The Frequency and Clinical Implications of the BRAFV600E Mutation in Papillary Thyroid Cancer Patients in Korea Over the Past Two Decades
Article information
Abstract
Background
Over the past several decades, there has been a rapid worldwide increase in the prevalence of papillary thyroid cancer (PTC) as well as a number of changes in the clinicopathological characteristics of this disease. BRAFV600E, which is a mutation of the proto-oncogene BRAF, has become the most frequent genetic mutation associated with PTC, particularly in Korea. Thus, the present study investigated whether the prevalence of the BRAFV600E mutation has increased over the past two decades in the Korean population and whether various PTC-related clinicopathological characteristics have changed.
Methods
The present study included 2,624 patients who underwent a thyroidectomy for PTC during two preselected periods; 1995 to 2003 and 2009 to 2012. The BRAFV600E mutation status of each patient was confirmed using the polymerase chain reaction-restriction fragment length polymorphism method or by the direct sequencing of DNA.
Results
The prevalence of the BRAFV600E mutation in Korean PTC patients increased from 62.2% to 73.7% (P=0.001) over the last two decades. Additionally, there was a greater degree of extrathyroidal extension (ETE) and lymph node metastasis in 2009 to 2012 patients with the BRAFV600E mutation and a higher frequency of thyroiditis and follicular variant-PTC in 2009 to 2012 patients with wild-type BRAF. However, only the frequency of ETE was significantly higher in 1995 to 2003 patients with the BRAFV600E mutation (P=0.047). Long-term recurrence rates during a 10-year median follow-up did not differ based on BRAFV600E mutation status.
Conclusion
The BRAFV600E mutation rate in Korean PTC patients has been persistently high (approximately 70%) over the past two decades and continues to increase. The present findings demonstrate that BRAFV600E-positive PTC was associated with more aggressive clinicopathological features, especially in patients who were recently diagnosed, suggesting that BRAFV600E mutation status may be a useful prognostic factor for PTC in patients recently diagnosed with this disease.
INTRODUCTION
Papillary thyroid cancer (PTC) is the most commonly occurring malignancy in the endocrine system and the incidence rate of this disease is increasing annually worldwide [1,2]. In particular, there has been a significant rise in the incidence of PTCs smaller than 1 cm, which are termed papillary thyroid microcarcinomas (PTMCs) [3]. To date, there is no clear explanation for the overall increase of PTCs. However, because the rate of PTCs with more aggressive pathological characteristics, such as lymph node metastasis (LNM) and extrathyroidal extension (ETE), has decreased over time, the overall increase in the occurrence of PTCs has primarily been attributed to advanced screening techniques and the early detection of cancer [4,5,6,7]. In contrast, the prevalence of distant metastases has increased, which indicates that improved detection capabilities may not be sufficient to explain the rising incidence of PTC [5,8]. These findings suggest that other causal factors such as environmental, hormonal, or genetic influences may also be associated with PTC [9,10,11,12].
The BRAFV600E mutation, which occurs in approximately 36% to 69% of PTC tumors, is the most common mutation observed in PTC patients [13,14,15]. This genetic mutation changes valine to glutamate in codon 600 of the BRAF protein, which produces the BRAFV600E protein that activates serine/threonine tyrosine kinase and its downstream protein kinase signaling pathway resulting in oncogenesis [16]. The BRAFV600E mutation is associated with poor prognostic factors of PTC including old age, LNM, ETE, loss of radioactive iodine (RAI) uptake, distant metastasis, and disease recurrence [14,16].
There is a greater incidence of PTC in Korea than in other countries and it continues to rapidly increase. The prevalence of PTC has risen from 88.1% to 91.5% of all thyroid cancers over the past 40 years and this increase is accompanied by changes in the clinicopathological characteristics of these tumors [17]. The prevalence of BRAFV600E in Korean PTC patients (81%) is also higher than in other countries (58%) suggesting that this mutation is associated with a greater possibility for pathophysiological characteristics [18,19,20]. However, it is unclear whether the frequency of the BRAFV600E mutation has changed over time. Thus, changes in the prevalence of the BRAFV600E mutation over the last two decades were retrospectively investigated using a relatively large cohort of Korean PTC patients and the association of these rates with the clinicohistopathological characteristics of PTC were also evaluated. Additionally, the association between the presence of the BRAFV600E mutation and the long-term clinical outcomes of PTC patients was assessed.
METHODS
Study subjects
This was a retrospective study conducted at Seoul National University Hospital in which the records of 2,624 patients who underwent thyroidectomy for PTC were retrospectively reviewed. Of these patients, 193 underwent surgery between April 1995 and June 2003 and 2,431 underwent surgery between February 2009 and August 2012. Four patients were diagnosed with PTC combined with follicular thyroid carcinoma and three patients were diagnosed with PTC combined with poorly differentiated carcinoma. The BRAFV600E mutation status of each patient was determined following surgical treatment in all cases and did not affect the postoperative treatment plan.
All medical records, pathological reports, and clinical outcomes were assessed via a review of the patient databases. The present study aimed to identify any correlations between sex, age, tumor size, LNM, multiplicity, thyroiditis, follicular variant (FV)-PTC, ETE, family history of thyroid cancer, and the pathological characteristics of the cancer. This study was approved by the Institutional Review Board (IRB No. 1207-124-420).
Treatment and follow-up
All patients were treated with one of three types of surgical resection: total thyroidectomy, subtotal thyroidectomy, or lobectomy. Therapeutic neck dissections were conducted for standard indications, and empirical central or anterior lymph node dissections have been performed since 2003. Postoperative treatment included conventional thyroid stimulating hormone suppression and RAI (131I) ablation. The ablation was conducted in patients with LNM, ETE, or distant metastasis until no further iodine uptake was detected on a postablation whole body scan (WBS). The dose of RAI depended on the individual pathological characteristics of the PTC. In patients with favorable pathological characteristics, 30 mCi of RAI was administered whereas a higher dose of RAI (100 to 200 mCi) was used for patients with aggressive pathological characteristics.
The follow-up period was defined as the time from the initial surgical treatment to the most recent clinical visit or death from any cause. A poor prognosis was defined as recurrent disease, persistent disease, or PTC-related mortality. Recurrent and persistent diseases were determined by the results of subsequent surgery, serum thyroglobulin level, neck ultrasound or computed tomography, 131I WBS, bone scan, or F-fluorodeoxyglucose positron emission tomography scan.
Histological evaluation of tissue specimens and DNA extraction
The tumor areas were marked by an endocrine pathologist using hematoxylin and eosin stained sections as a guide. Each marked area was dissected from the paraffin-embedded tumor block and transferred into Eppendorf tubes. All samples were digested with proteinase K (Sigma, St. Louis, MO, USA) for more than 24 hours at 56℃ and the DNA was then isolated from the digested tissue using a Tissue SV Mini kit (General Biosystem Inc., Seoul, Korea). The mutational status of BRAFV600E was confirmed using the polymerase chain reaction-restriction fragment length polymorphism (PCR-RFLP) method for the patients underwent surgery in 1995 to 2003 or by direct sequencing for the patients underwent surgery in 2009 to 2012.
PCR-RFLP for the BRAFV600E mutation
The PCR protocol for amplifying BRAF exon 15 used the following primers: forward, 5'-GCTTGCTCTGATAGGAAAATGAG-3' and reverse, 5'-GATACTCAGC AGCATCTCAGG-3'. The PCR analysis was conducted using the following amplification protocol: initial denaturation at 95℃ for 5 minutes, then 40 cycles of denaturation at 94℃ for 20 seconds, annealing at 56℃ for 20 seconds, elongation at 72℃ for 20 seconds, and a final extension at 72℃ for 10 minutes. The denatured PCR products were digested with restriction endonuclease TspRI (New England Biolabs, Beverly, MA, USA) and electrophoresed onto an agarose gel. The digestion of the PCR products with TspRI yielded three major bands at 125, 87, and 12 base pairs (bp) for the wild-type allele. The T1799A mutation abolished the restriction site and resulted in a prominent 212 bp band from the mutant allele and residual bands from the normal allele.
To confirm the reliability of the PCR-RFLP results, DNA from 13 PTC samples were chosen at random and sequenced. The sequencing was performed with a PTC-225 Peltier Thermal Cycler (MJ Research, Waltham, MA, USA) using an ABI PRISM BigDye Terminator Cycle Sequencing Kit and AmpliTaq DNA polymerase (Applied Biosystems, Foster City, CA, USA). All 13 sequencing results confirmed the BRAFV600E mutation statuses that were indicated by the PCR-RFLP method.
Direct sequencing of the BRAFV600E mutation
The BRAFV600E mutation was amplified with the PCR method using genomic DNA. Following purification of the PCR products, direct DNA bidirectional sequencing was conducted with an ABI 3130XL Genetic Analyzer and a BigDye Terminator cycle sequencing kit (Applied Biosystems).
Statistical analysis
All numeric data were expressed as mean±SD. Continuous variables were compared using a Student t test, and nonnumeric variables were analyzed with the chi-square test after excluding missing data. Chi-square tests were also performed to compare the incidence rates of recurrent disease, persistent disease, and PTC-related death in terms of BRAFV600E mutation status in the 1995 to 2003 patients diagnosed with PTC. All statistical analyses were conducted using SPSS version 20.0 (IBM Co., Armonk, NY, USA) and a P<0.05 was considered to be statistically significant.
RESULTS
Prevalence of BRAFV600E mutation status
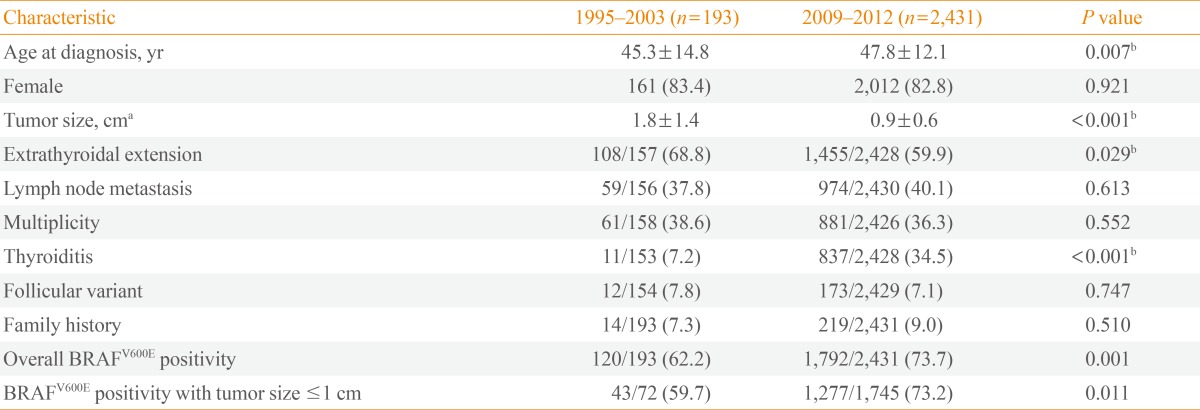
There was not a linear increasing trend for the presence of the BRAFV600E mutation over the past two decades (Fig. 1) but the mean rate of the BRAFV600E mutation was higher in 2009 to 2012 patients than in 1995 to 2003 patients (73.7% vs. 62.2%, P=0.001) (Table 1). Because detection of the BRAFV600E mutation in the two groups was performed using two different techniques, differences in the diagnostic accuracy of the detection methods were adjusted for, based on previous reports (sensitivity of RFLP-PCR, 78.6%; and sensitivity of direct DNA sequencing, 83.0%). Even after adjusting for differences in the diagnostic accuracy of the detection methods, there was still an increase in the rate of the BRAFV600E mutation from 1995 to 2003 to 2009 to 2012. The BRAFV600E mutation rates for PTMC were 59.7% and 73.2% in 1995 to 2003 and 2009 to 2012, respectively (P=0.011).

Changes in the prevalence of BRAFV600E mutational status in patients with papillary thyroid carcinoma over two decades in Korea.
Clinical and pathological features of PTC over the past two decades
The clinicopathological features of PTC during the two studied time periods are provided in Table 1. The mean age at diagnosis increased from 45.3 years in 1995 to 2003 patients to 47.8 years in 2009 to 2012 patients (P=0.007) but there was no significant difference in the distribution of male and female patients. The mean PTC tumor size was significantly larger in 1995 to 2003 patients (P<0.001) and the proportion of PTMC increased from 37.3% in 1995 to 2003 patients to 71.8% in 2009 to 2012 patients (P<0.001). There was a higher frequency of ETE in 1995 to 2003 patients with PTC but the frequency of thyroiditis was higher in 2009 to 2012 patients. There were no significant differences between the two groups for the frequency of LNM, multiplicity, FV, or family history of thyroid cancer. After adjusting for BRAFV600E mutation status, tumor size and the frequency of ETE remained significantly higher in 1995 to 2003 patients but only the frequency of thyroiditis remained significantly higher in 2009 to 2012 patients.
Clinicopathological features of PTC in relation to BRAFV600E mutation status
The associations between BRAFV600E mutation status and the clinicopathological features of PTC for the two time periods were analyzed (Table 2). In 1995 to 2003 patients, the frequency of ETE was significantly higher in patients with the BRAFV600E mutation (P=0.047) but there were no significant differences in mean age at diagnosis, proportion of females, tumor size, family history, frequency of LNM, multiplicity, thyroiditis, or FV. The median follow-up duration was 10.8 years in patients with the BRAFV600E mutation and 9.5 years in patients with the wild-type gene (P=0.571). Recurrent disease, persistent disease, and PTC-related mortality were found in 15 of the 98 patients with the BRAFV600E mutation (n=10, 4, and 1, respectively) and 12 of the 56 patients without a BRAFV600E mutation (recurrent disease, n=10; and PTC-related mortality, n=2). The recurrence rates for patients positive for the BRAFV600E mutation and for the wild-type gene were 10.2% and 17.9%, respectively (P=0.639). There was no difference in the overall prognosis by BRAFV600E mutation status in 1995 to 2003 patients diagnosed with PTC (P=0.381).

Clinicopathological Features of Papillary Thyroid Carcinomas in Relation to BRAFV600E Mutation Status
In 2009 to 2012, the BRAFV600E mutation was more frequently found in PTC patients with ETE and LNM. Patients with the BRAFV600E mutation were significantly older than those without the BRAFV600E mutation, and the predominance of female patients was lower. Thyroiditis and FV were more frequently found in patients without the BRAFV600E mutation (P<0.001 for both). When the clinicopathological features of PTC based on BRAFV600E mutation status were compared according to tumor size (≤1 cm vs. >1 cm), there were no significant differences (data not shown).
DISCUSSION
Since 1995, the prevalence of the BRAFV600E mutation in Korean patients with PTC has been approximately 70%. The present findings demonstrate that from 1995 to 2003 only ETE was more frequently observed in patients with the BRAFV600E mutation and that the clinical outcomes of PTC, including recurrence and PTC-related mortality, did not differ according to BRAFV600E mutation status. However, patients with the BRAFV600E mutation who were treated from 2009 to 2012 had a higher frequency of the more aggressive pathological features of PTC, including ETE and LNM, while the favorable features of PTC, such as thyroiditis and FV, were observed less frequently. Therefore, these findings suggest that the BRAFV600E mutation status may be a useful prognostic factor of PTC in recently diagnosed patients.
Because the statistical differences between the two groups of patients may have been due to the difference in the number of subjects (193 patients in 1995 to 2003 versus 2,431 patients in 2009 to 2012), the associations between BRAFV600E mutation status and the clinicopathological features of PTC were analyzed using all of the subjects (n=2,624). Patients with the BRAFV600E mutation were significantly older (48.0 years vs. 46.4 years) and exhibited a lower predominance of female patients than patients with wild-type BRAF. ETE and LNM were more frequently found in patients with the BRAFV600E mutation and the rates of thyroiditis and FV in these patients were significantly lower than in patients without the BRAFV600E mutation. Tumor size and the frequency of multiplicity did not significantly differ based on BRAFV600E mutation status for the overall population (data not shown).
In the present study, there was a trend for an increase in the mean rate of the BRAFV600E mutation from 62.2% to 73.7% over the two time periods (Fig. 1). In the subgroup analysis of PTMCs, the mean rate of the BRAFV600E mutation significantly increased from 59.7% to 73.2% over the two time periods. However, the increased rate of the BRAFV600E mutation between the two time periods may be attributed to differences in the diagnostic accuracy of the detection methods. The sensitivity of RFLP-PCR is 78.6% whereas the sensitivity of direct DNA sequencing is 83.0% [21]; and thus, direct DNA sequencing is more reliable for detection of the BRAFV600E mutation. Regardless, even after adjusting for differences in diagnostic accuracy, the rate of the BRAFV600E mutation still increased over the past two decades although it remains unclear why this trend has occurred. Considering that a point mutation is generated by mutagens such as environmental toxins there are any number of possible continuous environmental factors that may have influenced the prevalence of this mutation. As yet, data regarding this issue are not available.
A recent study demonstrated that the BRAFV600E mutation rate in the United States was stable at approximately 46% from 1974 to 2009 whereas the RAS mutation rate increased from 18% to 44% over the past four decades [22]. The frequency of the BRAFV600E mutation in that study was lower than that observed in the present study. Thus, the recent increase in the rates of PTC and PTMC do not seem to be pathogenically associated with the BRAFV600E mutation in the United States.
Although it remains unclear why the prevalence of the BRAFV600E mutation is higher in Korea than in other countries, the increasingly high rate of this mutation indicates that there are unique pathophysiological characteristics present in Korean PTC patients [18]. Iodine-rich diets or chronic thyroiditis in the Korean population may be associated with genetic alterations, including the BRAFV600E mutation. For example, there is a positive correlation between Hashimoto's thyroiditis and the development of PTC [23,24]. Because the prevalence of Hashimoto's thyroiditis is high in Korea, this positive correlation may provide an explanation for the high incidence of PTC in this country. However, in the present study, patients with the BRAFV600E mutation were less likely to have underlying Hashimoto's thyroiditis than patients with the wild-type gene. Moreover, Hashimoto's thyroiditis is associated with genetic alterations other than BRAFV600E mutation such as rearrangements of RAS, ERK, and RET-PTC [25,26]. Therefore, the relationship between the BRAFV600E mutation in PTC and chronic thyroiditis requires further assessment.
The frequency of thyroiditis was significantly higher in 2009 to 2012 patients than in 1995 to 2003 patients in the present study. The presence of thyroiditis was determined using the histopathological report after thyroidectomy rather than by the presence of thyroid auto-antibodies such as the antimicrosome antibody. Recent pathological reports have become more detailed and, thus, it was possible that in the past only prominent thyroiditis was described and any observed thyroiditis-likelihood features may not have been mentioned. Therefore, a direct comparison of the rate of thyroiditis between these two periods would be difficult.
Although there is controversy regarding whether the various histological variants or subtypes of PTC are associated with adverse outcomes, the tall cell variant is more frequently observed than FV in Korean PTC patients with the BRAFV600E mutation [27,28]. The present findings are consistent with these data in that the proportion of FV-PTC was significantly lower in patients with the BRAFV600E mutation than in those with the wild-type gene.
The BRAFV600E mutation is associated with the aggressive pathological features of PTC as well as a poor prognosis [14,29]. However, this association was not prominent in the Korean patients in the present study, which may be explained by the high rate of the BRAFV600E mutation in Korea [30,31,32]. In the present study, only the frequency of ETE differed significantly according to BRAFV600E mutation status in 1995 to 2003 patients whereas all other pathological features and the recurrence and mortality rates were not associated with BRAFV600E mutation status. However, although long-term patient outcomes were not evaluated in this study due to the relatively short duration of the follow-up period, 2009 to 2012 patients with the BRAFV600E mutation more commonly exhibited the aggressive features of PTC, such as ETE and LNM, while the favorable features of PTC, such as FV and thyroiditis, were less commonly observed. These findings demonstrate that a relationship exists between the BRAFV600E mutation and the prognosis of PTC.
A possible explanation for this poor prognostic correlation in 1995 to 2003 patients may be that the prognostic power of the BRAFV600E mutation was lower than, and thus overshadowed by, other aggressive pathological features because most PTCs are diagnosed in the more advanced stages. By contrast, the predictive power of the BRAFV600E mutation may have been better in 2009 to 2012 patients because the rate of PTCs that were smaller and had more favorable pathological characteristics increased due to improved early detection techniques. To test this hypothesis, the clinicopathological characteristics of the PTCs were compared according to tumor size (≤1 cm vs. >1 cm) but there were no significant differences. Thus, it remains unclear why the predictive power of the more recent BRAFV600E mutation is better. Based on the findings of a worldwide meta-analysis [14], there is a strong association between the BRAFV600E mutation and the aggressive features of PTC, including ETE, LNM, and advanced tumor node metastasis stages, after the year 2000 [33,34,35,36,37,38,39].
In conclusion, the present findings demonstrate that the prevalence of the BRAFV600E mutation was higher in Korea than in other countries and that it has been increasing over the last two decades. The clinical outcomes associated with PTC did not differ based on BRAFV600E mutation status in 1995 to 2003 patients but the BRAFV600E mutation was associated with the more aggressive features of PTC in 2009 to 2012 patients. This suggests that BRAFV600E mutation status may be a more useful prognostic factor for PTC in patients who have been more recently diagnosed, using early detection methods. Further study with long-term follow-up periods is required to more fully address this issue.
ACKNOWLEDGMENTS
This work was supported by grant No. 800-20120031 from the Seoul National University Hospital Research Fund and the Seoul National University College of Medicine.
Notes
No potential conflict of interest relevant to this article was reported.