Comparison of Serum Adipocytokine Levels according to Metabolic Health and Obesity Status
Article information
Abstract
Background
Metabolic health is an emerging concept that is highly correlated with various metabolic complications, and adipocytokines have been causally linked to a wide range of metabolic diseases. Thus, this study compared serum adipocytokine levels according to metabolic health and obesity status.
Methods
Four hundred and fifty-six nondiabetic subjects (mean age, 40.5 years) were categorized into four groups according to metabolic health and obesity status: metabolically healthy nonobese (MHNO), metabolically healthy obese (MHO), metabolically unhealthy nonobese (MUHNO), and metabolically unhealthy obese (MUHO). Being metabolically healthy was defined as the presence of fewer than two of the following five metabolic abnormalities: high blood pressure, high fasting blood glucose, high triglyceride, low high density lipoprotein cholesterol, and being in the highest decile of the homeostatic model assessment of insulin resistance index. Obesity status was assessed using body mass index (BMI), with obesity defined as a BMI higher than 25 kg/m2. Levels of serum interleukin-6 (IL-6), monocyte chemoattractant protein-1 (MCP-1), tumor necrosis factor α (TNF-α), and adipocyte fatty acid binding protein (A-FABP) were also evaluated.
Results
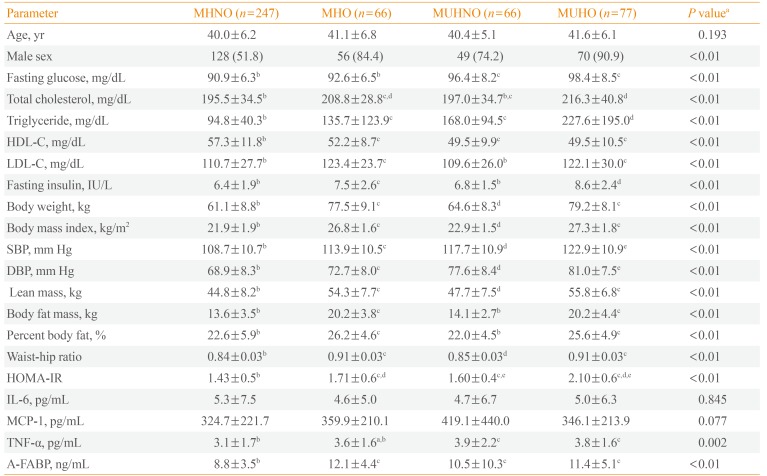
Of the 456 subjects, 247 (54.2%) were in the MHNO group, 66 (14.5%) were in the MHO group, 66 (14.5%) were in the MUHNO group, and 77 (16.9%) were in the MUHO group. There were no significant differences in IL-6 or MCP-1 levels among the groups, but levels of TNF-α and A-FABP were significantly higher in the MUHNO group compared to the MHNO group.
Conclusion
High TNF-α and A-FABP levels are significantly associated with metabolically unhealthiness in nonobese Korean individuals.
INTRODUCTION
The prevalence of obesity continues to increase worldwide, and it has been projected that more than 1 billion people will be afflicted with this condition by 2030 [1]. Obesity is a risk factor for comorbid conditions such as type 2 diabetes mellitus (T2DM), hypertension, cardiovascular disease, stroke, and several types of cancer [23], which are all associated with an increased risk for premature death.
The term metabolically healthy obese (MHO) is now widely used to describe a subtype of obesity that appears to be protected against obesity-related metabolic comorbidities and mortality [456]. Compared to metabolically unhealthy individuals, metabolically healthy individuals possess a favorable metabolic profile that is characterized by a high degree of insulin sensitivity [7], a lesser state of inflammation [8], and favorable lipid and hepatic enzyme profiles [910].
The discovery of adipocytokines, which are products of adipose tissue, was a turning point in the understanding of metabolic disease. Adipocytokines play an important role in the metabolic homeostasis of healthy subjects, and changes in the levels and activity of these factors in obese subjects contribute to metabolic complications [11]. Accordingly, the measurement of serum adipocytokine levels could be helpful for assessing subclinical metabolic disturbances. Although underlying mechanisms that could explain favorable metabolic profile of MHO individuals are largely unknown, adipocytokines might be key factors of metabolic health in view of the fact that they are significantly associated with metabolic diseases [12].
Relatively few studies have examined the relationships among adipocytokines, metabolic health, and obesity [913]. Thus, the present study compared serum adipocytokine levels according to metabolic health and obesity status in an Asian population.
METHODS
Subjects
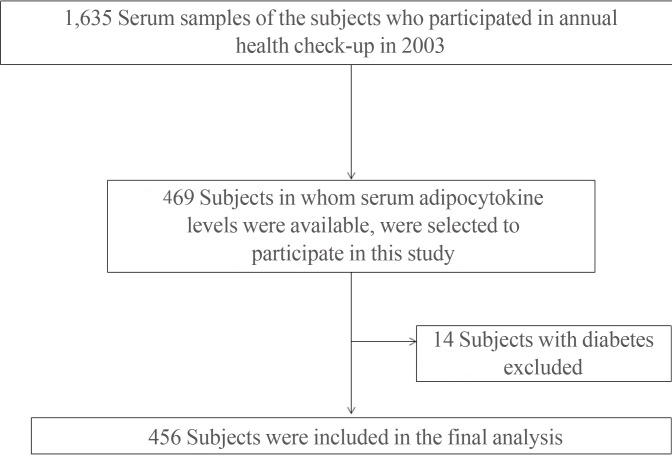
This study was performed as a substudy in the Kangbuk Samsung Medical Center-adipokine study, which is a longitudinal study performed in subjects who received annual health check-ups at the Health Promotion Center at Kangbuk Samsung Hospital in Seoul, Korea, between 2003 and 2007 [14]. One thousand six hundred and thirty-five serum samples of the subjects who participated in annual health check-up in 2003, 469 subjects in whom serum adipocytokine levels were available, were selected to participate in this study. Among these, 456 subjects (303 men and 153 women) after exclusion of 14 subjects with diabetes were enrolled in final analysis as a cross-sectional study (mean age, 40.5 years) (Fig. 1).
The study protocol conformed to ethical guidelines of the 1975 Declaration of Helsinki, and accordingly the Kangbuk Samsung Hospital Human Research Committee approved it. The Institutional Review Board of Kangbuk Samsung Hospital also approved this study and no specific informed consent was obtained. The informed consent requirement for this study was exempted by the Institutional Review Board at the time the study was in the planning phase because researchers only accessed the database for analysis purposes, which was free of identifying personal information.
Anthropometric and laboratory measurements
Height and weight were measured twice using automated instruments and then averaged. The body mass index (BMI) was calculated as by dividing the weight in kilogram by the square of the height in meters. Blood pressure (BP) was measured using a standardized sphygmomanometer after 5 minutes of rest. The waist circumference was measured in the standing position, at the middle point between anterior iliac crest and lower border of rib by a single examiner.
Body composition measurements of the subjects were carried out by segmental bioelectric impedance, using eight tractile electrodes according to the manufacturer's instructions (InBody 3.0, Biospace, Seoul, Korea). Lean mass (kg), fat mass (kg), percent fat mass (%), and waist-hip ratio as a marker of abdominal obesity, were measured.
All of the subjects were examined after an overnight fast. The hexokinase method was used to test fasting glucose concentrations (Hitachi Modular D2400, Roche, Tokyo, Japan). Fasting insulin concentrations were determined by electrochemiluminescence immunoassay (Hitachi Modular E170, Roche). An enzymatic calorimetric test was used to measure the total cholesterol (TC) and triglyceride (TG) concentrations. The selective inhibition method was used to measure the level of high density lipoprotein cholesterol (HDL-C), and a homogeneous enzymatic calorimetric test was used to measure the level of low density lipoprotein cholesterol (LDL-C). Samples for measurement of interleukin-6 (IL-6), monocyte chemoattractant protein-1 (MCP-1), tumor necrosis factor α (TNF-α), and adipocyte fatty acid binding protein (A-FABP) were distributed to tubes and stored at -80℃ prior to measurement of serum levels by an enzyme-linked immunosorbent assay method (BioVendor Laboratory Medicine, Modrice, The Czech Republic). Hemoglobin A1c was measured by immunoturbidimetric assay with a Cobra Integra 800 automatic analyzer (Roche Diagnostics, Basel, Switzerland) with a reference value of 4.4% to 6.4%. The methodology was aligned with the Diabetes Control and Complications Trial and National Glycohemoglobin Standardization Program (NGSP) standards [15]. The intra-assay coefficient of variation (CV) was 2.3% and interassay CV was 2.4%, both within the NGSP acceptable limits [16].
The subjects with underlying diabetes were excluded from the study. The presence of impaired fasting glucose and diabetes mellitus (DM) was determined according to the self-questionnaire of the participants and the diagnostic criteria of American Diabetes Association [17]. Insulin resistance was measured using the homeostatic model assessment of insulin resistance (HOMA-IR) and was obtained by applying the following formula: HOMA-IR=fasting insulin (IU/mL)×fasting blood glucose (mmol/L)/22.5 [18].
Definition of metabolic health and obesity status
Obesity status was defined based on the combined consideration of obesity status by BMI category (nonobese <25 kg/m2, obese ≥25 kg/m2). In 2000, the World Health Organization Western Pacific Region suggested revised Asia-Pacific criteria of obesity in Asian populations using reduced values for BMI ≥25 kg/m2 in both sexes [19].
Being metabolically healthy was defined by having less than two metabolic abnormalities among the four components of metabolic syndrome besides waist circumference criteria plus insulin resistance status defined by HOMA-IR, which was modified from the criteria by Wildman et al. [2021]:
(1) Systolic BP ≥130 mm Hg and/or diastolic BP ≥85 mm Hg or on antihypertensive treatment
(2) TG ≥150 mg/dL
(3) Fasting glucose ≥100 mg/dL
(4) HDL-C <40 mg/dL in men, <50 mg/dL in women
(5) HOMA-IR ≥90th percentile (≥2.28)
According to the above criteria, participants were divided into four groups:
(1) Metabolically healthy nonobese (MHNO): BMI <25 kg/m2 and <2 metabolic risk factor
(2) MHO: BMI ≥25 kg/m2 and <2 metabolic risk factor
(3) Metabolically unhealthy nonobese (MUHNO): BMI <25 kg/m2 and ≥2 metabolic risk factor
(4) Metabolically unhealthy obese (MUHO): BMI ≥25 kg/m2 and ≥2 metabolic risk factor
Statistical analysis
All data were analyzed using SPSS version 18.0 (SPSS Inc., Chicago, IL, USA). Comparisons of the mean values and the prevalence of metabolic variables among the four groups divided by metabolic health and obesity status were performed with one-way analysis of variance test and chi-square test, and data that do not follow normal distribution were analyzed after logarithmic transformation. Bivariate correlation analysis was performed to evaluate relation between metabolic parameters and adipocytokines. Statistical significance was defined as P<0.05.
RESULTS
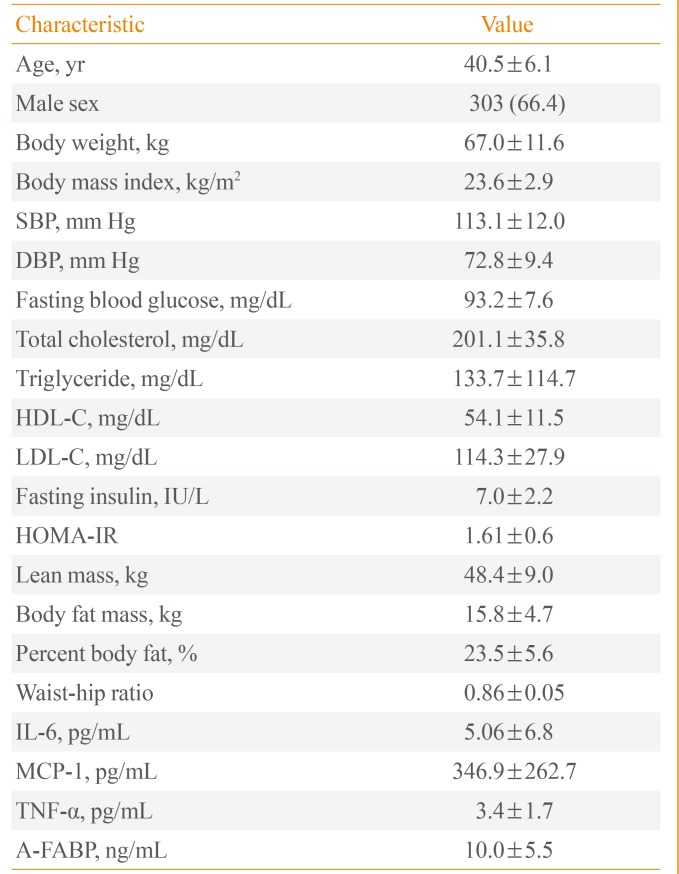
The general characteristics of the participants are presented in Table 1. For all participants, the mean age was 40.5 years, and the proportion of males was 66.4% (303/456). Of the 456 subjects, 247 (54.2%) were in the MHNO group, 66 (14.5%) were in the MHO group, 66 (14.5%) were in the MUHNO group, and 77 (16.9%) were in the MUHO group (Table 2).
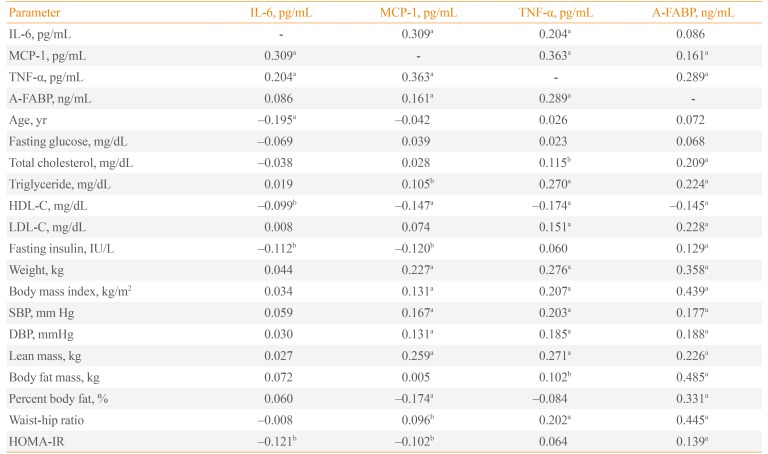
A bivariate correlation analysis, which included metabolic variables with adipocytokines, TNF-α and A-FABP showed significant correlation with TC, TG, HDL-C, LDL-C, BMI, BP, and body fat mass (Table 3).
MUHNO group had a higher proportion of males, higher average BMI and BP; and higher levels of serum fasting glucose and TG; and lower level of serum HDL-C compared with MHNO group. MUHO group had a higher proportion of males, higher BP; and higher levels of serum fasting glucose, TG, and fasting insulin compared with MHO group. Among measured adipocytokines, IL-6 and MCP-1 levels did not differ significantly among four groups. MUHNO group showed significantly higher levels of TNF-α and A-FABP than those of MHNO group (Fig. 2). Meanwhile, there was no significant difference in levels of TNF-α and A-FABP between MUHO and MHO groups.
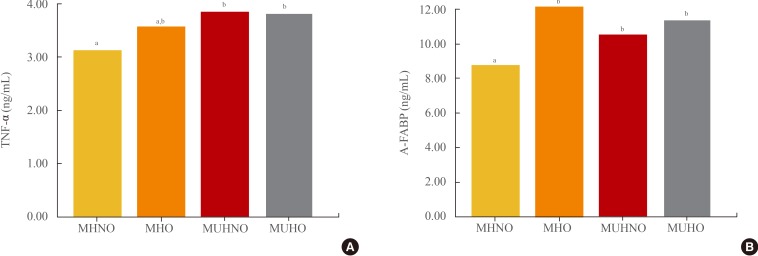
Comparison of mean (A) tumor necrosis factor α (TNF-α) and (B) adipocyte fatty acid binding protein (A-FABP) levels according to four groups divided by metabolic health and obesity. MHNO, metabolically healthy nonobese; MHO, metabolically healthy obese; MUHNO, metabolically unhealthy nonobese; MUHO, metabolically unhealthy obese. a,bDifferent letters denote significant differences between the designated groups in post hoc analyses. Otherwise, groups showed no significant differences between each groups with post hoc analyses.
DISCUSSION
The principal finding of this study is that metabolically unhealthy individuals exhibited significantly higher levels of several adipocytokines compared to metabolically healthy individuals in the nonobese groups (MHNO and MUHNO). Although this result was not observed in the obese groups, the present data indicate that there is an association between metabolic health and serum levels of adipocytokines.
Metabolic health has been highlighted as an important determinant of favorable clinical outcomes in recent literatures [122223]. Previously, our retrospective longitudinal study reported that metabolically unhealthy subjects showed significantly increased risk for diabetes development in a median 48.7 months of follow-up period compared with metabolically healthy subjects, regardless of obesity status assessed by BMI [24]. Moreover, a cross-sectional study conducted by our group that included 24,063 participants in a health screening program found that metabolically unhealthy subjects are more prone to coronary artery calcification (as assessed by coronary artery calcium scores) than metabolic healthy subjects [25].
Numerous studies have demonstrated that MHO individuals display a greater degree of sensitivity and lower fasting glucose and insulin levels compared to MUHO individuals [78262728]. Furthermore, MHO individuals have higher HDL-C levels but lower TG and hepatic enzyme levels compared to MUHO individuals [78132728]. Additional clinical characteristics of MHO individuals include lower free fatty acid concentrations [726], higher circulating levels of natural killer cells and cytotoxic T lymphocytes [29], and significantly lower levels of high-sensitivity C-reactive protein and alpha-1 antitrypsin [8]. Although the present study did not observe any significant differences between the MHO and MUHO groups in terms of adipocytokine levels, it still provides meaningful data. However, the reasons why only nonobese subjects showed significant differences according to metabolic health in terms of adipocytokines in the present study is a matter of debate. This discrepancy may be explained by the use of BMI to assess obesity rather than waist circumference, which specifically evaluates abdominal obesity. Further studies should be conducted using nonobese groups of individuals with an unhealthy metabolic status to clarify this issue.
The measurement of circulating adipocytokines could be useful to evaluate metabolic health. There are many studies that suggested the significant association between adipocytokines and metabolic complications such as DM microangiopathy [30], coronary atherosclerosis [3132], nonalcoholic fatty liver disease [33]. However, only a few studies reported about the relationship between adipocytokines and metabolic health and obesity. One cross-sectional analysis in 716 subjects reported that MHO individuals have adiponectin concentrations similar to those found in normal body weight subjects [12]. In this study, MHO was defined as a BMI above 30 kg/m2 plus HDL-C of at least 40 mg/dL in the absence of T2DM and hypertension. Another cross-sectional study evaluated 60 morbidly obese patients and found that serum concentrations of several adipocytokines were quite different between insulin-sensitive and insulin-resistant obese groups [9]. In contrast to the above studies, the present study defined metabolic health according to the presence or absence of various metabolic health-related components, such as, BP, fasting glucose, TG, HDL-C, and HOMA-IR [1920].
Of the four serum adipocytokines measured, TNF-α and A-FABP showed an association with metabolic health in nonobese individuals. TNF-α was the first proinflammatory cytokine identified in the adipose tissue of obese mice that plays a role as a functional link between inflammation and insulin resistance, marking the start of the metabolic inflammation concept [34]. Mice lacking TNF-α or its receptors maintained insulin sensitivity in both dietary and genetic models of obesity [35]. There is also a strong association between circulating TNF-α and insulin resistance or other metabolic complications in humans [3637]. Although few studies have been performed on TNF-α levels in metabolically unhealthy lean subjects, normal-weight women with polycystic ovarian syndrome, which is known to be caused by insulin resistance, showed significantly increased TNF-α levels compared with control subjects, suggesting increased TNF-α levels in lean, metabolically unhealthy subjects [38]. Also known as FABP4 or aP2, A-FABP is one of nine FABPs with tissue-specific function and patterns of expression [39]. In mouse models, A-FABP deficiency was resulted in reduced adiposity, enhanced insulin sensitivity and reduced hepatosteatosis [40]. Recently, A-FABP is considered as an independent marker of metabolic syndrome and atherosclerosis [414243].
In the present study, IL-6 and MCP-1 did not differ significantly among the groups. IL-6 is one of major proinflammatory cytokine that induces insulin resistance via an interruption of insulin-signaling pathways [44]. However, there is contradictory evidence from recent studies regarding the influence of IL-6 on insulin action and glucose metabolism [4546]. The release of IL-6 from skeletal muscle may have beneficial effects, including increased glucose uptake and fatty acid oxidation [47], and it appears that the activation of AMP-kinase by IL-6 mediates these effects [48]. The fact that IL-6 is produced by several organs might contribute to its complex effects on metabolic regulation. MCP-1 decreases insulin-stimulated glucose uptake in adipocytes [49], and plays a pivotal role in the development of atherosclerosis via the enhancement of adhesion molecules on leukocytes and endothelial cells [50]. However, recent studies investigating the role of MCP-1 on insulin resistance have produced inconsistent results [5152]. These inconsistent results regarding the association of IL-6 and MCP-1 serum levels with metabolic properties might be in line with the present findings.
Our study has several limitations. First, we used a cross-sectional study design and therefore could not establish a cause-and-effect relationship between adipocytokines and metabolic health. Second, as most of the participants were only slightly obese Asians (BMI <30 kg/m2), our data might not be applicable to the global population with higher grades of obesity. Third, among 1,635 subjects in whom serum samples were collected, serum adipocytokine levels were available only in 469 subjects. This might act as a confounding factor or a selection bias. Finally, since there is no unified definition of metabolic health, there might be considerable differences in data according to which definition is applied [53]. Despite limitations of the study, this study has significance in that it was the first study to examine the role of adipocytokines in metabolic health and obesity status.
In conclusion, the present study found that MUHNO subjects showed significantly higher levels of serum TNF-α and A-FABP compared to MHNO subjects. This suggests that adipocytokines may be significant determinants of metabolic health, but further longitudinal studies are needed to assess whether circulating adipocytokines represent a biomarker for metabolic health or whether these factors result in metabolic complications. Furthermore, it is necessary to determine whether the manipulation of adipocytokines could be a future therapy for metabolic abnormalities. If there is a causal relationship between adipocytokines and metabolic health, early lifestyle modifications or pharmacological interventions will likely provide beneficial effects for metabolically high-risk individuals.
Notes
CONFLICTS OF INTEREST: No potential conflict of interest relevant to this article was reported.