Search
- Page Path
- HOME > Search
Special Article
- Miscellaneous
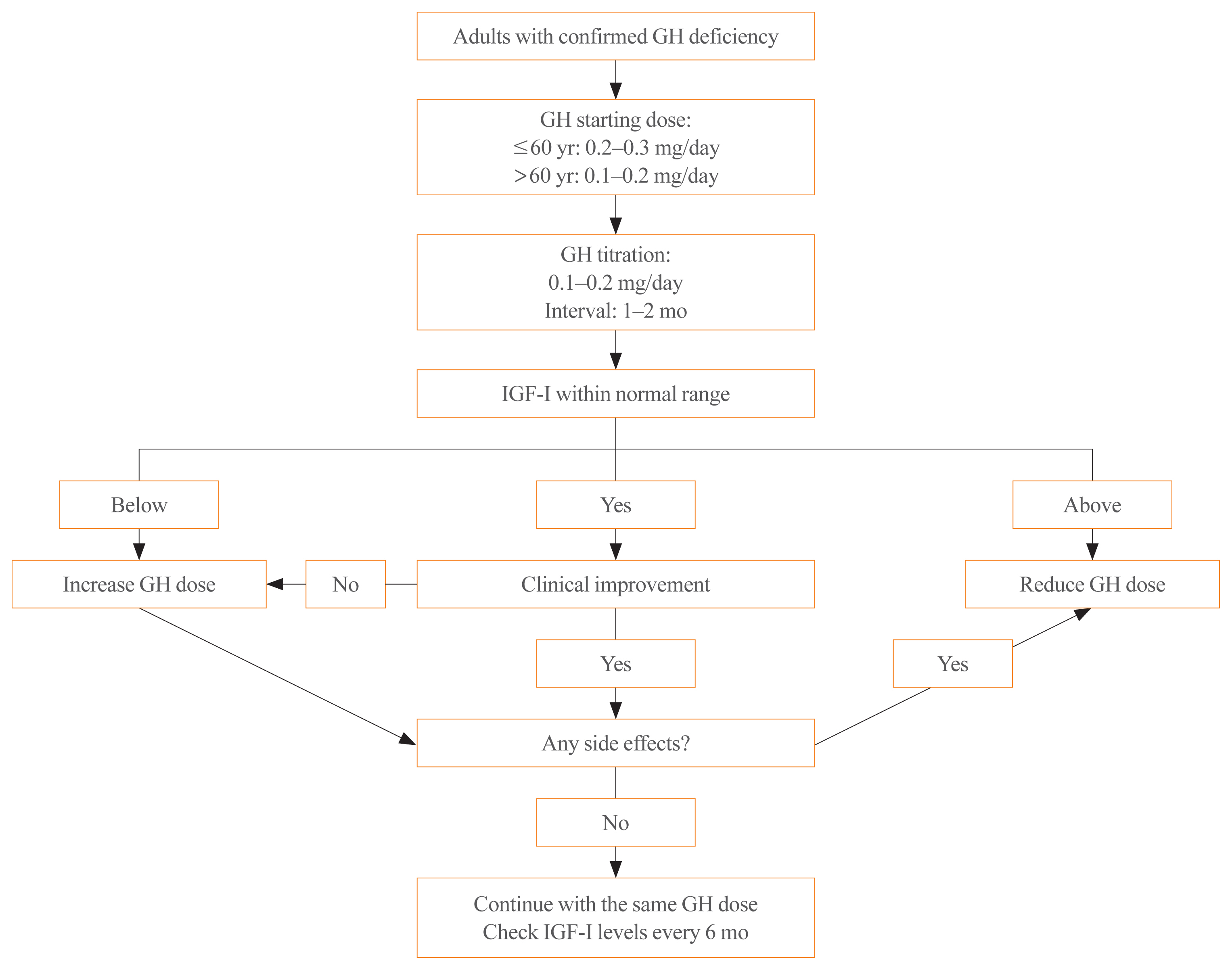
- Diagnosis and Treatment of Growth Hormone Deficiency: A Position Statement from Korean Endocrine Society and Korean Society of Pediatric Endocrinology
- Jung Hee Kim, Hyun Wook Chae, Sang Ouk Chin, Cheol Ryong Ku, Kyeong Hye Park, Dong Jun Lim, Kwang Joon Kim, Jung Soo Lim, Gyuri Kim, Yun Mi Choi, Seong Hee Ahn, Min Ji Jeon, Yul Hwangbo, Ju Hee Lee, Bu Kyung Kim, Yong Jun Choi, Kyung Ae Lee, Seong-Su Moon, Hwa Young Ahn, Hoon Sung Choi, Sang Mo Hong, Dong Yeob Shin, Ji A Seo, Se Hwa Kim, Seungjoon Oh, Sung Hoon Yu, Byung Joon Kim, Choong Ho Shin, Sung-Woon Kim, Chong Hwa Kim, Eun Jig Lee
- Endocrinol Metab. 2020;35(2):272-287. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.272
- 9,498 View
- 429 Download
- 14 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Growth hormone (GH) deficiency is caused by congenital or acquired causes and occurs in childhood or adulthood. GH replacement therapy brings benefits to body composition, exercise capacity, skeletal health, cardiovascular outcomes, and quality of life. Before initiating GH replacement, GH deficiency should be confirmed through proper stimulation tests, and in cases with proven genetic causes or structural lesions, repeated GH stimulation testing is not necessary. The dosing regimen of GH replacement therapy should be individualized, with the goal of minimizing side effects and maximizing clinical improvements. The Korean Endocrine Society and the Korean Society of Pediatric Endocrinology have developed a position statement on the diagnosis and treatment of GH deficiency. This position statement is based on a systematic review of evidence and expert opinions.
-
Citations
Citations to this article as recorded by- Once-Weekly Somapacitan as an Alternative Management of Growth Hormone Deficiency in Prepubertal Children: A Systematic Review and Meta-Analysis of Randomized Controlled Trial
Ghina Tsurayya, Cut Alifiya Nazhifah, Muhammad Rahmat Pirwanja, Putri Oktaviani Zulfa, Muhammad Raihan Ramadhan Tatroman, Fajar Fakri, Muhammad Iqhrammullah
Children.2024; 11(2): 227. CrossRef - Efficacy, safety, and patient satisfaction of norditropin and sogroya in patients with growth hormone deficiency: a systematic review and meta-analysis of randomized controlled trials
Obieda Altobaishat, Mohamed Abouzid, Mostafa Hossam El Din Moawad, Abdulrahman Sharaf, Yazan Al-Ajlouni, Tungki Pratama Umar, Abdallah Bani-salameh, Mohammad Tanashat, Omar Abdullah Bataineh, Abdulqadir J. Nashwan
Endocrine.2024;[Epub] CrossRef - Evaluation of Adult Height in Patients with Non-Permanent Idiopathic GH Deficiency
Agnese Murianni, Anna Lussu, Chiara Guzzetti, Anastasia Ibba, Letizia Casula, Mariacarolina Salerno, Marco Cappa, Sandro Loche
Endocrines.2023; 4(1): 169. CrossRef - The effect of hypothalamic involvement and growth hormone treatment on cardiovascular risk factors during the transition period in patients with childhood-onset craniopharyngioma
Sang Hee Park, Yun Jeong Lee, Jung-Eun Cheon, Choong Ho Shin, Hae Woon Jung, Young Ah Lee
Annals of Pediatric Endocrinology & Metabolism.2023; 28(2): 107. CrossRef - Continuous Glucose Monitoring: A Possible Aid for Detecting Hypoglycemic Events during Insulin Tolerance Tests
Soo Yeun Sim, Moon Bae Ahn
Sensors.2023; 23(15): 6892. CrossRef - The risk patients with AGHD have of developing CVD
Eisha Javed, Maha Zehra, Naz Elahi
International Journal of Cardiology Cardiovascular Risk and Prevention.2023; 19: 200221. CrossRef - Diagnosis of GH Deficiency Without GH Stimulation Tests
Anastasia Ibba, Sandro Loche
Frontiers in Endocrinology.2022;[Epub] CrossRef - Metabolic Impacts of Discontinuation and Resumption of Recombinant Human Growth Hormone Treatment during the Transition Period in Patients with Childhood-Onset Growth Hormone Deficiency
Yun Jeong Lee, Yunha Choi, Han-Wook Yoo, Young Ah Lee, Choong Ho Shin, Han Saem Choi, Ho-Seong Kim, Jae Hyun Kim, Jung Eun Moon, Cheol Woo Ko, Moon Bae Ahn, Byung-Kyu Suh, Jin-Ho Choi
Endocrinology and Metabolism.2022; 37(2): 359. CrossRef - A Radiomics-Based Model with the Potential to Differentiate Growth Hormone Deficiency and Idiopathic Short Stature on Sella MRI
Taeyoun Lee, Kyungchul Song, Beomseok Sohn, Jihwan Eom, Sung Soo Ahn, Ho-Seong Kim, Seung-Koo Lee
Yonsei Medical Journal.2022; 63(9): 856. CrossRef - Phenotypic spectrum of patients with mutations in CHD7: clinical implications of endocrinological findings
Ja Hye Kim, Yunha Choi, Soojin Hwang, Gu-Hwan Kim, Han-Wook Yoo, Jin-Ho Choi
Endocrine Connections.2022;[Epub] CrossRef - Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim
Endocrinology and Metabolism.2022; 37(6): 839. CrossRef - Laron syndrome: clinic, diagnostics (а clinical case)
P.M. Lіashuk, R.P. Lіashuk, N.I. Stankova, M.B. Kudina
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2022; 18(3): 193. CrossRef - Diagnosis for Pheochromocytoma and Paraganglioma: A Joint Position Statement of the Korean Pheochromocytoma and Paraganglioma Task Force
Eu Jeong Ku, Kyoung Jin Kim, Jung Hee Kim, Mi Kyung Kim, Chang Ho Ahn, Kyung Ae Lee, Seung Hun Lee, You-Bin Lee, Kyeong Hye Park, Yun Mi Choi, Namki Hong, A Ram Hong, Sang-Wook Kang, Byung Kwan Park, Moon-Woo Seong, Myungshin Kim, Kyeong Cheon Jung, Chan
Endocrinology and Metabolism.2021; 36(2): 322. CrossRef - Asian Conference on Tumor Ablation Guidelines for Adrenal Tumor Ablation
Byung Kwan Park, Masashi Fujimori, Shu-Huei Shen, Uei Pua
Endocrinology and Metabolism.2021; 36(3): 553. CrossRef - Asian Conference on Tumor Ablation guidelines for renal cell carcinoma
Byung Kwan Park, Shu-Huei Shen, Masashi Fujimori, Yi Wang
Investigative and Clinical Urology.2021; 62(4): 378. CrossRef - Diagnosis and Treatment of Adult Growth Hormone Deficiency
Jung Hee Kim
The Korean Journal of Medicine.2021; 96(5): 400. CrossRef
- Once-Weekly Somapacitan as an Alternative Management of Growth Hormone Deficiency in Prepubertal Children: A Systematic Review and Meta-Analysis of Randomized Controlled Trial

Original Article
- The Effect of Hormone Replacement Therapy on Carotid Intima-Media Thickness in Healthy Postmenopausal Women.
- Jang Yel Shin, Bong Soo Cha, Choon Hee Chung, Won Heum Shim, Hyun Chul Lee
- J Korean Endocr Soc. 2006;21(1):14-21. Published online February 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.1.14
- 1,694 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Cardiovascular disease is the leading cause of death in postmenopausal women. The use of hormone replacement therapy (HRT) preventing for cardiovascular disease in postmenopausal women remains controversial. We investigated the effect of HRT on carotid intima-media thickness (IMT) according to the HRT duration in healthy postmenopausal women. METHODS: One hundred and twenty postmenopausal women (mean age: 55.4 +/- 3.3 years) were classified into never users, short-term, and long-term users according to the HRT duration. Carotid IMT was measured, and the clinical and biochemical cardiovascular risk factors were examined. RESULTS: The mean IMT was significantly thinner in the long-term users than that in the never users (0.62 +/- 0.11 vs. 0.71 +/- 0.14 mm, P < 0.01). Also, the maximal IMT was significantly thinner in the short-term and the long-term users. However, there is no significant difference in the mean and maximal IMTs between the estrogen alone and estrogen plus progestins used group. The period exposed to menopause was significantly shorter in the long-term users than that in the never users (1.8 +/- 2.3 vs. 4.3 +/- 3.3 years, P < 0.001). CONCLUSION: Our findings suggest that if HRT is initiated during early postmenopausal period before the onset of atherosclerosis, HRT may have a beneficial effect on the prevention of carotid atherosclerosis.

Case Report
- A Case of Pancytopenia Caused by Sheehan's Syndorme Improved with Hormone Replacement Therapy.
- Sung Ki Kim, Yoon Ju Oh, Park Young Joo, Young Whan Kim, Seong Bin Hong, Mi Rim Kim, Moon Suk Nam, Yong Seong Kim
- J Korean Endocr Soc. 2000;15(4-5):595-599. Published online January 1, 2001
- 955 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - Postpartum ischemic necrosis of the pituitary gland, known as Sheehan's syndrome, is well- established clinical entity. In anterior pituitary insufficiency, there is very often a normochromic or hypochromic anemia but pancytopenia secondary to the hypopituitarism is less common. We report a case of pancytopenia due to complete aplasia of the bone marrow associated with Sheehan's syndrome, in which hormone replacement therapy alone produced full hematological recovery.

Original Articles
- Changes of Biochemical Bone Markers and Bone Mineral Density after Hormone Replacement Therapy in Korean Women.
- Kyong Soo Park, Do Joon Park, Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee, Jae Hyeon Kim, Jeong Goo Kim
- J Korean Endocr Soc. 2000;15(2):226-236. Published online January 1, 2001
- 930 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Biochemical bone markers have been suggested to reflect postmenopausal high bone turnover. These markers could be useful in following response to hormone replacement therapy (HRT). But we have few studies about the sequential changes of biochemical bone markers and bone mass after HRT in Korean women, and it is unclear whether women with early menopause have different response to HRT from women with normal menopause. The aims of the present study were to see the sequential changes of biochemical bone markers and bone mass after HRT in Korean women, to examine whether a single baseline biochemical bone marker or a change in biochemical bone marker could predict subsequent bone mass, and to determine the difference of response to HRT between women with early menopause and women with normal menopause. METHODS: Postmenopausal women (n=21) were divided with into three groups according to their age at menopause (AAM): the first group with AAM < or = 43 years (early menopause group, n=7), the second group with 43 years < or = AAM < or = 50 years (n=4), and the third group with AAM > or = 50 years (normal menopause group, n=10). For the HRT, conjugated estrogen (0.625mg per day) and continuous or cyclic medroxyprogesterone (2.5-10mg per day) were administered. Bone mineral density (BMD) was measured at baseline and 12 months and biochemical bone markers were measured at baseline and 3, 6, and 12 months during HRT. RESULTS: Deoxypyridinoline, type 1 collagen N-telopeptide, bone alkaline phosphatase, and osteocalcin were significantly decreased at 3 months, and mean percent changes from baseline of bone resorption markers were larger than those of bone formation markers. At 12 months, BMD was significantly increased at lumbar spine and Ward's triangle. But BMD was not significantly increased at femur neck and femur trochanter. Two baseline bone markers (bone alkaline phosphatase and type 1 collagen N-telopeptide) correlated with changes of BMD but any changes of bone markers at 3, 6 months didn't correlate with changes of BMD. In early menopause group, changes of bone markers and BMD were larger than those in normal menopause group, but the difference between the two groups was not significant. CONCLUSION: All four bone markers showed significant reduction at 3 months, but bone resorption markers were decreased more markedly and rapidly, and some baseline bone markers can predict the change of BMD after HRT. The difference of response to HRT between early menopause group and normal menopause group was not significant.

- Association of Estrogen Receptor Genotypes with Serum Lipids and Responsiveness of Serum Lipids to Hormonal Replacement Therapy in Korean Postmenopausal Women.
- So Ra Park, Jae Eun Park, Chung Kyu Hwang, Phil Ho Jung, Chang Hoon Yim, Ho Yeon Chung, Ki Ok Han, Hyun Ku Yoon, Hak Chul Jang, In Kwon Han
- J Korean Endocr Soc. 1999;14(3):553-561. Published online January 1, 2001
- 1,055 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Several biologically plausible mechanisms have been proposed for estrogen-mediated caridoprotection, including estrogen-assocaited changes in lipid metabolism and endothelial function of vessel walls. These effects are thought to be mediated via estrogen receptor (ER). Relationships between ER polymorphisms and serum lipid levels were not investigated enoughly. METHODS: Three restriction fragment length polymorphisms (RFLPs) at the ER gene locus, represented as B-variant, PvuII and XbaI, and their relationship to serum lipid levels were examined in 318 postmenopausal women. Their mean age was 54.5+/-6.5 years (mean+SD). An association between ER genotypes and changes in lipid levels after 1 year of estrogen replacement therapy was also investigated in follow-up 251 women. RESULTS: The B-variant was not found in Korean women. The distribution of the PvuII and XbaI polymorphisms was as follows: PP 109 (34%), Pp 166 (52%), pp 43 (14%), and XX 204 (64%), Xx 95 (30%), xx 19 (6%). Significant relationship was found between genotypes and changes in serum total cholesterol levels after lyr estrogen replacement therapy. There was no significant relationship between ER genotypes and changes in HDL cholesterol, LDL cholesterol and triglyceride levels after estrogen therapy. CONCLUSION: These data indicate that these polymorphisms are possible predictor on lipid response to estrogen replacement therapy.


 KES
KES

 First
First Prev
Prev



