Search
- Page Path
- HOME > Search
- Calcium & Bone Metabolism
- Update on Preoperative Parathyroid Localization in Primary Hyperparathyroidism
- Hye-Sun Park, Namki Hong, Jong Ju Jeong, Mijin Yun, Yumie Rhee
- Endocrinol Metab. 2022;37(5):744-755. Published online October 25, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1589
- 4,126 View
- 357 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Parathyroidectomy is the treatment of choice for primary hyperparathyroidism when the clinical criteria are met. Although bilateral neck exploration is traditionally the standard method for surgery, minimally invasive parathyroidectomy (MIP), or focused parathyroidectomy, has been widely accepted with comparable curative outcomes. For successful MIP, accurate preoperative localization of parathyroid lesions is essential. However, no consensus exists on the optimal approach for localization. Currently, ultrasonography and technetium-99m-sestamibi–single photon emission computed tomography/computed tomography are widely accepted in most cases. However, exact localization cannot always be achieved, especially in cases with multiglandular disease, ectopic glands, recurrent disease, and normocalcemic primary hyperparathyroidism. Therefore, new modalities for preoperative localization have been developed and evaluated. Positron emission tomography/computed tomography and parathyroid venous sampling have demonstrated improvements in sensitivity and accuracy. Both anatomical and functional information can be obtained by combining these methods. As each approach has its advantages and disadvantages, the localization study should be deliberately chosen based on each patient’s clinical profile, costs, radiation exposure, and the availability of experienced experts. In this review, we summarize various methods for the localization of hyperfunctioning parathyroid tissues in primary hyperparathyroidism.
-
Citations
Citations to this article as recorded by- Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue
Anne L. Worth, Mesrop Ayrapetyan, Susan J. Maygarden, Zibo Li, Zhanhong Wu, Chris B. Agala, Lawrence T. Kim
Journal of Surgical Research.2024; 293: 618. CrossRef - Use of [18F]fluorocholine PET/CT in the detection of primary hyperparathyroidism in paediatrics: a case report
Helena Martínez Sánchez, Francisca Moreno Macián, Sara León Cariñena, Carmen de Mingo Alemany, Lidia Blasco González, Raquel Sánchez Vañó
Journal of Pediatric Endocrinology and Metabolism.2024;[Epub] CrossRef - A Rare Case of Hyperfunctioning Lipoadenoma Presenting as a Cystic Pararthyroid Lesion
Jinyoung Kim, Ohjoon Kwon, Tae-Jung Kim, So Lyung Jung, Eun Ji Han, Ki-Ho Song
Journal of Bone Metabolism.2023; 30(2): 201. CrossRef - Role of 18F-Fluorocholine Positron Emission Tomography (PET)/Computed Tomography (CT) in Diagnosis of Elusive Parathyroid Adenoma
Janan R Badier, Pokhraj P Suthar, Jagadeesh S Singh, Miral D Jhaveri
Cureus.2023;[Epub] CrossRef - Pitfalls of DualTracer 99m-Technetium (Tc) Pertechnetate and Sestamibi Scintigraphy before Parathyroidectomy: Between Primary-Hyperparathyroidism-Associated Parathyroid Tumour and Ectopic Thyroid Tissue
Mara Carsote, Mihaela Stanciu, Florina Ligia Popa, Oana-Claudia Sima, Eugenia Petrova, Anca-Pati Cucu, Claudiu Nistor
Medicina.2023; 60(1): 15. CrossRef - Diagnostic Performance of Magnetic Resonance Imaging for Parathyroid Localization of Primary Hyperparathyroidism: A Systematic Review
Max H. M. C. Scheepers, Zaid Al-Difaie, Lloyd Brandts, Andrea Peeters, Bjorn Winkens, Mahdi Al-Taher, Sanne M. E. Engelen, Tim Lubbers, Bas Havekes, Nicole D. Bouvy, Alida A. Postma
Diagnostics.2023; 14(1): 25. CrossRef
- Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue

- Calcium & Bone Metabolism
- Computed Tomography-Derived Skeletal Muscle Radiodensity Is an Early, Sensitive Marker of Age-Related Musculoskeletal Changes in Healthy Adults
- Yeon Woo Jung, Namki Hong, Joon Chae Na, Woong Kyu Han, Yumie Rhee
- Endocrinol Metab. 2021;36(6):1201-1210. Published online December 13, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1206
- 3,732 View
- 135 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
A decrease in computed tomography (CT)-derived skeletal muscle radiodensity (SMD) reflects age-related ectopic fat infiltration of muscle, compromising muscle function and metabolism. We investigated the age-related trajectory of SMD and its association with vertebral trabecular bone density in healthy adults.
Methods
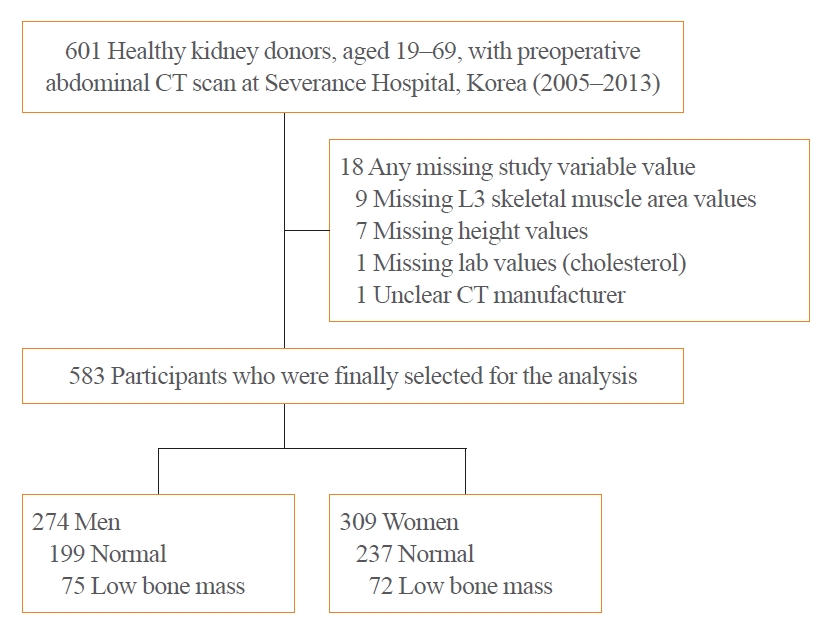
In a cohort of healthy adult kidney donors aged 19 to 69 years (n=583), skeletal muscle index (SMI, skeletal muscle area/height2), SMD, and visceral-to-subcutaneous fat (V/S) ratio were analyzed at the level of L3 from preoperative CT scans. Low bone mass was defined as an L1 trabecular Hounsfield unit (HU) <160 HU.
Results
L3SMD showed constant decline from the second decade (annual change –0.38% and –0.43% in men and women), whereas the decline of L3SMI became evident only after the fourth decade of life (–0.37% and –0.18% in men and women). One HU decline in L3SMD was associated with elevated odds of low bone mass (adjusted odds ratio, 1.07; 95% confidence interval, 1.02 to 1.13; P=0.003), independent of L3SMI, age, sex, and V/S ratio, with better discriminatory ability compared to L3SMI (area under the receiver-operating characteristics curve 0.68 vs. 0.53, P<0.001). L3SMD improved the identification of low bone mass when added to age, sex, V/S ratio, and L3SMI (category-free net reclassification improvement 0.349, P<0.001; integrated discrimination improvement 0.015, P=0.0165).
Conclusion
L3SMD can be an early marker for age-related musculoskeletal changes showing linear decline throughout life from the second decade in healthy adults, with potential diagnostic value for individuals with low bone mass. -
Citations
Citations to this article as recorded by- A review of radiological definitions of sarcopenia in cancer
James W. Wang, Jiarong Chen, Alison H. McGregor, Matthew Williams
JCSM Clinical Reports.2023; 8(2): 36. CrossRef - Weight‐adjusted waist as an integrated index for fat, muscle and bone health in adults
Kyoung Jin Kim, Serhim Son, Kyeong Jin Kim, Sin Gon Kim, Nam Hoon Kim
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(5): 2196. CrossRef
- A review of radiological definitions of sarcopenia in cancer

- Diabetes, Obesity and Metabolism
- Reference Values for Skeletal Muscle Mass at the Third Lumbar Vertebral Level Measured by Computed Tomography in a Healthy Korean Population
- Ja Kyung Yoon, Sunyoung Lee, Kyoung Won Kim, Ji Eun Lee, Jeong Ah Hwang, Taeyong Park, Jeongjin Lee
- Endocrinol Metab. 2021;36(3):672-677. Published online June 8, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1041
- 4,309 View
- 158 Download
- 13 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Sarcopenia is defined as the loss of skeletal muscle mass and is associated with negative clinical outcomes. This study aimed to establish sex-specific cutoff values for the skeletal muscle area (SMA) and skeletal muscle index (SMI) at the third lumbar vertebral (L3) level using computed tomography (CT) imaging to identify sarcopenia in healthy Korean liver donors.
Methods
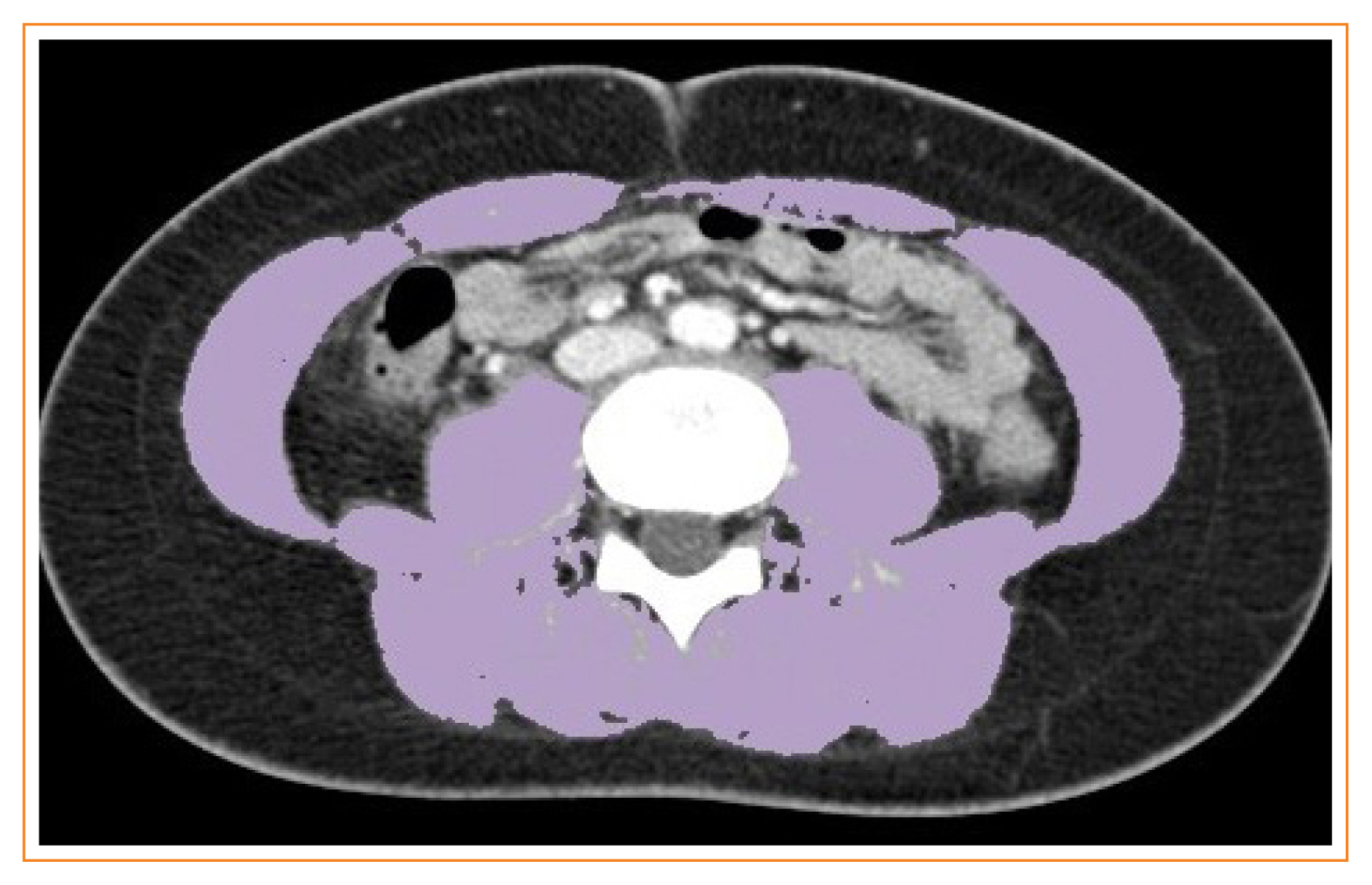
This retrospective study included 659 healthy liver donors (408 men and 251 women) aged 20 to 60 years who had undergone abdominal CT examinations between January 2017 and December 2018. Assessment of body composition was performed with an automated segmentation technique using a deep-learning system. Sex-specific SMA and SMI distributions were assessed, and cutoff values for determining sarcopenia were defined as values at either two standard deviations (SDs) below the mean reference value or below the fifth percentile.
Results
Using the SD definition, cutoff values for SMA and SMI were 117.04 cm2 and 39.33 cm2/m2, respectively, in men and 71.39 cm2 and 27.77 cm2/m2, respectively, in women. Using the fifth percentile definition, cutoff values for SMA and SMI were 126.88 cm2 and 40.96 cm2/m2, respectively, in men and 78.85 cm2 and 30.60 cm2/m2, respectively, in women.
Conclusion
Our data provide sex-specific cutoff values for the SMA and SMI at the L3 level measured by CT imaging in a healthy Korean population, which may be applicable for identifying sarcopenia in this population. -
Citations
Citations to this article as recorded by- Myosteatosis is associated with poor survival after kidney transplantation: a large retrospective cohort validation
Jie Chen, Yue Li, Chengjie Li, Turun Song
Abdominal Radiology.2024; 49(4): 1210. CrossRef - The effect of biological agent on body composition in patients with Crohn’s disease
Eun Jeong Choi, Dong Hoon Baek, Hong Sub Lee, Geun Am Song, Tae Oh Kim, Yong Eun Park, Chang Min Lee, Jong Hoon Lee
BMC Gastroenterology.2023;[Epub] CrossRef - The Association between the L3 Skeletal Muscle Index Derived from Computed Tomography and Clinical Outcomes in Patients with Urinary Tract Infection in the Emergency Department
Jinjoo An, Seung Pill Choi, Jae Hun Oh, Jong Ho Zhu, Sung Wook Kim, Soo Hyun Kim
Journal of Clinical Medicine.2023; 12(15): 5024. CrossRef - Validity of computed tomography defined body composition as a prognostic factor for functional outcome after kidney transplantation
Tim D. A. Swaab, Evelien E. Quint, Lisa B. Westenberg, Marcel Zorgdrager, Dorry L. Segev, Mara A. McAdams‐DeMarco, Stephan J. L. Bakker, Alain R. Viddeleer, Robert A. Pol
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(6): 2532. CrossRef - Assessment of the Diaphragm Thickness Decrease in Critically Ill COVID-19 Patients: Could Computed Tomography Be of Aid Regarding Diaphragm Muscle Mass?
Oana-Elena Branea, Sanda Maria Copotoiu, Diana Andreea Becica, AnaMaria Romina Budeanu, Razvan Gabriel Budeanu, Mihai Emanuel Becica, Dragos Constantin Cucoranu, Septimiu Voidazan, Monica Chis, Alexandra Elena Lazar
Cureus.2023;[Epub] CrossRef - Clinical implication of thoracic skeletal muscle volume as a predictor of ventilation-weaning failure in brain-injured patients: A retrospective observational study
Jimi Oh, Hyun Lim, Chang Won Jeong, Min Su Kim, Jinseok Lee, Wu Seong Kang, Ui Ri An, Joo Un Park, Youngick Ahn, Youe Ree Kim, Chul Park
Medicine.2023; 102(43): e35847. CrossRef - Estimation of Muscle Mass Using Creatinine/Cystatin C Ratio in Japanese Community-Dwelling Older People
Hiroshi Kusunoki, Yasuharu Tabara, Shotaro Tsuji, Yosuke Wada, Kayoko Tamaki, Koutatsu Nagai, Masako Itoh, Kyoko Sano, Manabu Amano, Hatsuo Maeda, Hideyuki Sugita, Yoko Hasegawa, Hiromitsu Kishimoto, Soji Shimomura, Michiya Igase, Ken Shinmura
Journal of the American Medical Directors Association.2022; 23(5): 902.e21. CrossRef - Defining reference values for low skeletal muscle index at the L3 vertebra level based on computed tomography in healthy adults: A multicentre study
Ming Kong, Nan Geng, Ying Zhou, Ning Lin, Wenyan Song, Manman Xu, Shanshan Li, Yuetong Piao, Zuoqing Han, Rong Guo, Chao Yang, Nan Luo, Zhong Wang, Mengyuan Jiang, Lili Wang, Wanchun Qiu, Junfeng Li, Daimeng Shi, Rongkuan Li, Eddie C. Cheung, Yu Chen, Zho
Clinical Nutrition.2022; 41(2): 396. CrossRef - The Value of Artificial Intelligence-Assisted Imaging in Identifying Diagnostic Markers of Sarcopenia in Patients with Cancer
Ying-Tzu Huang, Yi-Shan Tsai, Peng-Chan Lin, Yu-Min Yeh, Ya-Ting Hsu, Pei-Ying Wu, Meng-Ru Shen, Zhongjie Shi
Disease Markers.2022; 2022: 1. CrossRef - Assessment of Muscle Quantity, Quality and Function
Bo Kyung Koo
Journal of Obesity & Metabolic Syndrome.2022; 31(1): 9. CrossRef - Computed Tomography-Derived Skeletal Muscle Radiodensity Is an Early, Sensitive Marker of Age-Related Musculoskeletal Changes in Healthy Adults
Yeon Woo Jung, Namki Hong, Joon Chae Na, Woong Kyu Han, Yumie Rhee
Endocrinology and Metabolism.2021; 36(6): 1201. CrossRef
- Myosteatosis is associated with poor survival after kidney transplantation: a large retrospective cohort validation

- Thyroid
- Percutaneous Adrenal Radiofrequency Ablation: A Short Review for Endocrinologists
- Byung Kwan Park
- Endocrinol Metab. 2020;35(4):750-755. Published online December 2, 2020
- DOI: https://doi.org/10.3803/EnM.2020.880
- 4,522 View
- 125 Download
- 9 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
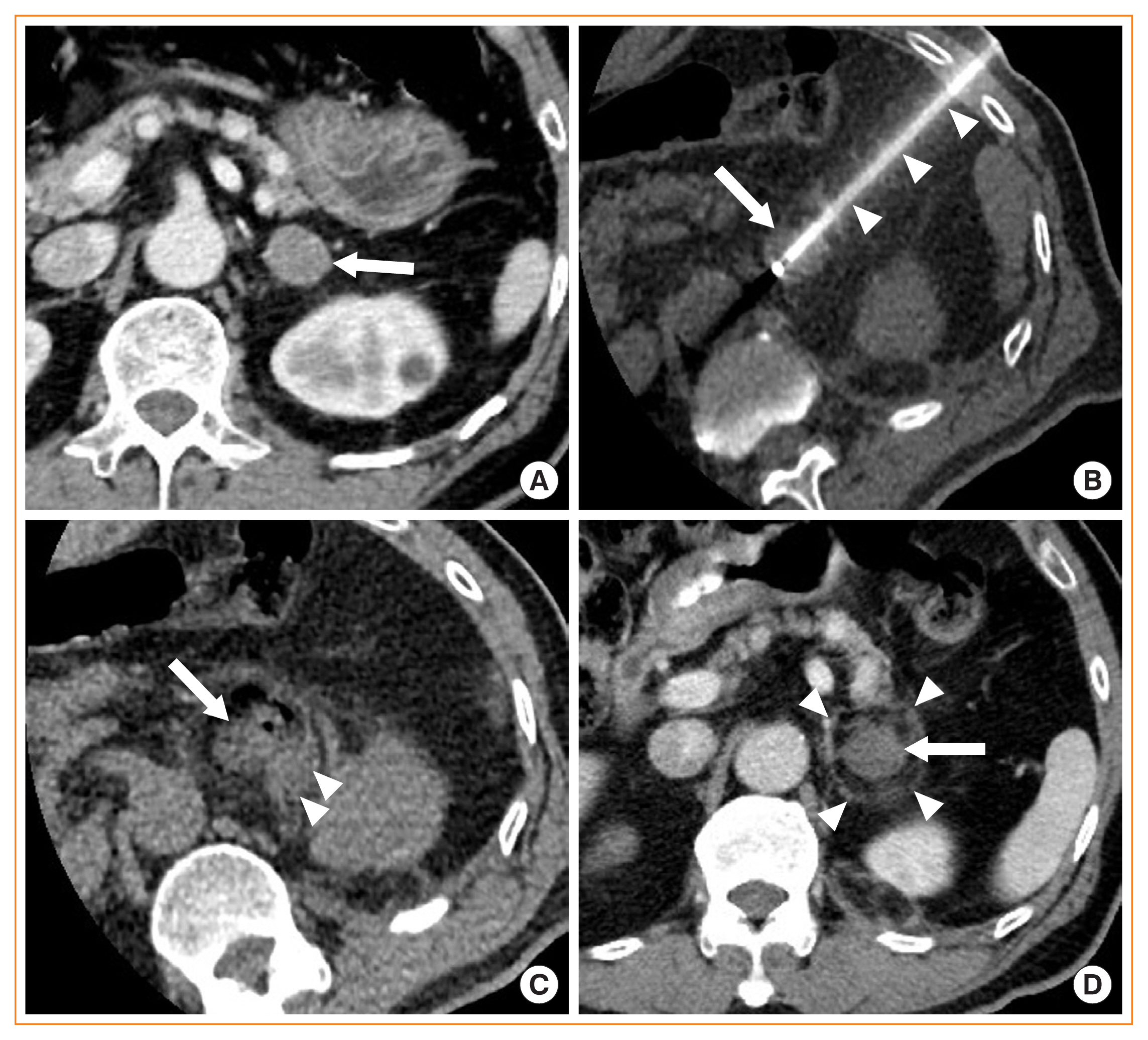
ePub - Image-guided radiofrequency ablation (RFA) has been accepted as a minimally invasive treatment for adrenal tumors in patients who are unable to undergo adrenalectomy. Accordingly, this treatment has become more readily available for treating functioning or non-functioning adrenal masses. Thus, endocrinologists need a better understanding of percutaneous RFA of adrenal tumors. The purpose of this review is to briefly describe the basic mechanism of RFA, indications and contraindications, patient preparation prior to RFA, type of complications, how to avoid complications, RFA procedures, and treatment outcomes.
-
Citations
Citations to this article as recorded by- Clinical Features and Etiology of Recurrent Hypertension after Adrenalectomy
Xilan Dong, Qianhui Ling, Jin Bian, Yuehua Li, Mengjia Chen, Sufang Hao, Wenjun Ma, Huimin Zhang, Jun Cai, Ying Lou
Cardiovascular Innovations and Applications.2024;[Epub] CrossRef - Short-term outcome of adrenal radiofrequency ablation of adrenal cysts: a single-center experience
Shin Jeong Pak, Yu-mi Lee, Pyo Nyun Kim, Byung-Chang Kim, Jae Won Cho, Won Woong Kim, Tae-Yon Sung, Ki-wook Chung, Suck Joon Hong
Scientific Reports.2023;[Epub] CrossRef - Case report of trans-renal ablation procedures for a recurrent pheochromocytoma in von Hippel-Lindau disease
Byung Kwan Park
Precision and Future Medicine.2023; 7(2): 90. CrossRef - Efficacy and safety of radiofrequency ablation in the treatment of inoperable patients with pulmonary malignant nodules
Peng Qie, Xuejiao Xun, Xiaodong Nie, Qifan Yin, Hongshang Cui, Lijun Liu, Huien Wang
ANZ Journal of Surgery.2023; 93(12): 2969. CrossRef - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - Minimally invasive techniques in benign and malignant adrenal tumors
Ahmet Bulent Dogrul, Omer Cennet, Anıl Hilmi Dincer
World Journal of Clinical Cases.2022; 10(35): 12812. CrossRef - Asian Conference on Tumor Ablation Guidelines for Adrenal Tumor Ablation
Byung Kwan Park, Masashi Fujimori, Shu-Huei Shen, Uei Pua
Endocrinology and Metabolism.2021; 36(3): 553. CrossRef - The role and place of mini-invasive methods of local tumor destruction in adrenal gland surgery
I.A. Kurganov, D.Yu. Bogdanov, S.I. Emelyanov, M.Sh. Mamistvalov
Endoskopicheskaya khirurgiya.2021; 27(6): 43. CrossRef
- Clinical Features and Etiology of Recurrent Hypertension after Adrenalectomy

- Adrenal gland
- C-Arm Computed Tomography-Assisted Adrenal Venous Sampling Improved Right Adrenal Vein Cannulation and Sampling Quality in Primary Aldosteronism
- Chung Hyun Park, Namki Hong, Kichang Han, Sang-Wook Kang, Cho Rok Lee, Sungha Park, Yumie Rhee
- Endocrinol Metab. 2018;33(2):236-244. Published online May 4, 2018
- DOI: https://doi.org/10.3803/EnM.2018.33.2.236
- 4,137 View
- 45 Download
- 9 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub Background Adrenal venous sampling (AVS) is a gold standard for subtype classification of primary aldosteronism (PA). However, this procedure has a high failure rate because of the anatomical difficulties in accessing the right adrenal vein. We investigated whether C-arm computed tomography-assisted AVS (C-AVS) could improve the success rate of adrenal sampling.
Methods A total of 156 patients, diagnosed with PA who underwent AVS from May 2004 through April 2017, were included. Based on the medical records, we retrospectively compared the overall, left, and right catheterization success rates of adrenal veins during the periods without C-AVS (2004 to 2010,
n =32) and with C-AVS (2011 to 2016,n =124). The primary outcome was adequate bilateral sampling defined as a selectivity index (SI) >5.Results With C-AVS, the rates of adequate bilateral AVS increased from 40.6% to 88.7% (
P <0.001), with substantial decreases in failure rates (43.7% to 0.8%,P <0.001). There were significant increases in adequate sampling rates from right (43.7% to 91.9%,P <0.001) and left adrenal veins (53.1% to 95.9%,P <0.001) as well as decreases in catheterization failure from right adrenal vein (9.3% to 0.0%,P <0.001). Net improvement of SI on right side remained significant after adjustment for left side (adjusted SI, 1.1 to 9.0;P =0.038). C-AVS was an independent predictor of adequate bilateral sampling in the multivariate model (odds ratio, 9.01;P <0.001).Conclusion C-AVS improved the overall success rate of AVS, possibly as a result of better catheterization of right adrenal vein.
-
Citations
Citations to this article as recorded by- Utility of right adrenal signature veins in venous sampling for primary aldosteronism
Zhenglin Shen, Shaoyong Xu, Siyu Guan, Bo Chen, Qingan Li, Ming Yu, Zhao Gao
Annals of Medicine.2023;[Epub] CrossRef - Key to the Treatment of Primary Aldosteronism in Secondary Hypertension: Subtype Diagnosis
Rui Zuo, Shuang Liu, Lu Xu, Hua Pang
Current Hypertension Reports.2023; 25(12): 471. CrossRef - A clinical assessment of portable point-of-care testing for quick cortisol assay during adrenal vein sampling
Ko Aiga, Mitsuhiro Kometani, Shigehiro Karashima, Seigo Konishi, Takuya Higashitani, Daisuke Aono, Xurong Mai, Mikiya Usukura, Takahiro Asano, Ayako Wakayama, Yuko Noda, Wataru Koda, Tetsuya Minami, Satoshi Kobayashi, Toshinori Murayama, Takashi Yoneda
Scientific Reports.2023;[Epub] CrossRef - Does Intraprocedural CT Improve the Success Rate of Adrenal Venous Sampling? A Systematic Review and Meta-Analysis of Data from 809 Patients
Nima Hafezi-Nejad, David M. Gullotti, Christopher R. Bailey, Mark L. Lessne, Brian P. Holly
CardioVascular and Interventional Radiology.2022; 45(1): 29. CrossRef - Prevalence and clinical characteristics of primary aldosteronism in a tertiary-care center in Korea
Minjae Yoon, Namki Hong, Jaehyung Ha, Chan Joo Lee, Cheol Ryong Ku, Yumie Rhee, Sungha Park
Hypertension Research.2022; 45(9): 1418. CrossRef - Cone-beam computed tomography is not a mandatory procedure in adrenal venous sampling for primary hyperaldosteronism
Ran Cai, Chao Hu, Hai-Yang Li
BMC Medical Imaging.2022;[Epub] CrossRef - Adrenal Venous Sampling for Subtype Diagnosis of Primary Hyperaldosteronism
Mitsuhide Naruse, Akiyo Tanabe, Koichi Yamamoto, Hiromi Rakugi, Mitsuhiro Kometani, Takashi Yoneda, Hiroki Kobayashi, Masanori Abe, Youichi Ohno, Nobuya Inagaki, Shoichiro Izawa, Masakatsu Sone
Endocrinology and Metabolism.2021; 36(5): 965. CrossRef - Controversies and advances in adrenal venous sampling in the diagnostic workup of primary aldosteronism
Martin Wolley, Moe Thuzar, Michael Stowasser
Best Practice & Research Clinical Endocrinology & Metabolism.2020; 34(3): 101400. CrossRef - Update on the Aldosterone Resolution Score and Lateralization in Patients with Primary Aldosteronism
Eun-Hee Cho
Endocrinology and Metabolism.2018; 33(3): 352. CrossRef
- Utility of right adrenal signature veins in venous sampling for primary aldosteronism

- Clinical Study
- A 5-Year Prospective Follow-Up Study of Lipid-Rich Adrenal Incidentalomas: No Tumor Growth or Development of Hormonal Hypersecretion
- Camilla Schalin-Jäntti, Merja Raade, Esa Hämäläinen, Timo Sane
- Endocrinol Metab. 2015;30(4):481-487. Published online December 31, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.4.481
- 3,617 View
- 45 Download
- 22 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Current guidelines for follow-up of adrenal incidentalomas are extensive and hampered by lack of follow-up studies. We tested the hypothesis that small lipid-rich adrenal incidentalomas, initially characterized by tumor size <40 mm and <10 Hounsfield units (HUs) on unenhanced computed tomography (CT) may not demonstrate excessive growth/hormonal hypersecretion on follow-up.
Methods Sixty-nine incidentalomas in 56 patients were restudied with unenhanced CT and screening for hypercortisolism (dexamethasone suppression test [DST], plasma adrenocorticotropic hormone) and pheochromocytoma (24-hour urinary metanephrines and normetanephrines) 5 years later. Primary hyperaldosteronism was excluded at base-line.
Results Tumor (
n =69) size was similar before and after 5 years follow-up (19±6 mm vs. 20±7 mm). Mean tumor growth was 1±2 mm. Largest increase in tumor size was 8 mm, this tumor was surgically removed and histopathology confirmed cortical adenoma. DST was normal in 54 patients and two patients (3.6%) were still characterized by subclinical hypercortisolism. Initial tumor size was >20 mm for the patient with largest tumor growth and those with subclinical hypercortisolism. All patients had normal 24-hour urinary metanephrines and normetanephrines. Low attenuation (<10 HU) was demonstrated in 97% of 67 masses re-evaluated with unenhanced CT.Conclusion None of the patients developed clinically relevant tumor growth or new subclinical hypercortisolism. Biochemical screening for pheochromocytoma in incidentalomas demonstrating <10 HU on unenhanced CT is not needed. For such incidentalomas <40 mm, it seems sufficient to perform control CT and screen for hypercortisolism after 5 years.
-
Citations
Citations to this article as recorded by- European Society of Endocrinology clinical practice guidelines on the management of adrenal incidentalomas, in collaboration with the European Network for the Study of Adrenal Tumors
Martin Fassnacht, Stylianos Tsagarakis, Massimo Terzolo, Antoine Tabarin, Anju Sahdev, John Newell-Price, Iris Pelsma, Ljiljana Marina, Kerstin Lorenz, Irina Bancos, Wiebke Arlt, Olaf M Dekkers
European Journal of Endocrinology.2023; 189(1): G1. CrossRef - Diagnostic Accuracy of CT Texture Analysis in Adrenal Masses: A Systematic Review
Filippo Crimì, Emilio Quaia, Giulio Cabrelle, Chiara Zanon, Alessia Pepe, Daniela Regazzo, Irene Tizianel, Carla Scaroni, Filippo Ceccato
International Journal of Molecular Sciences.2022; 23(2): 637. CrossRef - Susceptibility and characteristics of infections in patients with glucocorticoid excess or insufficiency: the ICARO tool
Marianna Minnetti, Valeria Hasenmajer, Emilia Sbardella, Francesco Angelini, Chiara Simeoli, Nicola Di Paola, Alessia Cozzolino, Claudia Pivonello, Dario De Alcubierre, Sabrina Chiloiro, Roberto Baldelli, Laura De Marinis, Rosario Pivonello, Riccardo Pofi
European Journal of Endocrinology.2022; 187(5): 719. CrossRef - Approach to large adrenal tumors
Urszula Ambroziak
Current Opinion in Endocrinology, Diabetes & Obesity.2021; 28(3): 271. CrossRef - Frequently asked questions and answers (if any) in patients with adrenal incidentaloma
F. Ceccato, M. Barbot, C. Scaroni, M. Boscaro
Journal of Endocrinological Investigation.2021; 44(12): 2749. CrossRef - Draft of the clinical practice guidelines “Adrenal incidentaloma”
D. G. Beltsevich, E. A. Troshina, G. A. Melnichenko, N. M. Platonova, D. O. Ladygina, A. Chevais
Endocrine Surgery.2021; 15(1): 4. CrossRef - Attenuation Value in Adrenal Incidentalomas: A Longitudinal Study
Filippo Ceccato, Irene Tizianel, Giacomo Voltan, Gianmarco Maggetto, Isabella Merante Boschin, Emilio Quaia, Filippo Crimì, Carla Scaroni
Frontiers in Endocrinology.2021;[Epub] CrossRef - Guía práctica sobre la evaluación inicial, seguimiento y tratamiento de los incidentalomas adrenales. Grupo de patología adrenal de la Sociedad Española de Endocrinología y Nutrición
Marta Araujo-Castro, Marta Iturregui Guevara, María Calatayud Gutiérrez, Paola Parra Ramírez, Paola Gracia Gimeno, Felicia Alexandra Hanzu, Cristina Lamas Oliveira
Endocrinología, Diabetes y Nutrición.2020; 67(6): 408. CrossRef - Practical guide on the initial evaluation, follow-up, and treatment of adrenal incidentalomas. Adrenal Diseases Group of the Spanish Society of Endocrinology and Nutrition
Marta Araujo-Castro, Marta Iturregui Guevara, María Calatayud Gutiérrez, Paola Parra Ramírez, Paola Gracia Gimeno, Felicia Alexandra Hanzu, Cristina Lamas Oliveira
Endocrinología, Diabetes y Nutrición (English ed.).2020; 67(6): 408. CrossRef - Endocrine Causes of Hypertension
Taniya de Silva, Gina Cosentino, Suneeta Ganji, Alejandra Riera-Gonzalez, Daniel S. Hsia
Current Hypertension Reports.2020;[Epub] CrossRef - Adrenocortical carcinoma: presentation and outcome of a contemporary patient series
Iiro Kostiainen, Liisa Hakaste, Pekka Kejo, Helka Parviainen, Tiina Laine, Eliisa Löyttyniemi, Mirkka Pennanen, Johanna Arola, Caj Haglund, Ilkka Heiskanen, Camilla Schalin-Jäntti
Endocrine.2019; 65(1): 166. CrossRef - CT Characteristics of Pheochromocytoma: Relevance for the Evaluation of Adrenal Incidentaloma
Letizia Canu, Janna A W Van Hemert, Michiel N Kerstens, Robert P Hartman, Aakanksha Khanna, Ivana Kraljevic, Darko Kastelan, Corin Badiu, Urszula Ambroziak, Antoine Tabarin, Magalie Haissaguerre, Edward Buitenwerf, Anneke Visser, Massimo Mannelli, Wiebke
The Journal of Clinical Endocrinology & Metabolism.2019; 104(2): 312. CrossRef - The Evaluation of Incidentally Discovered Adrenal Masses
Anand Vaidya, Amir Hamrahian, Irina Bancos, Maria Fleseriu, Hans K. Ghayee
Endocrine Practice.2019; 25(2): 178. CrossRef - Evaluation of quantitative parameters for distinguishing pheochromocytoma from other adrenal tumors
Youichi Ohno, Masakatsu Sone, Daisuke Taura, Toshinari Yamasaki, Katsutoshi Kojima, Kyoko Honda-Kohmo, Yorihide Fukuda, Koji Matsuo, Toshihito Fujii, Akihiro Yasoda, Osamu Ogawa, Nobuya Inagaki
Hypertension Research.2018; 41(3): 165. CrossRef - Long term follow-up of non functional adrenal incidentalomas in size: a single center experience
Güven Barış Cansu, Bengür Taşkıran, Eylem Bahadır
Ortadoğu Tıp Dergisi.2018; 10(4): 506. CrossRef - Unenhanced CT imaging is highly sensitive to exclude pheochromocytoma: a multicenter study
Edward Buitenwerf, Tijmen Korteweg, Anneke Visser, Charlotte M S C Haag, Richard A Feelders, Henri J L M Timmers, Letizia Canu, Harm R Haak, Peter H L T Bisschop, Elisabeth M W Eekhoff, Eleonora P M Corssmit, Nanda C Krak, Elise Rasenberg, Janneke van den
European Journal of Endocrinology.2018; 178(5): 431. CrossRef - The impact of an adrenal incidentaloma algorithm on the evaluation of adrenal nodules
Leslie S. Eldeiry, Marina M. Alfisher, Catherine F. Callahan, Nancy N. Hanna, Jeffrey R. Garber
Journal of Clinical & Translational Endocrinology.2018; 13: 39. CrossRef - Adrenal incidentaloma: differential diagnosis and management strategies
Valentina Morelli, Serena Palmieri
Minerva Endocrinologica.2018;[Epub] CrossRef - Adrenal Imaging
Mishal Mendiratta-Lala, Anca Avram, Adina F. Turcu, N. Reed Dunnick
Endocrinology and Metabolism Clinics of North America.2017; 46(3): 741. CrossRef - Update on the risks of benign adrenocortical incidentalomas
Guido Di Dalmazi
Current Opinion in Endocrinology, Diabetes & Obesity.2017; 24(3): 193. CrossRef - Management Scheme for Adrenal Incidentalomas: Who Gets What?
Glenda G. Callender, Robert Udelsman
Current Surgery Reports.2016;[Epub] CrossRef - Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors
Martin Fassnacht, Wiebke Arlt, Irina Bancos, Henning Dralle, John Newell-Price, Anju Sahdev, Antoine Tabarin, Massimo Terzolo, Stylianos Tsagarakis, Olaf M Dekkers
European Journal of Endocrinology.2016; 175(2): G1. CrossRef
- European Society of Endocrinology clinical practice guidelines on the management of adrenal incidentalomas, in collaboration with the European Network for the Study of Adrenal Tumors

- Adrenal gland
- Differential Diagnosis of Adrenal Mass Using Imaging Modality: Special Emphasis on F-18 Fluoro-2-Deoxy-D-Glucose Positron Emission Tomography/Computed Tomography
- Hong Je Lee, Jaetae Lee
- Endocrinol Metab. 2014;29(1):5-11. Published online March 14, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.1.5
- 4,098 View
- 30 Download
- 7 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Adrenal incidentalomas are adrenal masses serendipitously detected during an imaging study performed for reasons unrelated to suspicion of adrenal disease. The incidence of adrenal incidentalomas has increased because of the widespread use of various imaging modalities. In oncology patients with adrenal incidentalomas, the characterization of the adrenal masses is challenging because nearly 50% of incidental adrenal masses are metastatic lesions that need special medical attention. Although unenhanced computed tomography (CT) densitometry, chemical shift magnetic resonance imaging (MRI), delayed contrast-enhanced CT and CT histogram analysis have been used as sensitive and specific modalities for differentiating benign from malignant adrenal masses, F-18 fluoro-2-deoxy-D-glucose positron emission tomography (F-18 FDG PET)/CT is a highly accurate imaging modality compared to CT or MRI, especially when these two imaging modalities are combined. In addition, a semiquantitative analysis using standardized uptake value ratio further improves the diagnostic accuracy of F-18 FDG PET/CT in differentiating benign from malignant adrenal masses. Thus, F-18 FDG PET/CT is very helpful for determining the best therapeutic management, especially for assessing the need for surgery.
-
Citations
Citations to this article as recorded by- The F-18 FDG PET/CT evaluation of the metastatic adrenal lesions of the non-lung cancer tumors compared with pathology results
Zehra Pınar Koç, Pınar Pelin Özcan, Emel Sezer, Kadir Eser, Tuba Kara
Egyptian Journal of Radiology and Nuclear Medicine.2022;[Epub] CrossRef - Dual time point [18F]Flurodeoxyglucose (FDG) Positron Emission Tomography (PET)/Computed Tomography (CT) with water gastric distension in differentiation between malignant and benign gastric lesions
Hussein Farghaly, Mohamed Alshareef, Abdullah Alqarni, Mohamed Sayed, Hatem Nasr
European Journal of Radiology Open.2020; 7: 100268. CrossRef - 18F-FDG PET/CT Imaging of Adrenal Liposarcoma
Rang Wang, Qiuping Fan, Rong Tian
Clinical Nuclear Medicine.2020; 45(7): 570. CrossRef - Characterization of adrenocortical tumors by 18F-FDG PET/CT: Does steroid hormone hypersecretion status modify the uptake pattern?
Nunzia Cinzia Paladino, Carole Guérin, Aoïfe Lowery, Andrea Attard, Wassim Essamet, Eveline Slotema, Isabelle Morange, Frédéric Castinetti, Thierry Brue, Anderson Loundou, David Taïeb, Frédéric Sebag
Surgical Oncology.2018; 27(2): 231. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Adrenal masses in oncology patients
Rodney H Reznek
Cancer Imaging.2014;[Epub] CrossRef
- The F-18 FDG PET/CT evaluation of the metastatic adrenal lesions of the non-lung cancer tumors compared with pathology results

- Effect of Sequential Therapy with Incadronate after Withdrawal of Recombinant Human Parathyroid Hormone(1-84) on Bone Quantity and Quality in Ovariectomized Rats.
- Yumie Rhee, Jong Chan Youn, Ye Yeon Won, Myong Hyun Baek, Sung Kil Lim
- J Korean Endocr Soc. 2005;20(4):334-343. Published online August 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.4.334
- 1,338 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Human parathyroid hormone(hPTH) is a promising anabolic agent. However, since hPTH (1-34) is available only via injection, and has a critical side effect of causing bone tumors during life-long administration in the rat, it would be practical to use PTH for the shortest possible duration to obtain the maximal effect. In addition, acquired bone mass due to hPTH tend to decrease after drug cessation. To determine the effectiveness of the osteoporosis-reversing concept of lose, restore, and maintain(LRM), recombinant human PTH(1-84)[rhPTH(1-84)] and the respective anti-resorptive agents were sequentially studied. METHODS: Thirty six, 20-week-old, Sprague-Dawley rats were used in this study. Treatment was started on the 25th week after an ovariectomy, which had been performed at 20weeks of age, with 5weeks of rhPTH (1-84) 100(microgram/kg/d), 5days/wk, followed by the respective sequential therapies for 5 weeks as follows: 1) Ovariectomized rats(OVX, n=6), 2) Sham operated rats(SHAM, n=6), 3) OVX rats with PTH maintenance(PTH-M, n=6), 4) OVX rats treated with PTH then withdrawn(PTH-W, n=6), 5) PTH-treated OVX rats then treated with 17beta-estradiol(PTH-E, 10microgram/d, SQ, 5days/wk, n=6), 6) PTH-treated OVX rats then treated with incadronate(PTH-I, 3mg/kg, per os 5 days/wk, n=6). The bone mineral density(BMD) of the right femurs was measured using dual X-ray absorptiometry(DXA). Microcomputed tomography(microCT) was used to measure the structural parameters of the 2nd lumbar vertebrae. A three-point bending test of the femur and compressive tests of vertebrae were also performed. RESULTS: Bone quantity data showed that the femoral BMD was significantly higher in the PTH-M and PTH-I groups than in the OVX and PTH-W groups(P<0.05). Measurement of the cortical thickness revealed that only the PTH-M group had a significant increase(P=0.001). The ultimate force(Fu) at the midshaft of the femur was stronger in the PTH-M group than in the OVX group(P<0.001). However, no significant difference was found among the treated groups. CONCLUSION: PTH withdrawal resulted in the loss of the acquired BMD, but sequential therapy with the anti-resorptive, incadronate, prevented further bone loss. The use of incadronate after rhPTH(1-84), as a sequential regimen, was significantly effective on the maintenance in the bone mass, but further clarification in the improvement in the bone quality is needed.


 KES
KES

 First
First Prev
Prev



