Search
- Page Path
- HOME > Search
- Diabetes, obesity and metabolism
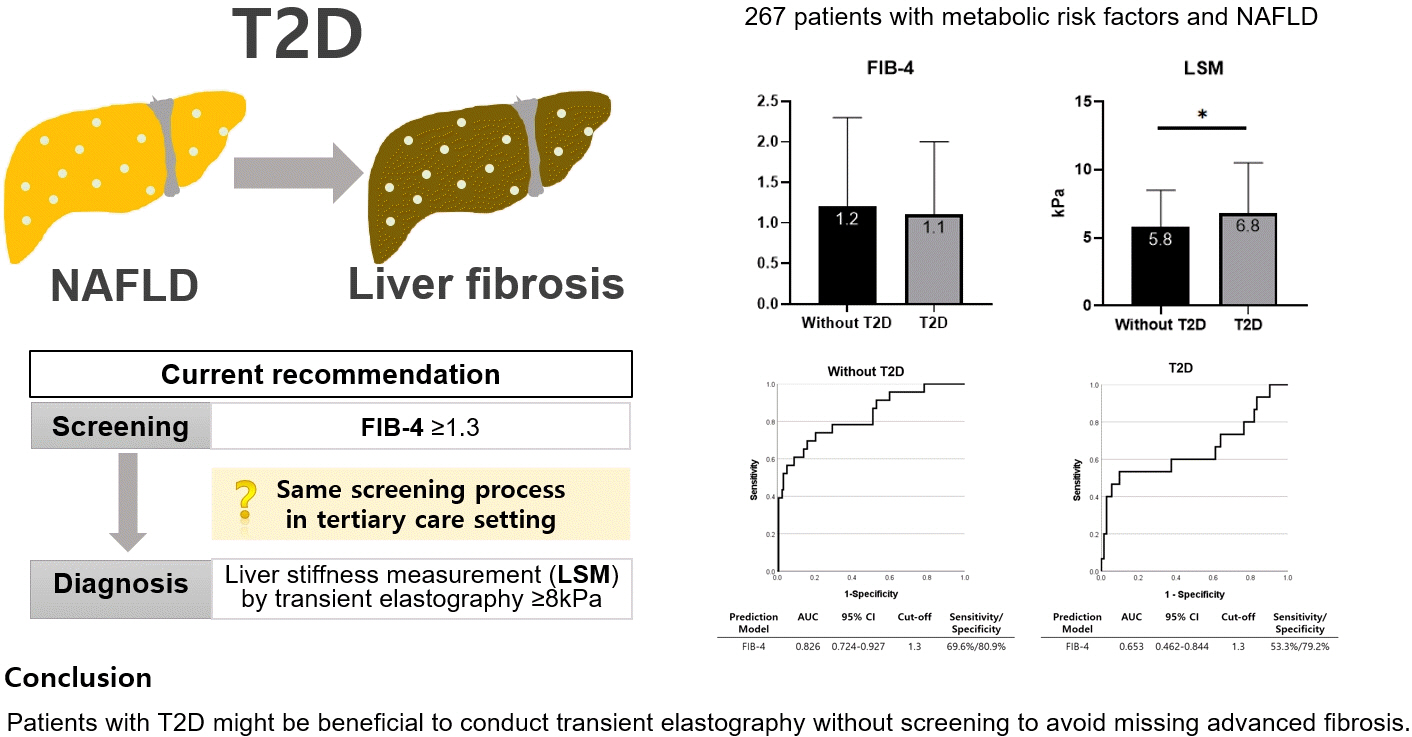
- Performance of Simple Fibrosis Score in Non-Alcoholic Fatty Liver Disease with and without Type 2 Diabetes
- Seung Min Chung, Min Kyu Kang, Jun Sung Moon, Jung Gil Park
- Endocrinol Metab. 2023;38(2):277-281. Published online March 13, 2023
- DOI: https://doi.org/10.3803/EnM.2022.1635
- 1,830 View
- 97 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - This cross-sectional study enrolled 267 patients with metabolic risk factors and established non-alcoholic fatty liver disease in the prospective cohort. The performance of fibrosis-4 (FIB-4) score (≥1.3) to diagnose advanced fibrosis using transient elastography (liver stiffness measurement [LSM] ≥8 kPa) was analyzed. Comparing patients with type 2 diabetes (T2D, n=87) and without (n=180), not FIB-4, but LSM was significantly higher in T2D (P=0.026). The prevalence of advanced fibrosis was 17.2% in T2D and 12.8% in non-T2D. FIB-4 exhibited higher proportion of false negatives in T2D patients (10.9%) than those without (5.2%). The diagnostic performance of FIB-4 was suboptimal in T2D (area under curve [AUC], 0.653; 95% confidence interval [CI], 0.462 to 0.844) compared to that in non-T2D (AUC, 0.826; 95% CI, 0.724 to 0.927). In conclusion, patients with T2D might be beneficial to conduct transient elastography without screening to avoid missing advanced fibrosis.
-
Citations
Citations to this article as recorded by- Prevalence of High and Moderate Risk of Liver Fibrosis Among Patients With Diabetes at a Noncommunicable Diseases (NCD) Clinic in a Primary Healthcare Center in Northern India
Anubhav Mondal, Aninda Debnath, Ghurumourthy Dhandapani, Abhishek Sharma, Shveta Lukhmana, Geeta Yadav
Cureus.2023;[Epub] CrossRef
- Prevalence of High and Moderate Risk of Liver Fibrosis Among Patients With Diabetes at a Noncommunicable Diseases (NCD) Clinic in a Primary Healthcare Center in Northern India

- Diabetes, Obesity and Metabolism
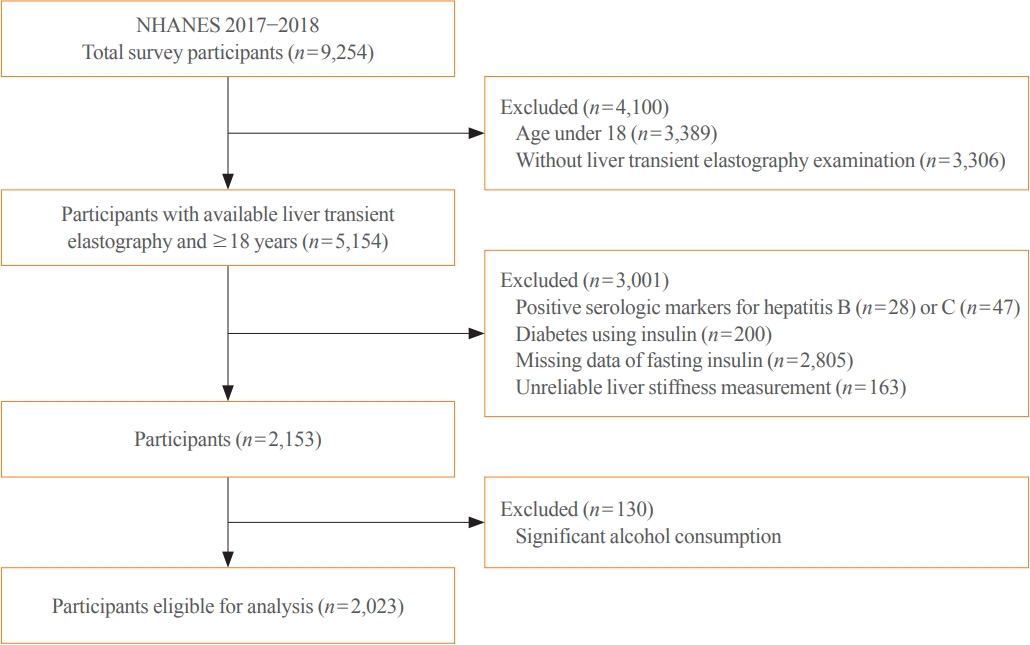
- The Impact of Insulin Resistance on Hepatic Fibrosis among United States Adults with Non-Alcoholic Fatty Liver Disease: NHANES 2017 to 2018
- Ji Cheol Bae, Lauren A. Beste, Kristina M. Utzschneider
- Endocrinol Metab. 2022;37(3):455-465. Published online June 21, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1434
- 4,208 View
- 135 Download
- 9 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
We aimed to investigate the association of hepatic steatosis with liver fibrosis and to assess the interactive effects of hepatic steatosis and insulin resistance on liver fibrosis in a nationally representative sample of United States adults.
Methods
We conducted a cross-sectional analysis using data from National Health and Nutrition Examination Survey 2017 to 2018, which for the first time included transient elastography to assess liver stiffness and hepatic steatosis. We evaluated the association between hepatic steatosis (using controlled attenuation parameter [CAP]) and clinically significant liver fibrosis (defined as liver stiffness ≥7.5 kPa) using logistic regression with an interaction term for hepatic steatosis and insulin resistance (defined as homeostatic model assessment of insulin resistance ≥3.0).
Results
Among adults undergoing transient elastography (n=2,023), 45.9% had moderate or greater hepatic steatosis and 11.3% had clinically significant liver fibrosis. After adjustment for demographic and metabolic factors, the odds of significant liver fibrosis increased as CAP score rose (odds ratio, 1.35 per standard deviation increment; 95% confidence interval, 1.11 to 1.64). We detected a significant interaction effect between CAP score and insulin resistance on the probability of significant liver fibrosis (P=0.016 for interaction). The probability of significant liver fibrosis increased in the presence of insulin resistance with increasing CAP score, while those without insulin resistance had low probability of significant liver fibrosis, even with high CAP scores.
Conclusion
Individuals with hepatic steatosis had higher odds of fibrosis when insulin resistance was present. Our findings emphasize the importance of the metabolic aspects of the disease on fibrosis risk and suggest a need to better identify patients with metabolic associated fatty liver disease. -
Citations
Citations to this article as recorded by- Association of insulin resistance indicators with hepatic steatosis and fibrosis in patients with metabolic syndrome
Tzu-chia Kuo, Yang-bor Lu, Chieh-lun Yang, Bin Wang, Lin-xin Chen, Ching-ping Su
BMC Gastroenterology.2024;[Epub] CrossRef - No More NAFLD: The Term Is Now MASLD
Ji Cheol Bae
Endocrinology and Metabolism.2024; 39(1): 92. CrossRef - Insulin Resistance/Sensitivity Measures as Screening Indicators of Metabolic-Associated Fatty Liver Disease and Liver Fibrosis
Mohammad E. Khamseh, Mojtaba Malek, Soodeh Jahangiri, Sohrab Nobarani, Azita Hekmatdoost, Marieh Salavatizadeh, Samira Soltanieh, Haleh Chehrehgosha, Hoda Taheri, Zeinab Montazeri, Fereshteh Attaran, Faramarz Ismail-Beigi, Fariba Alaei-Shahmiri
Digestive Diseases and Sciences.2024;[Epub] CrossRef - The association of Neuromedin U levels and non-alcoholic fatty liver disease: A comparative analysis
Murat Keskin, Sercan Avul, Aylin Beyaz, Nizameddin Koca
Heliyon.2024; 10(5): e27291. CrossRef - Oral Insulin Alleviates Liver Fibrosis and Reduces Liver Steatosis in Patients With Metabolic Dysfunction-associated Steatohepatitis and Type 2 Diabetes: Results of Phase II Randomized, Placebo-controlled Feasibility Clinical Trial
Yuval Ishay, Joel Neutel, Yotam Kolben, Ram Gelman, Orly Sneh Arbib, Oliver Lopez, Helena Katchman, Rizwana Mohseni, Miriam Kidron, Yaron Ilan
Gastro Hep Advances.2024; 3(3): 417. CrossRef - Comparative and Predictive Significance of Serum Leptin Levels in Non-alcoholic Fatty Liver Disease
Mehwish Qamar, Abeer Fatima, Ambreen Tauseef, Muhammad I Yousufzai, Ibrahim Liaqat, Qanbar Naqvi
Cureus.2024;[Epub] CrossRef - Greater Severity of Steatosis Is Associated with a Higher Risk of Incident Diabetes: A Retrospective Longitudinal Study
Ji Min Han, Jung Hwan Cho, Hye In Kim, Sunghwan Suh, Yu-Ji Lee, Jung Won Lee, Kwang Min Kim, Ji Cheol Bae
Endocrinology and Metabolism.2023; 38(4): 418. CrossRef - Hepatic T-cell senescence and exhaustion are implicated in the progression of fatty liver disease in patients with type 2 diabetes and mouse model with nonalcoholic steatohepatitis
Byeong Chang Sim, Yea Eun Kang, Sun Kyoung You, Seong Eun Lee, Ha Thi Nga, Ho Yeop Lee, Thi Linh Nguyen, Ji Sun Moon, Jingwen Tian, Hyo Ju Jang, Jeong Eun Lee, Hyon-Seung Yi
Cell Death & Disease.2023;[Epub] CrossRef - Familial clustering of nonalcoholic fatty liver disease in first‐degree relatives of adults with lean nonalcoholic fatty liver disease
Sorachat Niltwat, Chanin Limwongse, Natthinee Charatcharoenwitthaya, Duangkamon Bunditvorapoom, Wimolrak Bandidniyamanon, Phunchai Charatcharoenwitthaya
Liver International.2023; 43(12): 2713. CrossRef - Metabolic Score for Insulin Resistance Is Inversely Related to Incident Advanced Liver Fibrosis in Patients with Non-Alcoholic Fatty Liver Disease
Jun-Hyuk Lee, Yu-Jin Kwon, Kyongmin Park, Hye Sun Lee, Hoon-Ki Park, Jee Hye Han, Sang Bong Ahn
Nutrients.2022; 14(15): 3039. CrossRef - DPP-4 Inhibitor in Type 2 Diabetes Mellitus Patient with Non-Alcoholic Fatty Liver Disease: Achieving Two Goals at Once?
Ji Cheol Bae
Endocrinology and Metabolism.2022; 37(6): 858. CrossRef
- Association of insulin resistance indicators with hepatic steatosis and fibrosis in patients with metabolic syndrome

- Diabetes, Obesity and Metabolism
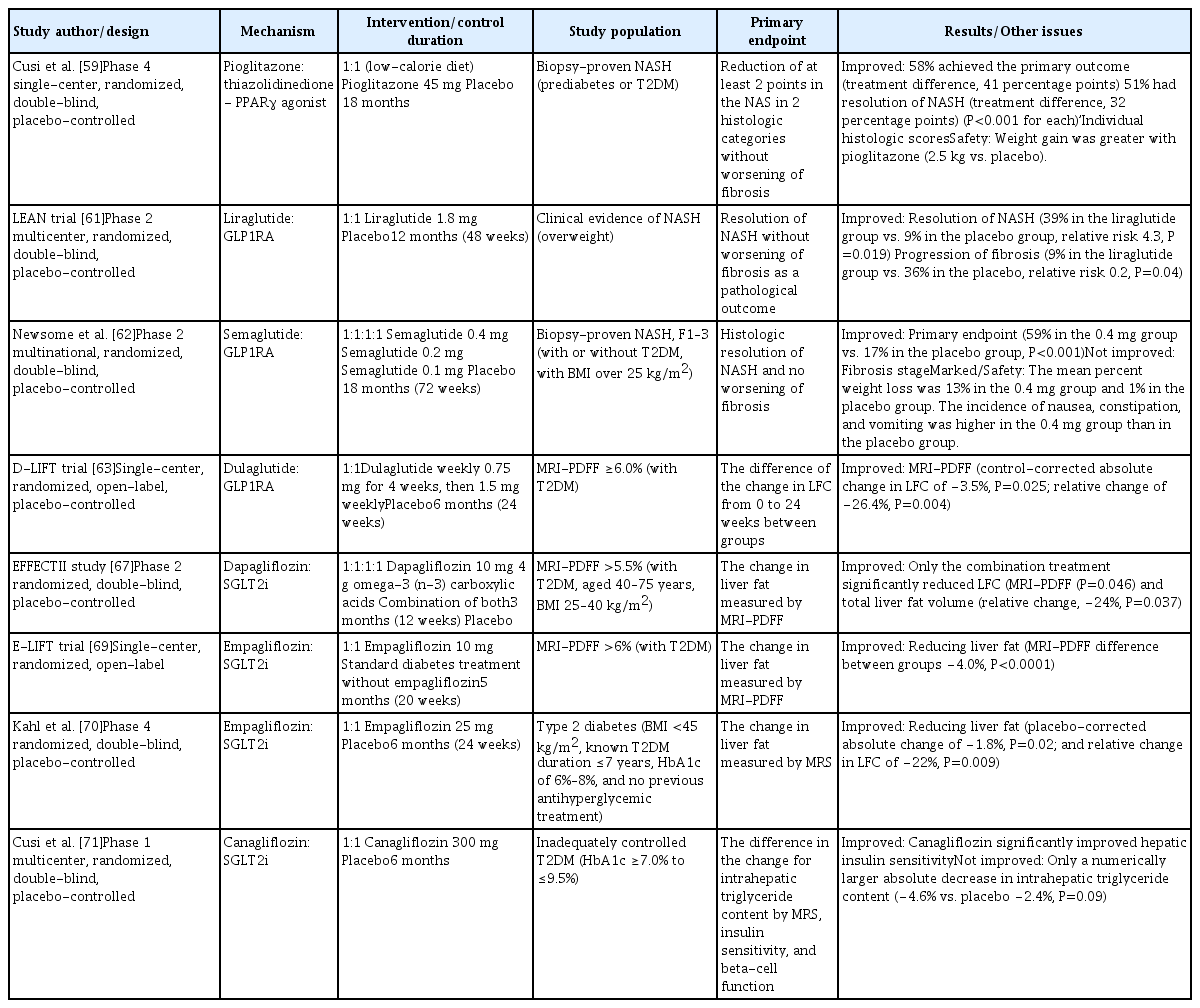
- State-of-the-Art Overview of the Pharmacological Treatment of Non-Alcoholic Steatohepatitis
- Yongin Cho, Yong-ho Lee
- Endocrinol Metab. 2022;37(1):38-52. Published online February 28, 2022
- DOI: https://doi.org/10.3803/EnM.2022.102
- 4,270 View
- 284 Download
- 2 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Non-alcoholic fatty liver disease (NAFLD) is the most common cause of chronic liver disease worldwide, and non-alcoholic steatohepatitis (NASH), a subtype of NAFLD, can progress to cirrhosis, hepatocellular carcinoma, and death. Nevertheless, the current treatment for NAFLD/NASH is limited to lifestyle modifications, and no drugs are currently officially approved as treatments for NASH. Many global pharmaceutical companies are pursuing the development of medications for the treatment of NASH, and results from phase 2 and 3 clinical trials have been published in recent years. Here, we review data from these recent clinical trials and reports on the efficacy of newly developed antidiabetic drugs in NASH treatment.
-
Citations
Citations to this article as recorded by- Association of non-alcoholic fatty liver disease with cardiovascular disease and all cause death in patients with type 2 diabetes mellitus: nationwide population based study
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
BMJ.2024; : e076388. CrossRef - Mitochondrial Quality Control: Its Role in Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD)
Soyeon Shin, Jaeyoung Kim, Ju Yeon Lee, Jun Kim, Chang-Myung Oh
Journal of Obesity & Metabolic Syndrome.2023; 32(4): 289. CrossRef - Sodium-glucose cotransporter 2 inhibitors for non-alcoholic fatty liver disease in patients with type 2 diabetes mellitus: A nationwide propensity-score matched cohort study
Jinyoung Kim, Kyungdo Han, Bongsung Kim, Ki-Hyun Baek, Ki-Ho Song, Mee Kyoung Kim, Hyuk-Sang Kwon
Diabetes Research and Clinical Practice.2022; 194: 110187. CrossRef
- Association of non-alcoholic fatty liver disease with cardiovascular disease and all cause death in patients with type 2 diabetes mellitus: nationwide population based study

- Diabetes, Obesity and Metabolism
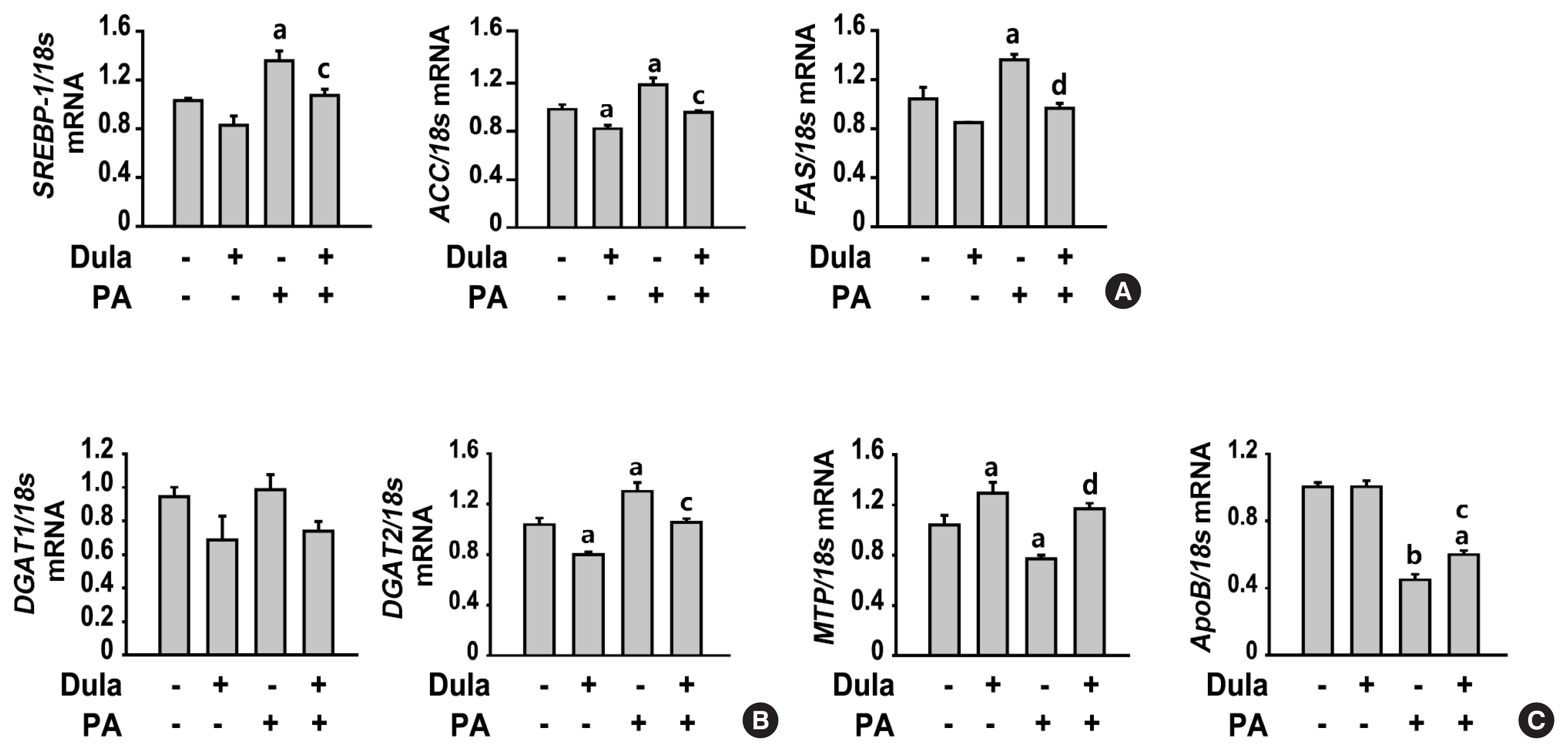
- Dulaglutide Ameliorates Palmitic Acid-Induced Hepatic Steatosis by Activating FAM3A Signaling Pathway
- Jinmi Lee, Seok-Woo Hong, Min-Jeong Kim, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
- Endocrinol Metab. 2022;37(1):74-83. Published online February 9, 2022
- DOI: https://doi.org/10.3803/EnM.2021.1293
- 4,904 View
- 235 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Dulaglutide, a long-acting glucagon-like peptide-1 receptor agonist (GLP-1RA), has been shown to reduce body weight and liver fat content in patients with type 2 diabetes. Family with sequence similarity 3 member A (FAM3A) plays a vital role in regulating glucose and lipid metabolism. The aim of this study was to determine the mechanisms by which dulaglutide protects against hepatic steatosis in HepG2 cells treated with palmitic acid (PA).
Methods
HepG2 cells were pretreated with 400 μM PA for 24 hours, followed by treatment with or without 100 nM dulaglutide for 24 hours. Hepatic lipid accumulation was determined using Oil red O staining and triglyceride (TG) assay, and the expression of lipid metabolism-associated factor was analyzed using quantitative real time polymerase chain reaction and Western blotting.
Results
Dulaglutide significantly decreased hepatic lipid accumulation and reduced the expression of genes associated with lipid droplet binding proteins, de novo lipogenesis, and TG synthesis in PA-treated HepG2 cells. Dulaglutide also increased the expression of proteins associated with lipolysis and fatty acid oxidation and FAM3A in PA-treated cells. However, exendin-(9-39), a GLP-1R antagonist, reversed the expression of FAM3A, and fatty acid oxidation-associated factors increased due to dulaglutide. In addition, inhibition of FAM3A by siRNA attenuated the reducing effect of dulaglutide on TG content and its increasing effect on regulation of fatty acid oxidation.
Conclusion
These results suggest that dulaglutide could be used therapeutically for improving nonalcoholic fatty liver disease, and its effect could be mediated in part via upregulation of FAM3A expression through a GLP-1R-dependent pathway. -
Citations
Citations to this article as recorded by- GLP-1/GLP-1RAs: New Options for the Drug Treatment of NAFLD
Haoran Jiang, Linquan Zang
Current Pharmaceutical Design.2024; 30(2): 100. CrossRef - GLP-1 Receptor Agonists in Non-Alcoholic Fatty Liver Disease: Current Evidence and Future Perspectives
Riccardo Nevola, Raffaella Epifani, Simona Imbriani, Giovanni Tortorella, Concetta Aprea, Raffaele Galiero, Luca Rinaldi, Raffaele Marfella, Ferdinando Carlo Sasso
International Journal of Molecular Sciences.2023; 24(2): 1703. CrossRef - FAM3A mediates the phenotypic switch of human aortic smooth muscle cells stimulated with oxidised low-density lipoprotein by influencing the PI3K-AKT pathway
Lei Yang, Baoshun Du, Shitao Zhang, Maode Wang
In Vitro Cellular & Developmental Biology - Animal.2023; 59(6): 431. CrossRef - ATP Secretion and Metabolism in Regulating Pancreatic Beta Cell Functions and Hepatic Glycolipid Metabolism
Jing Li, Han Yan, Rui Xiang, Weili Yang, Jingjing Ye, Ruili Yin, Jichun Yang, Yujing Chi
Frontiers in Physiology.2022;[Epub] CrossRef - Targeted therapeutics and novel signaling pathways in non-alcohol-associated fatty liver/steatohepatitis (NAFL/NASH)
Xiaohan Xu, Kyle L. Poulsen, Lijuan Wu, Shan Liu, Tatsunori Miyata, Qiaoling Song, Qingda Wei, Chenyang Zhao, Chunhua Lin, Jinbo Yang
Signal Transduction and Targeted Therapy.2022;[Epub] CrossRef
- GLP-1/GLP-1RAs: New Options for the Drug Treatment of NAFLD

- Diabetes, Obesity and Metabolism
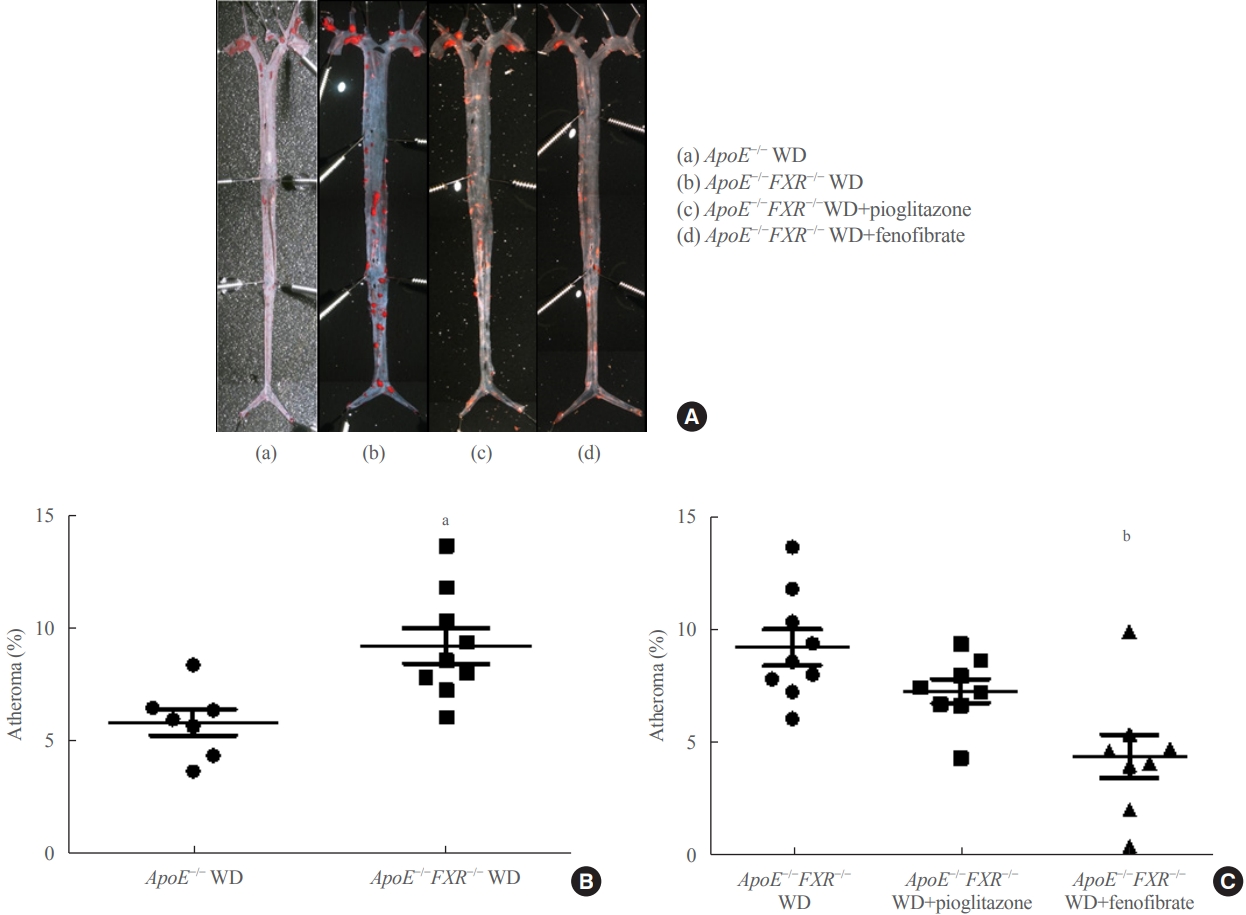
- The Effects of PPAR Agonists on Atherosclerosis and Nonalcoholic Fatty Liver Disease in ApoE−/−FXR−/− Mice
- Yenna Lee, Bo-Rahm Kim, Geun-Hyung Kang, Gwan Jae Lee, Young Joo Park, Haeryoung Kim, Hak Chul Jang, Sung Hee Choi
- Endocrinol Metab. 2021;36(6):1243-1253. Published online December 28, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1100
- 5,630 View
- 159 Download
- 11 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Farnesoid X receptor (FXR), a bile acid–activated nuclear receptor, is a potent regulator of glucose and lipid metabolism as well as of bile acid metabolism. Previous studies have demonstrated that FXR deficiency is associated with metabolic derangements, including atherosclerosis and nonalcoholic fatty liver disease (NAFLD), but its mechanism remains unclear. In this study, we investigated the role of FXR in atherosclerosis and NAFLD and the effect of peroxisome proliferator-activated receptor (PPAR) agonists in mouse models with FXR deficiency.
Methods
En face lipid accumulation analysis, liver histology, serum levels of glucose and lipids, and mRNA expression of genes related to lipid metabolism were compared between apolipoprotein E (ApoE)−/− and ApoE−/−FXR−/− mice. The effects of PPARα and PPARγ agonists were also compared in both groups of mice.
Results
Compared with ApoE−/− mice, ApoE−/−FXR−/− mice showed more severe atherosclerosis, hepatic steatosis, and higher levels of serum cholesterol, low-density lipoprotein cholesterol, and triglycerides, accompanied by increased mRNA expression of FAS, ApoC2, TNFα, IL-6 (liver), ATGL, TGH, HSL, and MGL (adipocytes), and decreased mRNA expressions of CPT2 (liver) and Tfam (skeletal muscle). Treatment with a PPARα agonist, but not with a PPARγ agonist, partly reversed atherosclerosis and hepatic steatosis, and decreased plasma triglyceride levels in the ApoE−/−FXR−/− mice, in association with increased mRNA expression of CD36 and FATP and decreased expression of ApoC2 and ApoC3 (liver).
Conclusion
Loss of FXR is associated with aggravation of atherosclerosis and hepatic steatosis in ApoE-deficient mice, which could be reversed by a PPARα agonist through induction of fatty acid uptake, β-oxidation, and triglyceride hydrolysis. -
Citations
Citations to this article as recorded by- Evaluation of the hepatotoxicity of Psoralea corylifolia L. based on a zebrafish model
Shu-Yan Gao, Jing-Cheng Zhao, Qing Xia, Chen Sun, Maimaiti Aili, Ainiwaer Talifu, Shi-Xia Huo, Yun Zhang, Zhi-Jian Li
Frontiers in Pharmacology.2024;[Epub] CrossRef - Advances in management of metabolic dysfunction-associated steatotic liver disease: from mechanisms to therapeutics
Yuxiao Jiang, Lili Wu, Xiaopeng Zhu, Hua Bian, Xin Gao, Mingfeng Xia
Lipids in Health and Disease.2024;[Epub] CrossRef - Mitochondrial carnitine palmitoyltransferase-II dysfunction: A possible novel mechanism for nonalcoholic fatty liver disease in hepatocarcinogenesis
Min Yao, Ping Zhou, Yan-Yan Qin, Li Wang, Deng-Fu Yao
World Journal of Gastroenterology.2023; 29(12): 1765. CrossRef - Emerging Roles of Gut Microbial Modulation of Bile Acid Composition in the Etiology of Cardiovascular Diseases
Tess Yntema, Debby P. Y. Koonen, Folkert Kuipers
Nutrients.2023; 15(8): 1850. CrossRef - The interplay between nonalcoholic fatty liver disease and atherosclerotic cardiovascular disease
Alexandra C. Finney, Sandeep Das, Dhananjay Kumar, M. Peyton McKinney, Bishuang Cai, Arif Yurdagul, Oren Rom
Frontiers in Cardiovascular Medicine.2023;[Epub] CrossRef - Targeting PPARs for therapy of atherosclerosis: A review
Miao Miao, Xue Wang, Tian Liu, Yan-Jie Li, Wen-Qian Yu, Tong-Mei Yang, Shou-Dong Guo
International Journal of Biological Macromolecules.2023; 242: 125008. CrossRef - Cabernet sauvignon dry red wine ameliorates atherosclerosis in mice by regulating inflammation and endothelial function, activating AMPK phosphorylation, and modulating gut microbiota
Xinlong Cheng, Xue Han, Liangfu Zhou, Yasai Sun, Qian Zhou, Xuan Lin, Zhe Gao, Jie Wang, Wen Zhao
Food Research International.2023; 169: 112942. CrossRef - Impacts of dietary lipids derived from animal or vegetable sources on healthy rats
Mostafa M Dalal, Gamal M Edrees, Hanaa A Hassan, Mamdouh Abdel-Mogib, Mai Alaa El-Dein
Egyptian Journal of Basic and Applied Sciences.2023; 10(1): 618. CrossRef - Whey protein hydrolysate alleviated atherosclerosis and hepatic steatosis by regulating lipid metabolism in apoE-/- mice fed a Western diet
Kai Wang, Zixin Fu, Xiaoyi Li, Hui Hong, Xin Zhan, Xiaohong Guo, Yongkang Luo, Yuqing Tan
Food Research International.2022; 157: 111419. CrossRef - Melatonin alleviates PM2.5‐induced glucose metabolism disorder and lipidome alteration by regulating endoplasmic reticulum stress
Zhou Du, Junjie Hu, Lisen Lin, Qingqing Liang, Mengqi Sun, Zhiwei Sun, Junchao Duan
Journal of Pineal Research.2022;[Epub] CrossRef - Lipoprotein Lipase: Is It a Magic Target for the Treatment of Hypertriglyceridemia
Joon Ho Moon, Kyuho Kim, Sung Hee Choi
Endocrinology and Metabolism.2022; 37(4): 575. CrossRef - The role of the gut microbiota in health and cardiovascular diseases
Lu Wang, Shiqi Wang, Qing Zhang, Chengqi He, Chenying Fu, Quan Wei
Molecular Biomedicine.2022;[Epub] CrossRef
- Evaluation of the hepatotoxicity of Psoralea corylifolia L. based on a zebrafish model

- Diabetes, Obesity and Metabolism
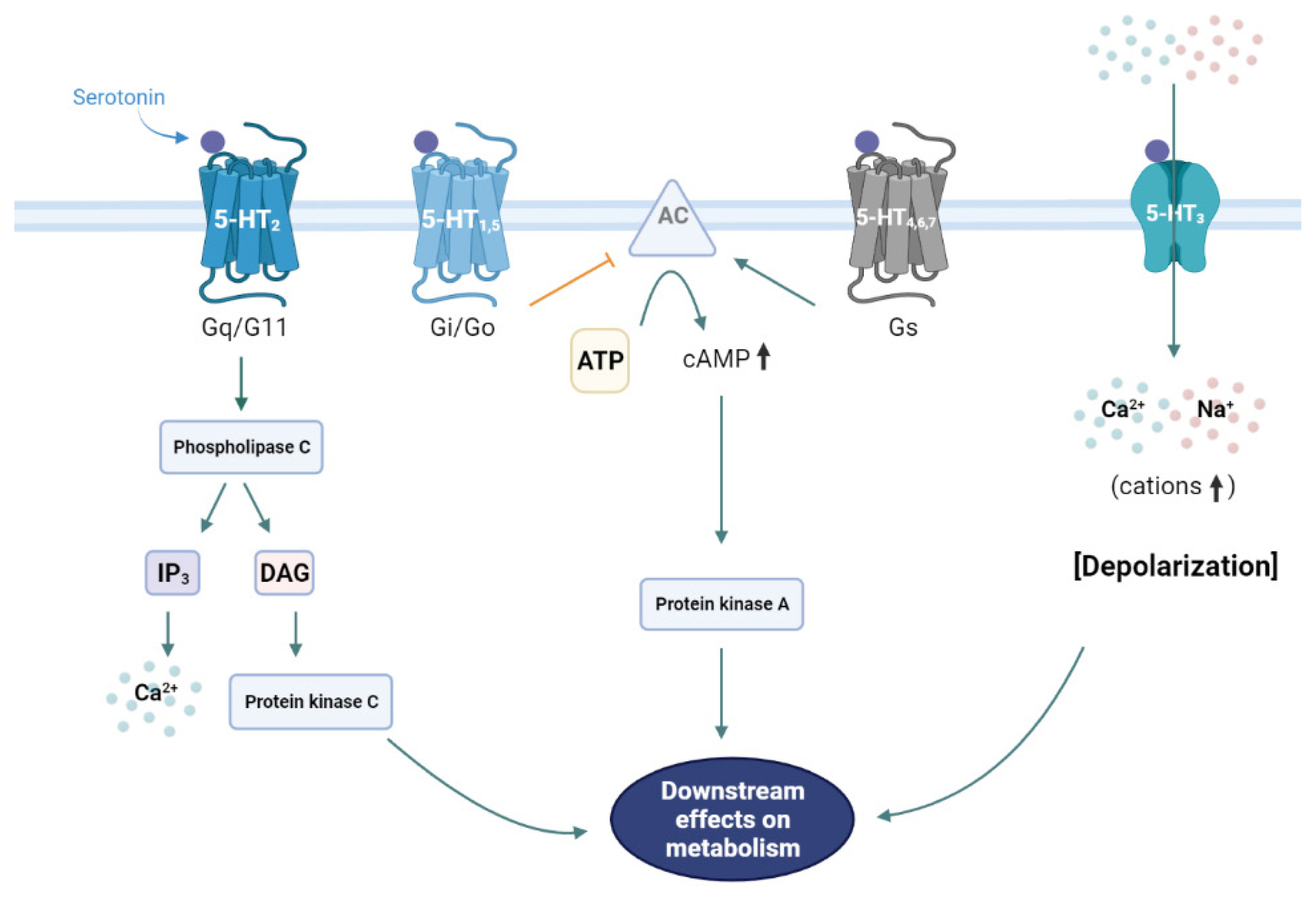
- Serotonergic Regulation of Hepatic Energy Metabolism
- Jiwon Park, Wooju Jeong, Chahyeon Yun, Hail Kim, Chang-Myung Oh
- Endocrinol Metab. 2021;36(6):1151-1160. Published online December 16, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1331
- 5,970 View
- 219 Download
- 7 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - The liver is a vital organ that regulates systemic energy metabolism and many physiological functions. Nonalcoholic fatty liver disease (NAFLD) is the commonest cause of chronic liver disease and end-stage liver failure. NAFLD is primarily caused by metabolic disruption of lipid and glucose homeostasis. Serotonin (5-hydroxytryptamine [5-HT]) is a biogenic amine with several functions in both the central and peripheral systems. 5-HT functions as a neurotransmitter in the brain and a hormone in peripheral tissues to regulate systemic energy homeostasis. Several recent studies have proposed various roles of 5-HT in hepatic metabolism and inflammation using tissue-specific knockout mice and 5-HT-receptor agonists/antagonists. This review compiles the most recent research on the relationship between 5-HT and hepatic metabolism, and the role of 5-HT signaling as a potential therapeutic target in NAFLD.
-
Citations
Citations to this article as recorded by- Maternal nutrient metabolism in the liver during pregnancy
Hongxu Fang, Qingyang Li, Haichao Wang, Ying Ren, Leying Zhang, Ling Yang
Frontiers in Endocrinology.2024;[Epub] CrossRef - Metabolic and Molecular Response to High-Fat Diet Differs between Rats with Constitutionally High and Low Serotonin Tone
Petra Baković, Maja Kesić, Darko Kolarić, Jasminka Štefulj, Lipa Čičin-Šain
International Journal of Molecular Sciences.2023; 24(3): 2169. CrossRef - Roles of gut microbes in metabolic-associated fatty liver disease
Chun-Yao Chen, Han-Chen Ho
Tzu Chi Medical Journal.2023; 35(4): 279. CrossRef - Imidazoles as Serotonin Receptor Modulators for Treatment of Depression: Structural Insights and Structure–Activity Relationship Studies
Kapil Kumar Goel, Somesh Thapliyal, Rajeev Kharb, Gaurav Joshi, Arvind Negi, Bhupinder Kumar
Pharmaceutics.2023; 15(9): 2208. CrossRef - Serotonin in the regulation of systemic energy metabolism
Joon Ho Moon, Chang‐Myung Oh, Hail Kim
Journal of Diabetes Investigation.2022; 13(10): 1639. CrossRef - Involvement of the liver-gut peripheral neural axis in nonalcoholic fatty liver disease pathologies via hepatic HTR2A
Takashi Owaki, Kenya Kamimura, Masayoshi Ko, Itsuo Nagayama, Takuro Nagoya, Osamu Shibata, Chiyumi Oda, Shinichi Morita, Atsushi Kimura, Takeki Sato, Toru Setsu, Akira Sakamaki, Hiroteru Kamimura, Takeshi Yokoo, Shuji Terai
Disease Models & Mechanisms.2022;[Epub] CrossRef - Non-alcoholic fatty liver disease (NAFLD) and mental illness: Mechanisms linking mood, metabolism and medicines
Anwesha Gangopadhyay, Radwa Ibrahim, Karli Theberge, Meghan May, Karen L. Houseknecht
Frontiers in Neuroscience.2022;[Epub] CrossRef
- Maternal nutrient metabolism in the liver during pregnancy

- Diabetes, Obesity and Metabolism
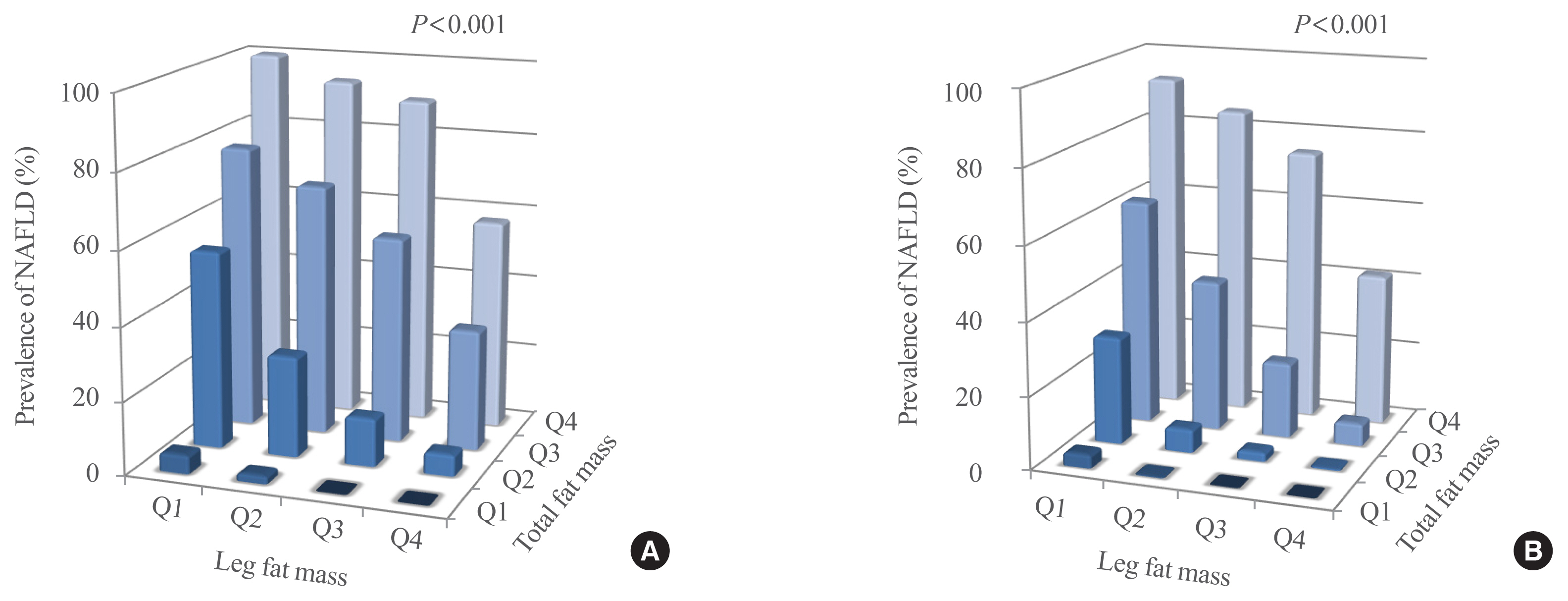
- The Leg Fat to Total Fat Ratio Is Associated with Lower Risks of Non-Alcoholic Fatty Liver Disease and Less Severe Hepatic Fibrosis: Results from Nationwide Surveys (KNHANES 2008–2011)
- Hyun Min Kim, Yong-ho Lee
- Endocrinol Metab. 2021;36(6):1232-1242. Published online November 23, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1087
- 3,811 View
- 130 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
The prevalence of non-alcoholic fatty liver disease (NAFLD) has rapidly increased worldwide. The aim of this study was to investigate whether there is an independent relationship between regional fat distribution, especially leg fat mass, and the presence of NAFLD using nationally representative data in Korea.
Methods
This cross-sectional study analyzed data from 14,502 participants in the Korea National Health and Nutrition Examination Survey 2008 to 2011. Total fat mass, leg fat mass, and appendicular skeletal muscle mass were measured by dual-energy X-ray absorptiometry. Validated NAFLD prediction models and scoring systems for hepatic fibrosis were used.
Results
The leg fat to total fat (LF/TF) ratio showed a negative relationship with many factors, including body mass index, waist circumference, blood pressure, fasting blood glucose, and liver enzyme levels. When the LF/TF ratio and indices of hepatic steatosis were stratified by quartiles, the LF/TF ratio showed a negative correlation with the scoring systems that were used. The LF/TF ratio showed better accuracy in predicting NAFLD than total fat mass or leg fat mass alone. After adjusting for various traditional and lifestyle factors, a low LF/TF ratio remained a risk factor for NAFLD. Among NAFLD subjects, the LF/TF ratio showed a negative relationship with hepatic fibrosis.
Conclusion
A lower LF/TF ratio was markedly associated with a higher risk of hepatic steatosis and advanced hepatic fibrosis using various predictive models in a Korean population. Therefore, the LF/TF ratio could be a useful anthropometric parameter to predict NAFLD or advanced hepatic fibrosis. -
Citations
Citations to this article as recorded by- A greater ratio of thigh subcutaneous fat to abdominal fat is associated with protection against non-alcoholic fatty liver disease
Yebei Liang, Peizhu Chen, Siyu Chen, Dan Liu, Fusong Jiang, Zhijun Zhu, Keqing Dong, Li Wei, Xuhong Hou
JHEP Reports.2023; 5(7): 100730. CrossRef - Association between Alcohol Consumption and Metabolic Dysfunction-Associated Steatotic Liver Disease Based on Alcohol Flushing Response in Men: The Korea National Health and Nutrition Examination Survey 2019–2021
Dae Eon Kang, Si Nae Oh
Nutrients.2023; 15(18): 3901. CrossRef
- A greater ratio of thigh subcutaneous fat to abdominal fat is associated with protection against non-alcoholic fatty liver disease

- Diabetes, Obesity and Metabolism
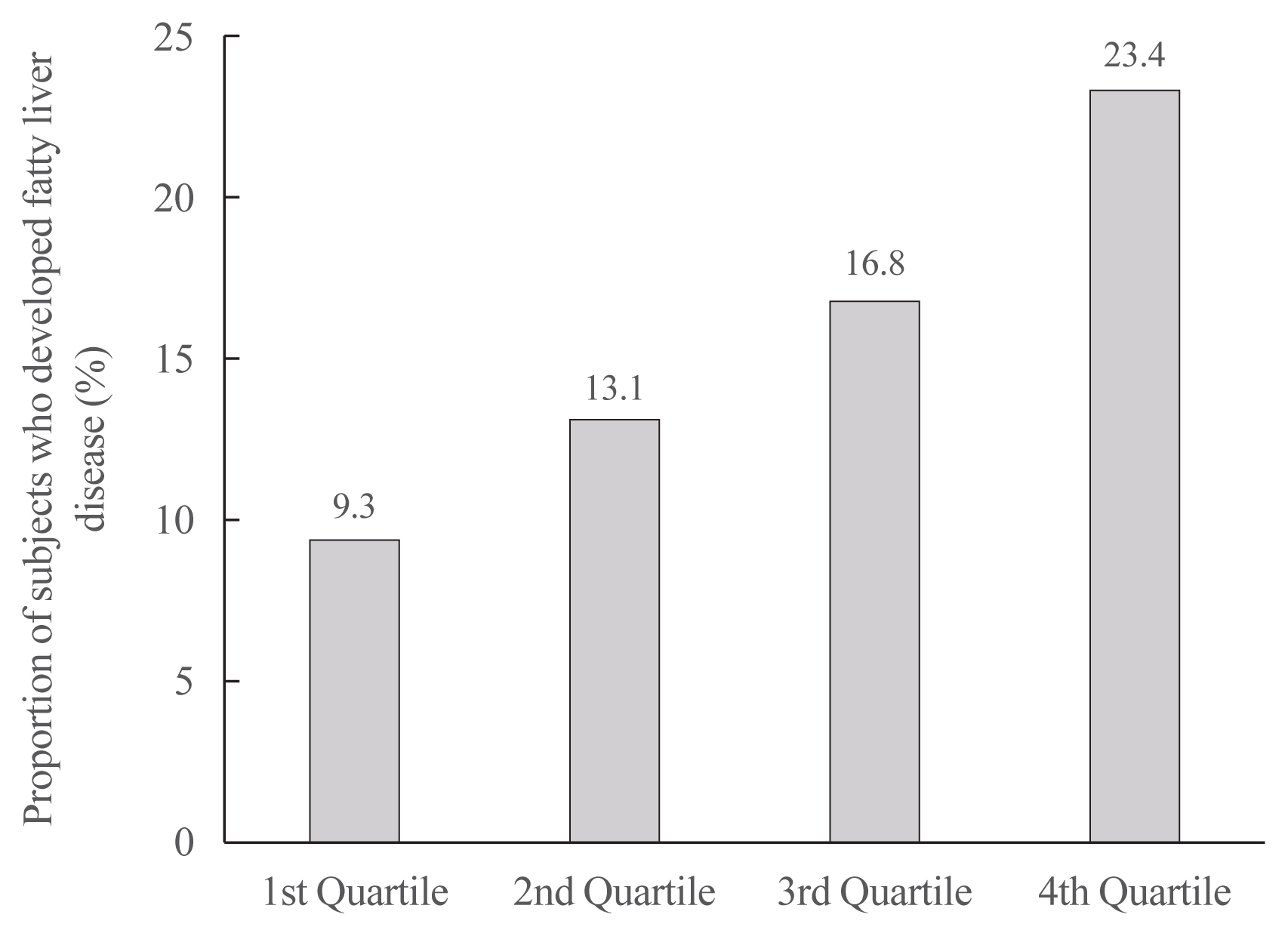
- Increased Risk of Nonalcoholic Fatty Liver Disease in Individuals with High Weight Variability
- Inha Jung, Dae-Jeong Koo, Mi Yeon Lee, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
- Endocrinol Metab. 2021;36(4):845-854. Published online August 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1098
- 4,930 View
- 140 Download
- 7 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Weight loss through lifestyle modification is recommended for patients with nonalcoholic fatty liver disease (NAFLD). Recent studies have suggested that repeated loss and gain of weight is associated with worse health outcomes. This study aimed to examine the association between weight variability and the risk of NAFLD in patients without diabetes.
Methods
We examined the health-checkup data of 30,708 participants who had undergone serial examinations between 2010 and 2014. Weight variability was assessed using coefficient of variation and the average successive variability of weight (ASVW), which was defined as the sum of absolute weight changes between successive years over the 5-year period divided by 4. The participants were classified according to the baseline body mass index and weight difference over 4 years.
Results
On dividing the participants into four groups according to ASVW quartile groups, those in the highest quartile showed a significantly increased risk of NAFLD compared to those in the lowest quartile (odds ratio [OR], 1.89; 95% confidence interval [CI], 1.63 to 2.19). Among participants without obesity at baseline, individuals with high ASVW showed increased risk of NAFLD (OR, 1.80; 95% CI, 1.61 to 2.01). Participants with increased weight over 4 years and high ASVW demonstrated higher risk of NAFLD compared to those with stable weight and low ASVW (OR, 4.87; 95% CI, 4.29 to 5.53).
Conclusion
Regardless of participant baseline obesity status, high weight variability was associated with an increased risk of developing NAFLD. Our results suggest that further effort is required to minimize weight fluctuations after achieving a desirable body weight. -
Citations
Citations to this article as recorded by- Changes in Macronutrients during Dieting Lead to Weight Cycling and Metabolic Complications in Mouse Model
Anouk Charlot, Anthony Bringolf, Léa Debrut, Joris Mallard, Anne-Laure Charles, Emilie Crouchet, Delphine Duteil, Bernard Geny, Joffrey Zoll
Nutrients.2024; 16(5): 646. CrossRef - Body weight variability and the risk of liver‐related outcomes in type 2 diabetes and steatotic liver disease: a cohort study
Nathalie C. Leite, Claudia R. L. Cardoso, Cristiane A. Villela‐Nogueira, Gil F. Salles
Obesity.2024;[Epub] CrossRef - Weight variability, physical functioning and incident disability in older adults
Katie J. McMenamin, Tamara B. Harris, Joshua F. Baker
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(4): 1648. CrossRef - Dulaglutide Ameliorates Palmitic Acid-Induced Hepatic Steatosis by Activating FAM3A Signaling Pathway
Jinmi Lee, Seok-Woo Hong, Min-Jeong Kim, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
Endocrinology and Metabolism.2022; 37(1): 74. CrossRef - Triglyceride and glucose index is a simple and easy‐to‐calculate marker associated with nonalcoholic fatty liver disease
Kyung‐Soo Kim, Sangmo Hong, Hong‐Yup Ahn, Cheol‐Young Park
Obesity.2022; 30(6): 1279. CrossRef - Metabolic (dysfunction)-associated fatty liver disease in individuals of normal weight
Mohammed Eslam, Hashem B. El-Serag, Sven Francque, Shiv K. Sarin, Lai Wei, Elisabetta Bugianesi, Jacob George
Nature Reviews Gastroenterology & Hepatology.2022; 19(10): 638. CrossRef - Impact of COVID-19 Lockdown on Non-Alcoholic Fatty Liver Disease and Insulin Resistance in Adults: A before and after Pandemic Lockdown Longitudinal Study
Ángel Arturo López-González, Bárbara Altisench Jané, Luis Masmiquel Comas, Sebastiana Arroyo Bote, Hilda María González San Miguel, José Ignacio Ramírez Manent
Nutrients.2022; 14(14): 2795. CrossRef - Higher Weight Variability Could Bring You a Fatty Liver
Yeoree Yang, Jae-Hyoung Cho
Endocrinology and Metabolism.2021; 36(4): 766. CrossRef - Autonomic Imbalance Increases the Risk for Non-alcoholic Fatty Liver Disease
Inha Jung, Da Young Lee, Mi Yeon Lee, Hyemi Kwon, Eun-Jung Rhee, Cheol-Young Park, Ki-Won Oh, Won-Young Lee, Sung-Woo Park, Se Eun Park
Frontiers in Endocrinology.2021;[Epub] CrossRef
- Changes in Macronutrients during Dieting Lead to Weight Cycling and Metabolic Complications in Mouse Model

- Diabetes, Obesity and Metabolism
- Non-Laboratory-Based Simple Screening Model for Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Developed Using Multi-Center Cohorts
- Jiwon Kim, Minyoung Lee, Soo Yeon Kim, Ji-Hye Kim, Ji Sun Nam, Sung Wan Chun, Se Eun Park, Kwang Joon Kim, Yong-ho Lee, Joo Young Nam, Eun Seok Kang
- Endocrinol Metab. 2021;36(4):823-834. Published online August 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1074
- 4,445 View
- 137 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Nonalcoholic fatty liver disease (NAFLD) is the most prevalent cause of chronic liver disease worldwide. Type 2 diabetes mellitus (T2DM) is a risk factor that accelerates NAFLD progression, leading to fibrosis and cirrhosis. Thus, here we aimed to develop a simple model to predict the presence of NAFLD based on clinical parameters of patients with T2DM.
Methods
A total of 698 patients with T2DM who visited five medical centers were included. NAFLD was evaluated using transient elastography. Univariate logistic regression analyses were performed to identify potential contributors to NAFLD, followed by multivariable logistic regression analyses to create the final prediction model for NAFLD.
Results
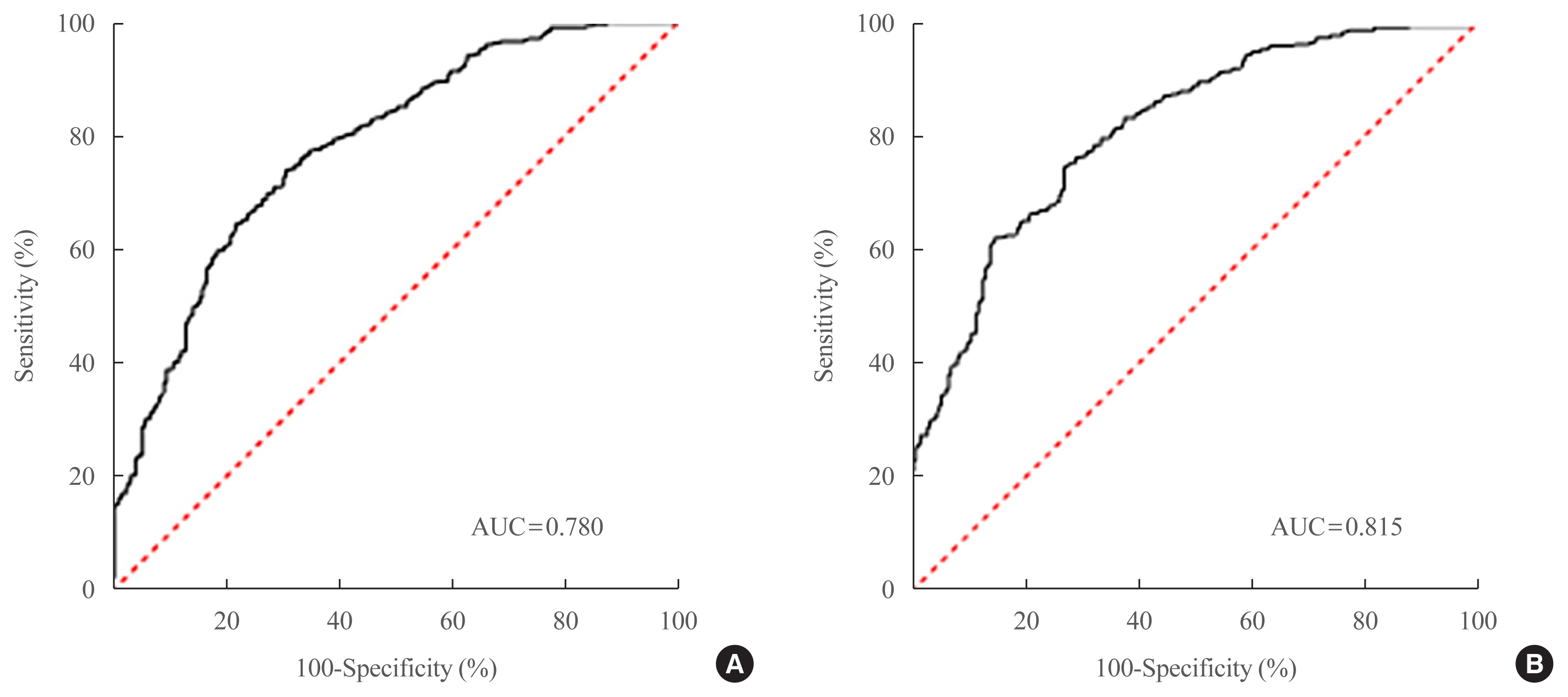
Two NAFLD prediction models were developed, with and without serum biomarker use. The non-laboratory model comprised six variables: age, sex, waist circumference, body mass index (BMI), dyslipidemia, and smoking status. For a cutoff value of ≥60, the prediction accuracy was 0.780 (95% confidence interval [CI], 0.743 to 0.817). The second comprehensive model showed an improved discrimination ability of up to 0.815 (95% CI, 0.782 to 0.847) and comprised seven variables: age, sex, waist circumference, BMI, glycated hemoglobin, triglyceride, and alanine aminotransferase to aspartate aminotransferase ratio. Our non-laboratory model showed non-inferiority in the prediction of NAFLD versus previously established models, including serum parameters.
Conclusion
The new models are simple and user-friendly screening methods that can identify individuals with T2DM who are at high-risk for NAFLD. Additional studies are warranted to validate these new models as useful predictive tools for NAFLD in clinical practice. -
Citations
Citations to this article as recorded by- Non-Alcoholic Fatty Liver Disease or Type 2 Diabetes Mellitus—The Chicken or the Egg Dilemma
Marcin Kosmalski, Agnieszka Śliwińska, Józef Drzewoski
Biomedicines.2023; 11(4): 1097. CrossRef
- Non-Alcoholic Fatty Liver Disease or Type 2 Diabetes Mellitus—The Chicken or the Egg Dilemma

- Diabetes, Obesity and Metabolism
- High Fibrosis-4 Index Is Related with Worse Clinical Outcome in Patients with Coronavirus Disease 2019 and Diabetes Mellitus: A Multicenter Observational Study
- Sung-Woo Kim, Jae-Han Jeon, Jun Sung Moon, Mi Kyung Kim
- Endocrinol Metab. 2021;36(4):800-809. Published online August 20, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1040
- 5,067 View
- 175 Download
- 6 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Based on recent evidence on the importance of the presence of diabetes mellitus (DM) and fibrosis-4 (FIB-4) index in coronavirus disease 2019 (COVID-19) mortality, we analyzed whether these factors could additively predict such mortality.
Methods
This multicenter observational study included 1,019 adult inpatients admitted to university hospitals in Daegu. The demographic and laboratory findings, mortality, prevalence of severe disease, and duration of quarantine were compared between patients with and without DM and/or a high FIB-4 index. The mortality risk and corresponding hazard ratio (HR) were analyzed using the Kaplan-Meier method and Cox proportional hazard models.
Results
The patients with DM (n=217) exhibited significantly higher FIB-4 index and mortality compared to those without DM. Although DM (HR, 2.66; 95% confidence interval [CI], 1.63 to 4.33) and a high FIB-4 index (HR, 4.20; 95% CI, 2.21 to 7.99) were separately identified as risk factors for COVID-19 mortality, the patients with both DM and high FIB-4 index had a significantly higher mortality (HR, 9.54; 95% CI, 4.11 to 22.15). Higher FIB-4 indices were associated with higher mortality regardless of DM. A high FIB-4 index with DM was more significantly associated with a severe clinical course with mortality (odds ratio, 11.24; 95% CI, 5.90 to 21.41) than a low FIB-4 index without DM, followed by a high FIB-4 index alone and DM alone. The duration of quarantine and hospital stay also tended to be longer in those with both DM and high FIB-4 index.
Conclusion
Both DM and high FIB-4 index are independent and additive risk factors for COVID-19 mortality. -
Citations
Citations to this article as recorded by- COVID-19 and hepatic injury: Diversity and risk assessment
Fares E M Ali, Mostafa K Abd El-Aziz, Mahmoud M Ali, Osama M Ghogar, Adel G Bakr
World Journal of Gastroenterology.2023; 29(3): 425. CrossRef - Differential Effects of COVID-19 Hospitalization on the Trajectory of Liver Disease Progression
Dilara Hatipoğlu, Connor Mulligan, Jeffrey Wang, Juan Peticco, Reid Grinspoon, Sanjay Gadi, Camilla Mills, Jay Luther, Raymond T. Chung
Gastro Hep Advances.2023; 2(4): 480. CrossRef - Association of non-alcoholic fatty liver and metabolic-associated fatty liver with COVID-19 outcomes: A systematic review and meta-analysis
Gowthami Sai Kogilathota Jagirdhar, Rakhtan K Qasba, Harsha Pattnaik, Kaanthi Rama, Akshat Banga, Shiva Teja Reddy, Anna Carolina Flumignan Bucharles, Rahul Kashyap, Praveen Reddy Elmati, Vikas Bansal, Yatinder Bains, Theodore DaCosta, Salim Surani
World Journal of Gastroenterology.2023; 29(21): 3362. CrossRef - COVID-19 and Fatty Liver Disorders
Maria Guarino, Valentina Cossiga, Francesco Cutolo, Maria Attanasio, Raffaele Lieto, Filomena Morisco
Journal of Clinical Medicine.2023; 12(13): 4316. CrossRef - Prevalence and Prognostic Significance of Liver Fibrosis in Patients With Aneurysmal Subarachnoid Hemorrhage
Tiangui Li, Peng Wang, Xiao Gong, Weelic Chong, Yang Hai, Chao You, Juan Kang, Fang Fang, Yu Zhang
Frontiers in Neurology.2022;[Epub] CrossRef
- COVID-19 and hepatic injury: Diversity and risk assessment

- Clinical Study
- Development of a Non-Invasive Liver Fibrosis Score Based on Transient Elastography for Risk Stratification in Patients with Type 2 Diabetes
- Chi-Ho Lee, Wai-Kay Seto, Kelly Ieong, David T.W. Lui, Carol H.Y. Fong, Helen Y. Wan, Wing-Sun Chow, Yu-Cho Woo, Man-Fung Yuen, Karen S.L. Lam
- Endocrinol Metab. 2021;36(1):134-145. Published online February 24, 2021
- DOI: https://doi.org/10.3803/EnM.2020.887
- 4,505 View
- 132 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
In non-alcoholic fatty liver disease (NAFLD), transient elastography (TE) is an accurate non-invasive method to identify patients at risk of advanced fibrosis (AF). We developed a diabetes-specific, non-invasive liver fibrosis score based on TE to facilitate AF risk stratification, especially for use in diabetes clinics where TE is not readily available.
Methods
Seven hundred sixty-six adults with type 2 diabetes and NAFLD were recruited and randomly divided into a training set (n=534) for the development of diabetes fibrosis score (DFS), and a testing set (n=232) for internal validation. DFS identified patients with AF on TE, defined as liver stiffness (LS) ≥9.6 kPa, based on a clinical model comprising significant determinants of LS with the lowest Akaike information criteria. The performance of DFS was compared with conventional liver fibrosis scores (NFS, FIB-4, and APRI), using area under the receiver operating characteristic curve (AUROC), sensitivity, specificity, positive and negative predictive values (NPV).
Results
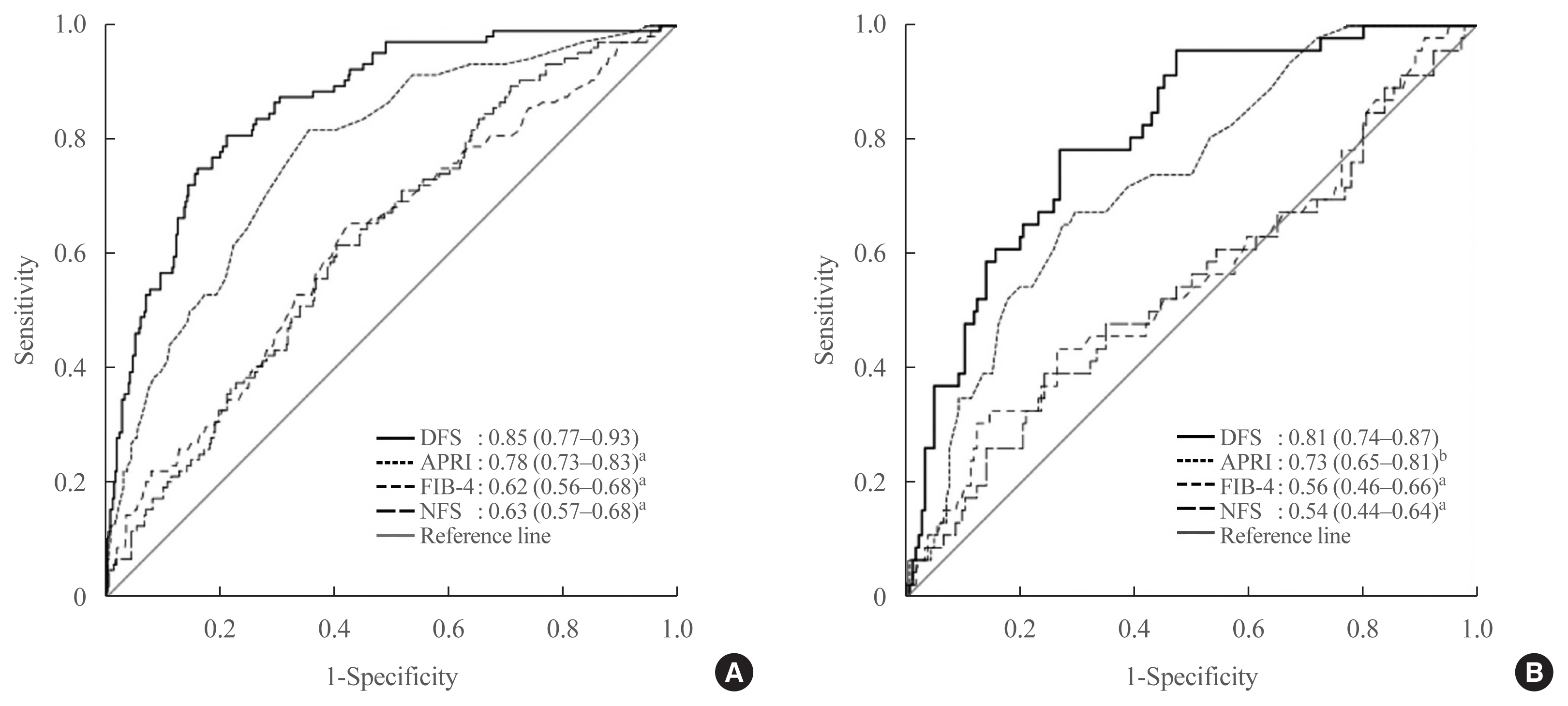
DFS comprised body mass index, platelet, aspartate aminotransferase, high-density lipoprotein cholesterol, and albuminuria, five routine measurements in standard diabetes care. Derived low and high DFS cut-offs were 0.1 and 0.3, with 90% sensitivity and 90% specificity, respectively. Both cut-offs provided better NPVs of >90% than conventional fibrosis scores. The AUROC of DFS for AF on TE was also higher (P<0.01) than the conventional fibrosis scores, being 0.85 and 0.81 in the training and testing sets, respectively.
Conclusion
Compared to conventional fibrosis scores, DFS, with a high NPV, more accurately identified diabetes patients at-risk of AF, who need further evaluation by hepatologists. -
Citations
Citations to this article as recorded by- Implementation of a liver health check in people with type 2 diabetes
Kushala W M Abeysekera, Luca Valenti, Zobair Younossi, John F Dillon, Alina M Allen, Mazen Noureddin, Mary E Rinella, Frank Tacke, Sven Francque, Pere Ginès, Maja Thiele, Philip N Newsome, Indra Neil Guha, Mohammed Eslam, Jörn M Schattenberg, Saleh A Alqa
The Lancet Gastroenterology & Hepatology.2024; 9(1): 83. CrossRef - Sequential algorithm to stratify liver fibrosis risk in overweight/obese metabolic dysfunction-associated fatty liver disease
Chi-Ho Lee, David Tak-Wai Lui, Raymond Hang-Wun Li, Michele Mae-Ann Yuen, Carol Ho-Yi Fong, Ambrose Pak-Wah Leung, Justin Chiu-Man Chu, Loey Lung-Yi Mak, Tai-Hing Lam, Jean Woo, Yu-Cho Woo, Aimin Xu, Hung-Fat Tse, Kathryn Choon-Beng Tan, Bernard Man-Yung
Frontiers in Endocrinology.2023;[Epub] CrossRef - Non-Invasive Measurement of Hepatic Fibrosis by Transient Elastography: A Narrative Review
Luca Rinaldi, Chiara Giorgione, Andrea Mormone, Francesca Esposito, Michele Rinaldi, Massimiliano Berretta, Raffaele Marfella, Ciro Romano
Viruses.2023; 15(8): 1730. CrossRef - Metabolic dysfunction-associated fatty liver disease — How relevant is this to primary care physicians and diabetologists?
Chi-Ho Lee
Primary Care Diabetes.2022; 16(2): 245. CrossRef - Non‐alcoholic fatty liver disease and type 2 diabetes: An update
Chi‐H Lee, David TW Lui, Karen SL Lam
Journal of Diabetes Investigation.2022; 13(6): 930. CrossRef - Ultrasound-Based Hepatic Elastography in Non-Alcoholic Fatty Liver Disease: Focus on Patients with Type 2 Diabetes
Georgiana-Diana Cazac, Cristina-Mihaela Lăcătușu, Cătălina Mihai, Elena-Daniela Grigorescu, Alina Onofriescu, Bogdan-Mircea Mihai
Biomedicines.2022; 10(10): 2375. CrossRef
- Implementation of a liver health check in people with type 2 diabetes

- Obesity and Metabolism
- Noninvasive Evaluation of Nonalcoholic Fatty Liver Disease
- Dae Ho Lee
- Endocrinol Metab. 2020;35(2):243-259. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.243
- 11,064 View
- 296 Download
- 19 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
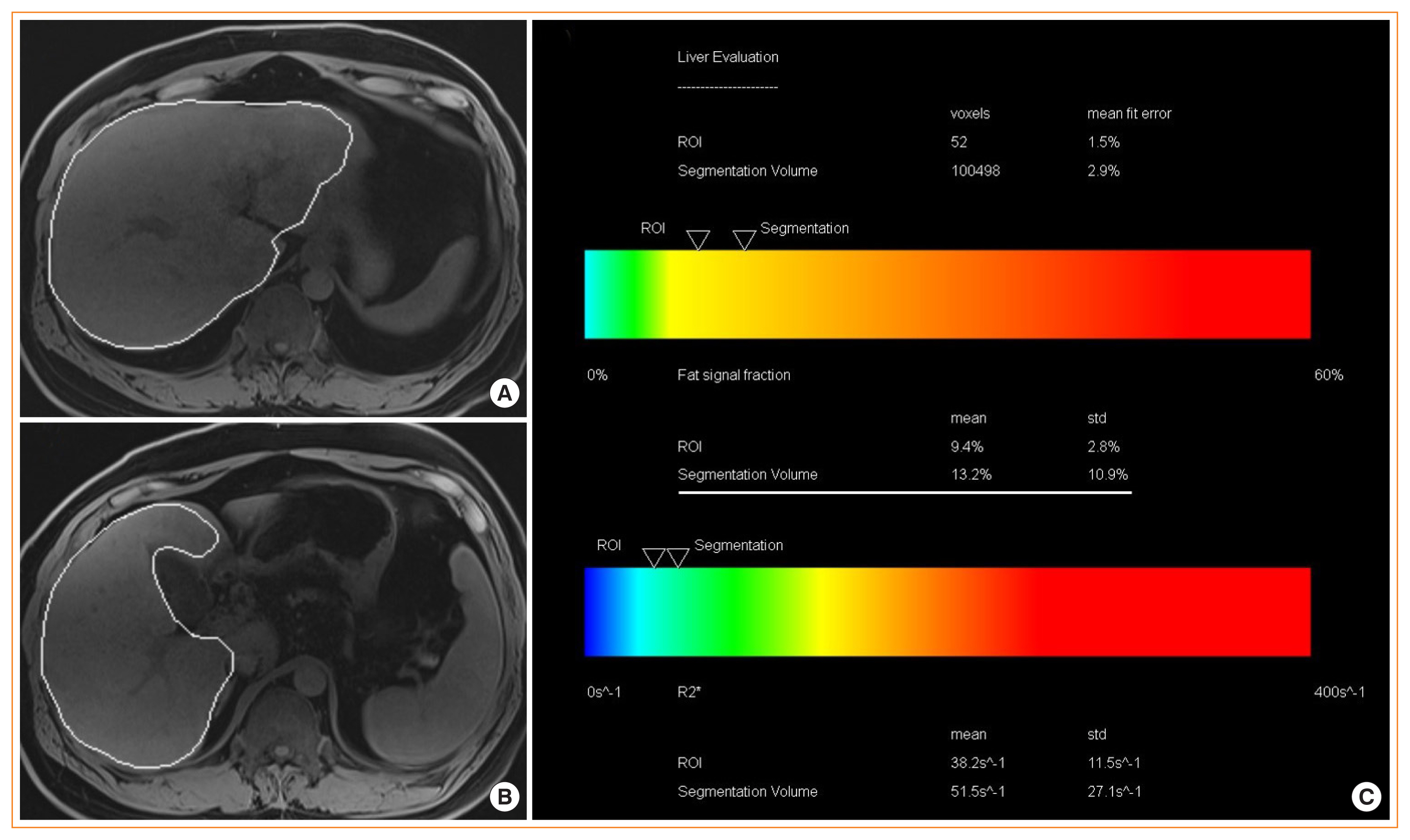
ePub - Nonalcoholic fatty liver disease (NAFLD) is the most prevalent liver diseases and can progress to advanced fibrosis and end-stage liver disease. Thus, intensive research has been performed to develop noninvasive methods for the diagnosis of nonalcoholic steatohepatitis (NASH) and fibrosis. Currently, no single noninvasive tool covers all of the stages of pathologies and conditions of NAFLD, and the cost and feasibility of known techniques are also important issues. Blood biomarkers for NAFLD may be useful to select subjects who need ultrasonography (US) screening for NAFLD, and noninvasive tools for assessing fibrosis may be helpful to exclude the probability of significant fibrosis and to predict advanced fibrosis, thus guiding the decision of whether to perform liver biopsy in patients with NAFLD. Among various methods, magnetic resonance-based methods have been shown to perform better than other methods in assessing steatosis as well as in detecting hepatic fibrosis. Many genetic markers are associated with the development and progression of NAFLD. Further well-designed studies are needed to determine which biomarker panels, imaging studies, genetic marker panels, or combinations thereof perform well for diagnosing NAFLD, differentiating NASH and fibrosis, and following-up NAFLD, respectively.
-
Citations
Citations to this article as recorded by- Recent Progresses on Pathophysiology, Diagnosis, Therapeutic Modalities,
and Management of Non-alcoholic Fatty Liver Disorder
Mahdi Barazesh, Sajad Jalili, Morteza Akhzari, Fouzieyeh Faraji, Ebrahim Khorramdin
Current Drug Therapy.2024; 19(1): 20. CrossRef - Intact ketogenesis predicted reduced risk of moderate-severe metabolic-associated fatty liver disease assessed by liver transient elastography in newly diagnosed type 2 diabetes
Sejeong Lee, Jaehyun Bae, Seung Up Kim, Minyoung Lee, Yong-ho Lee, Eun Seok Kang, Bong-Soo Cha, Byung-Wan Lee
Frontiers in Endocrinology.2024;[Epub] CrossRef - Association between nonalcoholic fatty liver disease and left ventricular diastolic dysfunction: A 7-year retrospective cohort study of 3,496 adults using serial echocardiography
Gyuri Kim, Tae Yang Yu, Jae Hwan Jee, Ji Cheol Bae, Mira Kang, Jae Hyeon Kim
Diabetes & Metabolism.2024; : 101534. CrossRef - Metabolic Dysfunction-Associated Fatty Liver Disease and Mortality: A Population-Based Cohort Study
Kyung-Soo Kim, Sangmo Hong, Hong-Yup Ahn, Cheol-Young Park
Diabetes & Metabolism Journal.2023; 47(2): 220. CrossRef - Non-invasive diagnosis and monitoring of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis
Monica A Tincopa, Rohit Loomba
The Lancet Gastroenterology & Hepatology.2023; 8(7): 660. CrossRef - Hepatic Involvement across the Metabolic Syndrome Spectrum: Non-Invasive Assessment and Risk Prediction Using Machine Learning
Adelaida Solomon, Călin Remus Cipăian, Mihai Octavian Negrea, Adrian Boicean, Romeo Mihaila, Corina Beca, Mirela Livia Popa, Sebastian Mihai Grama, Minodora Teodoru, Bogdan Neamtu
Journal of Clinical Medicine.2023; 12(17): 5657. CrossRef - Greater Severity of Steatosis Is Associated with a Higher Risk of Incident Diabetes: A Retrospective Longitudinal Study
Ji Min Han, Jung Hwan Cho, Hye In Kim, Sunghwan Suh, Yu-Ji Lee, Jung Won Lee, Kwang Min Kim, Ji Cheol Bae
Endocrinology and Metabolism.2023; 38(4): 418. CrossRef - Advances in Noninvasive Biomarkers for Nonalcoholic Fatty Liver Disease
Georgiana-Emmanuela Gîlcă-Blanariu, Daniela Simona Budur, Dana Elena Mitrică, Elena Gologan, Oana Timofte, Gheorghe Gh Bălan, Vasile Andrei Olteanu, Gabriela Ștefănescu
Metabolites.2023; 13(11): 1115. CrossRef - Plasma Aldo-Keto Reductase Family 1 Member B10 as a Biomarker Performs Well in the Diagnosis of Nonalcoholic Steatohepatitis and Fibrosis
Aron Park, Seung Joon Choi, Sungjin Park, Seong Min Kim, Hye Eun Lee, Minjae Joo, Kyoung Kon Kim, Doojin Kim, Dong Hae Chung, Jae Been Im, Jaehun Jung, Seung Kak Shin, Byung-Chul Oh, Cheolsoo Choi, Seungyoon Nam, Dae Ho Lee
International Journal of Molecular Sciences.2022; 23(9): 5035. CrossRef - Triglyceride and glucose index is a simple and easy‐to‐calculate marker associated with nonalcoholic fatty liver disease
Kyung‐Soo Kim, Sangmo Hong, Hong‐Yup Ahn, Cheol‐Young Park
Obesity.2022; 30(6): 1279. CrossRef - The Impact of Insulin Resistance on Hepatic Fibrosis among United States Adults with Non-Alcoholic Fatty Liver Disease: NHANES 2017 to 2018
Ji Cheol Bae, Lauren A. Beste, Kristina M. Utzschneider
Endocrinology and Metabolism.2022; 37(3): 455. CrossRef - Plasma Metabolomics and Machine Learning-Driven Novel Diagnostic Signature for Non-Alcoholic Steatohepatitis
Moongi Ji, Yunju Jo, Seung Joon Choi, Seong Min Kim, Kyoung Kon Kim, Byung-Chul Oh, Dongryeol Ryu, Man-Jeong Paik, Dae Ho Lee
Biomedicines.2022; 10(7): 1669. CrossRef - Evaluation of Liver Changes in Type-2 Diabetes Mellitus Patients using Computed Tomography
Nayyar Ashfaq, Akash John, Abid Ali, Amina Sharif Bhatti, Hateem Qaiser
DIET FACTOR (Journal of Nutritional & Food Sciences).2022; : 14. CrossRef - Accuracy of FIB-4 to Detect Elevated Liver Stiffness Measurements in Patients with Non-Alcoholic Fatty Liver Disease: A Cross-Sectional Study in Referral Centers
Mauro Viganò, Nicola Pugliese, Federica Cerini, Federica Turati, Vincenzo Cimino, Sofia Ridolfo, Simone Rocchetto, Francesca Foglio, Maria Terrin, Carlo La Vecchia, Maria Grazia Rumi, Alessio Aghemo
International Journal of Molecular Sciences.2022; 23(20): 12489. CrossRef - MAFLD vs. NAFLD: shared features and potential changes in epidemiology, pathophysiology, diagnosis, and pharmacotherapy
Ying-Xin Xian, Jian-Ping Weng, Fen Xu
Chinese Medical Journal.2021; 134(1): 8. CrossRef - Prognostic accuracy of FIB‐4, NAFLD fibrosis score and APRI for NAFLD‐related events: A systematic review
Jenny Lee, Yasaman Vali, Jerome Boursier, Rene Spijker, Quentin M. Anstee, Patrick M. Bossuyt, Mohammad H. Zafarmand
Liver International.2021; 41(2): 261. CrossRef - Serum syndecan‐4 is associated with nonalcoholic fatty liver disease
Shu Jing Xia, Li Zhong Tang, Wen Hua Li, Zhao Shan Xu, Li Li Zhang, Feng Gan Cheng, Hong Xia Chen, Zi Hua Wang, Yu Cheng Luo, An Na Dai, Jian Gao Fan
Journal of Digestive Diseases.2021; 22(9): 536. CrossRef - Non-Laboratory-Based Simple Screening Model for Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Developed Using Multi-Center Cohorts
Jiwon Kim, Minyoung Lee, Soo Yeon Kim, Ji-Hye Kim, Ji Sun Nam, Sung Wan Chun, Se Eun Park, Kwang Joon Kim, Yong-ho Lee, Joo Young Nam, Eun Seok Kang
Endocrinology and Metabolism.2021; 36(4): 823. CrossRef - Pemafibrate Ameliorates Liver Dysfunction and Fatty Liver in Patients with Non-Alcoholic Fatty Liver Disease with Hypertriglyceridemia: A Retrospective Study with the Outcome after a Mid-Term Follow-Up
Suguru Ikeda, Takaaki Sugihara, Takuya Kihara, Yukako Matsuki, Takakazu Nagahara, Tomoaki Takata, Sonoko Kitao, Tsuyoshi Okura, Kazuhiro Yamamoto, Hajime Isomoto
Diagnostics.2021; 11(12): 2316. CrossRef - Triglyceride Glucose-Waist Circumference Is Superior to the Homeostasis Model Assessment of Insulin Resistance in Identifying Nonalcoholic Fatty Liver Disease in Healthy Subjects
Hwi Seung Kim, Yun Kyung Cho, Eun Hee Kim, Min Jung Lee, Chang Hee Jung, Joong-Yeol Park, Hong-Kyu Kim, Woo Je Lee
Journal of Clinical Medicine.2021; 11(1): 41. CrossRef - The Leg Fat to Total Fat Ratio Is Associated with Lower Risks of Non-Alcoholic Fatty Liver Disease and Less Severe Hepatic Fibrosis: Results from Nationwide Surveys (KNHANES 2008–2011)
Hyun Min Kim, Yong-ho Lee
Endocrinology and Metabolism.2021; 36(6): 1232. CrossRef
- Recent Progresses on Pathophysiology, Diagnosis, Therapeutic Modalities,
and Management of Non-alcoholic Fatty Liver Disorder

- Clinical Study
- Visceral-to-Subcutaneous Abdominal Fat Ratio Is Associated with Nonalcoholic Fatty Liver Disease and Liver Fibrosis
- Chan-Hee Jung, Eun-Jung Rhee, Hyemi Kwon, Yoosoo Chang, Seungho Ryu, Won-Young Lee
- Endocrinol Metab. 2020;35(1):165-176. Published online March 19, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.1.165
- 6,532 View
- 137 Download
- 26 Web of Science
- 27 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub Background We evaluated the association of visceral-to-subcutaneous fat ratio (VSR) with nonalcoholic fatty liver disease (NAFLD) and advanced fibrosis degree based on noninvasive serum fibrosis markers in the general population with NAFLD.
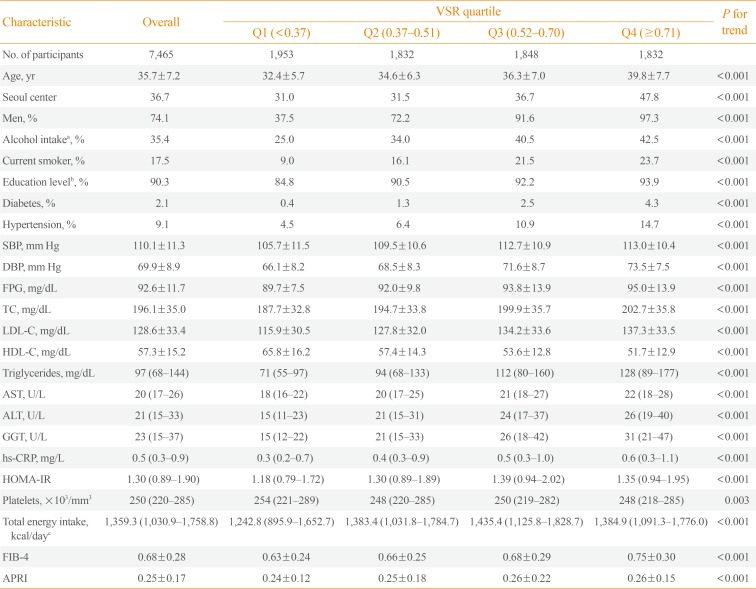
Methods This is a cross-sectional study, in 7,465 Korean adults who underwent health screening examinations. NAFLD was defined as fatty liver detected on ultrasonography, and visceral and subcutaneous abdominal fat was measured using computed tomography. We predicted fibrosis based on the fibrosis-4 (FIB-4) score and aspartate aminotransferase-to-platelet ratio index (APRI) and categorized the risk for advanced fibrosis as low, indeterminate, or high.
Results The multivariable-adjusted prevalence ratios for indeterminate to high risk of advanced fibrosis based on FIB-4, determined by comparing the second, third, and fourth quartiles with the first quartile of VSR, were 3.38 (95% confidence interval [CI], 0.64 to 17.97), 9.41 (95% CI, 1.97 to 45.01), and 19.34 (95% CI, 4.06 to 92.18), respectively. The multivariable-adjusted prevalence ratios for intermediate to high degree of fibrosis according to APRI also increased across VSR quartiles (5.04 [95% CI, 2.65 to 9.59], 7.51 [95% CI, 3.91 to 14.42], and 19.55 [95% CI, 9.97 to 38.34], respectively). High VSR was more strongly associated with the prevalence of NAFLD in nonobese subjects than in obese subjects, and the associations between VSR and intermediate to high probability of advanced fibrosis in NAFLD were stronger in obese subjects than in nonobese subjects.
Conclusion High VSR values predicted increased NAFLD risk and advanced fibrosis risk with NAFLD, and the predictive value of VSR for indeterminate to high risk of advanced fibrosis was higher in obese subjects than in nonobese subjects.
-
Citations
Citations to this article as recorded by- Opportunistic Extraction of Quantitative CT Biomarkers: Turning the Incidental Into Prognostic Information
Mohammad Nazri Md Shah, Raja Rizal Azman, Wai Yee Chan, Kwan Hoong Ng
Canadian Association of Radiologists Journal.2024; 75(1): 92. CrossRef - Positive Association Between the Chinese Visceral Adiposity Index and Nonalcoholic Fatty Liver Disease in Lean Adults
Shuxia Shen, Hangkai Huang, Jinghua Wang, Zexi Tang, Chao Shen, Chengfu Xu
Digestive Diseases and Sciences.2023; 68(2): 656. CrossRef - Association between Sarcopenic Obesity Status and Nonalcoholic Fatty Liver Disease and Fibrosis
Wolhwa Song, Sung Hwan Yoo, Jinsun Jang, Su Jung Baik, Byoung Kwon Lee, Hyun Woong Lee, Jong Suk Park
Gut and Liver.2023; 17(1): 130. CrossRef - Using hyperhomocysteinemia and body composition to predict the risk of non-alcoholic fatty liver disease in healthcare workers
Xiaoyan Hao, Honghai He, Liyuan Tao, Peng Wang
Frontiers in Endocrinology.2023;[Epub] CrossRef - Visceral and subcutaneous fat, muscle mass, and liver volume as noninvasive predictors of the progress of non-alcoholic fatty liver disease
Omar M. Mahmoud, Gehad Abd Elaziz Mahmoud, Haisam Atta, Wael A. Abbas, Hanan M. Ahmed, Mohamed A. A. Abozaid
Egyptian Journal of Radiology and Nuclear Medicine.2023;[Epub] CrossRef - Relationship between metabolic associated fatty liver disease and body fat ratio, visceral fat area, and resting metabolic rate estimated by bioelectrical impedance analysis
Deng-Hua He, Yong-Zhan Zhang, Liang Xu, Jia-Jia Pei, Ying Zhang, Zhong-Fang Yan
World Chinese Journal of Digestology.2023; 31(2): 56. CrossRef - Poor glycaemic control and ectopic fat deposition mediates the increased risk of non-alcoholic steatohepatitis in high-risk populations with type 2 diabetes: Insights from Bayesian-network modelling
T. Waddell, A. Namburete, P. Duckworth, A. Fichera, A. Telford, H. Thomaides-Brears, D. J. Cuthbertson, M. Brady
Frontiers in Endocrinology.2023;[Epub] CrossRef - Metabolic Dysfunction-Associated Fatty Liver Disease and Mortality: A Population-Based Cohort Study
Kyung-Soo Kim, Sangmo Hong, Hong-Yup Ahn, Cheol-Young Park
Diabetes & Metabolism Journal.2023; 47(2): 220. CrossRef - Subcutaneous Fat Obesity in a High Body Mass Index Donor Is Not a Contraindication to Living Donor Hepatectomy
Hirak Pahari, Amey Sonavane, Amruth Raj, Anup Kumar Agrawal, Ambreen Sawant, Deepak Kumar Gupta, Amit Gharat, Vikram Raut, Sorabh Kapoor
Case Reports in Hepatology.2023; 2023: 1. CrossRef - Comparison of cardiometabolic risk factors between obese and non-obese patients with nonalcoholic fatty liver disease
Zahra Yari, Danial Fotros, Azita Hekmatdoost
Scientific Reports.2023;[Epub] CrossRef - Association of Visceral Fat Obesity, Sarcopenia, and Myosteatosis with Non-Alcoholic Fatty Liver Disease without Obesity
Hong-Kyu Kim, Sung-Jin Bae, Min Jung Lee, Eun Hee Kim, Hana Park, Hwi Seung Kim, Yun Kyung Cho, Chang Hee Jung, Woo Je Lee, Jaewon Choe
Clinical and Molecular Hepatology.2023; 29(4): 987. CrossRef - Visceral Adipose Tissue Inflammation and Radiographic Visceral-to-Subcutaneous Adipose Tissue Ratio in Patients with Cirrhosis
Nghiem B. Ha, Soo-Jin Cho, Yara Mohamad, Dorothea Kent, Grace Jun, Randi Wong, Vivek Swarnakar, Shezhang Lin, Jacquelyn J. Maher, Jennifer C. Lai
Digestive Diseases and Sciences.2022; 67(7): 3436. CrossRef - The Influence of Obesity and Metabolic Health on Vascular Health
Eun-Jung Rhee
Endocrinology and Metabolism.2022; 37(1): 1. CrossRef - The effect of combined exercises on the plasma levels of retinol-binding protein 4 and its relationship with insulin resistance and hepatic fat content in postmenopausal women with nonalcoholic fatty liver disease
Masoumeh NOROUZPOUR, Sayyed M. MARANDI, Mohsen GHANBARZADEH, Abbasali ZARE MAIVAN
The Journal of Sports Medicine and Physical Fitness.2022;[Epub] CrossRef - The Perirenal Fat Thickness Was Associated with Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Mellitus
Yuxian Yang, Shuting Li, Yuechao Xu, Jing Ke, Dong Zhao
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2022; Volume 15: 1505. CrossRef - Visceral adiposity is an independent risk factor for high intra-operative blood loss during living-donor liver transplantation; could preoperative rehabilitation and nutritional therapy mitigate that risk?
Mahmoud Macshut, Toshimi Kaido, Siyuan Yao, Yosuke Miyachi, Mohamed Sharshar, Sena Iwamura, Masaaki Hirata, Hisaya Shirai, Naoko Kamo, Shintaro Yagi, Shinji Uemoto
Clinical Nutrition.2021; 40(3): 956. CrossRef - A review of non‐alcoholic fatty liver disease in non‐obese and lean individuals
Mitra Ahadi, Kasra Molooghi, Negin Masoudifar, Ali Beheshti Namdar, Hassan Vossoughinia, Mohammadreza Farzanehfar
Journal of Gastroenterology and Hepatology.2021; 36(6): 1497. CrossRef - Quantification of abdominal fat from computed tomography using deep learning and its association with electronic health records in an academic biobank
Matthew T MacLean, Qasim Jehangir, Marijana Vujkovic, Yi-An Ko, Harold Litt, Arijitt Borthakur, Hersh Sagreiya, Mark Rosen, David A Mankoff, Mitchell D Schnall, Haochang Shou, Julio Chirinos, Scott M Damrauer, Drew A Torigian, Rotonya Carr, Daniel J Rader
Journal of the American Medical Informatics Association.2021; 28(6): 1178. CrossRef - Hepatic Steatosis in Patients With Single Ventricle and a Fontan Circulation
David A. Katz, Daniel Peck, Adam M. Lubert, Mathias Possner, Faizeen Zafar, Andrew T. Trout, Joseph J. Palermo, Nadeem Anwar, Jonathan R. Dillman, Adam W. Powell, Stavra A. Xanthakos, Alexander R. Opotowsky, Gruschen Veldtman, Tarek Alsaied
Journal of the American Heart Association.2021;[Epub] CrossRef - Superficial vs Deep Subcutaneous Adipose Tissue: Sex-Specific Associations With Hepatic Steatosis and Metabolic Traits
Tessa Brand, Inge Christina Lamberta van den Munckhof, Marinette van der Graaf, Kiki Schraa, Helena Maria Dekker, Leonardus Antonius Bernardus Joosten, Mihai Gheorghe Netea, Niels Peter Riksen, Jacqueline de Graaf, Joseph Henricus Wilhelmus Rutten
The Journal of Clinical Endocrinology & Metabolism.2021; 106(10): e3881. CrossRef - Baseline homeostasis model assessment of insulin resistance associated with fibrosis progression in patients with nonalcoholic fatty liver disease without diabetes: A cohort study
Dae-Jeong Koo, Mi Yeon Lee, Inha Jung, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee, Ming-Lung Yu
PLOS ONE.2021; 16(8): e0255535. CrossRef - Randomised clinical trial: semaglutide versus placebo reduced liver steatosis but not liver stiffness in subjects with non‐alcoholic fatty liver disease assessed by magnetic resonance imaging
Anne Flint, Grit Andersen, Paul Hockings, Lars Johansson, Anni Morsing, Mads Sundby Palle, Thomas Vogl, Rohit Loomba, Leona Plum‐Mörschel
Alimentary Pharmacology & Therapeutics.2021; 54(9): 1150. CrossRef - Effects of IL-33 on 3T3-L1 cells and obese mice models induced by a high-fat diet
Yue Kai, Jingtao Gao, Hu Liu, Yubing Wang, Chenrui Tian, Sheng Guo, Ling He, Min Li, Zhongwei Tian, Xiangfeng Song
International Immunopharmacology.2021; 101: 108209. CrossRef - Lipid Accumulation Product as an Index for Visceral Obesity and Cardiovascular Risk among a Sample of Obese Egyptian Women
Nayera E. Hassan, Sahar A. El-Masry, Gamila S. M. El-Saeed, Mohamed S. El Hussieny
Open Access Macedonian Journal of Medical Sciences.2021; 9(B): 1229. CrossRef - Combined Effects of Dyslipidemia and High Adiposity on the Estimated Glomerular Filtration Rate in a Middle-Aged Chinese Population
Xichang Wang, Haoyu Wang, Jiashu Li, Xiaotong Gao, Yutong Han, Weiping Teng, Zhongyan Shan, Yaxin Lai
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2021; Volume 14: 4513. CrossRef - Determination of “indeterminate score” measurements in lean nonalcoholic fatty liver disease patients from western Saudi Arabia
Yasir Mohammed Khayyat
World Journal of Hepatology.2021; 13(12): 2150. CrossRef - Utility of Liver Function Tests and Fatty Liver Index to Categorize Metabolic Phenotypes in a Mediterranean Population
Dariusz Narankiewicz, Josefina Ruiz-Nava, Veronica Buonaiuto, María Isabel Ruiz-Moreno, María Dolores López-Carmona, Luis Miguel Pérez-Belmonte, Ricardo Gómez-Huelgas, María Rosa Bernal-López
International Journal of Environmental Research and Public Health.2020; 17(10): 3518. CrossRef
- Opportunistic Extraction of Quantitative CT Biomarkers: Turning the Incidental Into Prognostic Information

- Obesity and Metabolism
- Impact of Skeletal Muscle Mass on Metabolic Health
- Gyuri Kim, Jae Hyeon Kim
- Endocrinol Metab. 2020;35(1):1-6. Published online March 19, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.1.1
- 10,692 View
- 293 Download
- 64 Web of Science
- 68 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Skeletal muscle is regarded as an endocrine and paracrine organ. Muscle-derived secretory proteins, referred to as myokines, mediate interactions between skeletal muscle mass and other organs such as the liver, adipose tissue, pancreas, bone, and the cardiovascular system. As individuals age, reduced levels of physical activity and sarcopenia (loss of skeletal muscle mass and strength) are associated with physical frailty and disability. Recently, several studies have suggested that the loss of skeletal muscle mass may contribute to metabolic disease. Therefore, herein, we focus on the relationships between skeletal muscle mass and metabolic diseases, including metabolic syndrome and non-alcoholic fatty liver disease.
-
Citations
Citations to this article as recorded by- Sex differences in the association between dual‐energy x‐ray absorptiometry‐measured body composition and periodontitis
Peijun Zhu, An Li, Qingqing Cai, Yuntao Chen, Yang Liu, Harriët Jager‐Wittenaar, Geerten‐Has E. Tjakkes, Shulan Xu
Journal of Periodontology.2024; 95(3): 219. CrossRef - Advances in the treatment of functional male hypogonadism
Giovanni Corona, Giulia Rastrelli, Clotilde Sparano, Linda Vignozzi, Alessandra Sforza, Mario Maggi
Expert Review of Endocrinology & Metabolism.2024; 19(2): 163. CrossRef - Heterogeneously elevated branched-chain/aromatic amino acids among new-onset type-2 diabetes mellitus patients are potentially skewed diabetes predictors
Min Wang, Yang Ou, Xiang-Lian Yuan, Xiu-Fang Zhu, Ben Niu, Zhuang Kang, Bing Zhang, Anwar Ahmed, Guo-Qiang Xing, Heng Su
World Journal of Diabetes.2024; 15(1): 53. CrossRef - The Vicious Cycle of Type 2 Diabetes Mellitus and Skeletal Muscle Atrophy: Clinical, Biochemical, and Nutritional Bases
Jose M. Lopez-Pedrosa, Maria Camprubi-Robles, German Guzman-Rolo, Andres Lopez-Gonzalez, Jose Manuel Garcia-Almeida, Alejandro Sanz-Paris, Ricardo Rueda
Nutrients.2024; 16(1): 172. CrossRef - FGF21 Induces Skeletal Muscle Atrophy and Increases Amino Acids in Female Mice: A Potential Role for Glucocorticoids
Karlton R Larson, Devi Jayakrishnan, Karla A Soto Sauza, Michael L Goodson, Aki T Chaffin, Arik Davidyan, Suraj Pathak, Yanbin Fang, Diego Gonzalez Magaña, Benjamin F Miller, Karen K Ryan
Endocrinology.2024;[Epub] CrossRef - Mortality risk relationship using standard categorized BMI or knee-height based BMI – does the overweight/lower mortality paradox hold true?
Nivetha Natarajan Gavriilidou, Mats Pihlsgård, Sölve Elmståhl, Henrik Ekström
Aging Clinical and Experimental Research.2024;[Epub] CrossRef - Gromwell (Lithospermum erythrorhizon) Attenuates High-Fat-Induced Skeletal Muscle Wasting by Increasing Protein Synthesis and Mitochondrial Biogenesis
Ji-Sun Kim, Hyunjung Lee, Ahyoung Yoo, Hang Yeon Jeong, Chang Hwa Jung, Jiyun Ahn, Tae-Youl Ha
Journal of Microbiology and Biotechnology.2024; 34(3): 495. CrossRef - L-shaped association between lean body mass to visceral fat mass ratio with hyperuricemia: a cross-sectional study
Longti Li, Ya Shao, Huiqin Zhong, Yu Wang, Rong Zhang, Boxiong Gong, Xiaoxv Yin
Lipids in Health and Disease.2024;[Epub] CrossRef - Prevalence of adiposity-based chronic disease and its association with anthropometric and clinical indices: a cross-sectional study
Luis E González-Salazar, Aurora E Serralde-Zúñiga, Adriana Flores-López, Juan P Díaz-Sánchez, Isabel Medina-Vera, Edgar Pichardo-Ontiveros, Rocío Guizar-Heredia, Karla G Hernández-Gómez, Ana Vigil-Martínez, Liliana Arteaga-Sánchez, Azalia Avila-Nava, Nata
British Journal of Nutrition.2023; 130(1): 93. CrossRef - Skeletal Muscle Myokine Expression in Critical Illness, Association With Outcome and Impact of Therapeutic Interventions
Ilse Vanhorebeek, Jan Gunst, Michaël P Casaer, Inge Derese, Sarah Derde, Lies Pauwels, Johan Segers, Greet Hermans, Rik Gosselink, Greet Van den Berghe
Journal of the Endocrine Society.2023;[Epub] CrossRef - Effect of Circadian Rhythm Disturbance on the Human Musculoskeletal System and the Importance of Nutritional Strategies
Norsham Juliana, Liyana Azmi, Nadia Mohd Effendy, Nur Islami Mohd Fahmi Teng, Izuddin Fahmy Abu, Nur Nabilah Abu Bakar, Sahar Azmani, Noor Anisah Abu Yazit, Suhaini Kadiman, Srijit Das
Nutrients.2023; 15(3): 734. CrossRef - Molecular mechanisms of post‐burn muscle wasting and the therapeutic potential of physical exercise
Dorien Dombrecht, Ulrike Van Daele, Birgit Van Asbroeck, David Schieffelers, Pieter‐Jan Guns, Nick Gebruers, Jill Meirte, Eric van Breda
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(2): 758. CrossRef - Metabolic Impact of Frailty Changes Diabetes Trajectory
Alan J. Sinclair, Ahmed H. Abdelhafiz
Metabolites.2023; 13(2): 295. CrossRef - From Single- to Multi-organ-on-a-Chip System for Studying Metabolic Diseases
Minjeong Jang, Hong Nam Kim
BioChip Journal.2023; 17(2): 133. CrossRef - INFLUENCE OF SARCOPENIA ON THE COURSE AND PROGNOSIS IN PATIENTS WITH CHRONIC HEART FAILURE
Gulyaev N.I., Adamov A.A., Akhmetshin I.M.
"Medical & pharmaceutical journal "Pulse".2023; : 124. CrossRef - Frailty and the Interactions between Skeletal Muscle, Bone, and Adipose Tissue-Impact on Cardiovascular Disease and Possible Therapeutic Measures
María Elena Soto, Israel Pérez-Torres, María Esther Rubio-Ruiz, Agustina Cano-Martínez, Linaloe Manzano-Pech, Verónica Guarner-Lans
International Journal of Molecular Sciences.2023; 24(5): 4534. CrossRef - Sarcoplasmic Reticulum Ca2+ Buffer Proteins: A Focus on the Yet-To-Be-Explored Role of Sarcalumenin in Skeletal Muscle Health and Disease
Elena Conte, Giorgia Dinoi, Paola Imbrici, Annamaria De Luca, Antonella Liantonio
Cells.2023; 12(5): 715. CrossRef - Antarctic krill extracts enhance muscle regeneration and muscle function via mammalian target of rapamycin regulation
Seongmin Lee, Mi-Ock Baek, Sana Abdul Khaliq, Amna Parveen, Sun Yeou Kim, Jin-Hyoung Kim, Il-Chan Kim, Mee-Sup Yoon
Journal of Functional Foods.2023; 103: 105483. CrossRef - Pharmacological and physiological roles of adipokines and myokines in metabolic-related dementia
Archana Arjunan, Juhyun Song
Biomedicine & Pharmacotherapy.2023; 163: 114847. CrossRef - PRMT5 links lipid metabolism to contractile function of skeletal muscles
Kun Ho Kim, Zhihao Jia, Madigan Snyder, Jingjuan Chen, Jiamin Qiu, Stephanie N Oprescu, Xiyue Chen, Sabriya A Syed, Feng Yue, Bruno T Roseguini, Anthony N Imbalzano, Changdeng Hu, Shihuan Kuang
EMBO reports.2023;[Epub] CrossRef - “Biqi” Bayberry Extract Promotes Skeletal Muscle Fiber Type Remodeling by Increasing Fast Myofiber Formation via the Akt/FoxO1 Pathway in Mice
Jinjie Li, Yi Li, Xiangying Suo, Jiangtao Li, Da Huang, Guangning Kou
Foods.2023; 12(13): 2471. CrossRef - Effects of high-intensity interval training (HIIT) on skeletal muscle atrophy, function, and myokine profile in diabetic myopathy
Yeşim Özçatal, Fırat Akat, Yakup Tatar, Hakan Fıçıcılar, Bilge Serdaroğlu, Ferda Topal Çelikkan, Metin Baştuğ
Cytokine.2023; 169: 156279. CrossRef - Impaired proteostatic mechanisms other than decreased protein synthesis limit old skeletal muscle recovery after disuse atrophy
Jordan D. Fuqua, Marcus M. Lawrence, Zachary R. Hettinger, Agnieszka K. Borowik, Parker L. Brecheen, Marcelina M. Szczygiel, Claire B. Abbott, Frederick F. Peelor, Amy L. Confides, Michael Kinter, Sue C. Bodine, Esther E. Dupont‐Versteegden, Benjamin F. M
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(5): 2076. CrossRef - Body physique rating as a factor to identify at-risk Mexicans for Metabolic Syndrome
Oscar Herrera-Fomperosa, Sergio K. Bustamante-Villagomez, Sarahí Vazquez-Álvarez, Gabriela Vázquez-Marroquín, Leonardo M. Porchia, Enrique Torres-Rasgado, Ricardo Pérez-Fuentes, M. Elba Gonzalez-Mejia
Human Nutrition & Metabolism.2023; 33: 200206. CrossRef - Association between Fractional Oxygen Extraction from Resting Quadriceps Muscle and Body Composition in Healthy Men
Rodrigo Yáñez-Sepúlveda, Jorge Olivares-Arancibia, Guillermo Cortés-Roco, Aldo Vasquez-Bonilla, Matías Monsalves-Álvarez, Ildefonso Alvear-Órdenes, Marcelo Tuesta
Journal of Functional Morphology and Kinesiology.2023; 8(4): 149. CrossRef - Correlations between Mental Health, Physical Activity, and Body Composition in American College Students after the COVID-19 Pandemic Lockdown
Luis Torres, Manuela C. Caciula, Alin S. Tomoiaga, Carmen Gugu-Gramatopol
International Journal of Environmental Research and Public Health.2023; 20(22): 7045. CrossRef - Association between total body muscle percentage and prevalence of non-alcoholic fatty liver disease in Korean adults findings from an 18-year follow-up: a prospective cohort study
Byoung Chan Ahn, Chul Yong Park, Jung Hee Hong, Ki Ook Baek
Journal of Yeungnam Medical Science.2023; 40(Suppl): S47. CrossRef - The independent and joint associations among muscle strength, abdominal obesity and cardiometabolic variables among adults
Tiago Rodrigues de Lima, David Alejandro González‐Chica, Xuemei Sui, Diego Augusto Santos Silva
European Journal of Sport Science.2022; 22(7): 1122. CrossRef - Mentale Gesundheit und physische Aktivität
Wolfgang Laube
Manuelle Medizin.2022; 60(1): 13. CrossRef - A new paradigm in sarcopenia: Cognitive impairment caused by imbalanced myokine secretion and vascular dysfunction
Danbi Jo, Gwangho Yoon, Oh Yoen Kim, Juhyun Song
Biomedicine & Pharmacotherapy.2022; 147: 112636. CrossRef - Sarcopenia Is a Cause and Consequence of Metabolic Dysregulation in Aging Humans: Effects of Gut Dysbiosis, Glucose Dysregulation, Diet and Lifestyle
James W. Daily, Sunmin Park
Cells.2022; 11(3): 338. CrossRef - Leveraging deep phenotyping from health check-up cohort with 10,000 Korean individuals for phenome-wide association study of 136 traits
Eun Kyung Choe, Manu Shivakumar, Anurag Verma, Shefali Setia Verma, Seung Ho Choi, Joo Sung Kim, Dokyoon Kim
Scientific Reports.2022;[Epub] CrossRef - Zika virus disrupts gene expression in human myoblasts and myotubes: Relationship with susceptibility to infection
Ingo Riederer, Daniella Arêas Mendes-da-Cruz, Guilherme Cordenonsi da Fonseca, Mariela Natacha González, Otavio Brustolini, Cássia Rocha, Guilherme Loss, Joseane Biso de Carvalho, Mariane Talon Menezes, Lidiane Menezes Souza Raphael, Alexandra Gerber, Myr
PLOS Neglected Tropical Diseases.2022; 16(2): e0010166. CrossRef - Teil 1: Muskeldysfunktionen – mit Training gegen Schmerz
Wolfgang Laube
Manuelle Medizin.2022; 60(2): 84. CrossRef - Transcription factors KLF15 and PPARδ cooperatively orchestrate genome-wide regulation of lipid metabolism in skeletal muscle
Liyan Fan, David R. Sweet, Erica K. Fan, Domenick A. Prosdocimo, Annmarie Madera, Zhen Jiang, Roshan Padmanabhan, Saptarsi M. Haldar, Vinesh Vinayachandran, Mukesh K. Jain
Journal of Biological Chemistry.2022; 298(6): 101926. CrossRef - An Overview of the TRP-Oxidative Stress Axis in Metabolic Syndrome: Insights for Novel Therapeutic Approaches
Mizael C. Araújo, Suzany H. S. Soczek, Jaqueline P. Pontes, Leonardo A. C. Marques, Gabriela S. Santos, Gisele Simão, Laryssa R. Bueno, Daniele Maria-Ferreira, Marcelo N. Muscará, Elizabeth S. Fernandes
Cells.2022; 11(8): 1292. CrossRef - Effects of a 10-Week Physical Activity Intervention on Asylum Seekers’ Physiological Health
Matheus Guerra, Danilo Garcia, Maryam Kazemitabar, Erik Lindskär, Erica Schütz, Daniel Berglind
Brain Sciences.2022; 12(7): 822. CrossRef - Low muscle mass and mortality risk later in life: A 10-year follow-up study
Cristina Camargo Pereira, Valéria Pagotto, Cesar de Oliveira, Erika Aparecida Silveira, Kiyoshi Sanada
PLOS ONE.2022; 17(7): e0271579. CrossRef - Independent and joint associations of weightlifting and aerobic activity with all-cause, cardiovascular disease and cancer mortality in the Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial
Jessica Gorzelitz, Britton Trabert, Hormuzd A Katki, Steven C Moore, Eleanor L Watts, Charles E Matthews
British Journal of Sports Medicine.2022; 56(22): 1277. CrossRef - Handgrip Strength Cutoff Value Among Korean Adolescents with Metabolic Syndrome Components: Korean National Health and Nutrition Examination Survey Data 2014–2017
Chang Hoon Lee, Jun Hyeok Lee, Yong Whi Jeong, Hong Koh, Yunkoo Kang
Metabolic Syndrome and Related Disorders.2022; 20(10): 584. CrossRef - Physical activity level, sitting time, and skeletal muscle mass between esports players and non-esports players
Zhi H. SEE, Mohamad S. ABDUL HAMID
Gazzetta Medica Italiana Archivio per le Scienze Mediche.2022;[Epub] CrossRef - Impact of the Nutrition–Inflammation Status on the Functionality of Patients with Chronic Kidney Disease
Ángel Nogueira, Graciela Álvarez, Guillermina Barril
Nutrients.2022; 14(22): 4745. CrossRef - Does Timing Matter? A Narrative Review of Intermittent Fasting Variants and Their Effects on Bodyweight and Body Composition
Alan A. Aragon, Brad J. Schoenfeld
Nutrients.2022; 14(23): 5022. CrossRef - Sex- and region-specific associations of skeletal muscle mass with metabolic dysfunction-associated fatty liver disease
Pei Xiao, Pu Liang, Panjun Gao, Jinyi Wu
Frontiers in Endocrinology.2022;[Epub] CrossRef - Donor Skeletal Muscle Quality Affects Graft Mortality After Living Donor Liver Transplantation- A Single Center, Retrospective Study
Takahiro Tomiyama, Noboru Harada, Takeo Toshima, Yuki Nakayama, Katsuya Toshida, Akinari Morinaga, Yukiko Kosai-Fujimoto, Takahiro Tomino, Takeshi Kurihara, Kazuki Takeishi, Yoshihiro Nagao, Kazutoyo Morita, Shinji Itoh, Tomoharu Yoshizumi
Transplant International.2022;[Epub] CrossRef - Handgrip Strength Is Associated with Metabolic Syndrome and Insulin Resistance in Children and Adolescents: Analysis of Korea National Health and Nutrition Examination Survey 2014–2018
Hae Woon Jung, Jieun Lee, Jaehyun Kim
Journal of Obesity & Metabolic Syndrome.2022; 31(4): 334. CrossRef - Diet quality and a traditional dietary pattern predict lean mass in Australian women: Longitudinal data from the Geelong Osteoporosis Study
Jessica A. Davis, Mohammadreza Mohebbi, Fiona Collier, Amy Loughman, Nitin Shivappa, James R. Hébert, Julie A. Pasco, Felice N. Jacka
Preventive Medicine Reports.2021; 21: 101316. CrossRef - Association between serum FGF21 level and sarcopenia in older adults
Hee-Won Jung, Jin Hoon Park, Da Ae Kim, Il-Young Jang, So Jeong Park, Jin Young Lee, Seungjoo Lee, Jeoung Hee Kim, Hyon-Seung Yi, Eunju Lee, Beom-Jun Kim
Bone.2021; 145: 115877. CrossRef - Benchside to the bedside of frailty and cardiovascular aging: Main shared cellular and molecular mechanisms
Sandra Maria Barbalho, Ricardo José Tofano, Eduardo Federigui Baisi Chagas, Cláudia Rucco Penteado Detregiachi, Ricardo de Alvares Goulart, Uri Arian Princ Flato
Experimental Gerontology.2021; 148: 111302. CrossRef - Effect of CCL11 on In Vitro Myogenesis and Its Clinical Relevance for Sarcopenia in Older Adults
Da Ae Kim, So Jeong Park, Jin Young Lee, Jeoung Hee Kim, Seungjoo Lee, Eunju Lee, Il-Young Jang, Hee-Won Jung, Jin Hoon Park, Beom-Jun Kim
Endocrinology and Metabolism.2021; 36(2): 455. CrossRef - Sarcopenic obesity as a determinant of cardiovascular disease risk in older people: a systematic review
Katherine Evans, Dima Abdelhafiz, Ahmed H Abdelhafiz
Postgraduate Medicine.2021; 133(8): 831. CrossRef - Decreased continuous sitting time increases heart rate variability in patients with cardiovascular risk factors
Natsuki Nakayama, Masahiko Miyachi, Koji Tamakoshi, Toshio Hayashi, Koji Negi, Koji Watanabe, Makoto Hirai, Sharon Mary Brownie
PLOS ONE.2021; 16(6): e0253399. CrossRef - Muskeltraining – ein universelles Medikament
Wolfgang Laube
Manuelle Medizin.2021; 59(3): 179. CrossRef - The Effects of Oxytocin on Appetite Regulation, Food Intake and Metabolism in Humans
Liya Kerem, Elizabeth A. Lawson
International Journal of Molecular Sciences.2021; 22(14): 7737. CrossRef - Weight Loss Strategies and the Risk of Skeletal Muscle Mass Loss
David McCarthy, Aloys Berg
Nutrients.2021; 13(7): 2473. CrossRef - Association of FGF‐19 and FGF‐21 levels with primary sarcopenia
Rabia Bag Soytas, Veysel Suzan, Pinar Arman, Tugce Emiroglu Gedik, Damla Unal, Mahir Cengiz, Ibrahim Murat Bolayirli, Deniz Suna Erdincler, Alper Doventas, Hakan Yavuzer
Geriatrics & Gerontology International.2021; 21(10): 959. CrossRef - Der Muskulatur mehr Aufmerksamkeit schenken!
Wolfgang Laube
Manuelle Medizin.2021; 59(4): 302. CrossRef - Methodology, clinical applications, and future directions of body composition analysis using computed tomography (CT) images: A review
Antti Tolonen, Tomppa Pakarinen, Antti Sassi, Jere Kyttä, William Cancino, Irina Rinta-Kiikka, Said Pertuz, Otso Arponen
European Journal of Radiology.2021; 145: 109943. CrossRef - Waist and hip circumference are independently associated with the risk of liver disease in population‐based studies
Oscar Danielsson, Markku J. Nissinen, Antti Jula, Veikko Salomaa, Satu Männistö, Annamari Lundqvist, Markus Perola, Fredrik Åberg
Liver International.2021; 41(12): 2903. CrossRef - Understanding of sarcopenia: from definition to therapeutic strategies
Jee Won Kim, Ryuni Kim, Hyerim Choi, Sang-Jin Lee, Gyu-Un Bae
Archives of Pharmacal Research.2021; 44(9-10): 876. CrossRef - Muscle strength and its association with cardiometabolic variables in adolescents: does the expression of muscle strength values matter?
Tiago Rodrigues de Lima, Xuemei Sui, Luiz Rodrigo Augustemak de Lima, Diego Augusto Santos Silva
World Journal of Pediatrics.2021; 17(6): 597. CrossRef - Musclin Is Related to Insulin Resistance and Body Composition, but Not to Body Mass Index or Cardiorespiratory Capacity in Adults
Yeliana L. Sánchez, Manuela Yepes-Calderón, Luis Valbuena, Andrés F. Milán, María C. Trillos-Almanza, Sergio Granados, Miguel Peña, Mauricio Estrada-Castrillón, Juan C. Aristizábal, Raúl Narvez-Sanchez, Jaime Gallo-Villegas, Juan C. Calderón
Endocrinology and Metabolism.2021; 36(5): 1055. CrossRef - Physical Exercise and Myokines: Relationships with Sarcopenia and Cardiovascular Complications
Sandra Maria Barbalho, Uri Adrian Prync Flato, Ricardo José Tofano, Ricardo de Alvares Goulart, Elen Landgraf Guiguer, Cláudia Rucco P. Detregiachi, Daniela Vieira Buchaim, Adriano Cressoni Araújo, Rogério Leone Buchaim, Fábio Tadeu Rodrigues Reina, Piero
International Journal of Molecular Sciences.2020; 21(10): 3607. CrossRef Prevalence of Metabolic Syndrome and Association with Grip Strength in Older Adults: Findings from the HOPE Study
Reshma Aziz Merchant, Yiong Huak Chan, Jia Yi Lim, John E Morley
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2020; Volume 13: 2677. CrossRef- Lower Serum n-3 Fatty Acid Level in Older Adults with Sarcopenia
Il-Young Jang, Hee-Won Jung, Jin Hoon Park, Jeoung Hee Kim, Seungjoo Lee, Eunju Lee, Jin Young Lee, So Jeong Park, Da Ae Kim, Su Jung Kim, Hyun Ju Yoo, Beom-Jun Kim
Nutrients.2020; 12(10): 2959. CrossRef - Advances in understanding of health‐promoting benefits of medicine and food homology using analysis of gut microbiota and metabolomics
Minmin Yang, Tao Yan, Meng Yu, Jie Kang, Ruoxi Gao, Peng Wang, Yuhuan Zhang, Huafeng Zhang, Lin Shi
Food Frontiers.2020; 1(4): 398. CrossRef - The association of circulating kynurenine, a tryptophan metabolite, with frailty in older adults
Il-Young Jang, Jin Hoon Park, Jeoung Hee Kim, Seungjoo Lee, Eunju Lee, Jin Young Lee, So Jeong Park, Da Ae Kim, Mark W. Hamrick, Beom-Jun Kim
Aging.2020; 12(21): 22253. CrossRef - Sarcopenia and Muscle Aging: A Brief Overview
Tam Dao, Alexander E. Green, Yun A Kim, Sung-Jin Bae, Ki-Tae Ha, Karim Gariani, Mi-ra Lee, Keir J. Menzies, Dongryeol Ryu
Endocrinology and Metabolism.2020; 35(4): 716. CrossRef
- Sex differences in the association between dual‐energy x‐ray absorptiometry‐measured body composition and periodontitis

- Obesity and Metabolism
- Nonalcoholic Fatty Liver Disease and Diabetes: An Epidemiological Perspective
- Eun-Jung Rhee
- Endocrinol Metab. 2019;34(3):226-233. Published online September 26, 2019
- DOI: https://doi.org/10.3803/EnM.2019.34.3.226
- 10,691 View
- 313 Download
- 66 Web of Science
- 68 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Nonalcoholic fatty liver disease (NAFLD) is thought to stem from the body's inability to store excess energy in adipocytes; as such, it is commonly viewed as the hepatic manifestation of metabolic syndrome. The pathogenesis of NAFLD involves ectopic fat accumulation, which also takes place in the liver, muscle and visceral fat. NAFLD is rapidly becoming more widespread in Korea, with an estimated prevalence of 30% in adults. Type 2 diabetes mellitus (T2DM) and NAFLD share insulin resistance as a common pathophysiological mechanism, and each of these two diseases affects the development of the other. Recent studies have suggested that NAFLD is often present as a comorbidity in T2DM patients. The mutual interrelationship between these conditions is shown by findings suggesting that T2DM can exacerbate NAFLD by promoting progression to nonalcoholic hepatosteatosis or fibrosis, while NAFLD causes the natural course of diabetic complications to worsen in T2DM patients. It remains unknown whether one disease is the cause of the other or vice versa. In this review, I would like to discuss current epidemiological data on the associations between NAFLD and T2DM, and how each disease affects the course of the other.
-
Citations
Citations to this article as recorded by- Effect of exercise intervention on clinical parameters in patients with non-alcoholic fatty liver disease and type 2 diabetes mellitus: a meta-analysis of randomized controlled trials
Yu Zeng, Xuemei Zhang, Wenling Luo, Yunjian Sheng
European Journal of Gastroenterology & Hepatology.2024; 36(1): 1. CrossRef - Phase 2, open-label, rollover study of cenicriviroc for liver fibrosis associated with metabolic dysfunction–associated steatohepatitis
Sven M. Francque, Alexander Hodge, Jerome Boursier, Ziad H. Younes, Gerardo Rodriguez-Araujo, Grace S. Park, Naim Alkhouri, Manal F. Abdelmalek
Hepatology Communications.2024;[Epub] CrossRef - Two-Year Therapeutic Efficacy and Safety of Initial Triple Combination of Metformin, Sitagliptin, and Empagliflozin in Drug-Naïve Type 2 Diabetes Mellitus Patients
Young-Hwan Park, Minji Sohn, So Yeon Lee, Soo Lim
Diabetes & Metabolism Journal.2024; 48(2): 253. CrossRef - Research Progress of Traditional Chinese Medicine and Western Medicine on Non-Alcoholic Fatty Liver Disease
强江 郭
Advances in Clinical Medicine.2024; 14(03): 561. CrossRef - Anti-osteoporotic treatments in the era of non-alcoholic fatty liver disease: friend or foe
Maria Eleni Chondrogianni, Ioannis Kyrou, Theodoros Androutsakos, Christina-Maria Flessa, Evangelos Menenakos, Kamaljit Kaur Chatha, Yekaterina Aranan, Athanasios G. Papavassiliou, Eva Kassi, Harpal S. Randeva
Frontiers in Endocrinology.2024;[Epub] CrossRef - Obeticholic Acid and Insulin Sensitivity in Overweight Patients with Prediabetes
H. Amer, M. Nesim, H. Mansour, E. Nasr, N. Ahmed
Obesity and metabolism.2024;[Epub] CrossRef - Utility of Indices Obtained during Medical Checkups for Predicting Fatty Liver Disease in Non-obese People
Naoya Otsubo, Tatsuya Fukuda, Genhin Cho, Fumiaki Ishibashi, Tetsuya Yamada, Koshiro Monzen
Internal Medicine.2023; 62(16): 2307. CrossRef - Liraglutide on type 2 diabetes mellitus with nonalcoholic fatty liver disease: A systematic review and meta-analysis of 16 RCTs
Yan Zhao, Wenli Zhao, Huaien Bu, Maeda Toshiyoshi, Ye Zhao
Medicine.2023; 102(6): e32892. CrossRef - Metabolic Dysfunction-Associated Fatty Liver Disease and Mortality: A Population-Based Cohort Study
Kyung-Soo Kim, Sangmo Hong, Hong-Yup Ahn, Cheol-Young Park
Diabetes & Metabolism Journal.2023; 47(2): 220. CrossRef - Metabolomics analysis reveals serum biomarkers in patients with diabetic sarcopenia
Yuwei Tan, Xiaosong Liu, Yinping Yang, Baoying Li, Fei Yu, Wenqian Zhao, Chunli Fu, Xin Yu, Zhenxia Han, Mei Cheng
Frontiers in Endocrinology.2023;[Epub] CrossRef - Antagonizing apolipoprotein J chaperone promotes proteasomal degradation of mTOR and relieves hepatic lipid deposition
Shuangdi Duan, Nong Qin, Jiayi Pi, Pei Sun, Yating Gao, Lamei Liu, Zenghui Li, Ya Li, Liyang Shi, Qiang Gao, Ye Qiu, Songqing Tang, Chun-Hsiang Wang, Tzu-Ying Chen, Sin-Tian Wang, Kung-Chia Young, Hung-Yu Sun
Hepatology.2023; 78(4): 1182. CrossRef - The Influence of Metabolic Factors in Patients with Chronic Viral Hepatitis C Who Received Oral Antiviral Treatment
Oana Irina Gavril, Radu Sebastian Gavril, Florin Mitu, Otilia Gavrilescu, Iolanda Valentina Popa, Diana Tatarciuc, Andrei Drugescu, Andrei Catalin Oprescu, Andreea Gherasim, Laura Mihalache, Irina Mihaela Esanu
Metabolites.2023; 13(4): 571. CrossRef - The bidirectional relationship between NAFLD and type 2 diabetes: A prospective population-based cohort study
Minzhen Wang, Yanan Zhao, Yingqian He, Lulu Zhang, Jing Liu, Shan Zheng, Yana Bai
Nutrition, Metabolism and Cardiovascular Diseases.2023; 33(8): 1521. CrossRef - Visceral fat: A key mediator of NAFLD development and progression
Savita Bansal, Meenakshi Vachher, Taruna Arora, Bhupender Kumar, Archana Burman
Human Nutrition & Metabolism.2023; 33: 200210. CrossRef - Greater Severity of Steatosis Is Associated with a Higher Risk of Incident Diabetes: A Retrospective Longitudinal Study
Ji Min Han, Jung Hwan Cho, Hye In Kim, Sunghwan Suh, Yu-Ji Lee, Jung Won Lee, Kwang Min Kim, Ji Cheol Bae
Endocrinology and Metabolism.2023; 38(4): 418. CrossRef - The role of TRIM family in metabolic associated fatty liver disease
Jingyue Zhang, Yingming Zhang, Ze Ren, Dongmei Yan, Guiying Li
Frontiers in Endocrinology.2023;[Epub] CrossRef - Non-alcoholic fatty liver disease and diabetic retinopathy: Is there an association?
Mathew Jacob, Mary Joseph, Jyothi Idiculla
Journal of Family Medicine and Primary Care.2023; 12(9): 2028. CrossRef - Camel whey protein improves diabetic liver injury by targeting ACMSD and promoting de novo NAD+ synthesis
Zhihua Dou, Huaibin Yao, Yutong Xie, Ying Liu, Yang Gao, Jie Yang
Journal of Functional Foods.2023; 110: 105835. CrossRef - Gut microbiota and nonalcoholic fatty liver disease
Boyeon Kim, Bukyung Kim
Kosin Medical Journal.2023; 38(3): 169. CrossRef - Non-alcoholic fatty liver disease in patients with type 2 diabetes mellitus
E.G. Mankieva, E.I. Kukhareva
Dokazatel'naya gastroenterologiya.2023; 12(4): 103. CrossRef - Body Fat Distribution, Glucose Metabolism, and Diabetes Status Among Older Adults: The Multiethnic Cohort Adiposity Phenotype Study
Gertraud Maskarinec, Phyllis Raquinio, Bruce S. Kristal, Adrian A. Franke, Steven D. Buchthal, Thomas M. Ernst, Kristine R. Monroe, John A. Shepherd, Yurii B. Shvetsov, Loïc Le Marchand, Unhee Lim
Journal of Epidemiology.2022; 32(7): 314. CrossRef - Evaluation of the reciprocal interaction between hepatic steatosis and type 2 diabetes: a comparative analysis with respect to anti-diabetic treatment, glycemic control, renal and hepatic function
Teslime Ayaz, Hatice Beyazal Polat, Bilgesah Kilictas
International Journal of Diabetes in Developing Countries.2022; 42(3): 421. CrossRef - Glycemic control, the unconsidered outcome in the treatment of nonalcoholic fatty liver disease
Diego García-Compeán, Emanuela Orsi, Tsutomu Nishida, Ramesh Kumar
Annals of Hepatology.2022; 27(1): 100648. CrossRef - Prevalence of High and Moderate Risk Nonalcoholic Fatty Liver Disease Among Adults in the United States, 1999–2016
Pegah Golabi, James M. Paik, Michael Harring, Elena Younossi, Khaled Kabbara, Zobair M. Younossi
Clinical Gastroenterology and Hepatology.2022; 20(12): 2838. CrossRef - The Influence of Obesity and Metabolic Health on Vascular Health
Eun-Jung Rhee
Endocrinology and Metabolism.2022; 37(1): 1. CrossRef - Lifestyle as well as metabolic syndrome and non-alcoholic fatty liver disease: an umbrella review of evidence from observational studies and randomized controlled trials
Xiaojuan Peng, Juan Li, Hailiang Zhao, Junlong Lai, Junqin Lin, Shaohui Tang
BMC Endocrine Disorders.2022;[Epub] CrossRef - The Impact of Insulin Resistance on Hepatic Fibrosis among United States Adults with Non-Alcoholic Fatty Liver Disease: NHANES 2017 to 2018
Ji Cheol Bae, Lauren A. Beste, Kristina M. Utzschneider
Endocrinology and Metabolism.2022; 37(3): 455. CrossRef - Extra-Glycemic Effects of Anti-Diabetic Medications: Two Birds with One Stone?
Eun-Jung Rhee
Endocrinology and Metabolism.2022; 37(3): 415. CrossRef - Structurally‐engineered fatty acid 1024 (SEFA‐1024) improves diet‐induced obesity, insulin resistance, and fatty liver disease
Jordon D. Secor, Bennet S. Cho, Lumeng J. Yu, Amy Pan, Victoria H. Ko, Duy T. Dao, Michael Feigh, Lorenzo Anez‐Bustillos, Gillian L. Fell, David A. Fraser, Kathleen M. Gura, Mark Puder
Lipids.2022; 57(4-5): 241. CrossRef - Impact of COVID-19 Lockdown on Non-Alcoholic Fatty Liver Disease and Insulin Resistance in Adults: A before and after Pandemic Lockdown Longitudinal Study
Ángel Arturo López-González, Bárbara Altisench Jané, Luis Masmiquel Comas, Sebastiana Arroyo Bote, Hilda María González San Miguel, José Ignacio Ramírez Manent
Nutrients.2022; 14(14): 2795. CrossRef - Captopril and Spironolactone can Attenuate Diabetic Nephropathy in Wistar Rats
by Targeting ABCA1 and microRNA-33
Tina Ghaffari, Nariman Moradi, Elham Chamani, Zahra Ebadi, Reza Fadaei, Shahin Alizadeh-Fanalou, Sahar Yarahmadi, Soudabeh Fallah
Current Pharmaceutical Design.2022; 28(16): 1367. CrossRef - Elevated serum γ-glutamyl transferase is associated with low muscle function in adults independent of muscle mass
Seunghyun Lee, Dawon Song, Sungjae Shin, Namki Hong, Yumie Rhee
Nutrition.2022; 103-104: 111813. CrossRef - Cross-sectional association between prolactin levels and non-alcoholic fatty liver disease in patients with type 2 diabetes mellitus: a retrospective analysis of patients from a single hospital in China
Yuanyuan Zhang, Huaizhen Liu
BMJ Open.2022; 12(10): e062252. CrossRef - Non-invasive screening, staging and management of metabolic dysfunction-associated fatty liver disease (MAFLD) in type 2 diabetes mellitus patients : what do we know so far ?
Q Binet, A Loumaye, V Preumont, J-P Thissen, M.P. Hermans, N Lanthier
Acta Gastro Enterologica Belgica.2022; 85(2): 346. CrossRef - Diosgenin Ameliorated Type II Diabetes-Associated Nonalcoholic Fatty Liver Disease through Inhibiting De Novo Lipogenesis and Improving Fatty Acid Oxidation and Mitochondrial Function in Rats
Yujie Zhong, Zhiman Li, Ruyi Jin, Yanpeng Yao, Silan He, Min Lei, Xin Wang, Chao Shi, Li Gao, Xiaoli Peng
Nutrients.2022; 14(23): 4994. CrossRef - Correlation between Component Factors of Non-Alcoholic Fatty Liver Disease and Metabolic Syndrome in Nurses: An Observational and Cross-Sectional Study
Wen-Pei Chang, Yu-Pei Chang
International Journal of Environmental Research and Public Health.2022; 19(23): 16294. CrossRef - Recent advances and potentiality of postbiotics in the food industry: Composition, inactivation methods, current applications in metabolic syndrome, and future trends
Yujie Zhong, Tao Wang, Ruilin Luo, Jiayu Liu, Ruyi Jin, Xiaoli Peng
Critical Reviews in Food Science and Nutrition.2022; : 1. CrossRef - Holistic analysis of hepatosteatosis literature: a scientometric study of global hepatosteatosis publications between 1980 and 2019
Fatih ESKİN, Engin ŞENEL
Journal of Medicine and Palliative Care.2022; 3(4): 300. CrossRef - Terpenoids: Natural Compounds for Non-Alcoholic Fatty Liver Disease (NAFLD) Therapy
Pengyu Yao, Yajuan Liu
Molecules.2022; 28(1): 272. CrossRef - Association of Non-Alcoholic Fatty Liver Dis-ease and Diabetic Retinopathy in Patients with Type 2 Diabetes Mellitus: a Cross-Sectional Study
Zahra Heidari, Zahra Sharafi
Iranian South Medical Journal.2022; 25(1): 30. CrossRef - Race and Ethnicity in Non-Alcoholic Fatty Liver Disease (NAFLD): A Narrative Review
Kiarash Riazi, Mark G. Swain, Stephen E. Congly, Gilaad G. Kaplan, Abdel-Aziz Shaheen
Nutrients.2022; 14(21): 4556. CrossRef - MAFLD vs. NAFLD: shared features and potential changes in epidemiology, pathophysiology, diagnosis, and pharmacotherapy
Ying-Xin Xian, Jian-Ping Weng, Fen Xu
Chinese Medical Journal.2021; 134(1): 8. CrossRef - Factors associated with elevated alanine aminotransferase in employees of a German chemical company: results of a large cross-sectional study
Matthias Claus, Christoph Antoni, Bernd Hofmann
BMC Gastroenterology.2021;[Epub] CrossRef - Treatment potential of LPCN 1144 on liver health and metabolic regulation in a non-genomic, high fat diet induced NASH rabbit model
P. Comeglio, E. Sarchielli, S. Filippi, I. Cellai, G. Guarnieri, A. Morelli, G. Rastrelli, E. Maseroli, S. Cipriani, T. Mello, A. Galli, B. J. Bruno, K. Kim, K. Vangara, K. Papangkorn, N. Chidambaram, M. V. Patel, M. Maggi, L. Vignozzi
Journal of Endocrinological Investigation.2021; 44(10): 2175. CrossRef - Cellular protein markers, therapeutics, and drug delivery strategies in the treatment of diabetes-associated liver fibrosis
Chien-Yu Lin, Pratik Adhikary, Kun Cheng
Advanced Drug Delivery Reviews.2021; 174: 127. CrossRef - Trend for Clinical Use of Metabolic Associated Fatty Liver Disease (MAFLD)
Hiroshi Bando
Asploro Journal of Biomedical and Clinical Case Reports.2021; 4(2): 99. CrossRef - Prediction of Cardiovascular Risk Using Nonalcoholic Fatty Liver Disease Scoring Systems
Ye-Na Kweon, Hae-Jin Ko, A-Sol Kim, Hye-In Choi, Ji-Eun Song, Ji-Yeon Park, Sung-Min Kim, Hee-Eun Hong, Kyung-Jin Min
Healthcare.2021; 9(7): 899. CrossRef - Melatonin ameliorates hepatic steatosis by inhibiting NLRP3 inflammasome in db/db mice
Yongxiang Yu, Dongru Chen, Yuhua Zhao, Jianjun Zhu, Xiaohui Dong
International Journal of Immunopathology and Pharmacology.2021; 35: 205873842110368. CrossRef - Non-Alcoholic Fatty Liver Disease and Its Association With Diabetes Mellitus
Jaskamal Padda, Khizer Khalid, Anwar Khedr, Fahriba Tasnim, Ola A Al-Ewaidat, Ayden Charlene Cooper, Gutteridge Jean-Charles
Cureus.2021;[Epub] CrossRef - Nonalcoholic fatty liver disease and the risk of insulin-requiring gestational diabetes
Sang Youn You, Kyungdo Han, Seung-Hawn Lee, Mee Kyoung Kim
Diabetology & Metabolic Syndrome.2021;[Epub] CrossRef - Serum syndecan‐4 is associated with nonalcoholic fatty liver disease
Shu Jing Xia, Li Zhong Tang, Wen Hua Li, Zhao Shan Xu, Li Li Zhang, Feng Gan Cheng, Hong Xia Chen, Zi Hua Wang, Yu Cheng Luo, An Na Dai, Jian Gao Fan
Journal of Digestive Diseases.2021; 22(9): 536. CrossRef - Non-Laboratory-Based Simple Screening Model for Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Developed Using Multi-Center Cohorts
Jiwon Kim, Minyoung Lee, Soo Yeon Kim, Ji-Hye Kim, Ji Sun Nam, Sung Wan Chun, Se Eun Park, Kwang Joon Kim, Yong-ho Lee, Joo Young Nam, Eun Seok Kang
Endocrinology and Metabolism.2021; 36(4): 823. CrossRef - Grape pomace reduces the severity of non-alcoholic hepatic steatosis and the development of steatohepatitis by improving insulin sensitivity and reducing ectopic fat deposition in mice
Tehila Daniel, Michaella Ben-Shachar, Elyashiv Drori, Sharleen Hamad, Anna Permyakova, Elad Ben-Cnaan, Joseph Tam, Zohar Kerem, Tovit Rosenzweig
The Journal of Nutritional Biochemistry.2021; 98: 108867. CrossRef - The Interplay between Insulin Resistance, Inflammation, Oxidative Stress, Base Excision Repair and Metabolic Syndrome in Nonalcoholic Fatty Liver Disease
Sylwia Ziolkowska, Agata Binienda, Maciej Jabłkowski, Janusz Szemraj, Piotr Czarny
International Journal of Molecular Sciences.2021; 22(20): 11128. CrossRef - The Leg Fat to Total Fat Ratio Is Associated with Lower Risks of Non-Alcoholic Fatty Liver Disease and Less Severe Hepatic Fibrosis: Results from Nationwide Surveys (KNHANES 2008–2011)
Hyun Min Kim, Yong-ho Lee
Endocrinology and Metabolism.2021; 36(6): 1232. CrossRef - Tip 2 Diyabet Modeli Ratların Karaciğer Dokularında Kodlanan Genlerin İfade Düzeyleri
Lütfiye ÖZPAK, Ayfer PAZARBAŞI
Ankara Sağlık Bilimleri Dergisi.2021; 10(1): 25. CrossRef - Gut microbiota and human NAFLD: disentangling microbial signatures from metabolic disorders
Judith Aron-Wisnewsky, Chloé Vigliotti, Julia Witjes, Phuong Le, Adriaan G. Holleboom, Joanne Verheij, Max Nieuwdorp, Karine Clément
Nature Reviews Gastroenterology & Hepatology.2020; 17(5): 279. CrossRef - Non-alcoholic fatty liver disease and primary care physicians
Ludovico Abenavoli, Anna C. Procopio, Milica Medić-Stojanoska, Francesco Luzza
Minerva Gastroenterologica e Dietologica.2020;[Epub] CrossRef - The Role of Insulin Resistance and Diabetes in Nonalcoholic Fatty Liver Disease
Hideki Fujii, Norifumi Kawada
International Journal of Molecular Sciences.2020; 21(11): 3863. CrossRef - Active vitamin D supplementation alleviates initiation and progression of nonalcoholic fatty liver disease by repressing the p53 pathway
Yuanyuan Liu, Mengjie Wang, Wei Xu, Hongman Zhang, Weihe Qian, Xiang Li, Xingbo Cheng
Life Sciences.2020; 241: 117086. CrossRef - Serum lipoprotein(a) levels and insulin resistance have opposite effects on fatty liver disease
Inha Jung, Hyemi Kwon, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki-Won Oh, Sung-Woo Park, Eun-Jung Rhee
Atherosclerosis.2020; 308: 1. CrossRef - The effect of liraglutide on nonalcoholic fatty liver disease in type 2 diabetes mellitus
Xueyang Zhang, Ran Bai, Yong Jia, Junwei Zong, Yongbo Wang, Yanan Dong
International Journal of Diabetes in Developing Countries.2020; 40(4): 491. CrossRef - Association between Thyroid Function and Nonalcoholic Fatty Liver Disease in Euthyroid Type 2 Diabetes Patients
Bin Huang, Shengju Yang, Shandong Ye
Journal of Diabetes Research.2020; 2020: 1. CrossRef - The Absence of NLRP3-inflammasome Modulates Hepatic Fibrosis Progression, Lipid Metabolism, and Inflammation in KO NLRP3 Mice during Aging
Paloma Gallego, Beatriz Castejón-Vega, José A. del Campo, Mario D. Cordero
Cells.2020; 9(10): 2148. CrossRef - Prevalence of people at risk of developing type 2 diabetes mellitus and the involvement of community pharmacies in a national screening campaign: a pioneer action in Brazil
Cassyano J. Correr, Wendel Coura-Vital, Josélia C. Q. P. Frade, Renata C. R. M. Nascimento, Lúbia G. Nascimento, Eliete B. Pinheiro, Wesley M. Ferreira, Janice S. Reis, Karla F. S. Melo, Roberto Pontarolo, Mônica S. A. Lenzi, José V. Almeida, Hermelinda C
Diabetology & Metabolic Syndrome.2020;[Epub] CrossRef - Beneficial effect of anti-diabetic drugs for nonalcoholic fatty liver disease
Kyung-Soo Kim, Byung-Wan Lee
Clinical and Molecular Hepatology.2020; 26(4): 430. CrossRef Elevated TPOAb is a Strong Predictor of Autoimmune Development in Patients of Type 2 Diabetes Mellitus and Non-Alcoholic Fatty Liver Disease: A Case–Control Study
Chenyi Wang, Qianglong Niu, Haihong Lv, Qian Li, Yuping Ma, Jiaojiao Tan, Chunhua Liu
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2020; Volume 13: 4369. CrossRef- Sarcopoterium spinosum Inhibited the Development of Non-Alcoholic Steatosis and Steatohepatitis in Mice
Ayala Wollman, Tehila Daniel, Tovit Rosenzweig
Nutrients.2019; 11(12): 3044. CrossRef
- Effect of exercise intervention on clinical parameters in patients with non-alcoholic fatty liver disease and type 2 diabetes mellitus: a meta-analysis of randomized controlled trials


 KES
KES

 First
First Prev
Prev



