Search
- Page Path
- HOME > Search
- Diabetes, obesity and metabolism
- Performance of Simple Fibrosis Score in Non-Alcoholic Fatty Liver Disease with and without Type 2 Diabetes
- Seung Min Chung, Min Kyu Kang, Jun Sung Moon, Jung Gil Park
- Endocrinol Metab. 2023;38(2):277-281. Published online March 13, 2023
- DOI: https://doi.org/10.3803/EnM.2022.1635
- 1,819 View
- 97 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
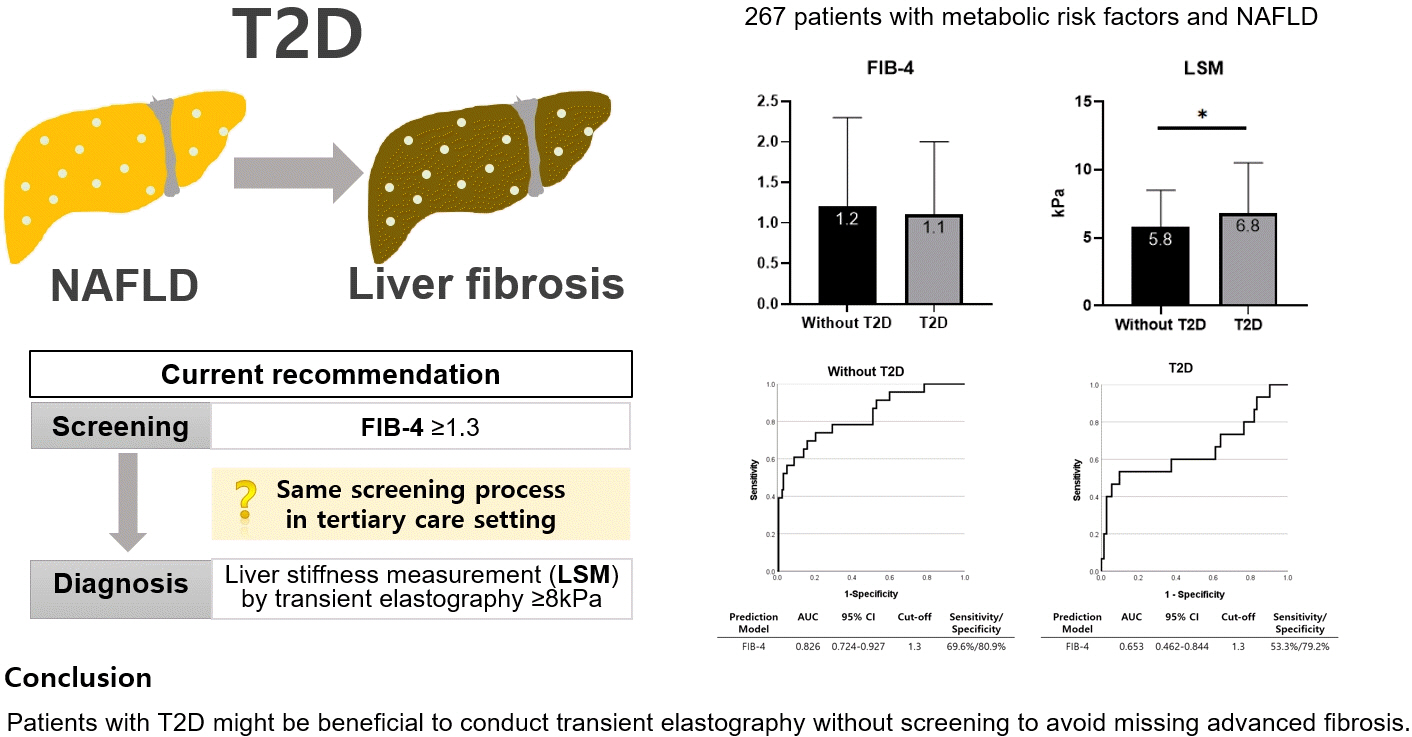
ePub - This cross-sectional study enrolled 267 patients with metabolic risk factors and established non-alcoholic fatty liver disease in the prospective cohort. The performance of fibrosis-4 (FIB-4) score (≥1.3) to diagnose advanced fibrosis using transient elastography (liver stiffness measurement [LSM] ≥8 kPa) was analyzed. Comparing patients with type 2 diabetes (T2D, n=87) and without (n=180), not FIB-4, but LSM was significantly higher in T2D (P=0.026). The prevalence of advanced fibrosis was 17.2% in T2D and 12.8% in non-T2D. FIB-4 exhibited higher proportion of false negatives in T2D patients (10.9%) than those without (5.2%). The diagnostic performance of FIB-4 was suboptimal in T2D (area under curve [AUC], 0.653; 95% confidence interval [CI], 0.462 to 0.844) compared to that in non-T2D (AUC, 0.826; 95% CI, 0.724 to 0.927). In conclusion, patients with T2D might be beneficial to conduct transient elastography without screening to avoid missing advanced fibrosis.
-
Citations
Citations to this article as recorded by- Prevalence of High and Moderate Risk of Liver Fibrosis Among Patients With Diabetes at a Noncommunicable Diseases (NCD) Clinic in a Primary Healthcare Center in Northern India
Anubhav Mondal, Aninda Debnath, Ghurumourthy Dhandapani, Abhishek Sharma, Shveta Lukhmana, Geeta Yadav
Cureus.2023;[Epub] CrossRef
- Prevalence of High and Moderate Risk of Liver Fibrosis Among Patients With Diabetes at a Noncommunicable Diseases (NCD) Clinic in a Primary Healthcare Center in Northern India

- Thyroid
Thyroid Cancer Screening - Survival Comparison of Incidentally Found versus Clinically Detected Thyroid Cancers: An Analysis of a Nationwide Cohort Study
- Shinje Moon, Eun Kyung Lee, Hoonsung Choi, Sue K. Park, Young Joo Park
- Endocrinol Metab. 2023;38(1):81-92. Published online February 27, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1668
- 1,734 View
- 154 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The true benefit of thyroid cancer screening is incompletely understood. This study investigated the impact of ultrasound screening on thyroid cancer outcomes through a comparison with symptomatic thyroid cancer using data from a nationwide cohort study in Korea.
Methods
Cox regression analysis was performed to assess the hazard ratios (HRs) for all-cause and thyroid cancer-specific mortality. Considering the possible bias arising from age, sex, year of thyroid cancer registration, and confounding factors for mortality (including smoking/drinking status, diabetes, and hypertension), all analyses were conducted with stabilized inverse probability of treatment weighting (IPTW) according to the route of detection.
Results
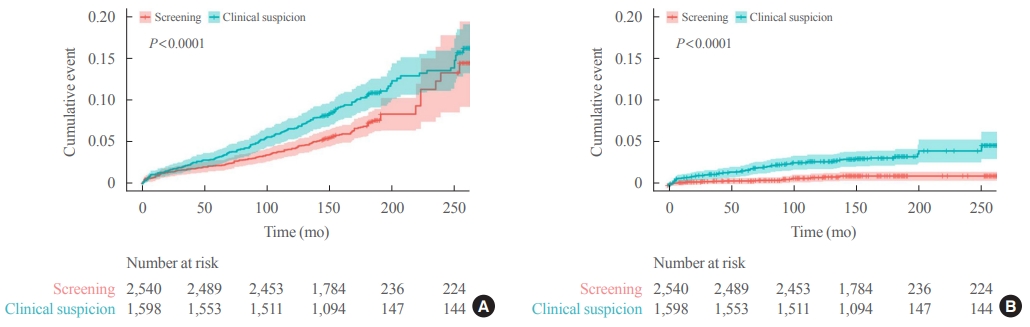
Of 5,796 patients with thyroid cancer, 4,145 were included and 1,651 were excluded due to insufficient data. In comparison with the screening group, the clinical suspicion group was associated with large tumors (17.2±14.6 mm vs. 10.4±7.9 mm), advanced T stage (3–4) (odds ratio [OR], 1.24; 95% confidence interval [CI], 1.09 to 1.41), extrathyroidal extension (OR, 1.16; 95% CI, 1.02 to 1.32), and advanced stage (III–IV) (OR, 1.16; 95% CI, 1.00 to 1.35). In IPTW-adjusted Cox regression analysis, the clinical suspicion group had significantly higher risks of all-cause mortality (HR, 1.43; 95% CI, 1.14 to 1.80) and thyroid cancer-specific mortality (HR, 3.07; 95% CI, 1.77 to 5.29). Mediation analysis showed that the presence of thyroid-specific symptoms was directly associated with a higher risk of cancer-specific mortality. Thyroid-specific symptoms also indirectly affected thyroid cancer-specific mortality, mediated by tumor size and advanced clinicopathologic status.
Conclusion
Our findings provide important evidence for the survival benefit of early detection of thyroid cancer compared to symptomatic thyroid cancer. -
Citations
Citations to this article as recorded by- Cost-Utility Analysis of Early Detection with Ultrasonography of Differentiated Thyroid Cancer: A Retrospective Study on a Korean Population
Han-Sang Baek, Jeonghoon Ha, Kwangsoon Kim, Ja Seong Bae, Jeong Soo Kim, Sungju Kim, Dong-Jun Lim, Chul-Min Kim
Endocrinology and Metabolism.2024; 39(2): 310. CrossRef - Clinical Characteristics, Diagnostic Approach and Outcome of Thyroid Incidental Findings vs. Clinically Overt Thyroid Nodules: An Observational Single-Centre Study
Tom Jansen, Nike Stikkelbroeck, Annenienke van de Ven, Ilse van Engen-van Grunsven, Marcel Janssen, Han Bonenkamp, Martin Gotthardt, Romana T. Netea-Maier
Cancers.2023; 15(8): 2350. CrossRef - Lower Thyroid Cancer Mortality in Patients Detected by Screening: A Meta-Analysis
Shinje Moon, Young Shin Song, Kyong Yeun Jung, Eun Kyung Lee, Young Joo Park
Endocrinology and Metabolism.2023; 38(1): 93. CrossRef - To Screen or Not to Screen?
Do Joon Park
Endocrinology and Metabolism.2023; 38(1): 69. CrossRef - The 2017 United States Preventive Services Task Force Recommendation for Thyroid Cancer Screening Is No Longer the Gold Standard
Ka Hee Yi
Endocrinology and Metabolism.2023; 38(1): 72. CrossRef - Thyroid Cancer Screening: How to Maximize Its Benefits and Minimize Its Harms
Jung Hwan Baek
Endocrinology and Metabolism.2023; 38(1): 75. CrossRef
- Cost-Utility Analysis of Early Detection with Ultrasonography of Differentiated Thyroid Cancer: A Retrospective Study on a Korean Population

- Thyroid
Thyroid Cancer Screening - Lower Thyroid Cancer Mortality in Patients Detected by Screening: A Meta-Analysis
- Shinje Moon, Young Shin Song, Kyong Yeun Jung, Eun Kyung Lee, Young Joo Park
- Endocrinol Metab. 2023;38(1):93-103. Published online February 27, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1667
- 2,184 View
- 117 Download
- 3 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Thyroid cancer screening has contributed to the skyrocketing prevalence of thyroid cancer. However, the true benefit of thyroid cancer screening is not fully understood. This study aimed to evaluate the impact of screening on the clinical outcomes of thyroid cancer by comparing incidental thyroid cancer (ITC) with non-incidental thyroid cancer (NITC) through a meta-analysis.
Methods
PubMed and Embase were searched from inception to September 2022. We estimated and compared the prevalence of high-risk features (aggressive histology of thyroid cancer, extrathyroidal extension, metastasis to regional lymph nodes or distant organs, and advanced tumor-node-metastasis [TNM] stage), thyroid cancer-specific death, and recurrence in the ITC and NITC groups. We also calculated pooled risks and 95% confidence intervals (CIs) of the outcomes derived from these two groups.
Results
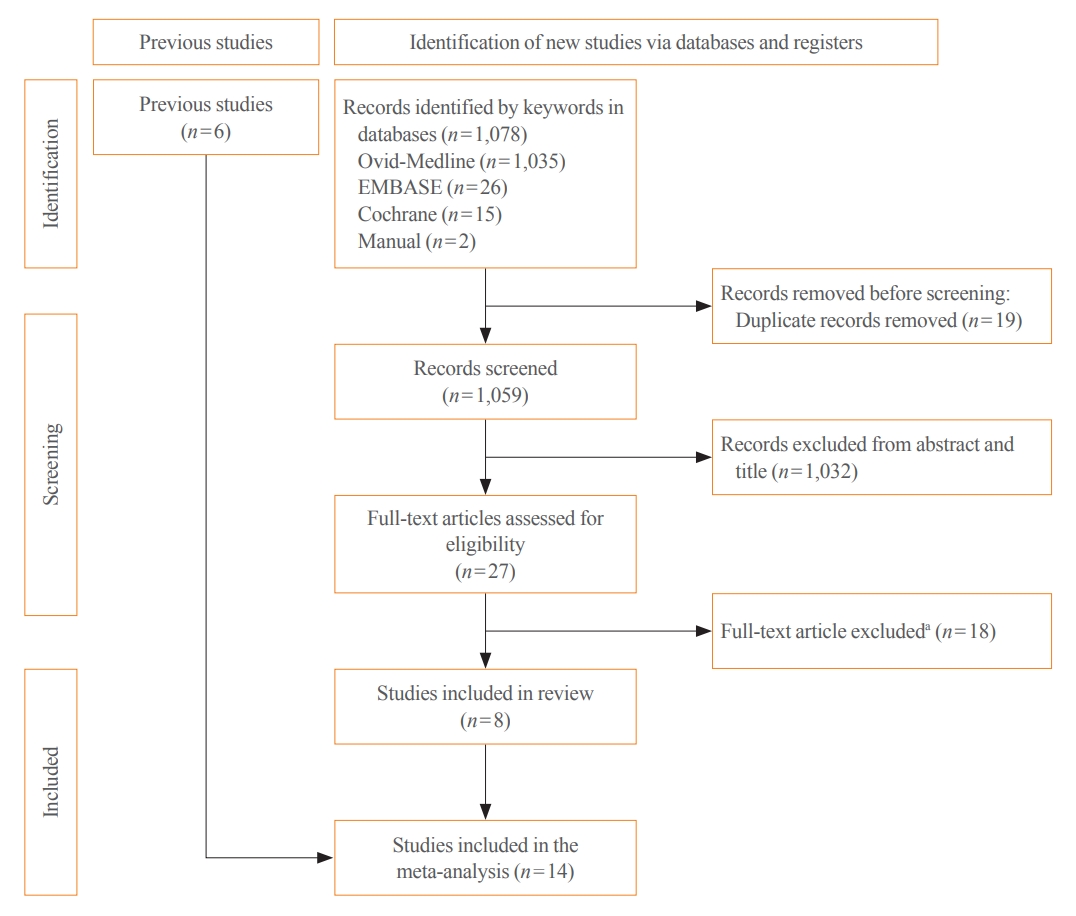
From 1,078 studies screened, 14 were included. In comparison to NITC, the ITC group had a lower incidence of aggressive histology (odds ratio [OR], 0.46; 95% CI, 0.31 to 0.7), smaller tumors (mean difference, −7.9 mm; 95% CI, −10.2 to −5.6), lymph node metastasis (OR, 0.64; 95% CI, 0.48 to 0.86), and distant metastasis (OR, 0.42; 95% CI, 0.23 to 0.77). The risks of recurrence and thyroid cancer-specific mortality were also lower in the ITC group (OR, 0.42; 95% CI, 0.25 to 0.71 and OR, 0.46; 95% CI, 0.28 to 0.74) than in the NITC group.
Conclusion
Our findings provide important evidence of a survival benefit from the early detection of thyroid cancer compared to symptomatic thyroid cancer. -
Citations
Citations to this article as recorded by- To Screen or Not to Screen?
Do Joon Park
Endocrinology and Metabolism.2023; 38(1): 69. CrossRef - The 2017 United States Preventive Services Task Force Recommendation for Thyroid Cancer Screening Is No Longer the Gold Standard
Ka Hee Yi
Endocrinology and Metabolism.2023; 38(1): 72. CrossRef - Thyroid Cancer Screening: How to Maximize Its Benefits and Minimize Its Harms
Jung Hwan Baek
Endocrinology and Metabolism.2023; 38(1): 75. CrossRef - Delayed Surgery for and Outcomes of Papillary Thyroid Cancer: Is the Pendulum Still Swinging?
Giorgio Grani
Clinical Thyroidology.2023; 35(5): 192. CrossRef
- To Screen or Not to Screen?

- Calcium & Bone Metabolism
- Bone Mineral Density Screening Interval and Transition to Osteoporosis in Asian Women
- Hyunju Park, Heera Yang, Jung Heo, Hye Won Jang, Jae Hoon Chung, Tae Hyuk Kim, Yong-Ki Min, Sun Wook Kim
- Endocrinol Metab. 2022;37(3):506-512. Published online June 9, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1429

- 3,049 View
- 103 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Bone mineral density (BMD) testing is indicated for women aged 65 years, but screening strategies for osteoporosis are controversial. Currently, there is no study focusing on the BMD testing interval in Asian populations. The current study aimed to evaluate the estimated time interval for screening osteoporosis.
Methods
We conducted a study of 6,385 subjects aged 50 years and older who underwent dual-energy X-ray absorptiometry screening more than twice at Samsung Medical Center as participants in a routine health checkup. Subjects were divided based on baseline T-score into mild osteopenia (T-score, <–1.0 to >–1.5), moderate osteopenia (T-score, ≤–1.5 to >–2.0), and severe osteopenia (T-score, ≤–2.0 to >–2.5). Information about personal medical and social history was collected by a structured questionnaire.
Results
The adjusted estimated BMD testing interval for 10% of the subjects to develop osteoporosis was 13.2 years in mild osteopenia, 5.0 years in moderate osteopenia, and 1.5 years in severe osteopenia.
Conclusion
Our study provides extended information about BMD screening intervals in Asian female population. Baseline T-score was important for predicting BMD screening interval, and repeat BMD testing within 5 years might not be necessary in mild osteopenia subjects. -
Citations
Citations to this article as recorded by- Effects of Bazedoxifene/Vitamin D Combination Therapy on Serum Vitamin D Levels and Bone Turnover Markers in Postmenopausal Women with Osteopenia: A Randomized Controlled Trial
Chaiho Jeong, Jeonghoon Ha, Jun-Il Yoo, Young-Kyun Lee, Jung Hee Kim, Yong-Chan Ha, Yong-Ki Min, Dong-Won Byun, Ki-Hyun Baek, Ho Yeon Chung
Journal of Bone Metabolism.2023; 30(2): 189. CrossRef - Bone-modifying agents for non–small-cell lung cancer patients with bone metastases during the era of immune checkpoint inhibitors: A narrative review
Jinyoung Kim, Chaiho Jeong, Jeongmin Lee, Jeonghoon Ha, Ki-Hyun Baek, Seohyun Kim, Tai Joon An, Chan Kwon Park, Hyoung Kyu Yoon, Jeong Uk Lim
Seminars in Oncology.2023; 50(3-5): 105. CrossRef
- Effects of Bazedoxifene/Vitamin D Combination Therapy on Serum Vitamin D Levels and Bone Turnover Markers in Postmenopausal Women with Osteopenia: A Randomized Controlled Trial

- Calcium & Bone Metabolism
- Computed Tomography-Derived Skeletal Muscle Radiodensity Is an Early, Sensitive Marker of Age-Related Musculoskeletal Changes in Healthy Adults
- Yeon Woo Jung, Namki Hong, Joon Chae Na, Woong Kyu Han, Yumie Rhee
- Endocrinol Metab. 2021;36(6):1201-1210. Published online December 13, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1206
- 3,707 View
- 135 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
A decrease in computed tomography (CT)-derived skeletal muscle radiodensity (SMD) reflects age-related ectopic fat infiltration of muscle, compromising muscle function and metabolism. We investigated the age-related trajectory of SMD and its association with vertebral trabecular bone density in healthy adults.
Methods
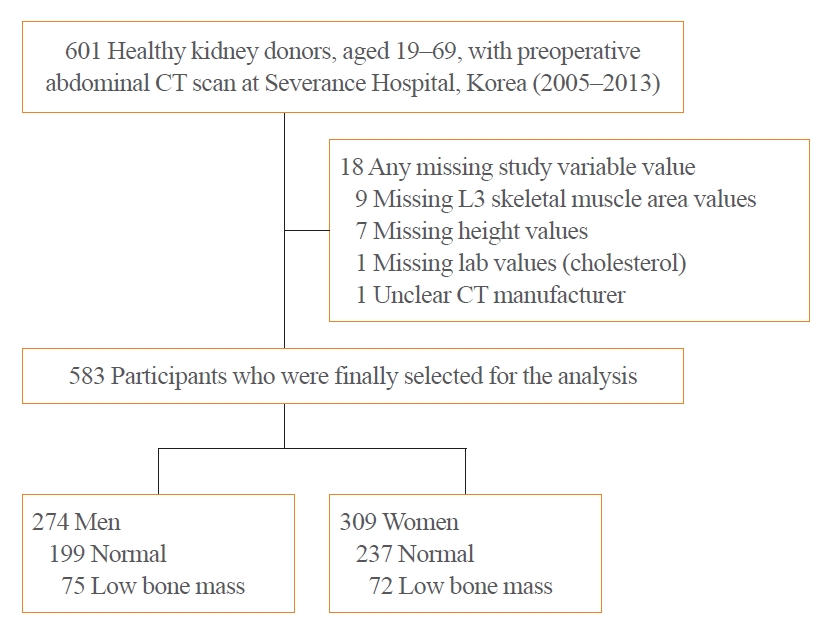
In a cohort of healthy adult kidney donors aged 19 to 69 years (n=583), skeletal muscle index (SMI, skeletal muscle area/height2), SMD, and visceral-to-subcutaneous fat (V/S) ratio were analyzed at the level of L3 from preoperative CT scans. Low bone mass was defined as an L1 trabecular Hounsfield unit (HU) <160 HU.
Results
L3SMD showed constant decline from the second decade (annual change –0.38% and –0.43% in men and women), whereas the decline of L3SMI became evident only after the fourth decade of life (–0.37% and –0.18% in men and women). One HU decline in L3SMD was associated with elevated odds of low bone mass (adjusted odds ratio, 1.07; 95% confidence interval, 1.02 to 1.13; P=0.003), independent of L3SMI, age, sex, and V/S ratio, with better discriminatory ability compared to L3SMI (area under the receiver-operating characteristics curve 0.68 vs. 0.53, P<0.001). L3SMD improved the identification of low bone mass when added to age, sex, V/S ratio, and L3SMI (category-free net reclassification improvement 0.349, P<0.001; integrated discrimination improvement 0.015, P=0.0165).
Conclusion
L3SMD can be an early marker for age-related musculoskeletal changes showing linear decline throughout life from the second decade in healthy adults, with potential diagnostic value for individuals with low bone mass. -
Citations
Citations to this article as recorded by- A review of radiological definitions of sarcopenia in cancer
James W. Wang, Jiarong Chen, Alison H. McGregor, Matthew Williams
JCSM Clinical Reports.2023; 8(2): 36. CrossRef - Weight‐adjusted waist as an integrated index for fat, muscle and bone health in adults
Kyoung Jin Kim, Serhim Son, Kyeong Jin Kim, Sin Gon Kim, Nam Hoon Kim
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(5): 2196. CrossRef
- A review of radiological definitions of sarcopenia in cancer

- Diabetes, Obesity and Metabolism
- Non-Laboratory-Based Simple Screening Model for Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Developed Using Multi-Center Cohorts
- Jiwon Kim, Minyoung Lee, Soo Yeon Kim, Ji-Hye Kim, Ji Sun Nam, Sung Wan Chun, Se Eun Park, Kwang Joon Kim, Yong-ho Lee, Joo Young Nam, Eun Seok Kang
- Endocrinol Metab. 2021;36(4):823-834. Published online August 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1074
- 4,435 View
- 137 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Nonalcoholic fatty liver disease (NAFLD) is the most prevalent cause of chronic liver disease worldwide. Type 2 diabetes mellitus (T2DM) is a risk factor that accelerates NAFLD progression, leading to fibrosis and cirrhosis. Thus, here we aimed to develop a simple model to predict the presence of NAFLD based on clinical parameters of patients with T2DM.
Methods
A total of 698 patients with T2DM who visited five medical centers were included. NAFLD was evaluated using transient elastography. Univariate logistic regression analyses were performed to identify potential contributors to NAFLD, followed by multivariable logistic regression analyses to create the final prediction model for NAFLD.
Results
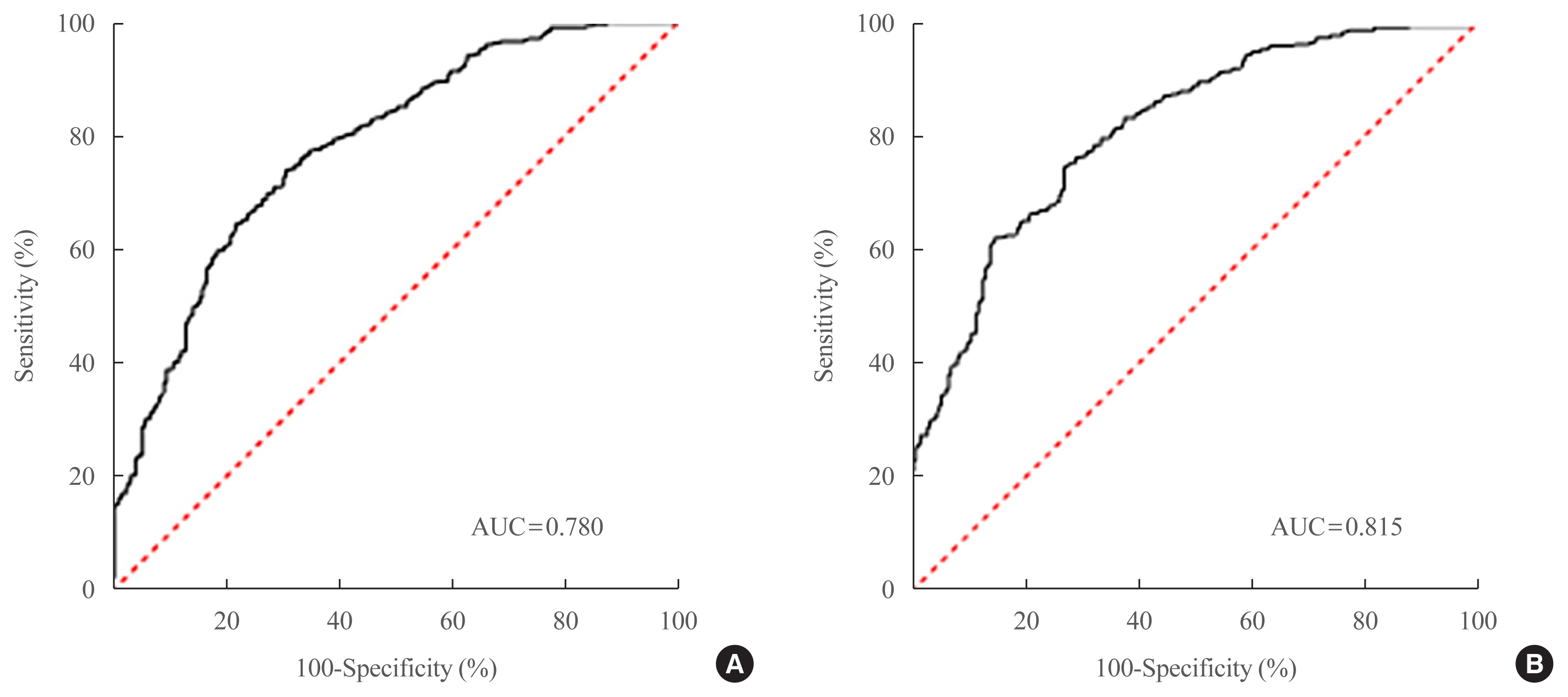
Two NAFLD prediction models were developed, with and without serum biomarker use. The non-laboratory model comprised six variables: age, sex, waist circumference, body mass index (BMI), dyslipidemia, and smoking status. For a cutoff value of ≥60, the prediction accuracy was 0.780 (95% confidence interval [CI], 0.743 to 0.817). The second comprehensive model showed an improved discrimination ability of up to 0.815 (95% CI, 0.782 to 0.847) and comprised seven variables: age, sex, waist circumference, BMI, glycated hemoglobin, triglyceride, and alanine aminotransferase to aspartate aminotransferase ratio. Our non-laboratory model showed non-inferiority in the prediction of NAFLD versus previously established models, including serum parameters.
Conclusion
The new models are simple and user-friendly screening methods that can identify individuals with T2DM who are at high-risk for NAFLD. Additional studies are warranted to validate these new models as useful predictive tools for NAFLD in clinical practice. -
Citations
Citations to this article as recorded by- Non-Alcoholic Fatty Liver Disease or Type 2 Diabetes Mellitus—The Chicken or the Egg Dilemma
Marcin Kosmalski, Agnieszka Śliwińska, Józef Drzewoski
Biomedicines.2023; 11(4): 1097. CrossRef
- Non-Alcoholic Fatty Liver Disease or Type 2 Diabetes Mellitus—The Chicken or the Egg Dilemma

- Obesity and Metabolism
- Current Challenges in Diabetic Retinopathy: Are We Really Doing Better?
- Jae Hyuck Lee, Su Jeong Song
- Endocrinol Metab. 2016;31(2):254-257. Published online June 10, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.2.254
- 3,586 View
- 36 Download
- 8 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Management of diabetic complications has been a worldwide major global health issue for decades. Recent studies from many parts of the world indicate improvement in this area. However, it is unknown if such an improvement is being realized in Koreans. Although there is limited information regarding diabetic retinopathy management among Koreans, recent epidemiologic studies have indicated improved screening rates and less frequent visual impairment among type 2 diabetics. Moreover, results achieved with new diagnostic and treatment modalities aimed to improve diabetic retinopathy management are encouraging for both physicians and patients.
-
Citations
Citations to this article as recorded by- Plasma amino acids and oxylipins as potential multi-biomarkers for predicting diabetic macular edema
Sang Youl Rhee, Eun Sung Jung, Dong Ho Suh, Su Jin Jeong, Kiyoung Kim, Suk Chon, Seung-Young Yu, Jeong-Taek Woo, Choong Hwan Lee
Scientific Reports.2021;[Epub] CrossRef - Urine protein: Urine creatinine ratio correlation with diabetic retinopathy
Samya Mujeeb, GladysR Rodrigues, RajeshR Nayak, AjayR Kamath, SumanaJ Kamath, Gurudutt Kamath
Indian Journal of Ophthalmology.2021; 69(11): 3359. CrossRef - Diabetic Retinopathy in the Asia-Pacific
Asia-Pacific Journal of Ophthalmology.2019;[Epub] CrossRef - Plasma glutamine and glutamic acid are potential biomarkers for predicting diabetic retinopathy
Sang Youl Rhee, Eun Sung Jung, Hye Min Park, Su Jin Jeong, Kiyoung Kim, Suk Chon, Seung-Young Yu, Jeong-Taek Woo, Choong Hwan Lee
Metabolomics.2018;[Epub] CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Normal-to-mildly increased albuminuria predicts the risk for diabetic retinopathy in patients with type 2 diabetes
Min-Kyung Lee, Kyung-Do Han, Jae-Hyuk Lee, Seo-Young Sohn, Oak-Kee Hong, Jee-Sun Jeong, Mee-Kyoung Kim, Ki-Hyun Baek, Ki-Ho Song, Hyuk-Sang Kwon
Scientific Reports.2017;[Epub] CrossRef
- Plasma amino acids and oxylipins as potential multi-biomarkers for predicting diabetic macular edema

- Clinical Study
- Diagnostic Role of Captopril Challenge Test in Korean Subjects with High Aldosterone-to-Renin Ratios
- Jung Hee Kim, Kyeong Seon Park, A Ram Hong, Chan Soo Shin, Seong Yeon Kim, Sang Wan Kim
- Endocrinol Metab. 2016;31(2):277-283. Published online May 13, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.2.277
- 5,279 View
- 53 Download
- 14 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Diagnosis of primary aldosteronism (PA) begins with aldosterone-to-renin ratio (ARR) measurement followed by confirmative tests. However, the ARR has high false positive rates which led to unnecessary confirmatory tests. Captopril challenge test (CCT) has been used as one of confirmatory tests, but the accuracy of it in the diagnosis of PA is still controversial. We aimed to examine the clinical efficacy of CCT as a post-screening test in PA.
Methods In a prospective study, we enrolled subjects with suspected PA who had hypertension and ARR >20 (ng/dL)/(ng/mL/hr). Sixty-four patients who underwent both the saline infusion test and the CCT were included.
Results The diagnostic performance of plasma aldosterone concentration (PAC) post-CCT was greater than that of ARR post-CCT and ARR pre-CCT in PA (area under the curve=0.956, 0.797, and 0.748, respectively;
P =0.001). A cut-off value of 13 ng/dL showed the highest diagnostic odds ratio considering PAC post-CCT at 60 and 90 minutes. A PAC post-CCT of 19 ng/dL had a specificity of 100%, which can be used as a cut-off value for the confirmative test. Determining the diagnostic performance of PAC post-CCT at 90 minutes was sufficient for PA diagnosis. Subjects with PAC post-CCT at 90 minutes <13 ng/dL are less likely to have PA, and those with PAC post-CCT at 90 minutes ≥13 but <19 ng/dL should undergo secondary confirmatory tests.Conclusion The CCT test may be a reliable post-screening test to avoid the hospitalization in the setting of falsely elevated ARR screening tests.
-
Citations
Citations to this article as recorded by- Exclusion Tests in Unilateral Primary Aldosteronism (ExcluPA) Study
Rui Zhu, Tungalagtamir Shagjaa, Giacomo Rossitto, Brasilina Caroccia, Teresa Maria Seccia, Dario Gregori, Gian Paolo Rossi
The Journal of Clinical Endocrinology & Metabolism.2023; 108(2): 496. CrossRef - Captopril challenge test in the diagnosis of primary aldosteronism: consistency between 1- and 2- h sampling
Xinyu Liu, Chao Guo, Jin Bian, Sufang Hao, Ying Lou, Huimin Zhang, Xianliang Zhou, Jun Cai, Wenjun Ma
Frontiers in Endocrinology.2023;[Epub] CrossRef - Performance of Confirmatory Tests for Diagnosing Primary Aldosteronism: a Systematic Review and Meta-Analysis
Alexander A. Leung, Christopher J. Symonds, Gregory L. Hundemer, Paul E. Ronksley, Diane L. Lorenzetti, Janice L. Pasieka, Adrian Harvey, Gregory A. Kline
Hypertension.2022; 79(8): 1835. CrossRef - Baseline Plasma Aldosterone Level and Renin Activity Allowing Omission of Confirmatory Testing in Primary Aldosteronism
Junji Kawashima, Eiichi Araki, Mitsuhide Naruse, Isao Kurihara, Katsutoshi Takahashi, Kouichi Tamura, Hiroki Kobayashi, Shintaro Okamura, Shozo Miyauchi, Koichi Yamamoto, Shoichiro Izawa, Tomoko Suzuki, Akiyo Tanabe
The Journal of Clinical Endocrinology & Metabolism.2020; 105(5): e1990. CrossRef - The number of positive confirmatory tests is associated with the clinical presentation and incidence of cardiovascular and cerebrovascular events in primary aldosteronism
Aya Saiki, Daisuke Tamada, Reiko Hayashi, Kosuke Mukai, Tetsuhiro Kitamura, Mitsuyoshi Takahara, Michio Otsuki, Iichiro Shimomura
Hypertension Research.2019; 42(8): 1186. CrossRef - The characteristics of captopril challenge test–positive patients using various criteria
Satoshi Kidoguchi, Naoki Sugano, Naomi Hayashi-Ishikawa, Norihiko Morisawa, Goro Tokudome, Takashi Yokoo
Journal of the Renin-Angiotensin-Aldosterone System.2019; 20(3): 147032031987089. CrossRef - Confirmatory tests for the diagnosis of primary aldosteronism: A systematic review and meta‐analysis
Sicen Wu, Jun Yang, Jinbo Hu, Ying Song, Wenwen He, Shumin Yang, Rong Luo, Qifu Li
Clinical Endocrinology.2019; 90(5): 641. CrossRef - The captopril challenge test for diagnosing primary Aldosteronism in a Chinese population
Ke-ying Zhu, Yan Zhang, Wen-jing Zhang, Hong-yun Li, Wen-huan Feng, Da-long Zhu, Ping Li
BMC Endocrine Disorders.2019;[Epub] CrossRef - Confirmatory Tests for the Diagnosis of Primary Aldosteronism
Ying Song, Shumin Yang, Wenwen He, Jinbo Hu, Qingfeng Cheng, Yue Wang, Ting Luo, Linqiang Ma, Qianna Zhen, Suhua Zhang, Mei Mei, Zhihong Wang, Hua Qing, Dennis Bruemmer, Bin Peng, Qifu Li
Hypertension.2018; 71(1): 118. CrossRef - Evaluation of the Saline Infusion Test and the Captopril Challenge Test in Chinese Patients With Primary Aldosteronism
Xiao Meng, Yanyan Li, Xiaohao Wang, Jianwei Li, Yuping Liu, Yerong Yu
The Journal of Clinical Endocrinology & Metabolism.2018; 103(3): 853. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Optimal follow-up strategies for adrenal incidentalomas: reappraisal of the 2016 ESE-ENSAT guidelines in real clinical practice
A Ram Hong, Jung Hee Kim, Kyeong Seon Park, Kyong Young Kim, Ji Hyun Lee, Sung Hye Kong, Seo Young Lee, Chan Soo Shin, Sang Wan Kim, Seong Yeon Kim
European Journal of Endocrinology.2017; 177(6): 475. CrossRef - Agkihpin, a novel SVTLE from Gloydius halys Pallas, promotes platelet aggregation in vitro and inhibits thrombus formation in vivo in murine models of thrombosis
Huiqiong Xie, Miao Huang, Qiping Hu, Kejian Sun, Huayu Wu, Wei Shu, Xiaolong Li, Ling Fang
Toxicon.2016; 122: 78. CrossRef
- Exclusion Tests in Unilateral Primary Aldosteronism (ExcluPA) Study

- Early Detection of Medullary Thyroid Cancer by Screening of the RET Proto-oncogene Germ Line Point Mutation in Family Members Affected with Hereditary Medullary Thyroid Cancer .
- Sun Wook Kim, Tae Yong Kim, Young Joo Park, Won Bae Kim, Chan Soo Shin, Do Joon Park, Kyoung Soo Park, Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee
- J Korean Endocr Soc. 2001;16(1):54-64. Published online February 1, 2001
- 1,064 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Conventional biochemical screening for family members with hereditary medullary thyroid cancer (MTC) is associated with problems of sensitivity and, specificity and it frequently detects gene carriers only after disease progression. Molecular genetic screening tests that detect germ-line point mutations of the RET proto-oncogene has changed our approach to hereditary MTC. In this study we screened members of a large Korean family that had a history of hereditary MTC by a molecular genetic method and propose a therapeutic approach in managing the disorder. METHODS: Using DNA acquired from peripheral blood leukocytes of the index patient, we performed PCR and direct sequencing of exon 10 of the RET proto-oncogene. PCR-RFLP using an Mbo II restriction enzyme was performed on family members who were at risk of MTC according to the family pedigree. Basal serum calcitonin level was determined in family members who had a point mutation of the RET proto-oncogene and a pentagastrin stimulation test was performed in 3 members. RESULTS: Genetic analysis in the index case revealed a mutation in exon 10, codon 618 of the RET proto-oncogene (TGC to AGC). Out of 28 members who were at risk of MTC, 24 members participated in the screening test. 9 members tested positive for a mutation in the same chromosomal location as the index patient by PCR-RFLP. Basal serum calcitonins were above 100 pg/mL in 2 members. 3 members who had a RET point muatation but a normal basal serum calcitonin level participated in the pentagastrin stimulation test and the results were negative in all members. We found a small medullary thyroid carcinoma that had a diameter of 0.2 cm in a 16 years old boy according to a negative pentagastrin stimulation test and who had received a prophylactic total thyroidectomy. He had no evidence of a lymph node metastasis. CONCLUSION: We detected a germ-line mutation of the RET proto-oncogene in codon 618 of Exon 10 by a molecular genetic method in a family with a hereditary MTC and found 9 members that had a negative history of MTC but had a RET point mutation. There was a very small MTC found in a 16 years old boy who had a normal pentagastrin stimulation test result. Therefore, It is recommended that a prophylactic total thyroidectomy be performed as well as in members that have a mutation of the RET proto-oncogene because MTC can metastasize early in its disease course.'


 KES
KES

 First
First Prev
Prev



