Previous issues
- Page Path
- HOME > BROWSE ARTICLES > Previous issues
In Memoriam
- Miscellaneous
- In Memoriam: Remembering Professor Hun-Ki Min (1928–2021)
- Young Min Cho
- Endocrinol Metab. 2021;36(2):207-208. Published online April 20, 2021
- DOI: https://doi.org/10.3803/EnM.2021.204
- 3,000 View
- 153 Download

Review Articles
- Obesity and Metabolism
- Food Preferences and Obesity
- Sara Spinelli, Erminio Monteleone
- Endocrinol Metab. 2021;36(2):209-219. Published online April 19, 2021
- DOI: https://doi.org/10.3803/EnM.2021.105
- 6,163 View
- 281 Download
- 20 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Obesity is a multifactorial disease with several potential causes that remain incompletely understood. Recent changes in the environment, which has become increasingly obesogenic, have been found to interact with individual factors. Evidence of the role of taste responsiveness and food preference in obesity has been reported, pointing to a lower taste sensitivity and a higher preference and intake of fat and, to a lesser extent, sweet foods in obese people. Studies in the last decades have also suggested that individual differences in the neurophysiology of food reward may lead to overeating, contributing to obesity. However, further studies are needed to confirm these findings. In fact, only a limited number of studies has been conducted on large samples, and several studies were conducted only on women. Larger balanced studies in terms of sex/gender and age are required in order to control the confounding effect of these variables. As many factors are intertwined in obesity, a multidisciplinary approach is needed. This will allow a better understanding of taste alteration and food behaviours in obese people in order to design more effective strategies to promote healthier eating and to prevent obesity and the related chronic disease risks.
-
Citations
Citations to this article as recorded by- Phytochemical composition, toxicological profiling and effect on pup birth weight of Corchorus olitorius leaf extract in rats: Implications for fetal macrosomia control
Onyinye Mkpola Ukpai, Solomon Nnah Ijioma, Kingsley Kanu, Daniel Orieke, Peace Amarachi Chinedu-Ndukwe, Kingsley Chijioke Ugwuanyi, Eziuche Amadike Ugbogu
Journal of Ethnopharmacology.2024; 319: 117170. CrossRef - Sex Differences in Effects of Mood, Eating-Related Behaviors, and BMI on Food Appeal and Desire to Eat: A Cross-Sectional Survey Study
Kristina T. Legget, Marc-Andre Cornier, Lauren Sarabia, Eve M. Delao, Susan K. Mikulich-Gilbertson, Crystal Natvig, Christina Erpelding, Tessa Mitchell, Allison Hild, Eugene Kronberg, Jason R. Tregellas
Nutrients.2023; 15(3): 762. CrossRef - Estimation of Free Sugars in the Filipino Food Composition Table and Evaluation of Population-Level Intake
Fabio Mainardi, Vanessa Caroline Campos, Richard Gaston Côté, Nele Kristin Silber, Roko Plestina, Imelda Angeles-Agdeppa
Nutrients.2023; 15(6): 1343. CrossRef - Genetic Obesity in Pregnant Ay Mice Does Not Affect Susceptibility to Obesity and Food Choice in Offspring
Elena Makarova, Anastasia Dubinina, Elena Denisova, Antonina Kazantseva
International Journal of Molecular Sciences.2023; 24(6): 5610. CrossRef - How Food Choices Impact College Going Students' Health in Urban Settings
Nikita Yadav, Ms. Rhitika Sharma, Ms. Divyanshi Kapoor, Dr. Payal Mahajan
International Journal of Scientific Research in Science and Technology.2023; : 774. CrossRef - Mediators of the association between maternal body mass index and breastfeeding duration in 3 international cohorts
Madeline Keyes, Chloe Andrews, Vishal Midya, Paula Carrasco, Mònica Guxens, Alba Jimeno-Romero, Mario Murcia, Cristina Rodriguez-Dehli, Dora Romaguera, Loreto Santa-Maria, Marina Vafeiadi, Lida Chatzi, Emily Oken, Martine Vrijheid, Damaskini Valvi, Sarbat
The American Journal of Clinical Nutrition.2023; 118(1): 255. CrossRef - Analysis of Determinants of Food Preferences in a Polish Population-Based Sample of Primary School Adolescents: Diet and Activity of Youth during COVID-19 (DAY-19) Study
Aleksandra Kołota, Dominika Głąbska
Nutrients.2023; 15(11): 2504. CrossRef - Is obesity associated with taste alterations? a systematic review
Beatriz Rodrigues Risuenho Peinado, Deborah Ribeiro Frazão, Leonardo Oliveira Bittencourt, Renata Duarte de Souza-Rodrigues, Maria Tereza Campos Vidigal, Douglas Teixeira da Silva, Luiz Renato Paranhos, Marcela Baraúna Magno, Nathalia Carolina Fernandes F
Frontiers in Endocrinology.2023;[Epub] CrossRef - The Relationship between Dietary Intake and Adiposity in South African Female Adolescents: A Systematic Review
Nokuthula Vilakazi, Sithabile Mathunjwa, Heather Legodi, Pedro Terrence Pisa
Applied Sciences.2023; 13(19): 10813. CrossRef - Fat mass and obesity-associated gene (FTO) rs9939609 (A/T) polymorphism and food preference in obese people with low-calorie intake and non-obese individuals with high-calorie intake
Mehran Rahimlou, Bijan Ghobadian, Ali Ramezani, Ehsan Hejazi, Saeideh Mazloomzadeh, Jalal Hejazi
BMC Nutrition.2023;[Epub] CrossRef - The Role of the Olfactory System in Obesity and Metabolism in Humans: A Systematic Review and Meta-Analysis
Lolita Matiashova, Anouk Lisa Hoogkamer, Katharina Timper
Metabolites.2023; 14(1): 16. CrossRef - Taste of Fat and Obesity: Different Hypotheses and Our Point of View
Laurent Brondel, Didier Quilliot, Thomas Mouillot, Naim Akhtar Khan, Philip Bastable, Vincent Boggio, Corinne Leloup, Luc Pénicaud
Nutrients.2022; 14(3): 555. CrossRef - Long-Term Consumption of a Sugar-Sweetened Soft Drink in Combination with a Western-Type Diet Is Associated with Morphological and Molecular Changes of Taste Markers Independent of Body Weight Development in Mice
Barbara Lieder, Jozef Čonka, Agnes T. Reiner, Victoria Zabel, Dominik Ameur, Mark M. Somoza, Katarína Šebeková, Peter Celec, Veronika Somoza
Nutrients.2022; 14(3): 594. CrossRef - Phenotyping of Drosophila Melanogaster—A Nutritional Perspective
Virginia Eickelberg, Kai Lüersen, Stefanie Staats, Gerald Rimbach
Biomolecules.2022; 12(2): 221. CrossRef - Consumer Expectation of Flavored Water Function, Sensory Quality, and Sugar Reduction, and the Impact of Demographic Variables and Woman Consumer Segment
Uijeong An, Xiaofen Du, Wanyi Wang
Foods.2022; 11(10): 1434. CrossRef - Sex as an independent variable in the measurement of satiation: a retrospective cohort study
Maria D. Hurtado, Lizeth Cifuentes, Alejandro Campos, Alan De La Rosa, Ekta Kapoor, Stephanie S. Faubion, Donald D. Hensrud, Michael Camilleri, Andres Acosta
International Journal of Obesity.2022; 46(12): 2156. CrossRef - Associations between Overweight and Obesity and Common Mental Disorders and Eating Behaviors of Adult Women
Ana Clara Justino Valencio, Andressa Bueno Antunes, Lilian Fonseca, Julia Araujo, Maria Clara Goyer Silva, Marcia Costa, Juliana Gomes e Silva Czermainski, Carolina Böettge Rosa, Chaline Caren Coghetto, Randhall Bruce Carteri
Obesities.2022; 2(4): 350. CrossRef - Appetitive Motivation and Associated Neurobiology Change Differentially across the Life Course of Mouse Offspring Exposed to Peri- and Postnatal High Fat Feeding
Laura Contu, Christopher J. Heath, Cheryl A. Hawkes
Nutrients.2022; 14(23): 5161. CrossRef - Toward a Better Understanding of Diet–Taste Relations
Beverly J Tepper
The Journal of Nutrition.2021; 151(9): 2503. CrossRef - The Same Metabolic Response to FGF21 Administration in Male and Female Obese Mice Is Accompanied by Sex-Specific Changes in Adipose Tissue Gene Expression
Elena Makarova, Antonina Kazantseva, Anastasia Dubinina, Tatiana Jakovleva, Natalia Balybina, Konstantin Baranov, Nadezhda Bazhan
International Journal of Molecular Sciences.2021; 22(19): 10561. CrossRef - Influence of leptin administration to pregnant female mice on obesity development, taste preferences, and gene expression in the liver and muscles of their male and female offspring
E. I. Denisova, M. M. Savinkova, E. N. Makarova
Vavilov Journal of Genetics and Breeding.2021; 25(6): 669. CrossRef
- Phytochemical composition, toxicological profiling and effect on pup birth weight of Corchorus olitorius leaf extract in rats: Implications for fetal macrosomia control

- Obesity and Metabolism
- Digital Therapeutics for Obesity and Eating-Related Problems
- Meelim Kim, Hyung Jin Choi
- Endocrinol Metab. 2021;36(2):220-228. Published online March 24, 2021
- DOI: https://doi.org/10.3803/EnM.2021.107
- 9,333 View
- 406 Download
- 13 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
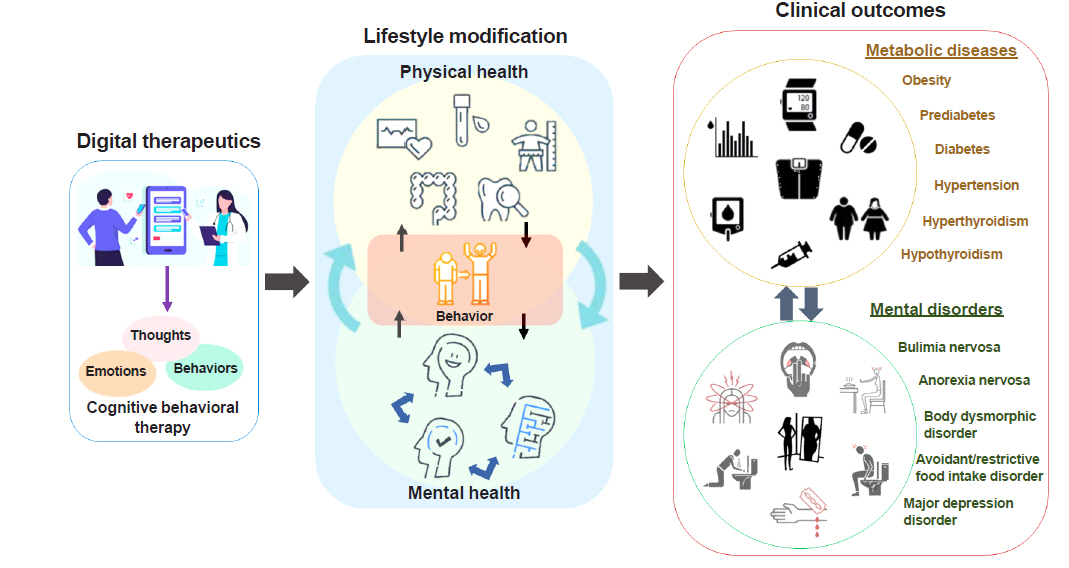
ePub - In recent years, digital technologies have rapidly advanced and are being applied to remedy medical problems. These technologies allow us to monitor and manage our physical and mental health in our daily lives. Since lifestyle modification is the cornerstone of the management of obesity and eating behavior problems, digital therapeutics (DTx) represent a powerful and easily accessible treatment modality. This review discusses the critical issues to consider for enhancing the efficacy of DTx in future development initiatives. To competently adapt and expand public access to DTx, it is important for various stakeholders, including health professionals, patients, and guardians, to collaborate with other industry partners and policy-makers in the ecosystem.
-
Citations
Citations to this article as recorded by- KIOS: A smartphone app for self‐monitoring for patients with bipolar disorder
Mehak Pahwa, Susan L. McElroy, Richard Priesmeyer, Gregg Siegel, Phyllis Siegel, Sharon Nuss, Charles L. Bowden, Rif S. El‐Mallakh
Bipolar Disorders.2024; 26(1): 84. CrossRef - What digital health technology types are used in mental health prevention and intervention? Review of systematic reviews for systematization of technologies
Naomichi Tani, Hiroaki Fujihara, Kenji Ishii, Yoshiyuki Kamakura, Mafu Tsunemi, Chikae Yamaguchi, Hisashi Eguchi, Kotaro Imamura, Satoru Kanamori, Noriko Kojimahara, Takeshi Ebara
Journal of Occupational Health.2024;[Epub] CrossRef - Digital therapeutics from bench to bedside
Changwon Wang, Chungkeun Lee, Hangsik Shin
npj Digital Medicine.2023;[Epub] CrossRef - Digital Therapeutics: Emerging New Therapy for Nonalcoholic Fatty Liver Disease
Run Zhou, Yunpeng Gu, Binbin Zhang, Tingting Kong, Wei Zhang, Jie Li, Junping Shi
Clinical and Translational Gastroenterology.2023; 14(4): e00575. CrossRef - Digital Therapeutics as a New Therapeutic Modality: A Review from the Perspective of Clinical Pharmacology
Benjamin Ribba, Richard Peck, Lucy Hutchinson, Imein Bousnina, Dario Motti
Clinical Pharmacology & Therapeutics.2023; 114(3): 578. CrossRef - eHealth in obesity care
Bukhosi Raymond Sithole, Yannis Pappas, Gurch Randhawa
Clinical Medicine.2023; 23(4): 347. CrossRef - Strategies for Long-Term Weight Loss and Maintenance
Yoo-Bin Seo
Korean Journal of Family Practice.2023; 13(3): 128. CrossRef - Implications of immersive technologies in healthcare sector and its built environment
Eunsil Yang
Frontiers in Medical Technology.2023;[Epub] CrossRef - Cost-effectiveness analysis of digital therapeutics for home-based cardiac rehabilitation for patients with atrial fibrillation after catheter ablation
Tianyi Liu, Zhijie Tang, Cheng Cai, Nan Wu, Jian Jia, Gang Yang, Wenhong Zhang
DIGITAL HEALTH.2023;[Epub] CrossRef - Cost-effectiveness analysis of digital therapeutics for home-based cardiac rehabilitation for patients with chronic heart failure: model development and data analysis
Tianyi Liu, Yiyang Zhan, Silei Chen, Wenhong Zhang, Jian Jia
Cost Effectiveness and Resource Allocation.2023;[Epub] CrossRef - Comprehensive traditional East Asian medicine treatment strategy for obesity considering the therapeutic effects and adverse events
Hongmin Chu, Byungsoo Kang, Bo-Young Youn, Kwan-il Kim, Jinbong Park, Jungtae Leem
Medicine.2022; 101(6): e28673. CrossRef - Clinical Evaluation of Digital Therapeutics: Present and Future
Ki Young Huh, Jaeseong Oh, SeungHwan Lee, Kyung-Sang Yu
Healthcare Informatics Research.2022; 28(3): 188. CrossRef - Health-Related Indicators Measured Using Earable Devices: Systematic Review
Jin-Young Choi, Seonghee Jeon, Hana Kim, Jaeyoung Ha, Gyeong-suk Jeon, Jeong Lee, Sung-il Cho
JMIR mHealth and uHealth.2022; 10(11): e36696. CrossRef - Clinical Efficacy of a Digital Intervention for Patients with Atopic Dermatitis: a Prospective Single-Center Study
Sigrídur Lára Gudmundsdóttir, Tommaso Ballarini, María L. Ámundadóttir, Judit Mészáros, Jenna H. Eysteinsdóttir, Ragna H. Thorleifsdóttir, Sigrídur K. Hrafnkelsdóttir, Heida B. Bragadóttir, Saemundur Oddsson, Jonathan I. Silverberg
Dermatology and Therapy.2022; 12(11): 2601. CrossRef
- KIOS: A smartphone app for self‐monitoring for patients with bipolar disorder

- Obesity and Metabolism
- Dopaminergic Control of the Feeding Circuit
- Ja-Hyun Baik
- Endocrinol Metab. 2021;36(2):229-239. Published online April 6, 2021
- DOI: https://doi.org/10.3803/EnM.2021.979

- 9,102 View
- 469 Download
- 12 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - There is increasing evidence demonstrating that reward-related motivational food intake is closely connected with the brain’s homeostatic system of energy balance and that this interaction might be important in the integrative control of feeding behavior. Dopamine regulates motivational behavior, including feeding behaviors, and the dopamine reward system is recognized as the most prominent system that controls appetite and motivational and emotional drives for food. It appears that the dopamine system exerts a critical role in the control of feeding behavior not only by the reward-related circuit, but also by contributing to the homeostatic circuit of food intake, suggesting that dopamine plays an integrative role across the converging circuitry of control of food intake by linking energy state-associated signals to reward-related behaviors. This review will cover and discuss up-to-date findings on the dopaminergic control of food intake by both the reward-related circuit and the homeostatic hypothalamic system.
-
Citations
Citations to this article as recorded by- Cross-cultural adaptation and psychometric investigation of the palatable eating motives scale (PEMS) for a sample of Brazilian adults
Priscila Carvalho Santos, Wanderson Roberto da Silva, João Marôco, Juliana Alvares Duarte Bonini Campos
Current Psychology.2024; 43(7): 6360. CrossRef - The Calmodulin-interacting peptide Pcp4a regulates feeding state-dependent behavioral choice in zebrafish
Margherita Zaupa, Nagarjuna Nagaraj, Anna Sylenko, Herwig Baier, Suphansa Sawamiphak, Alessandro Filosa
Neuron.2024; 112(7): 1150. CrossRef - Maternal nanoplastic ingestion induces an increase in offspring body weight through altered lipid species and microbiota
Bohyeon Jeong, Ji-Sun Kim, A Ra Kwon, Jangjae Lee, Subin Park, Jahong Koo, Wang Sik Lee, Jeong Yeob Baek, Won-Ho Shin, Jung-Sook Lee, Jinyoung Jeong, Won Kon Kim, Cho-Rok Jung, Nam-Soon Kim, Sung-Hee Cho, Da Yong Lee
Environment International.2024; 185: 108522. CrossRef - Satiety: a gut–brain–relationship
Ghinwa M. Barakat, Wiam Ramadan, Ghaith Assi, Noura B. El Khoury
The Journal of Physiological Sciences.2024;[Epub] CrossRef - Effect of Probiotic Lacticaseibacillus rhamnosus LB1.5 on Anxiety-like Behavior, Neuroprotection and Neuroinflammation Markers of Male Mice Fed a High-Fat Diet
Natália Perin Schmidt, Patrícia Molz, Brenda Santos Fraga, Nicole Hiller Bondarczuk, Priscila Dutra Silveira, Milena Henrique Ferri, Thais Busatto Crestani, Gabriela Merker Breyer, Giuliano Rizzoto Guimarães, Amanda de Souza da Motta, Renata Padilha Guede
Nutrients.2024; 16(6): 879. CrossRef -
Retracted
: Pan‐neuronal knockdown of Ras GTPase‐activating protein 1 alters
Drosophila
activity and sleep behavior
Francisco Alejandro Lagunas‐Rangel
Archives of Insect Biochemistry and Physiology.2023;[Epub] CrossRef - Maternal Over- and Malnutrition and Increased Risk for Addictive and Eating Disorders in the Offspring
Mathilde C. C. Guillaumin, Daria Peleg-Raibstein
Nutrients.2023; 15(5): 1095. CrossRef - Carving the senescent phenotype by the chemical reactivity of catecholamines: An integrative review
Aleksei G. Golubev
Ageing Research Reviews.2022; 75: 101570. CrossRef - Obesity I: Overview and molecular and biochemical mechanisms
Robert H. Lustig, David Collier, Christopher Kassotis, Troy A. Roepke, Min Ji Kim, Etienne Blanc, Robert Barouki, Amita Bansal, Matthew C. Cave, Saurabh Chatterjee, Mahua Choudhury, Michael Gilbertson, Dominique Lagadic-Gossmann, Sarah Howard, Lars Lind,
Biochemical Pharmacology.2022; 199: 115012. CrossRef - Food preferences and thyroid hormones in children and adolescents with obesity
Daniela Staníková, Lea Krajčovičová, Linda Demková, Petronela Forišek-Paulová, Lucia Slobodová, Eva Vitariušová, Lubica Tichá, Barbara Ukropcová, Juraj Staník, Jozef Ukropec
Frontiers in Psychiatry.2022;[Epub] CrossRef - Dopamine systems and biological rhythms: Let’s get a move on
Qijun Tang, Dina R. Assali, Ali D. Güler, Andrew D. Steele
Frontiers in Integrative Neuroscience.2022;[Epub] CrossRef - Suprachiasmatic to paraventricular nuclei interaction generates normal food searching rhythms in mice
Iwona Olejniczak, Benjamin Campbell, Yuan-Chen Tsai, Shiva K. Tyagarajan, Urs Albrecht, Jürgen A. Ripperger
Frontiers in Physiology.2022;[Epub] CrossRef - THE ROLE OF CIRCADIAN REGULATION OF GHRELIN LEVELS IN PARKINSON’S DISEASE (LITERATURE REVIEW)
Kateryna A. Tarianyk, Nataliya V. Lytvynenko, Anastasiia D. Shkodina, Igor P. Kaidashev
Wiadomości Lekarskie.2021; 74(7): 1750. CrossRef
- Cross-cultural adaptation and psychometric investigation of the palatable eating motives scale (PEMS) for a sample of Brazilian adults

- Diabetes
- Continuous Glucose Monitoring in the Hospital
- M. Citlalli Perez-Guzman, Trisha Shang, Jennifer Y. Zhang, Donna Jornsay, David C. Klonoff
- Endocrinol Metab. 2021;36(2):240-255. Published online March 31, 2021
- DOI: https://doi.org/10.3803/EnM.2021.201
- 16,744 View
- 664 Download
- 26 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
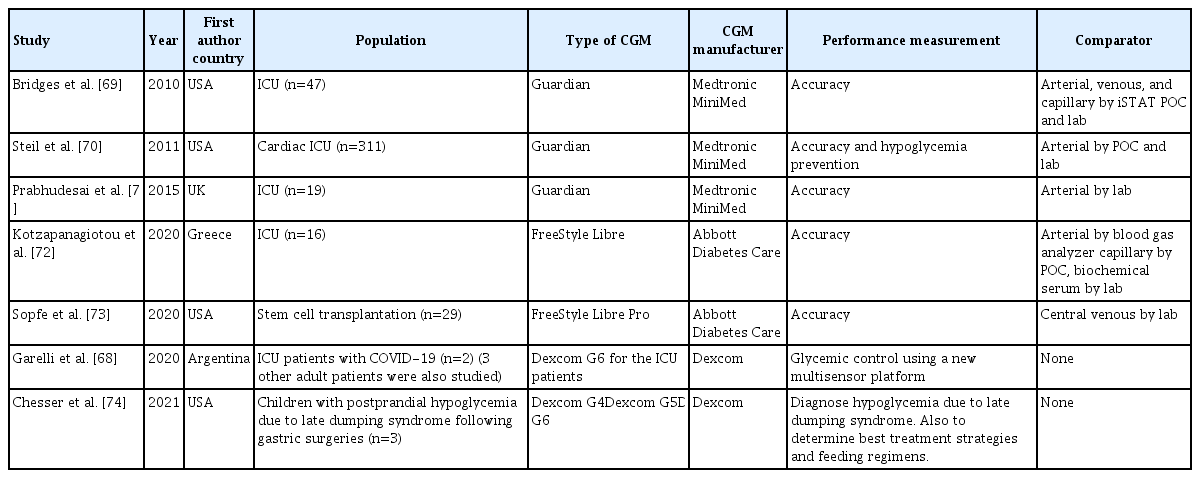
ePub - Continuous glucose monitors (CGMs) have suddenly become part of routine care in many hospitals. The coronavirus disease 2019 (COVID-19) pandemic has necessitated the use of new technologies and new processes to care for hospitalized patients, including diabetes patients. The use of CGMs to automatically and remotely supplement or replace assisted monitoring of blood glucose by bedside nurses can decrease: the amount of necessary nursing exposure to COVID-19 patients with diabetes; the amount of time required for obtaining blood glucose measurements, and the amount of personal protective equipment necessary for interacting with patients during the blood glucose testing. The United States Food and Drug Administration (FDA) is now exercising enforcement discretion and not objecting to certain factory-calibrated CGMs being used in a hospital setting, both to facilitate patient care and to obtain performance data that can be used for future regulatory submissions. CGMs can be used in the hospital to decrease the frequency of fingerstick point of care capillary blood glucose testing, decrease hyperglycemic episodes, and decrease hypoglycemic episodes. Most of the research on CGMs in the hospital has focused on their accuracy and only recently outcomes data has been reported. A hospital CGM program requires cooperation of physicians, bedside nurses, diabetes educators, and hospital administrators to appropriately select and manage patients. Processes for collecting, reviewing, storing, and responding to CGM data must be established for such a program to be successful. CGM technology is advancing and we expect that CGMs will be increasingly used in the hospital for patients with diabetes.
-
Citations
Citations to this article as recorded by- Accuracy and Safety of the 15-Day CareSens Air Continuous Glucose Monitoring System
Kyung-Soo Kim, Seung-Hwan Lee, Won Sang Yoo, Cheol-Young Park
Diabetes Technology & Therapeutics.2024; 26(4): 222. CrossRef - Glucose management in critically ill adults: A qualitative study from the experiences of health care providers
Miao Huang, Li Yang, Chuanlai Zhang, Xiuni Gan
Heliyon.2024; 10(3): e24545. CrossRef - The Need for Data Standards and Implementation Policies to Integrate CGM Data into the Electronic Health Record
Juan Espinoza, Nicole Y. Xu, Kevin T. Nguyen, David C. Klonoff
Journal of Diabetes Science and Technology.2023; 17(2): 495. CrossRef - Staff knowledge, attitudes and practices regarding glycaemic management in adult intensive care units: A national survey
Miao Huang, Ruiqi Yang, Chuanlai Zhang, Xiuni Gan
Nursing in Critical Care.2023; 28(6): 931. CrossRef - Continuous Glucose Monitoring for Patients with COVID-19 Pneumonia: Initial Experience at a Tertiary Care Center
Adrian G. Dumitrascu, Michelle F. Perry, Rebecca J. Boone, Maria P. Guzman, Razvan M. Chirila, Allyson W. McNally, Dorin T. Colibaseanu, Shon E. Meek, Colleen T. Ball, Launia J. White, Ana-Maria Chindris
Endocrine Practice.2023; 29(3): 155. CrossRef - Use of Continuous Glucose Monitors to Manage Type 1 Diabetes Mellitus: Progress, Challenges, and Recommendations
Jared G Friedman, Zulma Cardona Matos, Emily D Szmuilowicz, Grazia Aleppo
Pharmacogenomics and Personalized Medicine.2023; Volume 16: 263. CrossRef - Type 1 Diabetes Overview and Perioperative Management
Grace B. Nelson, Kathryn M. Sumpter
Orthopedic Clinics of North America.2023; 54(3): 287. CrossRef - Real-Time Continuous Glucose Monitoring in the Hospital: A Real-World Experience
Samantha R. Spierling Bagsic, Addie L. Fortmann, Rebekah Belasco, Alessandra Bastian, Suzanne Lohnes, Anna Ritko, Haley Sandoval, Mariya Chichmarenko, Emily C. Soriano, Laura Talavera, Athena Philis-Tsimikas
Journal of Diabetes Science and Technology.2023; 17(3): 656. CrossRef - Implementation of Continuous Glucose Monitoring in Critical Care: A Scoping Review
Eileen R. Faulds, Kathleen M. Dungan, Molly McNett
Current Diabetes Reports.2023; 23(6): 69. CrossRef - Clinical Use of Continuous Glucose Monitoring in Critically Ill Pediatric Patients with Diabetic Ketoacidosis
Esther Park, Minsun Kim
Diabetes Technology & Therapeutics.2023; 25(8): 529. CrossRef - Comparison of Glycemia Risk Index with Time in Range for Assessing Glycemic Quality
Ji Yoon Kim, Jee Hee Yoo, Jae Hyeon Kim
Diabetes Technology & Therapeutics.2023; 25(12): 883. CrossRef - A randomized trial of continuous glucose monitoring to improve post‐transplant glycemic control
Nicholas Jandovitz, Sam J. George, Mersema Abate, Adam M. Kressel, Alexandra C. Bolognese, Lawrence Lau, Vinay Nair, Elliot Grodstein
Clinical Transplantation.2023;[Epub] CrossRef - More Green, Less Red: How Color Standardization May Facilitate Effective Use of CGM Data
Richard M. Bergenstal, Gregg D. Simonson, Lutz Heinemann
Journal of Diabetes Science and Technology.2022; 16(1): 3. CrossRef - Continuous glucose monitoring in the hospital: an update in the era of COVID-19
Chikara Gothong, Lakshmi G. Singh, Medha Satyarengga, Elias K. Spanakis
Current Opinion in Endocrinology, Diabetes & Obesity.2022; 29(1): 1. CrossRef - Breakthrough technology for in-hospital glucose monitoring
David Kerr, David Klonoff
The Lancet Diabetes & Endocrinology.2022; 10(5): 304. CrossRef - The Role of the Diabetes Care and Education Specialist in the Hospital Setting
The Science of Diabetes Self-Management and Care.2022; 48(3): 184. CrossRef - Real-Time Monitoring of Blood Parameters in the Intensive Care Unit: State-of-the-Art and Perspectives
Rebecca Bockholt, Shaleen Paschke, Lars Heubner, Bergoi Ibarlucea, Alexander Laupp, Željko Janićijević, Stephanie Klinghammer, Sascha Balakin, Manfred F. Maitz, Carsten Werner, Gianaurelio Cuniberti, Larysa Baraban, Peter Markus Spieth
Journal of Clinical Medicine.2022; 11(9): 2408. CrossRef - Novel Glycemic Index Based on Continuous Glucose Monitoring to Predict Poor Clinical Outcomes in Critically Ill Patients: A Pilot Study
Eun Yeong Ha, Seung Min Chung, Il Rae Park, Yin Young Lee, Eun Young Choi, Jun Sung Moon
Frontiers in Endocrinology.2022;[Epub] CrossRef - Stress-Induced Hyperglycemia: Consequences and Management
Deepanjali Vedantam, Devyani S Poman, Lakshya Motwani, Nailah Asif, Apurva Patel, Krishna Kishore Anne
Cureus.2022;[Epub] CrossRef - Hospital Diabetes Meeting 2022
Jingtong Huang, Andrea M. Yeung, Kevin T. Nguyen, Nicole Y. Xu, Jean-Charles Preiser, Robert J. Rushakoff, Jane Jeffrie Seley, Guillermo E. Umpierrez, Amisha Wallia, Andjela T. Drincic, Roma Gianchandani, M. Cecilia Lansang, Umesh Masharani, Nestoras Math
Journal of Diabetes Science and Technology.2022; 16(5): 1309. CrossRef - Effects of Patient-Driven Lifestyle Modification Using Intermittently Scanned Continuous Glucose Monitoring in Patients With Type 2 Diabetes: Results From the Randomized Open-label PDF Study
Hun Jee Choe, Eun-Jung Rhee, Jong Chul Won, Kyong Soo Park, Won-Young Lee, Young Min Cho
Diabetes Care.2022; 45(10): 2224. CrossRef - The Devil Is in the Details: Use, Limitations, and Implementation of Continuous Glucose Monitoring in the Inpatient Setting
Rebecca Rick Longo, Renu Joshi
Diabetes Spectrum.2022; 35(4): 405. CrossRef
- Accuracy and Safety of the 15-Day CareSens Air Continuous Glucose Monitoring System

- Diabetes
- Cardiorenal Protection in Diabetic Kidney Disease
- Jason F. Lee, Ecaterina Berzan, Vikas S. Sridhar, Ayodele Odutayo, David Z.I. Cherney
- Endocrinol Metab. 2021;36(2):256-269. Published online April 19, 2021
- DOI: https://doi.org/10.3803/EnM.2021.987

- 5,713 View
- 300 Download
- 8 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Over the last 5 years there have been many new developments in the management of diabetic kidney disease. Glucagon-like peptide-1 receptor agonists (GLP-1 RA) and sodium-glucose cotransporter-2 (SGLT2) inhibitors were initially used for glycemic control, but more recent studies have now shown that their benefits extend to cardiovascular and kidney outcomes. The recent addition of data on the novel mineralocorticoid receptor antagonist (MRA) gives us another approach to further decrease the residual risk of diabetic kidney disease progression. In this review we describe the mechanism of action, key studies, and possible adverse effects related to these three classes of medications. The management of type 2 diabetes now includes an increasing number of medications for the management of comorbidities in a patient population at significant risk of cardiovascular disease and progression of chronic kidney disease. It is from this perspective that we seek to outline the rationale for the sequential and/or combined use of SGLT2 inhibitors, GLP-1 RA and MRAs in patients with type 2 diabetes for heart and kidney protection.
-
Citations
Citations to this article as recorded by- Relative and Absolute Risks of Adverse Events with Real-World Use of SGLT2 Inhibitors in CKD
Ayodele Odutayo, Adeera Levin
Clinical Journal of the American Society of Nephrology.2023; 18(5): 557. CrossRef - Renal Protection of Mineralocorticoid Receptor Antagonist, Finerenone, in Diabetic Kidney Disease
Dong-Lim Kim, Seung-Eun Lee, Nan Hee Kim
Endocrinology and Metabolism.2023; 38(1): 43. CrossRef - Intrarenal Mechanisms of Sodium-Glucose Cotransporter-2 Inhibitors on Tubuloglomerular Feedback and Natriuresis
Eun Sil Koh, Gheun-Ho Kim, Sungjin Chung
Endocrinology and Metabolism.2023; 38(4): 359. CrossRef - SGLT2 and DPP4 inhibitors improve Alzheimer’s disease–like pathology and cognitive function through distinct mechanisms in a T2D–AD mouse model
A Young Sim, Da Hyun Choi, Jong Youl Kim, Eun Ran Kim, A-ra Goh, Yong-ho Lee, Jong Eun Lee
Biomedicine & Pharmacotherapy.2023; 168: 115755. CrossRef - Narrative review investigating the nephroprotective mechanisms of sodium glucose cotransporter type 2 inhibitors in diabetic and nondiabetic patients with chronic kidney disease
Emma S. Speedtsberg, Martin Tepel
Frontiers in Endocrinology.2023;[Epub] CrossRef - Management of CKD
Nimrit Goraya, Jennifer D. Moran
Nephrology Self-Assessment Program.2022; 21(2): 146. CrossRef - Nonsteroidal mineralocorticoid receptor antagonism for cardiovascular and renal disorders − New perspectives for combination therapy
Peter Kolkhof, Amer Joseph, Ulrich Kintscher
Pharmacological Research.2021; 172: 105859. CrossRef - Sodium‐Glucose Cotransporter 2 Inhibitors, All‐Cause Mortality, and Cardiovascular Outcomes in Adults with Type 2 Diabetes: A Bayesian Meta‐Analysis and Meta‐Regression
Ayodele Odutayo, Bruno R. da Costa, Tiago V. Pereira, Vinay Garg, Samir Iskander, Fatimah Roble, Rahim Lalji, Cesar A. Hincapié, Aquila Akingbade, Myanca Rodrigues, Arnav Agarwal, Bishoy Lawendy, Pakeezah Saadat, Jacob A. Udell, Francesco Cosentino, Peter
Journal of the American Heart Association.2021;[Epub] CrossRef - Finerenone: A Potential Treatment for Patients with Chronic Kidney Disease and Type 2 Diabetes Mellitus
Luis D’Marco, María Jesús Puchades, Lorena Gandía, Claudia Forquet, Elena Giménez-Civera, Nayara Panizo, Javier Reque, Isabel Juan-García, Valmore Bermúdez, José Luis Gorriz
touchREVIEWS in Endocrinology.2021; 17(2): 84. CrossRef - Sodium-Glucose Cotransporter 2 Inhibitors Mechanisms of Action: A Review
Jorge I. Fonseca-Correa, Ricardo Correa-Rotter
Frontiers in Medicine.2021;[Epub] CrossRef
- Relative and Absolute Risks of Adverse Events with Real-World Use of SGLT2 Inhibitors in CKD

- Bone Metabolism
- Operationalizing Treat-to-Target for Osteoporosis
- E. Michael Lewiecki
- Endocrinol Metab. 2021;36(2):270-278. Published online March 24, 2021
- DOI: https://doi.org/10.3803/EnM.2021.970

- 5,524 View
- 297 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Treat-to-target (TTT) for osteoporosis is a concept for individualizing patient treatment decisions that focuses on achieving an acceptable level of fracture risk rather than response to treatment alone. While a response to treatment is essential in order to achieve an acceptable level of risk, it is not necessarily sufficient. Some patients have a good response to treatment yet remain at high level of fracture risk. Since there is no way to directly measure bone strength in patients treated for osteoporosis, a surrogate measurement must be used. Bone mineral density (BMD) is commonly used to select patients for treatment and has emerged as the most useful surrogate for assessing reduction of fracture risk after treatment is started. Recent large meta-regression studies have shown a robust correlation between larger increases in BMD with treatment and greater reductions in fracture risk. Application of TTT for osteoporosis involves assessing fracture risk before starting treatment and initiating treatment with an agent that is most likely to reduce fracture risk to an acceptable level, represented by a target BMD T-score, over a reasonable period of time. This review offers suggestions for implementing TTT for osteoporosis in clinical practice and managing patients who fail or succeed in reaching the target. More study is needed to fully validate the use of TTT for osteoporosis for initiating and modifying treatments to reduce fracture risk.
-
Citations
Citations to this article as recorded by- Treatment sequencing using the dual amylin and calcitonin receptor agonist KBP-336 and semaglutide results in durable weight loss
Anna Thorsø Larsen, Morten A. Karsdal, Kim Henriksen
European Journal of Pharmacology.2023; 954: 175837. CrossRef - Osteoporosis: Spotlight on current approaches to pharmacological treatment
Dilşad Sindel
Turkish Journal of Physical Medicine and Rehabilitation.2023; 69(2): 140. CrossRef - Postmenopausal Osteoporosis
Caren G. Solomon, Marcella Donovan Walker, Elizabeth Shane
New England Journal of Medicine.2023; 389(21): 1979. CrossRef - Prevalence and Risk Factors of T-Score Spine-Hip Discordance in Patients with Osteoporotic Vertebral Compression Fracture
Byung-Ho Yoon, Ho Won Kang, Su Min Kim, Young Do Koh
Journal of Bone Metabolism.2022; 29(1): 43. CrossRef - Pharmacological treatment of osteoporosis: 2022 update
Yunkyung Jeon, In-Joo Kim
Journal of the Korean Medical Association.2022; 65(4): 241. CrossRef
- Treatment sequencing using the dual amylin and calcitonin receptor agonist KBP-336 and semaglutide results in durable weight loss

- Obesity and Metabolism
- Role of PCSK9 Inhibitors in Patients with Familial Hypercholesterolemia
- Brian Tomlinson, Nivritti Gajanan Patil, Manson Fok, Christopher Wai Kei Lam
- Endocrinol Metab. 2021;36(2):279-295. Published online April 19, 2021
- DOI: https://doi.org/10.3803/EnM.2021.964
- 6,511 View
- 295 Download
- 14 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
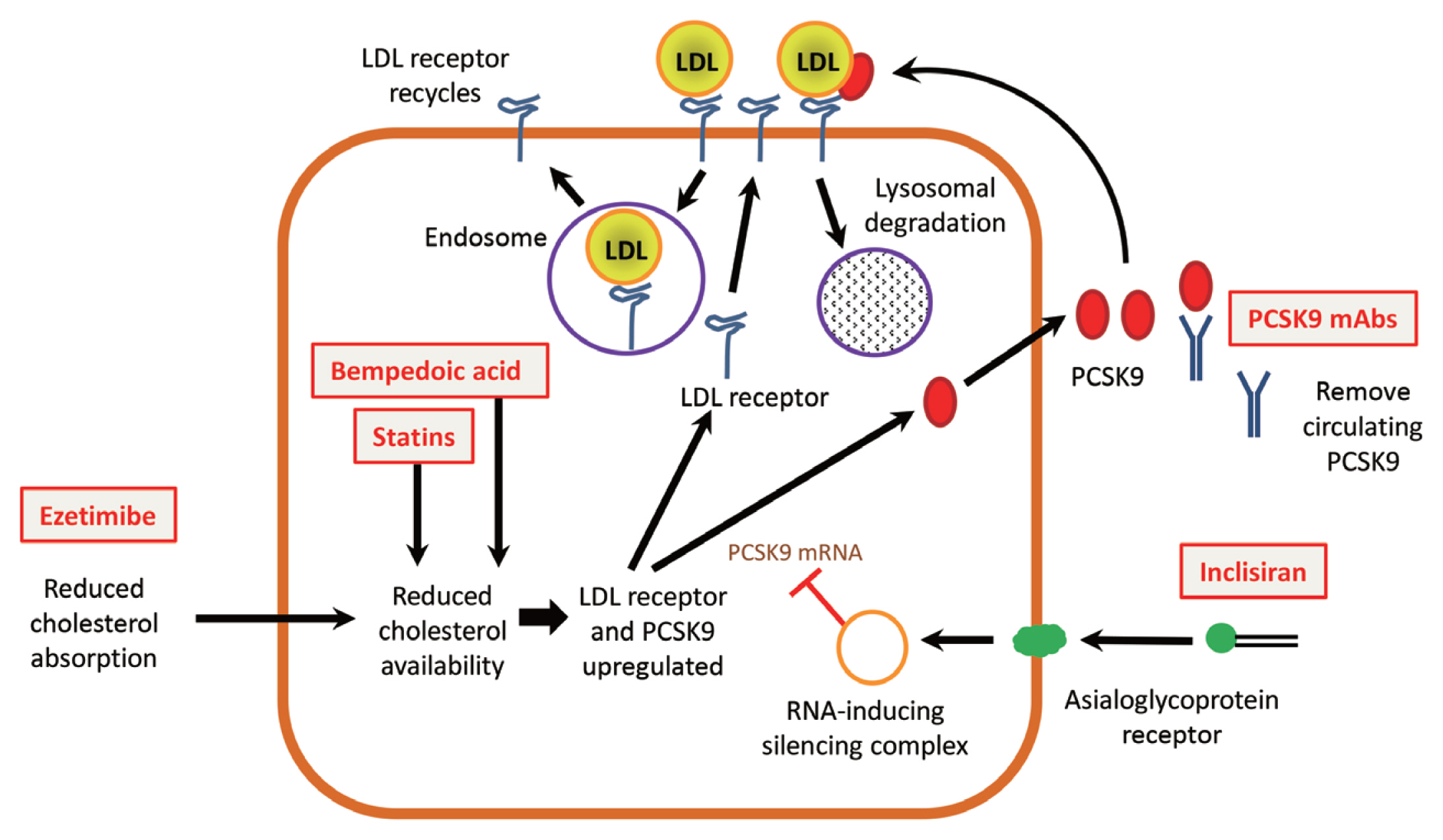
ePub - Patients with familial hypercholesterolemia (FH) are at high or very high risk for cardiovascular disease. Those with heterozygous FH (HeFH) often do not reach low-density lipoprotein cholesterol (LDL-C) targets with statin and ezetimibe therapy, and those with homozygous FH (HoFH) usually require additional lipid-modifying therapies. Drugs that inhibit proprotein convertase subtilisin/kexin type 9 (PCSK9) offer a novel approach to reduce LDL-C. The monoclonal antibodies, alirocumab and evolocumab, given by subcutaneous injection every 2 or 4 weeks produce reductions in LDL-C of 50% to 60% in patients with HeFH, allowing many of them to achieve their LDL-C goals. Patients with HoFH show a reduced and more variable LDL-C response, which appears to depend on residual LDL receptor activity, and those with receptor-negative mutations may show no response. Inclisiran is a long-acting small interfering RNA therapeutic agent that inhibits the synthesis of PCSK9. Subcutaneous doses of 300 mg can reduce LDL-C by more than 50% for at least 6 months and the responses in HeFH and HoFH patients are similar to those achieved with monoclonal antibodies. These PCSK9 inhibitors are generally well tolerated and they provide a new opportunity for effective treatment for the majority of patients with FH.
-
Citations
Citations to this article as recorded by- Phenotypic homozygous familial hypercholesterolemia successfully treated with proprotein convertase subtilisin/kexin type 9 inhibitors
Ryosuke Tani, Keiji Matsunaga, Yuta Toda, Tomoko Inoue, Hai Ying Fu, Tetsuo Minamino
Clinical Case Reports.2024;[Epub] CrossRef - Targeting Lipoprotein(a): Can RNA Therapeutics Provide the Next Step in the Prevention of Cardiovascular Disease?
Henriette Thau, Sebastian Neuber, Maximilian Y. Emmert, Timo Z. Nazari-Shafti
Cardiology and Therapy.2024; 13(1): 39. CrossRef - Technologies of gene editing and related clinical trials for the treatment of genetic and acquired diseases: a systematic review
Wessam Sharaf-Eldin
Egyptian Journal of Medical Human Genetics.2024;[Epub] CrossRef - Qualitative and Quantitative Effects of PCSK9 Inhibitors in familial Hypercholesterolemia: a Synthetic Review
Aamina Shakir, Kyle Barron, Kalgi Modi
Current Problems in Cardiology.2023; 48(4): 101550. CrossRef - Inhibition of PCSK9 Improves the Development of Pulmonary Arterial Hypertension Via Down-Regulating Notch3 Expression
Peng Ye, Xiao-Min Jiang, Wei-Chun Qian, Juan Zhang
Cardiovascular Drugs and Therapy.2023;[Epub] CrossRef - Barriers and shortcomings in access to cardiovascular management and prevention for familial hypercholesterolemia during the COVID‐19 pandemic
Helen Huang, Keith S. K. Leung, Tulika Garg, Adele Mazzoleni, Goshen D. Miteu, Farida Zakariya, Wireko A. Awuah, Elaine T. S. Yin, Faaraea Haroon, Zarish Hussain, Narjiss Aji, Vikash Jaiswal, Gary Tse
Clinical Cardiology.2023; 46(8): 831. CrossRef - Familial Hypercholesterolemia in Children. The Current State of the Problem
Dinara I. Sadykova, Karina R. Salakhova, Liliya F. Galimova, Eugeniya S. Slastnikova, Chulpan D. Khaliullina
Current Pediatrics.2023; 22(3): 231. CrossRef - Long-term safety and effectiveness of alirocumab and evolocumab in familial hypercholesterolemia (FH) in Belgium
Marc Snel, Olivier S. Descamps
Acta Cardiologica.2023; : 1. CrossRef - PCSK9 inhibitors revisited: Effectiveness and safety of PCSK9 inhibitors in a real-life Spanish cohort
Juan Vicente-Valor, Xandra García-González, Sara Ibáñez-García, María Esther Durán-García, Ana de Lorenzo-Pinto, Carmen Rodríguez-González, Irene Méndez-Fernández, Juan Carlos Percovich-Hualpa, Ana Herranz-Alonso, María Sanjurjo-Sáez
Biomedicine & Pharmacotherapy.2022; 146: 112519. CrossRef - Development of small-molecule PCSK9 inhibitors for the treatment of hypercholesterolemia
Shakir Ahamad, Shintu Mathew, Waqas A. Khan, Kishor Mohanan
Drug Discovery Today.2022; 27(5): 1332. CrossRef - The biological relevance of PCSK9: when less is better…
Majambu Mbikay, Michel Chrétien
Biochemistry and Cell Biology.2022; 100(3): 189. CrossRef - Fenofibrate add-on to statin treatment is associated with low all-cause death and cardiovascular disease in the general population with high triglyceride levels
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
Metabolism.2022; 137: 155327. CrossRef - Homozygous Familial Hypercholesterolemia
Lisa Young, Emily E. Brown, Seth S. Martin
JACC: Case Reports.2022; 4(23): 101666. CrossRef - Familial Hypercholesterolemia and Its Current Diagnostics and Treatment Possibilities: A Literature Analysis
Kristina Zubielienė, Gintarė Valterytė, Neda Jonaitienė, Diana Žaliaduonytė, Vytautas Zabiela
Medicina.2022; 58(11): 1665. CrossRef - Efficacy and Safety of Alirocumab in Children and Adolescents With Homozygous Familial Hypercholesterolemia: Phase 3, Multinational Open-Label Study
Eric Bruckert, Sonia Caprio, Albert Wiegman, Min-Ji Charng, Cézar A. Zárate-Morales, Marie T. Baccara-Dinet, Garen Manvelian, Anne Ourliac, Michel Scemama, Stephen R. Daniels
Arteriosclerosis, Thrombosis, and Vascular Biology.2022; 42(12): 1447. CrossRef
- Phenotypic homozygous familial hypercholesterolemia successfully treated with proprotein convertase subtilisin/kexin type 9 inhibitors

- Obesity and Metabolism
- An Update on Contraception in Polycystic Ovary Syndrome
- Seda Hanife Oguz, Bulent Okan Yildiz
- Endocrinol Metab. 2021;36(2):296-311. Published online April 15, 2021
- DOI: https://doi.org/10.3803/EnM.2021.958
- 11,862 View
- 753 Download
- 14 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
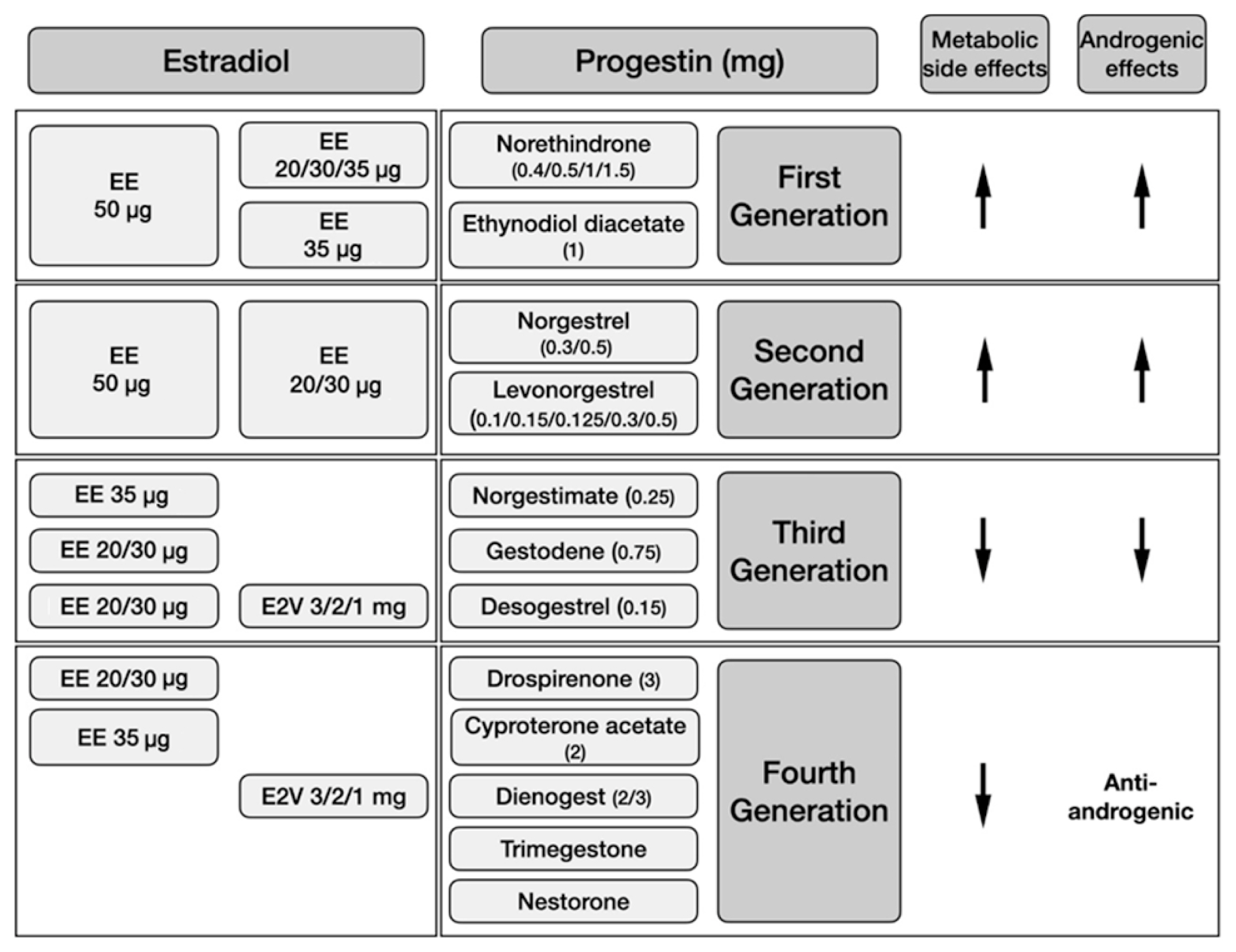
ePub - Polycystic ovary syndrome (PCOS) is a common endocrine disorder in reproductive-aged women, characterized by hyperandrogenism, oligo/anovulation, and polycystic ovarian morphology. Combined oral contraceptives (COCs), along with lifestyle modifications, represent the first-line medical treatment for the long-term management of PCOS. Containing low doses of estrogen and different types of progestin, COCs restore menstrual cyclicity, improve hyperandrogenism, and provide additional benefits such as reducing the risk of endometrial cancer. However, potential cardiometabolic risk associated with these agents has been a concern. COCs increase the risk of venous thromboembolism (VTE), related both to the dose of estrogen and the type of progestin involved. Arterial thrombotic events related to COC use occur much less frequently, and usually not a concern for young patients. All patients diagnosed with PCOS should be carefully evaluated for cardiometabolic risk factors at baseline, before initiating a COC. Age, smoking, obesity, glucose intolerance or diabetes, hypertension, dyslipidemia, thrombophilia, and family history of VTE should be recorded. Patients should be re-assessed at consecutive visits, more closely if any baseline cardiometabolic risk factor is present. Individual risk assessment is the key in order to avoid unfavorable outcomes related to COC use in women with PCOS.
-
Citations
Citations to this article as recorded by- Clinical management of androgen excess and defect in women
Elena Rosato, Francesca Sciarra, Marianna Minnetti, Anisa Degjoni, Mary Anna Venneri
Expert Review of Endocrinology & Metabolism.2024; 19(1): 21. CrossRef - Il rischio tromboembolico nella sindrome dell’ovaio policistico
Davide Ceccato, Francesca Dassie, Pietro Maffei, Roberto Mioni
L'Endocrinologo.2024; 25(2): 151. CrossRef - Systematic exploration of network pharmacology, in silico modeling and pharmacokinetic profiling for vitamin E in polycystic ovarian syndrome
Rukaiah Fatma Begum, Sumithra Mohan
Future Science OA.2024;[Epub] CrossRef - Current and emerging drug treatment strategies for polycystic ovary syndrome
Nafiye Helvaci, Bulent Okan Yildiz
Expert Opinion on Pharmacotherapy.2023; 24(1): 105. CrossRef - Weighted Gene Co-Expression Network Analysis (WGCNA) Discovered Novel Long Non-Coding RNAs for Polycystic Ovary Syndrome
Roozbeh Heidarzadehpilehrood, Maryam Pirhoushiaran, Malina Binti Osman, Habibah Abdul Hamid, King-Hwa Ling
Biomedicines.2023; 11(2): 518. CrossRef - The mechanism of Leonuri Herba in improving polycystic ovary syndrome was analyzed based on network pharmacology and molecular docking
Mali Wu, Hua Liu, Jie Zhang, Fangfang Dai, Yiping Gong, Yanxiang Cheng
Journal of Pharmacy & Pharmaceutical Sciences.2023;[Epub] CrossRef - Evaluation of the efficacy of an antioxidant combination for the modulation of metabolic, endocrine, and clinical parameters in patients with polycystic ovary syndrome
Carmen Pingarrón Santofímia, Silvia Poyo Torcal, Helena López Verdú, Alexandra Henríquez Linares, Virginia Calvente Aguilar, Pablo Terol Sánchez, María Sol Martínez García, Pilar Lafuente González
Gynecological Endocrinology.2023;[Epub] CrossRef - Contemporary Management of the Patient with Polycystic Ovary Syndrome
Nicolás Omar Francone, Tia Ramirez, Christina E. Boots
Obstetrics and Gynecology Clinics of North America.2023; 50(4): 695. CrossRef - Challenges in diagnosis and health care in polycystic ovary syndrome in Canada: a patient view to improve health care
Beate C. Sydora, Michaelann S. Wilke, Maggie McPherson, Sarah Chambers, Mahua Ghosh, Donna F. Vine
BMC Women's Health.2023;[Epub] CrossRef - Effect of Berberine Phytosome on reproductive, dermatologic, and metabolic characteristics in women with polycystic ovary syndrome: a controlled, randomized, multi-centric, open-label clinical trial
Francesco Di Pierro, Ruqqia Sultana, Amna Zia Eusaph, Saida Abrar, Mahroo Bugti, Fauzia Afridi, Umer Farooq, Somia Iqtadar, Fareeha Ghauri, Syeda Makhduma, Shazia Nourin, Ayesha Kanwal, Aasiya Bano, Ali Akbar Bugti, Shah Mureed, Ayesha Ghazal, Romana Irsh
Frontiers in Pharmacology.2023;[Epub] CrossRef - Investigation of taste function and eating behavior in women with polycystic ovary syndrome
Sila Cetik, Aylin Acikgoz, Bulent Okan Yildiz
Appetite.2022; 168: 105776. CrossRef - microRNAs and long non‐coding RNAs as biomarkers for polycystic ovary syndrome
Mona Tamaddon, Mostafa Azimzadeh, Seyed Mohammad Tavangar
Journal of Cellular and Molecular Medicine.2022; 26(3): 654. CrossRef - Effect of orlistat during individualized comprehensive life-style intervention on visceral fat in overweight or obese PCOS patients
Min Min, Xiangyan Ruan, Husheng Wang, Jiaojiao Cheng, Suiyu Luo, Zhongting Xu, Meng Li, Alfred Otto Mueck
Gynecological Endocrinology.2022; 38(8): 676. CrossRef - Effect of metformin and exenatide on pregnancy rate and pregnancy outcomes in overweight or obese infertility PCOS women: long-term follow-up of an RCT
Renyuan Li, Tingting Mai, Siyuan Zheng, Ying Zhang
Archives of Gynecology and Obstetrics.2022; 306(5): 1711. CrossRef - Oral contraceptives and stroke: Foes or friends
Varun Reddy, Megan Wurtz, Shahil H. Patel, Micheline McCarthy, Ami P. Raval
Frontiers in Neuroendocrinology.2022; 67: 101016. CrossRef - Clinical profiling of polycystic ovary syndrome patients in Kashmir population
Ahila Ashraf, Rajesh Singh, Shahnawaz Mir
Matrix Science Pharma.2022; 6(1): 23. CrossRef
- Clinical management of androgen excess and defect in women

- Miscellaneous
- Clinical Characteristics, Management, and Potential Biomarkers of Endocrine Dysfunction Induced by Immune Checkpoint Inhibitors
- Shintaro Iwama, Tomoko Kobayashi, Hiroshi Arima
- Endocrinol Metab. 2021;36(2):312-321. Published online April 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1007

- 5,472 View
- 267 Download
- 15 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Immune-related adverse events (irAEs) affecting the endocrine glands are among the most frequent irAEs induced by immune checkpoint inhibitors (ICIs) and include hypopituitarism, primary adrenal insufficiency, thyrotoxicosis, hypothyroidism, hypoparathyroidism, and type 1 diabetes mellitus. Since the incidence and clinical features of endocrine irAEs vary according to the ICI used, it is important to understand the characteristics of these irAEs and to manage each one appropriately. Since some endocrine irAEs, including adrenal crisis and diabetic ketoacidosis, are potentially life-threatening, predicting the risk of endocrine irAEs before their onset is critical. Several autoantibodies have been detected in patients who develop endocrine irAEs, among which anti-thyroid antibodies may be predictive biomarkers of thyroid dysfunction. In this review, we describe the clinical features of each endocrine irAE induced by ICIs and discuss their potential biomarkers, including autoantibodies.
-
Citations
Citations to this article as recorded by- Clinical characteristics and potential biomarkers of thyroid and pituitary immune-related adverse events
Tomoko Kobayashi, Shintaro Iwama, Hiroshi Arima
Endocrine Journal.2024; 71(1): 23. CrossRef - A case of rapidly progressive insulin-dependent diabetes mellitus without islet autoantibodies developed over two years after the first dose of nivolumab
Kota Nishihama, Yuko Okano, Chisa Inoue, Kanako Maki, Kazuhito Eguchi, Soichiro Tanaka, Atsuro Takeshita, Mei Uemura, Taro Yasuma, Toshinari Suzuki, Esteban C. Gabazza, Yutaka Yano
Diabetology International.2024;[Epub] CrossRef - Endocrinopathies Associated With Immune Checkpoint Inhibitor Use
Anupam Kotwal, Randol Kennedy, Nupur Kikani, Sonali Thosani, Whitney Goldner, Afreen Shariff
Endocrine Practice.2024;[Epub] CrossRef - Recovery from insulin dependence in immune checkpoint inhibitor‐associated diabetes mellitus: A case report
Marie Okubo, Yuji Hataya, Kanta Fujimoto, Toshio Iwakura, Naoki Matsuoka
Journal of Diabetes Investigation.2023; 14(1): 147. CrossRef - Case Report: A Rising Cause of New-Onset Endocrinopathies After Immunotherapy
Charity Tan, Sarah Hendricks, Kristina Hernandez, Martha Benavides, Rupinderjit Samra
The Journal for Nurse Practitioners.2023; 19(5): 104582. CrossRef - Risk of Thyroid Dysfunction in PD-1 Blockade Is Stratified by the Pattern of TgAb and TPOAb Positivity at Baseline
Xin Zhou, Shintaro Iwama, Tomoko Kobayashi, Masahiko Ando, Hiroshi Arima
The Journal of Clinical Endocrinology & Metabolism.2023; 108(10): e1056. CrossRef - Severe thyrotoxicosis induced by tislelizumab: a case report and literature review
Liman Huo, Chao Wang, Haixia Ding, Xuelian Shi, Bin Shan, Ruoying Zhou, Ping Liang, Juan Hou
Frontiers in Oncology.2023;[Epub] CrossRef - Life-Threatening Endocrinological Immune-Related Adverse Events of Immune Checkpoint Inhibitor Therapy
Aleksandra Basek, Grzegorz K. Jakubiak, Grzegorz Cieślar, Agata Stanek
Cancers.2023; 15(24): 5786. CrossRef - Increased Risk of Thyroid Dysfunction by PD-1 and CTLA-4 Blockade in Patients Without Thyroid Autoantibodies at Baseline
Shintaro Iwama, Tomoko Kobayashi, Yoshinori Yasuda, Takayuki Okuji, Masaaki Ito, Masahiko Ando, Xin Zhou, Ayana Yamagami, Takeshi Onoue, Yohei Kawaguchi, Takashi Miyata, Mariko Sugiyama, Hiroshi Takagi, Daisuke Hagiwara, Hidetaka Suga, Ryoichi Banno, Tets
The Journal of Clinical Endocrinology & Metabolism.2022; 107(4): e1620. CrossRef - Biomarkers and risk factors for the early prediction of immune-related adverse events: a review
Ying Zhang, Xiaoling Zhang, Weiling Li, Yunyi Du, Wenqing Hu, Jun Zhao
Human Vaccines & Immunotherapeutics.2022;[Epub] CrossRef - Immune Checkpoint Inhibitors as a Threat to the Hypothalamus–Pituitary Axis: A Completed Puzzle
Agnese Barnabei, Andrea Corsello, Rosa Maria Paragliola, Giovanni Maria Iannantuono, Luca Falzone, Salvatore Maria Corsello, Francesco Torino
Cancers.2022; 14(4): 1057. CrossRef - Elevated TSH Level, TgAb, and Prior Use of Ramucirumab or TKIs as Risk Factors for Thyroid Dysfunction in PD-L1 Blockade
Tomoko Kobayashi, Shintaro Iwama, Ayana Yamagami, Yoshinori Yasuda, Takayuki Okuji, Masaaki Ito, Xin Zhou, Masahiko Ando, Takeshi Onoue, Takashi Miyata, Mariko Sugiyama, Daisuke Hagiwara, Hidetaka Suga, Ryoichi Banno, Tetsunari Hase, Masahiro Morise, Taka
The Journal of Clinical Endocrinology & Metabolism.2022; 107(10): e4115. CrossRef - Preconditioning of the immune system modulates the response of papillary thyroid cancer to immune checkpoint inhibitors
Fabiana Pani, Yoshinori Yasuda, Sylvie T Rousseau, Kevin C Bermea, Solmaz Roshanmehr, Rulin Wang, Srinivasan Yegnasubramanian, Patrizio Caturegli, Luigi Adamo
Journal for ImmunoTherapy of Cancer.2022; 10(12): e005538. CrossRef - Survival benefit of endocrine dysfunction following immune checkpoint inhibitors for nonthyroidal cancers
Anupam Kotwal, Mabel Ryder
Current Opinion in Endocrinology, Diabetes & Obesity.2021; 28(5): 517. CrossRef
- Clinical characteristics and potential biomarkers of thyroid and pituitary immune-related adverse events

Special Article
- Adrenal gland
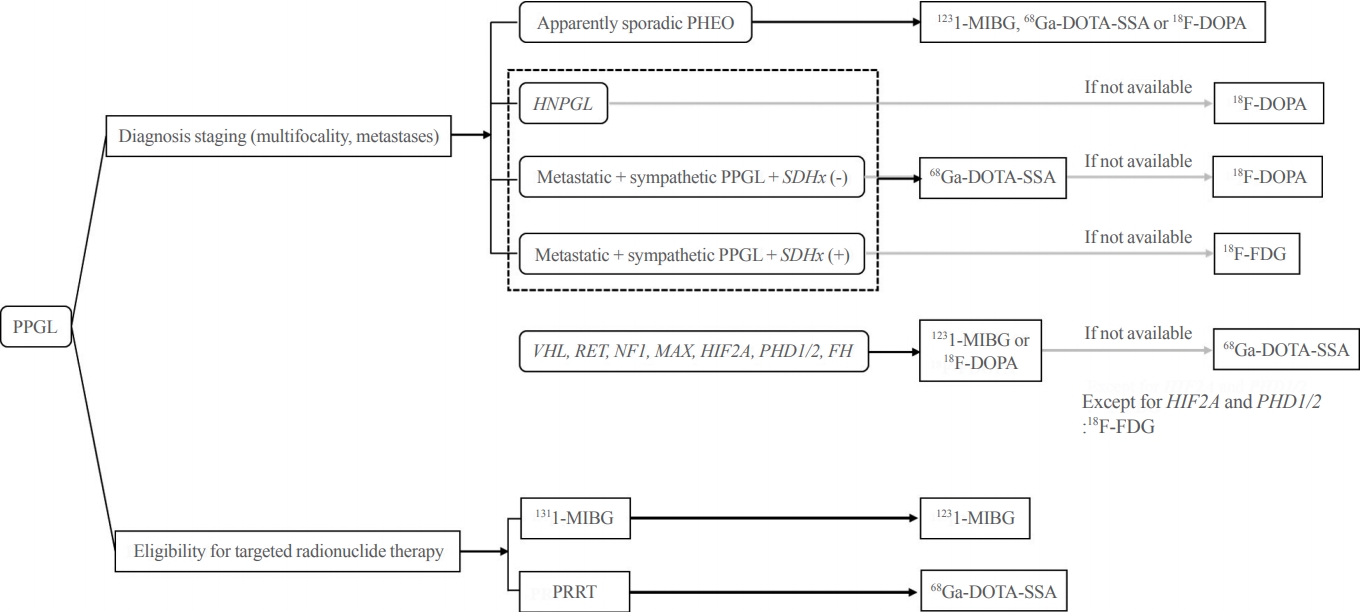
- Diagnosis for Pheochromocytoma and Paraganglioma: A Joint Position Statement of the Korean Pheochromocytoma and Paraganglioma Task Force
- Eu Jeong Ku, Kyoung Jin Kim, Jung Hee Kim, Mi Kyung Kim, Chang Ho Ahn, Kyung Ae Lee, Seung Hun Lee, You-Bin Lee, Kyeong Hye Park, Yun Mi Choi, Namki Hong, A Ram Hong, Sang-Wook Kang, Byung Kwan Park, Moon-Woo Seong, Myungshin Kim, Kyeong Cheon Jung, Chan Kwon Jung, Young Seok Cho, Jin Chul Paeng, Jae Hyeon Kim, Ohk-Hyun Ryu, Yumie Rhee, Chong Hwa Kim, Eun Jig Lee
- Endocrinol Metab. 2021;36(2):322-338. Published online April 6, 2021
- DOI: https://doi.org/10.3803/EnM.2020.908
- 7,491 View
- 572 Download
- 8 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Pheochromocytoma and paraganglioma (PPGLs) are rare catecholamine-secreting neuroendocrine tumors but can be life-threatening. Although most PPGLs are benign, approximately 10% have metastatic potential. Approximately 40% cases are reported as harboring germline mutations. Therefore, timely and accurate diagnosis of PPGLs is crucial. For more than 130 years, clinical, molecular, biochemical, radiological, and pathological investigations have been rapidly advanced in the field of PPGLs. However, performing diagnostic studies to localize lesions and detect metastatic potential can be still challenging and complicated. Furthermore, great progress on genetics has shifted the paradigm of genetic testing of PPGLs. The Korean PPGL task force team consisting of the Korean Endocrine Society, the Korean Surgical Society, the Korean Society of Nuclear Medicine, the Korean Society of Pathologists, and the Korean Society of Laboratory Medicine has developed this position statement focusing on the comprehensive and updated diagnosis for PPGLs.
-
Citations
Citations to this article as recorded by- A Prospective Comparative Study of 18F-FDOPA PET/CT Versus 123I-MIBG Scintigraphy With SPECT/CT for the Diagnosis of Pheochromocytoma and Paraganglioma
Changhwan Sung, Hyo Sang Lee, Dong Yun Lee, Yong-il Kim, Jae Eun Kim, Sang Ju Lee, Seung Jun Oh, Tae-Yon Sung, Yu-Mi Lee, Young Hoon Kim, Beom-Jun Kim, Jung-Min Koh, Seung Hun Lee, Jin-Sook Ryu
Clinical Nuclear Medicine.2024; 49(1): 27. CrossRef - Evaluation and Management of Bone Health in Patients with Thyroid Diseases: A Position Statement of the Korean Thyroid Association
A Ram Hong, Ho-Cheol Kang
Endocrinology and Metabolism.2023; 38(2): 175. CrossRef - Lesion-based indicators predict long-term outcomes of pheochromocytoma and paraganglioma– SIZEPASS
Helena Hanschell, Salvador Diaz-Cano, Alfredo Blanes, Nadia Talat, Gabriele Galatá, Simon Aylwin, Klaus Martin Schulte
Frontiers in Endocrinology.2023;[Epub] CrossRef - Interleukin-6-producing paraganglioma as a rare cause of systemic inflammatory response syndrome: a case report
Yin Young Lee, Seung Min Chung
Journal of Yeungnam Medical Science.2023; 40(4): 435. CrossRef - (Extremely rare intrapericardial location of paraganglioma)
Jaroslav Zajíc, Aleš Mokráček, Ladislav Pešl, Jiří Haniš, Dita Schaffelhoferová
Cor et Vasa.2023; 65(4): 692. CrossRef - A Case of Von Hippel-Lindau Disease With Recurrence of Paraganglioma and No Other Associated Symptoms: The Importance of Genetic Testing and Establishing Follow-Up Policies
Naoki Okada, Akihiro Shioya, Sumihito Togi, Hiroki Ura, Yo Niida
Cureus.2023;[Epub] CrossRef - KSNM60 in Nuclear Endocrinology: from the Beginning to the Future
Chae Moon Hong, Young Jin Jeong, Hae Won Kim, Byeong-Cheol Ahn
Nuclear Medicine and Molecular Imaging.2022; 56(1): 17. CrossRef - Change of Computed Tomography-Based Body Composition after Adrenalectomy in Patients with Pheochromocytoma
Yousun Ko, Heeryoel Jeong, Seungwoo Khang, Jeongjin Lee, Kyung Won Kim, Beom-Jun Kim
Cancers.2022; 14(8): 1967. CrossRef - Evaluation and Management of Bone Health in Patients with Thyroid Diseases: a Position Statement from the Korean Thyroid Association
A Ram Hong, Hwa Young Ahn, Bu Kyung Kim, Seong Hee Ahn, So Young Park, Min-Hee Kim, Jeongmin Lee, Sun Wook Cho, Ho-Cheol Kang
International Journal of Thyroidology.2022; 15(1): 1. CrossRef - Pheochromocytoma with Retroperitoneal Metastasis: A Case Report
建新 崔
Advances in Clinical Medicine.2021; 11(05): 2239. CrossRef
- A Prospective Comparative Study of 18F-FDOPA PET/CT Versus 123I-MIBG Scintigraphy With SPECT/CT for the Diagnosis of Pheochromocytoma and Paraganglioma

Editorial
- Diabetes
- New Era for Renal-Protective Therapy in Type 2 Diabetes: Better Renal Outcomes in Patients with Type 2 Diabetes Taking Sodium-Glucose Cotransporter 2 Inhibitors versus Dipeptidyl Peptidase-4 Inhibitors
- Chan-Hee Jung
- Endocrinol Metab. 2021;36(2):339-341. Published online April 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.203
- 3,037 View
- 122 Download

Original Articles
- Clinical Study
- Associations of GNAS Mutations with Surgical Outcomes in Patients with Growth Hormone-Secreting Pituitary Adenoma
- Hyein Jung, Kyungwon Kim, Daham Kim, Ju Hyung Moon, Eui Hyun Kim, Se Hoon Kim, Cheol Ryong Ku, Eun Jig Lee
- Endocrinol Metab. 2021;36(2):342-350. Published online March 23, 2021
- DOI: https://doi.org/10.3803/EnM.2020.875

- 4,335 View
- 143 Download
- 4 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The guanine nucleotide-binding protein, alpha stimulating (GNAS) gene has been associated with growth hormone (GH)-secreting pituitary adenoma. We investigated the prevalence of GNAS mutations in Korean patients with acromegaly and assessed whether mutation status correlated with biochemical or clinical characteristics.
Methods
We studied 126 patients with acromegaly who underwent surgery between 2005 and 2014 at Severance Hospital. We performed GNAS gene analysis and evaluated age, sex, hormone levels, postoperative biochemical remission, and immunohistochemical staining results of the tumor.
Results
GNAS mutations were present in 75 patients (59.5%). Patients with and without GNAS mutations showed similar age distribution and Knosp classification. The proportion of female patients was 76.5% and 48.0% in the GNAS-negative and GNAS-mutation groups, respectively (P=0.006). In immunohistochemical staining, the GNAS-mutation group showed higher GH expression in pituitary tumor tissues than the mutation-negative group (98.7% vs. 92.2%, P=0.015). Patients with GNAS mutations had higher preoperative insulin-like growth factor-1 levels (791.3 ng/mL vs. 697.0 ng/mL, P=0.045) and lower immediate postoperative basal (0.9 ng/mL vs. 1.0 ng/mL, P=0.191) and nadir GH levels (0.3 ng/mL vs. 0.6 ng/mL, P=0.012) in oral glucose tolerance tests. Finally, the GNAS-mutation group showed significantly higher surgical remission rates than the mutation-negative group, both at 1 week and 6 months after surgical resection (70.7% vs. 54.9%, P=0.011; 85.3% vs. 82.4%, P=0.007, respectively).
Conclusion
GNAS mutations in GH-secreting pituitary tumors are associated with higher preoperative insulin-like growth factor-1 levels and surgical remission rates and lower immediate postoperative nadir GH levels. Thus, GNAS mutation status can predict surgical responsiveness in patients with acromegaly. -
Citations
Citations to this article as recorded by- Genetic diagnosis in acromegaly and gigantism: From research to clinical practice
Claudia Ramírez-Rentería, Laura C. Hernández-Ramírez
Best Practice & Research Clinical Endocrinology & Metabolism.2024; : 101892. CrossRef - CD8/PD-L1 immunohistochemical reactivity and gene alterations in cutaneous squamous cell carcinoma
Haruto Nishida, Yoshihiko Kondo, Takahiro Kusaba, Kazuhiro Kawamura, Yuzo Oyama, Tsutomu Daa, Avaniyapuram Kannan Murugan
PLOS ONE.2023; 18(2): e0281647. CrossRef - Dynamic monitoring of circulating tumor DNA to analyze genetic characteristics and resistance profile of lorlatinib in ALK positive previously treated NSCLC
Xiya Ma, Kun Zhang, Jing Xu, Hongjun Gao, Shaoxing Yang, Haifeng Qin, Hong Wang, Fang Gao, Xiaoqing Liu
Thoracic Cancer.2023; 14(20): 1980. CrossRef - Multiomics Approach to Acromegaly: Unveiling Translational Insights for Precision Medicine
Kyungwon Kim, Cheol Ryong Ku, Eun Jig Lee
Endocrinology and Metabolism.2023; 38(5): 463. CrossRef - Hotspots of Somatic Genetic Variation in Pituitary Neuroendocrine Tumors
Mariana Torres-Morán, Alexa L. Franco-Álvarez, Rosa G. Rebollar-Vega, Laura C. Hernández-Ramírez
Cancers.2023; 15(23): 5685. CrossRef
- Genetic diagnosis in acromegaly and gigantism: From research to clinical practice

- Clinical Study
- Radioactive Parathyroid Adenomas on Sestamibi Scans: Low Parathyroid Hormone Secretory Potential and Large Volume
- Sung Hye Kong, Jung Hee Kim, Sang Wan Kim, Chan Soo Shin
- Endocrinol Metab. 2021;36(2):351-358. Published online April 6, 2021
- DOI: https://doi.org/10.3803/EnM.2020.823
- 3,350 View
- 123 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
We investigated the clinical characteristics of parathyroid adenomas according to radioactivity on 99mTc-methoxyisobutylisonitrile (99mTc-MIBI) single-photon emission computed tomography/computed tomography (SPECT/CT) in primary hyperparathyroidism (PHPT) patients.
Methods
The study included 217 patients diagnosed with PHPT from 2000 to 2019 at Seoul National University Hospital who underwent 99mTc-MIBI SPECT/CT scans. On SPECT/CT, the radioactivity of parathyroid adenomas was measured as the ratio of the mean radioactivity count of the parathyroid adenoma to that of the contralateral thyroid.
Results
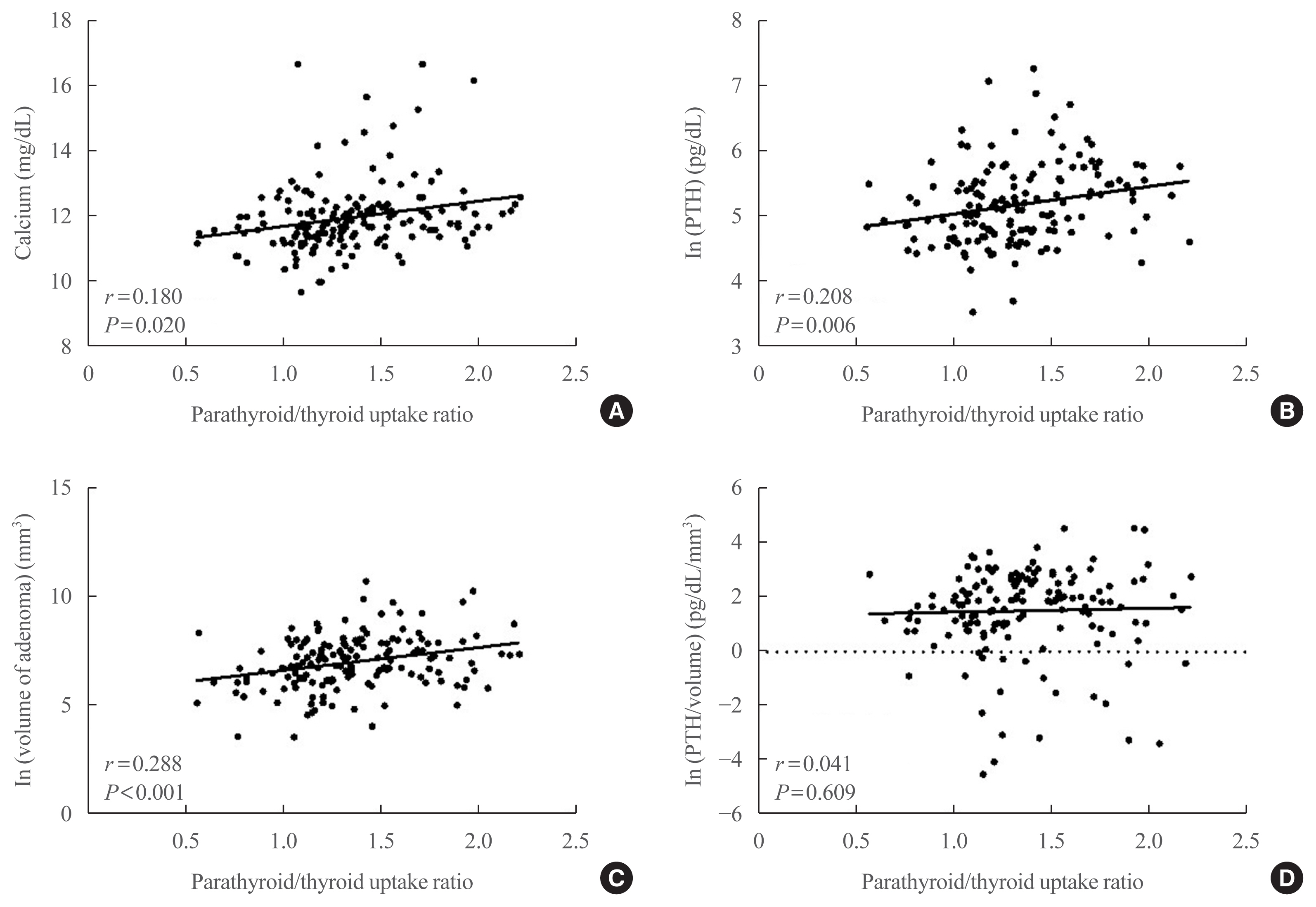
Tumors were localized by MIBI scans in 190 patients (MIBI [+] group) and by ultrasound or parathyroid four-dimensional CT in 27 patients (MIBI [–] group). The mean age was 55 years, and mean body mass index was 23.4 kg/m2. Patients in the MIBI (+) group had higher parathyroid hormone (iPTH) and lower 25-hydroxy vitamin D levels than those in the MIBI (–) group (168.0 pg/mL [interquartile range, IQR, 111.0 to 250.7] vs. 134.7 pg/mL [IQR, 98.2 to 191.2], P=0.049; 15.4 ng/mL [IQR, 11.1 to 20.8] vs. 21.2 ng/mL [IQR, 13.9 to 24.8], P=0.012, respectively). Patients in the MIBI (+) group had larger tumor volumes, but lower iPTH/volume ratios than those in the MIBI (–) group (1,216.66 [IQR, 513.40 to 2,663.02], 499.82 mm3 [IQR, 167.77 to 1,229.80], P=0.002; 0.18 [IQR, 0.08 to 0.46], 0.40 pg/mL/mm3 [IQR, 0.16 to 1.29], P=0.016, respectively). Adenoma radioactivity was positively correlated with calcium, iPTH, and volume (r=0.180, P=0.020; r=0.208, P=0.006; r=0.288, P<0.001, respectively), but not with iPTH/volume.
Conclusion
Parathyroid adenomas with positive MIBI scans had larger volumes and higher iPTH than adenomas with negative scans, but lower iPTH per unit volume. -
Citations
Citations to this article as recorded by- Atypical parathyroid tumor: clinical and parathyroid hormone response to surgical treatment
Antonio Giulio Napolitano, Massimo Monacelli, Valeria Liparulo, Eleonora Coviello, Domenico Pourmolkara, Stefano Avenia, Andrea Polistena
Annals of Surgical Treatment and Research.2023; 105(2): 76. CrossRef - The Relationship between Planar and SPECT/CT Parameters and Functional Markers in Primary Hyperparathyroidism
Guler Silov, Serpil Erdogan Ozbodur
Diagnostics.2023; 13(20): 3182. CrossRef
- Atypical parathyroid tumor: clinical and parathyroid hormone response to surgical treatment

- Clinical Study
- Protocol for a Korean Multicenter Prospective Cohort Study of Active Surveillance or Surgery (KoMPASS) in Papillary Thyroid Microcarcinoma
- Min Ji Jeon, Yea Eun Kang, Jae Hoon Moon, Dong Jun Lim, Chang Yoon Lee, Yong Sang Lee, Sun Wook Kim, Min-Hee Kim, Bo Hyun Kim, Ho-Cheol Kang, Minho Shong, Sun Wook Cho, Won Bae Kim
- Endocrinol Metab. 2021;36(2):359-364. Published online March 23, 2021
- DOI: https://doi.org/10.3803/EnM.2020.890
- Correction in: Endocrinol Metab 2022;37(1):181

- 5,792 View
- 202 Download
- 17 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
A Korean Multicenter Prospective cohort study of Active Surveillance or Surgery (KoMPASS) for papillary thyroid microcarcinomas (PTMCs) has been initiated. The aim is to compare clinical outcomes between active surveillance (AS) and an immediate lobectomy for low-risk PTMCs. We here outline the detailed protocol for this study.
Methods
Adult patients with a cytopathologically confirmed PTMC sized 6.0 to 10.0 mm by ultrasound (US) will be included. Patients will be excluded if they have a suspicious extra-thyroidal extension or metastasis of a PTMC or multiple thyroid nodules or other thyroid diseases which require a total thyroidectomy. Printed material describing the prognosis of PTMCs, and the pros and cons of each management option, will be provided to eligible patients to select their preferred intervention. For the AS group, thyroid US, thyroid function, and quality of life (QoL) parameters will be monitored every 6 months during the first year, and then annually thereafter. Disease progression will be defined as a ≥3 mm increase in maximal diameter of a PTMC, or the development of new thyroid cancers or metastases. If progression is detected, patients should undergo appropriate surgery. For the lobectomy group, a lobectomy with prophylactic central neck dissection will be done within 6 months. After initial surgery, thyroid US, thyroid function, serum thyroglobulin (Tg), anti-Tg antibody, and QoL parameters will be monitored every 6 months during the first year and annually thereafter. Disease progression will be defined in these cases as the development of new thyroid cancers or metastases.
Conclusion
KoMPASS findings will help to confirm the role of AS, and develop individualized management strategies, for low-risk PTMCs. -
Citations
Citations to this article as recorded by- Active Surveillance for Low-Risk Thyroid Cancers: A Review of Current Practice Guidelines
Min Joo Kim, Jae Hoon Moon, Eun Kyung Lee, Young Shin Song, Kyong Yeun Jung, Ji Ye Lee, Ji-hoon Kim, Kyungsik Kim, Sue K. Park, Young Joo Park
Endocrinology and Metabolism.2024; 39(1): 47. CrossRef - It Is Time to Understand the Additional Benefits of Active Surveillance for Low-Risk Papillary Thyroid Carcinoma
Kyeong Jin Kim
Endocrinology and Metabolism.2024; 39(1): 95. CrossRef - Active Surveillance for Low-Risk Papillary Thyroid Carcinoma as an Acceptable Management Option with Additional Benefits: A Comprehensive Systematic Review
Jee Hee Yoon, Wonsuk Choi, Ji Yong Park, A Ram Hong, Hee Kyung Kim, Ho-Cheol Kang
Endocrinology and Metabolism.2024; 39(1): 152. CrossRef - Active Surveillance for Low-Risk Papillary Thyroid Carcinoma as an Acceptable Management Option with Additional Benefits: A Comprehensive Systematic Review
Jee Hee Yoon, Wonsuk Choi, Ji Yong Park, A Ram Hong, Hee Kyung Kim, Ho-Cheol Kang
Endocrinology and Metabolism.2024; 39(1): 152. CrossRef - Thyroid‐Stimulating Hormone, Age, and Tumor Size are Risk Factors for Progression During Active Surveillance of Low‐Risk Papillary Thyroid Microcarcinoma in Adults
Yasuhiro Ito, Akira Miyauchi, Makoto Fujishima, Takuya Noda, Tsutomu Sano, Takahiro Sasaki, Taketoshi Kishi, Tomohiko Nakamura
World Journal of Surgery.2023; 47(2): 392. CrossRef - Thyroid FNA cytology: The Eastern versus Western perspectives
Mitsuyoshi Hirokawa, Manon Auger, Chan Kwon Jung, Fabiano Mesquita Callegari
Cancer Cytopathology.2023; 131(7): 415. CrossRef - To Screen or Not to Screen?
Do Joon Park
Endocrinology and Metabolism.2023; 38(1): 69. CrossRef - Lower Thyroid Cancer Mortality in Patients Detected by Screening: A Meta-Analysis
Shinje Moon, Young Shin Song, Kyong Yeun Jung, Eun Kyung Lee, Young Joo Park
Endocrinology and Metabolism.2023; 38(1): 93. CrossRef - Long-Term Outcomes of Active Surveillance and Immediate Surgery for Adult Patients with Low-Risk Papillary Thyroid Microcarcinoma: 30-Year Experience
Akira Miyauchi, Yasuhiro Ito, Makoto Fujishima, Akihiro Miya, Naoyoshi Onoda, Minoru Kihara, Takuya Higashiyama, Hiroo Masuoka, Shiori Kawano, Takahiro Sasaki, Mitsushige Nishikawa, Shuji Fukata, Takashi Akamizu, Mitsuru Ito, Eijun Nishihara, Mako Hisakad
Thyroid®.2023; 33(7): 817. CrossRef - Active Surveillance Outcomes of Patients with Low-Risk Papillary Thyroid Microcarcinoma According to Levothyroxine Treatment Status
Masashi Yamamoto, Akira Miyauchi, Yasuhiro Ito, Makoto Fujishima, Takahiro Sasaki, Takumi Kudo
Thyroid®.2023; 33(10): 1182. CrossRef - Cost-Effectiveness of Active Surveillance Compared to Early Surgery of Small Papillary Thyroid Cancer: A Retrospective Study on a Korean Population
Han-Sang Baek, Jeonghoon Ha, Kwangsoon Kim, Jaseong Bae, Jeong Soo Kim, Sungju Kim, Dong-Jun Lim, Chulmin Kim
Journal of Korean Medical Science.2023;[Epub] CrossRef - Optimal Cutoff Values of the Contact Angle of Tumor on Sonography System for Predicting Extrathyroidal Extension of Papillary Thyroid Carcinoma by Tumor Location
Ik Beom Shin, Do Hoon Koo, Dong Sik Bae
Clinical Medicine Insights: Oncology.2023;[Epub] CrossRef - Thermal ablation for papillary thyroid microcarcinoma located in the isthmus: a study with 3 years of follow-up
Lin Zheng, Fang-yi Liu, Jie Yu, Zhi-gang Cheng, Xiao-ling Yu, Xiao-cong Dong, Zhi-yu Han, Ping Liang
Future Oncology.2022; 18(4): 471. CrossRef - Trends in the Management of Localized Papillary Thyroid Carcinoma in the United States (2000–2018)
Elisa Pasqual, Julie Ann Sosa, Yingxi Chen, Sara J. Schonfeld, Amy Berrington de González, Cari M. Kitahara
Thyroid.2022; 32(4): 397. CrossRef - Management of Low-Risk Thyroid Cancers: Is Active Surveillance a Valid Option? A Systematic Review of the Literature
Renato Patrone, Nunzio Velotti, Stefania Masone, Alessandra Conzo, Luigi Flagiello, Chiara Cacciatore, Marco Filardo, Vincenza Granata, Francesco Izzo, Domenico Testa, Stefano Avenia, Alessandro Sanguinetti, Andrea Polistena, Giovanni Conzo
Journal of Clinical Medicine.2021; 10(16): 3569. CrossRef - Cost-Effectiveness Analysis of Active Surveillance Compared to Early Surgery in Small Papillary Thyroid Cancer: A Systemic Review
Han-sang Baek, Chai-ho Jeong, Jeonghoon Ha, Ja-Seong Bae, Jeong-soo Kim, Dong-Jun Lim, Chul-Min Kim
Cancer Management and Research.2021; Volume 13: 6721. CrossRef - Active Surveillance as an Effective Management Option for Low-Risk Papillary Thyroid Microcarcinoma
Min Ji Jeon, Won Gu Kim, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Endocrinology and Metabolism.2021; 36(4): 717. CrossRef
- Active Surveillance for Low-Risk Thyroid Cancers: A Review of Current Practice Guidelines


 KES
KES



 First
First Prev
Prev



