there were 187 all-cause deaths, 97 cardiovascular deaths, 127 major adverse cardiovascular events (MACE), 11 myocardial infarctions, one unstable angina, 70 strokes, 30 hospitalizations due to heart failure, 101 atrial fibrillation, and 33 coronary revascularizations. The incidence of all-cause mortality after CABG was significantly higher in patients with SCH (n=36, 55.4%) than in euthyroid patients (n=120, 30.3%), with a hazard ratio of 1.70 (95% confidence interval, 1.10 to 2.63; P=0.018) after adjustment for age, sex, current smoking status, body mass index, underlying diseases, left ventricular dysfunction, and emergency operation. Interestingly, low total triiodothyronine (T3) levels in euthyroid patients who underwent CABG were significantly associated with increased risks of all-cause mortality, cardiovascular mortality, and MACE, but those associations were not observed in HVS patients. Both free thyroxine and thyroid-stimulating hormone levels in euthyroid patients were not related with any cardiovascular outcomes in either the CABG or HVS group.
Conclusion
SCH or low total T3 might be associated with a poor prognosis after CABG, but not after HVS, implying that preoperative thyroid hormonal status may be important in ischemic heart disease patients. -
Citations
Citations to this article as recorded by- Subclinical hypothyroidism and clinical outcomes after cardiac surgery: A systematic review and meta-analysis
Michele Dell’Aquila, Camilla S. Rossi, Tulio Caldonazo, Gianmarco Cancelli, Lamia Harik, Giovanni J. Soletti, Kevin R. An, Jordan Leith, Hristo Kirov, Mudathir Ibrahim, Michelle Demetres, Arnaldo Dimagli, Mohamed Rahouma, Mario Gaudino
JTCVS Open.2024; 18: 64. CrossRef - The Association Between Hypothyroidism Treatment and Mortality in Patients Hospitalized in Surgical Wards
Hiba Masri-Iraqi, Yaron Rudman, Carmel Friedrich Dubinchik, Idit Dotan, Talia Diker-Cohen, Liat Sasson, Tzipora Shochat, Ilan Shimon, Eyal Robenshtok, Amit Akirov
Endocrine Research.2023; 48(2-3): 68. CrossRef - Mid-term outcomes of patients with subclinical hypothyroidism after coronary bypass surgery
Dong Zhao, Wei Zhao, Chuangshi Wang, Fei Xu, Wei Zhao, Xieraili Tiemuerniyazi, Hao Ma, Wei Feng
Interdisciplinary CardioVascular and Thoracic Surgery.2023;[Epub] CrossRef - Thyroid Pathology in High-Risk Cardiac Surgery Patients with Coronary Artery Disease
Olena K. Gogayeva, Anatoliy V. Rudenko, Vasyl V. Lazoryshynets, Serhii A. Rudenko, Tetiana A. Andrushchenko
Ukrainian Journal of Cardiovascular Surgery.2022; 30(1 (46)): 9. CrossRef - High-TSH Subclinical Hypothyroidism Is Associated With Postoperative Mortality in Acute Type A Aortic Dissection
Shi-Pan Wang, Yuan Xue, Hai-Yang Li, Wen-Jian Jiang, Hong-Jia Zhang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Triiodothyronine improves contractile recovery of human atrial trabeculae after hypoxia/reoxygenation
Petra Kleinbongard, Philipp Kuthan, Chantal Eickelmann, Philipp Jakobs, Joachim Altschmied, Judith Haendeler, Arjang Ruhparwar, Matthias Thielmann, Gerd Heusch
International Journal of Cardiology.2022; 363: 159. CrossRef - Hypothyroidism Is Correlated with Ventilator Complications and Longer Hospital Days after Coronary Artery Bypass Grafting Surgery in a Relatively Young Population: A Nationwide, Population-Based Study
Jiun-Yu Lin, Pei-Chi Kao, Yi-Ting Tsai, Chi-Hsiang Chung, Wu-Chien Chien, Chih-Yuan Lin, Chieh-Hua Lu, Chien-Sung Tsai
Journal of Clinical Medicine.2022; 11(13): 3881. CrossRef - Minor perturbations of thyroid homeostasis and major cardiovascular endpoints—Physiological mechanisms and clinical evidence
Patrick Müller, Melvin Khee-Shing Leow, Johannes W. Dietrich
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Subclinical Hypothyroidism: Prevalence, Health Impact, and Treatment Landscape
Won Sang Yoo, Hyun Kyung Chung
Endocrinology and Metabolism.2021; 36(3): 500. CrossRef
- Subclinical hypothyroidism and clinical outcomes after cardiac surgery: A systematic review and meta-analysis

Case Report
- A Case of Pituitary Feedback Adenoma Caused by Primary Hypothyroidism.
- Soon Jib Yoo, Sang A Chang, Yoo Bae Ahn, Hyun Sik Son, Kun Ho Yoon, Moo Il Kang, Bong Yun Cha, Kwang Woo Lee, Ho Young Son, Sung Koo Kang, Myung Hee Chung
- J Korean Endocr Soc. 1996;11(2):199-206. Published online November 7, 2019
- 1,147 View
- 29 Download
-
 Abstract
Abstract
 PDF
PDF - A 14-year-old girl presented with severe headache and grand mal seizure. A magnetic resonance imaging(MRI) of brain showed a pituitary mass(1.0X1.5X1.3cm) incidentally during seizure evaluation. On physical examination, nodular goiter was detected on her anterior neck. The hormone study showed markdly increased basal thyroid stimulating hormone(TSH) level compared to thyroid hormone level, hyperprolactinemia and decreased basal growth hormone level. TSH and prolactin showed exaggerated response to thyrotropin releasing hormone(TRH) and the growth hormone showed delayed and blunted response to insulin-induced hypoglycemia. With the results of thyroid autoantibody and thyroid scan, the diagnosis of Hashimoto's thyroiditis was possible. Thyroid hormone and anticonvulsant drug were started with close observation of clinical status under the impression of pituitary feedback adenoma caused by hypothyroidism. After 3 months replacement therapy of levothyroxine sodium, she achieved euthyroid state with disappearance of headache and nodular goiter. After continuous replacement therapy for 9 months more, the pituitary mass was successfully regressed on follow up MRI with normalization of basal prolactin level. Grand mal seizure was developed after withholding anticonvulsant drug even though continuous admmistration of thyroid hormone. Because of similarity among pituitary adenoma discovered incidentally, careful hormonal study and high index of suspicion should be maintained to achieve correct diagnosis in order to avoid unnecessary pituitary surgery in these patients.

Original Articles
- Serum Insulin-like Growth Factor-1(IGF-1) and Insulin-like Growth Factor Binding Proteins in Hyperthyroidism and Hypothyroidism.
- Hyun Mo Song, Sang Seok Park, Tae Seon Park, Hong Sun Baek, Dae Yeol Lee
- J Korean Endocr Soc. 1996;11(1):52-60. Published online November 7, 2019
- 1,128 View
- 30 Download
-
 Abstract
Abstract
 PDF
PDF - Background
s: Thyroid hormones play a fundamental role in the initiation and maintenance of somatic growth in mammalian species, and the insulin-like growth factors(IGFs) occupy a position of central importance in the growth of all tissues. To evaluate the changes in serum insulin-like growth factor-I(IGF-I) and insulin-like growth factor binding proteins in hyperthyroid and hypothyroid patients, sera was obtained from 19 hyperthyroid patients, 9 hypothyroid patients, and 10 healthy volunteers. Methods: IGF-I concentration was determined by radioimmunoassay, and changes in IGFBPs were assesed by Western Ligand Blotting. To evaluate the binding pattern of IGF-I & IGFBPs, autoradiographs were obtained. Results & Conclusion: IGF-I levels were increased significantly in hyperthyroid patients(mean ±SE, 267.88±9.80 ng/ml, p<0.05) and decreased significantly in hypothyroid patients(154.81±1.43 ng/ml, p<0.01) compaired to healthy control group(209.45±.60 ng/ml). Autoradiograph of serum IGFBPs from patients with hyperthyroidism and hypothyroidism did not show any change in the intensity of IGFBP-3 bands(40-45 KD) and IGFBP-1 bands, but in hyperthyroid patients, it showed increased intensity of IGFBP-2 band compared to healthy control group and hypothyroid patients.

- Changes in Serum Lipids and Apolipoproteins Levels According to the Thyroxine Treatment in The Patients with Subclinical Hypothyroidism.
- Hye Young Park, Bo Youn Cho, Won Bae Kim, Hong Gyu Lee, Chang Soon Koh, Geon Sang Park, Hyung Kyu Park, Sook Kyung Kim, Chan Soo Shin, Seong Yeon Kim
- J Korean Endocr Soc. 1996;11(1):41-51. Published online November 7, 2019
- 1,211 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Subclinical hypothyroidism(SCH) is a common biochemical abnormality which can be found in routine screening tests of thyroid function. We are increasingly faced with the question of whether its an indication for thyroxine replacement therapy. The effect of thyroxine replacement on lipid profile in SCH has aroused a great interest because of an association of overt hypothyroidism(OVH) with hyperlipidemia and increased risk of coronary artery disease. Method: We prospectively evaluated the changes in lipids and apoproteins before and after thyroxine replacement therapy in 23 patients with SCH and in 37 patients with OVH. We measured serum total cholesterol and triglyceride using autoanalyzer, high density lipoprotein(HDL) chole-sterol by dextran sulfate method, Apo A1 and Apo B by immunonephelometric assay. Results: Thyroxine replacement therapy significantly decreased total cholesterol, low density lipoprotein(LDL) cholesterol and apo B levels, but did not affect the level of triglyceride, HDL cholesterol or apo AI in patients with OVH. In SCH, thyroxine replacement therapy with the doses to normalize serum TSH concentrations also decreased significantly the level of cholesterol and LDL cholesterol albeit apo B levels did not change. Moreover, in most of patients with OVH (11 of 12) and in all of patients with SCH(5 of 5) who had had hyperchlesterolemia before treatment, thyroxine replament normalized their cholesterol and LDL cholesterol levels. Conclusion: In regard to the beneficial changes in blood lipid levels, patients with SCH should be treated, especially in cases who have other risk factors for the development of atherosclerosis. If thyroxine replacement only will reduce the incidence of coronary artery disease in SCH remains to be elucidated by long-term prospective studies.

- Spontaneous Recovery from Hypothyroidism in Autommune Thyroiditis.
- Bo Youn Cho, Jae Hoon Chung, Kwang Won Kim, Kyu Jeung Ahn, Yong Ki Min, Myung Shik Lee, Moon Kyu Lee
- J Korean Endocr Soc. 1996;11(1):30-40. Published online November 7, 2019
- 2,178 View
- 34 Download
-
 Abstract
Abstract
 PDF
PDF - Background
A lifelong thyroxine therapy is indicated in all patients who have hypothyroidism as a result of autoimmune thyroiditis. However, it has been reported that some hypothyroid patients with autoimmune thyroiditis have spontaneous remission with restriction of iodine intake instead of thyroxine therapy. The purpose of study was to investigate how many hypothyroid patients with autoimmune thyroiditis can recover from hypothyroidism with restriction of iodine intake instead of thyroxine therapy and which factors predict recovery from hypothyroidism. Methods: We studied 64 patients with autoimmune thyroiditis(goitrous autoimmune thyroiditis 56, atrophic autoimmune thyroiditis 8). Thyroxine therapy was discontinued in patients with goitrous autoimmune thyroiditis on the way(group 1, n=32) or from the beginning(group 2, n=24) and atrophic autoimmune thyroiditis on the way(group 3, n-8). All patients were asked to avoid iodine-rich foods and thyroid function was monitored every one to two months for up to 35 months. Serum T3, T4, TSH concentrations, antithyroglobulin and antimicrosomal antibodies were measured by radioimmunoassay(RIA). TSH binding inhibitor immunoglobulin(TBII) was measured in serum using radioreceptor assay. Two hundred micrograms of thyrotropin releasing hormone (TRH) were given as intravenous bolus and TSH levels were measured in blood samples taken at 0, 30, and 60 minutes. All values were expressed as mean+-SEM. Statistical analysis was done with paired or non-paired t-test, ANOVA, and the Chi-square test. Statistical significance was defined as p-value below 0.05. Results: Thirteen(40.6%) of 32 patients in group 1 remained euthyroid after 12-35 months of discontinuation of thyroxine therapy. The other 19(59.4%) patients in group 1 had recurrences of hypothyroidism within 3 months after discontinuation of thyroxine therapy. In 11(45.8%) out of 24 patients in group 2, serum TSH concentrations declined below 5 mU/L within 3 months without thyroxine therapy. The other 13(54.2%) patients in group 2 remained hypothyroid till 2-16 months and the thyroxine was given. In contrast, all 8 patients in group 3 had recurrences of hypothy- roidism within 3 months after stopping thyroxine therapy. When we compared the recovered patients of goitrous autoimmune thyroiditis with the non-recovered patients of goitrous autoimmune thyroiditis, regardless of thyroxine therapy from the beginning, age at onset of disease of the 24 recovered patients was significantly younger than the 32 non-recovered patients(30.1+2.0 years vs. 40.2+ 2.4 years; p=0.004). Concl#usion: These findings suggest that 42.9% of hypothyroid patients with goitrous autoim- mune thyroiditis remain or become spontaneously euthyroid with restriction of iodine intake instead of thyroxine therapy. Young age may be a predicting factor of recovery from hypothyroidism in goitrous autoimmune thyroiditis.

Case Report
- A Case of Subclinical Hypothyroidism Associated with Turner's Syndrome.
- In Kwon Han, Jung Gil Lee, Sun Wha Lee, Seong Kyu Lee, Chan Moon Pak, Ho Yeon Chung
- J Korean Endocr Soc. 1994;9(1):35-38. Published online November 6, 2019
- 1,242 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - Recently it is known that Turner's syndrome is frequently associated with hypothyroidism. We report a case of Turner's syndrome associated with subclinical hypothyroidism. A 23-year-old female was admitted to the hospital with complaints of amenorrhea and short stature. She had a mosaicism of 45, X0/46, Xi(X_q) in the cell, cultured from the peripheral blood. The plasma thyroxine and triiodothyronine were normal and there was no clinical symptom of hypothyroidism. But the thyroid-stimulating hormone(TSH) concentration was unusually higher(184 uU/L). She has been treated with the cyclic therapy of conjugated estrogen and medroxyprogesterone, in addition to the thyroxine replacement therapy. After 2 months, the menstruation was restored and TSH was normalized.


 KES
KES

 First
First Prev
Prev



