Articles
- Page Path
- HOME > Endocrinol Metab > Volume 33(1); 2018 > Article
-
Original ArticleHigh Brachial Ankle Pulse Wave Velocity as a Marker for Predicting Coronary Artery Stenosis in Patients with Type 2 Diabetes
-
Bo Hyun Kim1*
 , Jae Sik Jang2*
, Jae Sik Jang2* , Yong Seop Kwon3
, Yong Seop Kwon3 , June Hyung Kim4
, June Hyung Kim4 , In Joo Kim1
, In Joo Kim1 , Chang Won Lee3
, Chang Won Lee3
-
Endocrinology and Metabolism 2018;33(1):88-96.
DOI: https://doi.org/10.3803/EnM.2018.33.1.88
Published online: March 21, 2018
1Department of Internal Medicine, Pusan National University Hospital and Biomedical Research Institute, Pusan National University School of Medicine, Busan, Korea.
2Department of Internal Medicine, Inje University Busan Paik Hospital, Inje University College of Medicine, Busan, Korea.
3Department of Internal Medicine, Busan St. Mary's Hospital, Busan, Korea.
4Department of Radiology, Busan St. Mary's Hospital, Busan, Korea.
- Corresponding author: Chang Won Lee. Department of Internal Medicine, Busan St. Mary's Hospital, 25-14 Yongho-ro 232beon-gil, Nam-gu, Busan 48575, Korea. Tel: +82-51-933-7235, Fax: +82-51-932-8600, koje94@hanmail.net
- *These authors contributed equally to this work.
Copyright © 2018 Korean Endocrine Society
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Background
- We evaluated the ability of brachial ankle pulse wave velocity (baPWV) to predict coronary artery stenosis (CAS) in patients with type 2 diabetes, and compared the predictive power of baPWV to that of well-known cardiovascular disease (CVD) risk calculators.
-
Methods
- The study group included 83 consecutive patients over 30 years old with type 2 diabetes who complained of vague chest discomfort. An automatic pulse waveform analyzer was used to measure baPWV. CAS was measured using multi-slice computed tomographic (MSCT) angiography.
-
Results
- Age, maximal baPWV, duration of diabetes, current smoking, the UK Prospective Diabetes Study (UKPDS) Risk Engine score, American College of Cardiology/American Heart Association (ACC/AHA) risk estimator score, the Framingham risk calculator score, and coronary artery calcium score were greater in patients with CAS than in those without CAS. An area under the curve (AUC) indicative of a predictive value for CAS (≥20%) was found for several parameters. The AUC of maximal baPWV, the UKPDS Risk Engine, the ACC/AHA ASCVD risk estimator, and the Framingham risk calculator were 0.672 (95% confidence interval [CI], 0.554 to 0.785; P=0.010), 0.777 (95% CI, 0.675 to 0.878; P<0.001), 0.763 (95% CI, 0.660 to 0.866; P<0.001), and 0.736 (95% CI, 0.629 to 0.843; P<0.001), respectively. The optimal cutoff value of baPWV for the detection of CAS was 1,650 cm/sec (sensitivity, 68.9%; specificity, 63.2%).
-
Conclusion
- Maximal baPWV was closely related with CAS detected by MSCT coronary angiography in patients with type 2 diabetes. baPWV has the potential to be a useful, noninvasive screening tool for the prediction of occult CAS in patients with type 2 diabetes.
- Coronary artery disease (CAD) is major cause of death in individuals with diabetes, and asymptomatic CAD develops more frequently in person with diabetes than in the healthy population. The prevalence of asymptomatic CAD and the incidence of sudden cardiac death are much higher in patients with a long duration of diabetes than in those with a short duration [1]. Thus, the integrated management of multiple risk factors including hypertension, dyslipidemia, and diabetes is essential for the prevention of future cardiovascular disease (CVD) [23]. In addition, early detection of patients at a high risk of CVD is critical.
- Pulse wave velocity (PWV) is a simple, noninvasive method for estimating arterial stiffness, and it is a predictor of the severity of vascular damage [4] and the prognosis of CVD in patients with hypertension [5] and diabetes [6]. Brachial ankle pulse wave velocity (baPWV) measurements have recently become available as a tool for estimating PWV and baPWV can be measured more simply than the carotid-femoral PWV, which is not easy to measure in routine clinical settings. The baPWV is considered to be a simple tool for assessing vascular damage reflecting stiffness of the aorta and/or the peripheral arteries. The measurement of baPWV has been validated, and the reproducibility of baPWV was also previously reported elsewhere [78910].
- The newest-generation multi-slice computed tomography (MSCT) is considered to be an accurate imaging method for detecting significant CAD; however, radiation exposure and its high cost restrict the use of MSCT as a screening tool to detect asymptomatic CAD [1112]. Recent studies have demonstrated that baPWV was closely associated with risk factors for CVD in patients with occult CAD detected by MSCT. However, in those studies, the participants were relatively healthy, as they drawn from members of the general population who underwent routine health evaluations, and the proportion of patients with diabetes was only 10% to 18% [1314].
- However, there is little evidence regarding the relationship between baPWV and the presence of coronary artery stenosis (CAS) as evaluated by MSCT angiography in patients with type 2 diabetes mellitus who have atypical symptoms and equivocal exercise test results. The aim of this study was to evaluate the association of baPWV as an index of arterial stiffness in the lower-extremity arteries and CAS in patients with type 2 diabetes with atypical chest pain using non-invasive MSCT angiography. The associations of various CVD risk calculator with CAS were also evaluated.
INTRODUCTION
- Study population
- We retrospectively enrolled 83 patients over 30 years old with type 2 diabetes who underwent MSCT angiography for suspected CAD because of vague chest discomfort with inconclusive treadmill exercise electrocardiography (ECG) and/or nuclear stress test results between January 2008 and December 2009. An automatic pulse waveform analyzer was used to measure baPWV. The usual anthropometric and clinical laboratory data were collected from patients. Those who had previous atherosclerotic disease, including peripheral artery disease with a low ankle brachial index (<0.9), stroke, chronic kidney disease (estimated glomerular filtration rate <60 mL/min/1.73 m2), previous CAD, a history of percutaneous coronary intervention (PCI) or coronary arterial bypass surgery, or New York Heart Association class II to IV heart failure were excluded from the current study. Written informed consent was provided by all enrolled patients. This study was approved by the Institutional Review Board of Busan St. Mary's Hospital (Busan, Korea, IRB no. BSM 2008-04).
- Anthropometric and laboratory evaluations
- Blood pressure (BP) in the seated position was measured by a digital sphygmomanometer after at least 5 minutes of rest. The body mass index (BMI) was calculated as the weight in kilograms divided by the squared height in meters (kg/m2), using the values of the height and weight of the patients that were measured just before measuring baPWV. Fasting blood samples were concurrently collected on the day of the study and the usual clinical parameters were checked, such as fasting plasma glucose (FPG), aspartate aminotransferase, alanine aminotransferase (ALT), the lipid profile, and gamma glutamyl transpeptidase (γ-GTP). The fasting state was defined as a fasting duration of at least 8 hours. Hemoglobin A1c (HbA1c) was measured by high performance liquid chromatography using the Variant TM II Turbo (Bio-Rad Laboratories, Hercules, CA, USA). The patients' smoking status, alcohol intake, and medication use were evaluated by an electronic chart review and a questionnaire.
- baPWV measurements
- Patients were allowed to take their regular medications on the study day, and were examined in the supine position after 5 minutes of rest in a quiet room. A baPWV was measured using an automatic waveform analyzer (VP-1000, Colin, Komaki, Japan) according to the manufacturer's recommendations and a previous validated method [15]. Both left and right baPWVs were measured, and the higher value was defined as the maximum baPWV (max-baPWV) [16].
- MSCT angiography and image analysis
- Data were acquired using a 64 multi-detector computed tomographic scanner (Toshiba Medical Systems, Tokyo, Japan). Angiographic images were acquired with 16×0.75 mm slice collimation, a gantry rotation time of 420 ms, a tube energy of 120 kV, a table feed of 2.8 mm/rotation, and an effective tube current of 500 mAs according to a previously published protocol [1314]. An intravenous contrast agent (Visipaque, GE-Healthcare Amersham, Piscataway, NJ, USA) was injected at a rate of 4 mL/sec. A β-blocker (5 mg of metoprolol) was intravenously injected in all patients with a heart rate >65 beats per minute before the computed tomographic angiography scan. In this study, to estimate the degree of stenosis, we visually traced the coronary lumen at the point with maximal stenosis. Coronary stenosis was considered to be present if ≥20% stenosis of the coronary artery lumen was observed at the maximal stenotic site, and severe coronary stenosis was defined as the presence of ≥50% stenosis at the maximal stenotic site. The quantitative coronary artery calcium (CAC) score was measured using the most widely used method [17].
- Coronary artery disease risk calculators
- The United Kingdom Prospective Diabetes Study (UKPDS) Risk Engine program was downloaded from https://www.dtu.ox.ac.uk/riskengine/download.php. The American College of Cardiology/American Heart Association (ACC/AHA) atherosclerotic cardiovascular disease (ASCVD) risk estimator was downloaded from http://www.cvriskcalculator.com/ as a Microsoft Excel file. In addition, the Framingham risk calculator was downloaded from http://cvrisk.mvm.ed.ac.uk/calculator/excelcalc.htm as a Microsoft Excel file.
- Statistical analysis
- Data are expressed as mean±standard deviation (SD). The unpaired t test was used to assess differences in continuous variables, and the chi-square test was applied to categorical variables between subjects with and without CAS. Spearman correlation analysis was performed to evaluate the associations of the severity of CAS, with max-baPWV and other clinical variables. Age- adjusted partial correlation analysis was performed for statistically significant clinical variables. A receiver operating characteristic (ROC) curve analysis was performed to estimate the baPWV cut-off point predicting the presence of CAS. The value with the highest sum of sensitivity and specificity was identified as the cutoff point. The predictive accuracy of the parameters was calculated as the area under the curve (AUC). We used a comparative ROC curve analysis to test the statistical significance of the differences among the various CVD calculators and max- baPWV for predicting CAS. Multivariable logistic regression analysis was performed to assess independent associations between the presence of CAS and baPWV after adjusting for age, sex, hypertension, smoking, and dyslipidemia. MedCalc (MedCalc Software, Mariakerke, Belgium) was used for all statistical analyses. A P values <0.05 were considered to indicate statistical significance.
METHODS
- Clinical characteristics of the patients
- The baseline clinical characteristics of the patients with or without CAS (≥20%) are shown in Table 1. The proportion of patients with CAS (≥20%) and severe CAS (≥50%) was 43 of 83 (51.8%) and 34 of 83 (40.9%), respectively. Most patients with CAS (34 of 43, 79.1%) had severe CAS. CAS was associated with old age, current smoking, and a longer duration of diabetes. Max-baPWV was significantly greater in patients with CAS than in those without CAS. The scores of the UKPDS Risk Engine, the ACA/AHA ASCVD risk calculator, and the Framingham risk calculator were significantly higher in patients with CAS. However, there were no statistically significant differences in BMI, BP, HbA1c, total cholesterol, low density lipoprotein cholesterol (LDL-C), high density lipoprotein cholesterol, triglycerides, ALT, GTP, or FPG between patients with and without CAS. There were no significant differences in statin use, anti-platelet agent use, renin-angiotensin system blockers, and insulin therapy between the two groups (Table 1).
- Correlations between CAS, baPWV, and other variables
- The severity of CAS showed significant correlations with age, the amount of cigarette smoking (pack-years), max-baPWV, duration of diabetes, the UKPDS Risk Engine score, the ACC/AHA ASCVD risk estimator score, the Framingham risk calculator score, and the CAC score (Table 2). After age adjustment, the severity of CAS showed a significant correlation with amount of cigarette smoking (pack-years), duration of diabetes, the UKPDS Risk Engine score, the ACC/AHA ASCVD risk estimator score, the Framingham risk calculator score, and the CAC score. However, the severity of CAS was not associated with max-baPWV after adjustment for age (Table 2).
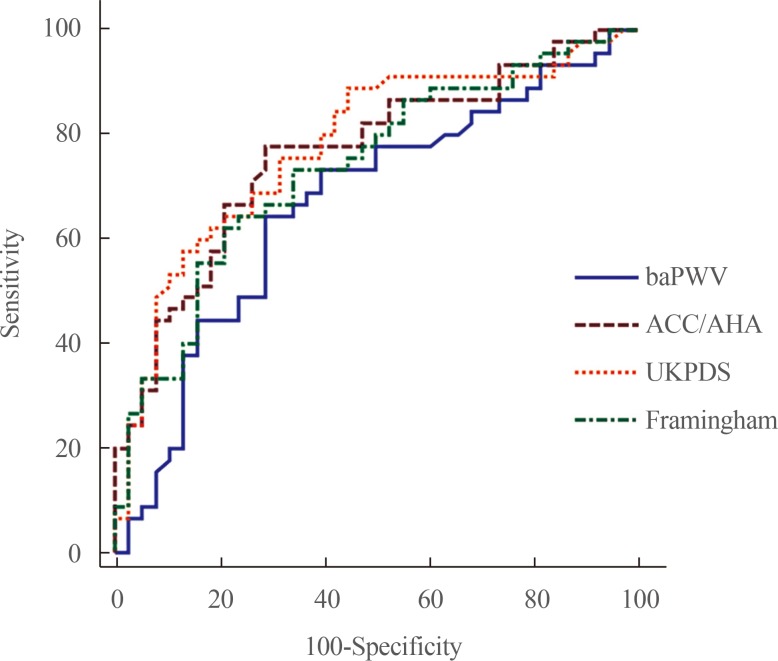
- Fig. 1 shows the ROC curve of the association between baPWV and the presence of CAS in patients with type 2 diabetes. The AUC was 0.672 (95% confidence interval [CI], 0.554 to 0.785; P=0.010). ROC curve analysis showed that the best cutoff point for a baPWV value predicting the presence of CAS was 1,650 cm/sec. When a baPWV greater than 1,650 cm/sec was used as the cutoff value, sensitivity and specificity were 68.9% and 63.2%, respectively. In a comparative ROC curve analysis, no significant difference was found between max-baPWV and three CVD estimating calculators (Table 3, Fig. 2).
- In the multivariable analysis, a baPWV >1,650 cm/sec was an independent predictor of the presence of CAS (≥20%) after adjusting for potential confounders including age, sex, hypertension, dyslipidemia, and smoking (odds ratio, 4.34; 95% CI, 1.19 to 15.79; P<0.026) (Table 4).
RESULTS
- The present study showed that baPWV can be used as a screening tool for patients with type 2 diabetes at risk of developing atherosclerosis and that a higher baPWV is a significant predictor of CAS as detected by MSCT coronary angiography. Our study suggests that baPWV value above a cutoff value of 1,650 cm/sec may be an acceptable predictor of occult CAD in patients with diabetes.
- PWV reflects arterial stiffness, which is caused by a central elastic component and a peripheral muscular component, and the latter is greater in baPWV than in carotid-femoral PWV [18]. Elevated baPWV values have been observed in patients with CVD risk factors, including hypertension, diabetes, and dyslipidemia. Many studies have evaluated the use of baPWV to predict cardiovascular risk, and it has been widely measured in various clinical situations [16171819]. In patients with diabetes, baPWV was found to be closely associated with age and BP [1619]. Nakamura et al. [20] suggested that baPWV may be useful for assessing macrovascular damage, and Choi et al. [21] reported a close association of baPWV with the CVD risk factors of metabolic syndrome. Various cutoff values have been proposed. In a recent study, a baPWV cutoff value of 1,400 cm/sec was found to be useful for risk stratification by the Framingham score and for detecting of patients with atherosclerotic CVD [22]. Several other studies have proposed baPWV cutoffs of 1,400 to 1,800 cm/sec for the prediction of cardiovascular risk factors or overt CAD with high diagnostic accuracy [131423].
- In our study, a baPWV >1,650 cm/sec was an independent marker of the presence of CAS (≥20%) after adjusting for various confounders including age, sex, smoking, hypertension, and dyslipidemia in the multivariable analysis. Therefore, we think that the presence of CAS might be detected by the use of baPWV in patients with diabetes. We also determined the prognostic ability of high baPWV (>1,650 cm/sec) for the presence of CAS in patients with diabetes, finding a sensitivity of 70% and a specificity of 63%. These results suggest that it may be necessary to perform a non-invasive study such as an exercise treadmill test or myocardial scintigraphy if a high value of baPWV is documented in patients with diabetes. However, whether a coronary evaluation of patients is indicated should be decided based on their clinical presentation, including their history of angina symptoms, ECG, and echocardiographic findings.
- Arterial stiffness increases systolic BP, whereas it decreases diastolic BP, resulting in a wide pulse pressure [24,25]. The increased systolic BP has a negative effect on the heart due to an increased workload, while a reduced diastolic BP may limit coronary artery perfusion. Cross-sectional studies have proposed that these effects may explain the association between arterial stiffness and acute coronary syndrome [2627]. However, hemodynamic data and coronary risk factors including BP, pulse pressure, total cholesterol, LDL-C, triglycerides, and plasma glucose were not significantly associated with the presence of CAS in our study. This may be explained by the fact that a significant proportion (>60%) of the patients with CVD risk factors in our study had been previously treated with statins, anti-platelet agents, and renin-angiotensin receptor blockers. The strong association between max-baPWV and the presence of CAS in patients with diabetes observed in our study may provide an additional explanation for the association between arterial stiffness and CVD.
- In our study, the presence of CAS (≥20%) was closely associated with baPWV in the AUC analysis but the presence of significant CAS (≥50%) was not. Seo et al. [27] evaluated the predictive value of baPWV for CAD risk, and found that baPWV did not have a significant association with coronary stenosis. We suggest that the finding in this study of no relationship between baPWV and significant CAS was related to the fact that severe CAS was defined by ≥50% occlusion. Because baPWV reflects arterial stiffness, it is likely to be correlated with early-stage CAD, but not advanced CAD.
- Various tools have used to evaluate the risk of CVD in advance. The UKPDS Risk Engine was developed to estimate the risk of CAD in diabetic patients [28]. The ASCVD risk estimator can evaluate the 10-year risk of CAD in adults aged 40–79 [29]. The Framingham risk calculator can be used to evaluate the risk of various atherosclerotic CVD events [30]. In our study, the relationship between the presence of CAS and scores on these three risk estimating tools (the UKPDS Risk Engine, the ASCVD risk estimator, and the Framingham risk calculator) was quite strong. In several studies, the predictive value of these evaluation tools was compared with that of non-invasive exams, and the predictive value was found to be improved by using these tools together with non-invasive exams [313233]. In our study, the predictive value of baPWV for CAD was compared with that of various risk evaluation tools, and the value of baPWV was somewhat lower than that of the other risk evaluation tools. However, no significant difference was found between the predictive value of max-PWV and the three CVD estimating calculators (Fig. 2).
- In current clinical practice, the management of patients with CAD depends on an initial clinical evaluation, with higher-risk patients referred for a conventional coronary angiogram and PCI in most cases [34]. However, MSCT coronary angiography is a reliable, noninvasive imaging modality for the diagnosis of CAD. The negative predictive value of MSCT angiography is approximately 100%, allowing CAD to be ruled out [3335]. Based on the diagnostic accuracy of MSCT coronary angiography, we used this noninvasive modality as a diagnostic tool to define CAS in our study population instead of conventional coronary angiography.
- Our study has some potential limitations. First, the current study was a single-center, retrospective study. Second, a gross examination of the coronary angiographic data was not performed to determine the degree of coronary artery narrowing. Third, there might have been many confounding factors that could not be properly adjusted for in the quantitative analysis of CAS. In addition, we were not able to obtain comprehensive data regarding the total atherosclerotic burden of the entire coronary tree, although baPWV may be more closely related to the total coronary atherosclerotic burden than the severity of coronary stenosis. Last, the present study included a relatively small number of patients.
- In conclusion, this study showed a significant correlation between max-baPWV and a noninvasive MSCT angiographic assessment of CAD in patients with type 2 diabetes with atypical symptoms and inconclusive stress test results. In addition, this study suggests that the cutoff value of 1,650 cm/sec for baPWV can be an acceptable marker for predicting CAD in patients with type 2 diabetes. Further studies are needed to evaluate whether specific values of baPWV may be related to adverse clinical outcomes in patients with type 2 diabetes.
DISCUSSION
-
Acknowledgements
- This work was supported by a clinical research grant from Pusan National University Hospital in 2016, and the research fund of the Busan and Ulsan and the Kyungnam Branch of the Korean Endocrine Society (2015).
ACKNOWLEDGMENTS
-
CONFLICTS OF INTEREST: No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS: Conception or design: B.H.K., J.S.J., C.W.L. Acquisition, analysis, or interpretation of data: B.H.K., J.S.J., Y.S.K., J.H.K. Drafting the work or revising: B.H.K., J.S.J. Final approval of the manuscript: I.J.K., C.W.L.
Article information
- 1. Yoo WS, Kim HJ, Kim D, Lee MY, Chung HK. Early detection of asymptomatic coronary artery disease in patients with type 2 diabetes mellitus. Korean J Intern Med 2009;24:183–189. ArticlePubMedPMCPDF
- 2. Pearson TA. New tools for coronary risk assessment: what are their advantages and limitations? Circulation 2002;105:886–892. ArticlePubMed
- 3. Wood D. Joint European Societies Task Force. Established and emerging cardiovascular risk factors. Am Heart J 2001;141(2 Suppl):S49–S57. ArticlePubMed
- 4. van Popele NM, Grobbee DE, Bots ML, Asmar R, Topouchian J, Reneman RS, et al. Association between arterial stiffness and atherosclerosis: the Rotterdam Study. Stroke 2001;32:454–460. ArticlePubMed
- 5. Laurent S, Boutouyrie P, Asmar R, Gautier I, Laloux B, Guize L, et al. Aortic stiffness is an independent predictor of all-cause and cardiovascular mortality in hypertensive patients. Hypertension 2001;37:1236–1241. ArticlePubMed
- 6. Cruickshank K, Riste L, Anderson SG, Wright JS, Dunn G, Gosling RG. Aortic pulse-wave velocity and its relationship to mortality in diabetes and glucose intolerance: an integrated index of vascular function? Circulation 2002;106:2085–2090. ArticlePubMed
- 7. Yamashina A, Tomiyama H, Takeda K, Tsuda H, Arai T, Hirose K, et al. Validity, reproducibility, and clinical significance of noninvasive brachial-ankle pulse wave velocity measurement. Hypertens Res 2002;25:359–364. ArticlePubMed
- 8. Suzuki E, Kashiwagi A, Nishio Y, Egawa K, Shimizu S, Maegawa H, et al. Increased arterial wall stiffness limits flow volume in the lower extremities in type 2 diabetic patients. Diabetes Care 2001;24:2107–2114. ArticlePubMed
- 9. Tomiyama H, Yamashina A, Arai T, Hirose K, Koji Y, Chikamori T, et al. Influences of age and gender on results of noninvasive brachial-ankle pulse wave velocity measurement: a survey of 12517 subjects. Atherosclerosis 2003;166:303–309. ArticlePubMed
- 10. Ha BK, Kim BG, Kim DH, Lee SI, Jung SM, Park JY, et al. Relationships between brachial-ankle pulse wave velocity and peripheral neuropathy in type 2 diabetes. Diabetes Metab J 2012;36:443–451. ArticlePubMedPMC
- 11. Hamon M, Biondi-Zoccai GG, Malagutti P, Agostoni P, Morello R, Valgimigli M, et al. Diagnostic performance of multislice spiral computed tomography of coronary arteries as compared with conventional invasive coronary angiography: a meta-analysis. J Am Coll Cardiol 2006;48:1896–1910. ArticlePubMed
- 12. Hoffmann U, Moselewski F, Nieman K, Jang IK, Ferencik M, Rahman AM, et al. Noninvasive assessment of plaque morphology and composition in culprit and stable lesions in acute coronary syndrome and stable lesions in stable angina by multidetector computed tomography. J Am Coll Cardiol 2006;47:1655–1662. ArticlePubMed
- 13. Nam HJ, Jung IH, Kim J, Kim JH, Suh J, Kim HS, et al. Association between brachial-ankle pulse wave velocity and occult coronary artery disease detected by multi-detector computed tomography. Int J Cardiol 2012;157:227–232. ArticlePubMed
- 14. Kim HL, Jin KN, Seo JB, Choi YH, Chung WY, Kim SH, et al. The association of brachial-ankle pulse wave velocity with coronary artery disease evaluated by coronary computed tomography angiography. PLoS One 2015;10:e0123164. ArticlePubMedPMC
- 15. Asmar R, Benetos A, Topouchian J, Laurent P, Pannier B, Brisac AM, et al. Assessment of arterial distensibility by automatic pulse wave velocity measurement: validation and clinical application studies. Hypertension 1995;26:485–490. ArticlePubMed
- 16. Lee SW, Yun KW, Yu YS, Lim HK, Bae YP, Lee BD, et al. Determinants of the brachial-ankle Pulse Wave Velocity (baPWV) in patients with type 2 diabetes mellitus. J Korean Endocr Soc 2008;23:253–259.Article
- 17. Agatston AS, Janowitz WR, Hildner FJ, Zusmer NR, Viamonte M Jr, Detrano R. Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol 1990;15:827–832. ArticlePubMed
- 18. Blacher J, Asmar R, Djane S, London GM, Safar ME. Aortic pulse wave velocity as a marker of cardiovascular risk in hypertensive patients. Hypertension 1999;33:1111–1117. ArticlePubMed
- 19. Yamashina A, Tomiyama H, Arai T, Hirose K, Koji Y, Hirayama Y, et al. Brachial-ankle pulse wave velocity as a marker of atherosclerotic vascular damage and cardiovascular risk. Hypertens Res 2003;26:615–622. ArticlePubMed
- 20. Nakamura U, Iwase M, Nohara S, Kanai H, Ichikawa K, Iida M. Usefulness of brachial-ankle pulse wave velocity measurement: correlation with abdominal aortic calcification. Hypertens Res 2003;26:163–167. ArticlePubMed
- 21. Choi KM, Lee KW, Seo JA, Oh JH, Kim SG, Kim NH, et al. Relationship between brachial-ankle pulse wave velocity and cardiovascular risk factors of the metabolic syndrome. Diabetes Res Clin Pract 2004;66:57–61. ArticlePubMed
- 22. Imanishi R, Seto S, Toda G, Yoshida M, Ohtsuru A, Koide Y, et al. High brachial-ankle pulse wave velocity is an independent predictor of the presence of coronary artery disease in men. Hypertens Res 2004;27:71–78. ArticlePubMed
- 23. Tsuchiya M, Suzuki E, Egawa K, Nishio Y, Maegawa H, Inoue S, et al. Stiffness and impaired blood flow in lower-leg arteries are associated with severity of coronary artery calcification among asymptomatic type 2 diabetic patients. Diabetes Care 2004;27:2409–2415. ArticlePubMed
- 24. London GM, Guerin AP. Influence of arterial pulse and reflected waves on blood pressure and cardiac function. Am Heart J 1999;138:220–224. ArticlePubMed
- 25. Benetos A, Safar M, Rudnichi A, Smulyan H, Richard JL, Ducimetieere P, et al. Pulse pressure: a predictor of long-term cardiovascular mortality in a French male population. Hypertension 1997;30:1410–1415. ArticlePubMed
- 26. Millar JA, Lever AF, Burke V. Pulse pressure as a risk factor for cardiovascular events in the MRC mild hypertension trial. J Hypertens 1999;17:1065–1072. ArticlePubMed
- 27. Seo WW, Chang HJ, Cho I, Yoon YY, Suh JW, Kim KI, et al. The value of brachial-ankle pulse wave velocity as a predictor of coronary artery disease in high-risk patients. Korean Circ J 2010;40:224–229. ArticlePubMedPMC
- 28. Stevens RJ, Kothari V, Adler AI, Stratton IM. United Kingdom Prospective Diabetes Study (UKPDS) Group. The UKPDS risk engine: a model for the risk of coronary heart disease in type II diabetes (UKPDS 56). Clin Sci (Lond) 2001;101:671–679. ArticlePubMed
- 29. Goff DC Jr, Lloyd-Jones DM, Bennett G, Coady S, D'Agostino RB, Gibbons R, et al. 2013 ACC/AHA guideline on the assessment of cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 2014;129(25 Suppl 2):S49–S73. ArticlePubMed
- 30. D'Agostino RB Sr, Vasan RS, Pencina MJ, Wolf PA, Cobain M, Massaro JM, et al. General cardiovascular risk profile for use in primary care: the Framingham Heart Study. Circulation 2008;117:743–753. ArticlePubMed
- 31. Ankle Brachial Index Collaboration. Fowkes FG, Murray GD, Butcher I, Heald CL, Lee RJ, et al. Ankle brachial index combined with Framingham risk score to predict cardiovascular events and mortality: a meta-analysis. JAMA 2008;300:197–208. ArticlePubMedPMC
- 32. Fujihara K, Suzuki H, Sato A, Ishizu T, Kodama S, Heianza Y, et al. Comparison of the Framingham risk score, UK Prospective Diabetes Study (UKPDS) Risk Engine, Japanese Atherosclerosis Longitudinal Study-Existing Cohorts Combine (JALS-ECC) and maximum carotid intima-media thickness for predicting coronary artery stenosis in patients with asymptomatic type 2 diabetes. J Atheroscler Thromb 2014;21:799–815. ArticlePubMed
- 33. Schuijf JD, Bax JJ, Shaw LJ, de Roos A, Lamb HJ, van der Wall EE, et al. Meta-analysis of comparative diagnostic performance of magnetic resonance imaging and multislice computed tomography for noninvasive coronary angiography. Am Heart J 2006;151:404–411. ArticlePubMed
- 34. Management of stable angina pectoris. Recommendations of the Task Force of the European Society of Cardiology. Eur Heart J 1997;18:394–413. ArticlePubMed
- 35. Mollet NR, Cademartiri F, van Mieghem CA, Runza G, McFadden EP, Baks T, et al. High-resolution spiral computed tomography coronary angiography in patients referred for diagnostic conventional coronary angiography. Circulation 2005;112:2318–2323. ArticlePubMed
References
Receiver operating characteristic curve to determine the cutoff value of brachial ankle pulse wave velocity for coronary artery stenosis. The cutoff point of 1,650 cm/sec showed a sensitivity of 68.9%, a specificity of 63%, and an area under the curve of 0.672.
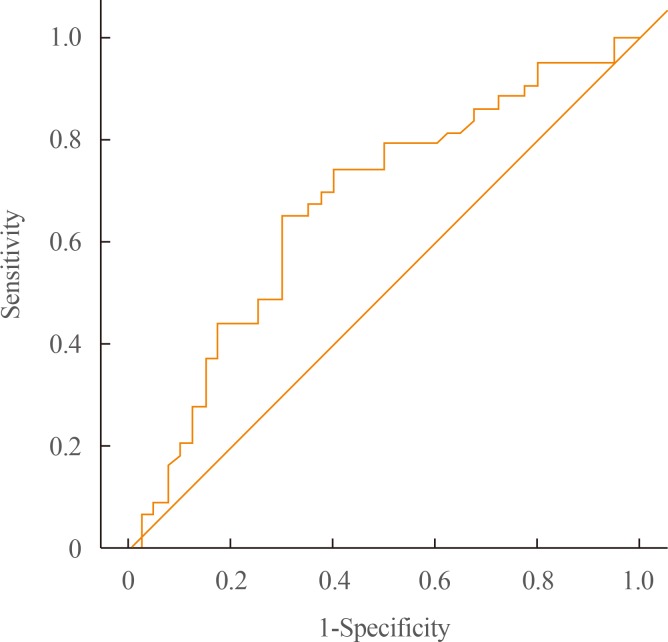
Pairwise comparison of the receiver operating characteristic curves of maximal brachial ankle pulse wave velocity (baPWV) and 3 cardiovascular disease (CVD) risk estimators, assessing their predictive value for coronary artery stenosis (≥20%). No significant differences were found between maximal baPWV and the three CVD risk estimators (all P values >0.05). UKPDS, United Kingdom Prospective Diabetes Study; ACC/AHA, American College of Cardiology/American Heart Association.

Baseline Clinical Characteristics According to the Presence of Coronary Artery Stenosis (≥20%)
Values are expressed as mean±SD or number (%). P values <0.05 were considered to indicate significance.
BP, blood pressure; baPWV, brachial ankle pulse wave velocity; HbA1c, hemoglobin A1c; FPG, fasting plasma glucose; LDL-C, low density lipoprotein cholesterol; HDL-C, high density lipoprotein cholesterol; ALT, alanine aminotransferase; γ-GTP, gamma glutamyl transpeptidase; PLT, platelet; RAS, renin-angiotensin system; UKPDS, United Kingdom Prospective Diabetes Study; ACC/AHA, American College of Cardiology/American Heart Association; CAC, coronary artery calcium.
Correlation and Age Adjusted Partial Correlation Analysis between Percentage of Stenosis at the Maximal Stenotic Site of Coronary Artery and Clinical Variables
P values <0.05 were considered to be indicate significance.
baPWV, brachial ankle pulse wave velocity; DM, diabetes mellitus; UKPDS, United Kingdom Prospective Diabetes Study; ACC/AHA, American College of Cardiology/American Heart Association; ASCVD, atherosclerotic cardiovascular disease; CAC, coronary artery calcium.
AUC Analysis of the Predictive Value of Various Parameters for CAS
P values <0.05 were considered to be indicate significance.
AUC, area under the curve; CAS, coronary artery stenosis; CVD, cardiovascular disease; CI, confidence interval; baPWV, brachial ankle pulse wave velocity; UKPDS, United Kingdom Prospective Diabetes Study; ACC/AHA, American College of Cardiology/American Heart Association.
Independent Predictors of Coronary Artery Stenosis (≥20%) on Coronary Computed Tomography Angiography
Figure & Data
References
Citations

- Polyvinyl Alcohol Phantoms With Heterogeneous Plaques: Estimation of Pulse Wave Velocity at the Stenotic Region Using Pulse Wave Imaging
Nima Mobadersany, Pengcheng Liang, Paul Kemper, Elisa E. Konofagou
Ultrasound in Medicine & Biology.2024; 50(1): 91. CrossRef - The risk factors of early arterial stiffness in type 2 diabetes without diabetic macroangiopathy
Jia-Hui Wu, Rui Wang, Xiao-Jiao Jia, Na Lu, Qiang Lu, Fu-Zai Yin, Chun-Ming Ma
International Journal of Diabetes in Developing Countries.2023;[Epub] CrossRef - Arterial Stiffness as a Predictor of the Index of Atherosclerotic Cardiovascular Disease in Hypertensive Patients
Guili Chang, Yueliang Hu, Qian Ge, Shaoli Chu, Alberto Avolio, Junli Zuo
International Journal of Environmental Research and Public Health.2023; 20(4): 2832. CrossRef - Pulse wave imaging of a stenotic artery model with plaque constituents of different stiffnesses: Experimental demonstration in phantoms and fluid-structure interaction simulation
Nima Mobadersany, Nirvedh H. Meshram, Paul Kemper, C.V. Sise, Grigorios M. Karageorgos, Pengcheng Liang, Gerard A. Ateshian, Elisa E. Konofagou
Journal of Biomechanics.2023; 149: 111502. CrossRef - Computational clustering reveals differentiated coronary artery calcium progression at prevalent levels of pulse wave velocity by classifying high-risk patients
Maximo Rousseau-Portalis, Leandro Cymberknop, Ignacio Farro, Ricardo Armentano
Frontiers in Cardiovascular Medicine.2023;[Epub] CrossRef - Pepsinogen ratio and brachial-ankle pulse wave velocity: a cross-sectional study on their interrelationship in atherosclerosis
Yuexi Li, Xiaoqin Liu, Yuhan Luo, Qiaoli Wang
BMC Cardiovascular Disorders.2023;[Epub] CrossRef - The Plasma Atherogenic Index is an Independent Predictor of Arterial Stiffness in Healthy Koreans
Ji Sun Nam, Min Kyung Kim, Kahui Park, Arim Choi, Shinae Kang, Chul Woo Ahn, Jong Suk Park
Angiology.2022; 73(6): 514. CrossRef - Risk assessment indicators and brachial-ankle pulse wave velocity to predict atherosclerotic cardiovascular disease
Hung-Ju Ko, Chuan-Chuan Liu, Po-Jui Hsu, Kuang-Chun Hu, Chung-Lieh Hung, Lo-Yip Yu, Yun-Chieh Huang, Shou-Chuan Shih
Medicine.2022; 101(32): e29609. CrossRef - Brachial-ankle pulse wave velocity as a predictor of long-term cardiovascular events in 2174 subjects with type 2 diabetes mellitus: A retrospective cohort study
Hack-Lyoung Kim, Won Kyeong Jeon, Hyun Sung Joh, Woo-Hyun Lim, Jae-Bin Seo, Sang-Hyun Kim, Joo-Hee Zo, Myung-A Kim
Medicine.2022; 101(45): e31758. CrossRef - Ultrasound Methods in the Evaluation of Atherosclerosis: From Pathophysiology to Clinic
Gabriel Cismaru, Teodora Serban, Alexandru Tirpe
Biomedicines.2021; 9(4): 418. CrossRef - A model to predict risk of stroke in middle-aged adults with type 2 diabetes generated from a nationwide population-based cohort study in Korea
Mee-Kyoung Kim, Kyungdo Han, Jae-Hyoung Cho, Hyuk-Sang Kwon, Kun-Ho Yoon, Seung-Hwan Lee
Diabetes Research and Clinical Practice.2020; 163: 108157. CrossRef - Association of impaired arterial wall properties with the presence of coronary artery disease in patients with abdominal aortic aneurysms
Pinelopi Rafouli‐Stergiou, Ignatios Ikonomidis, Niki Katsiki, Nikolaos P. E. Kadoglou, Stefanos Vlachos, John Thymis, John Parissis, Konstantinos G. Moulakakis, John D. Kakisis
The Journal of Clinical Hypertension.2020; 22(2): 187. CrossRef - Association of serum FAM19A5 with metabolic and vascular risk factors in human subjects with or without type 2 diabetes
You-Bin Lee, Hwan-Jin Hwang, Jung A Kim, Soon Young Hwang, Eun Roh, So-hyeon Hong, Kyung Mook Choi, Sei Hyun Baik, Hye Jin Yoo
Diabetes and Vascular Disease Research.2019; 16(6): 530. CrossRef - Pulse Wave Velocity in Atherosclerosis
Hack-Lyoung Kim, Sang-Hyun Kim
Frontiers in Cardiovascular Medicine.2019;[Epub] CrossRef

 KES
KES
 PubReader
PubReader ePub Link
ePub Link Cite
Cite