Search
- Page Path
- HOME > Search
Original Articles
- Calcium & bone metabolism
- Protein Signatures of Parathyroid Adenoma according to Tumor Volume and Functionality
- Sung Hye Kong, Jeong Mo Bae, Jung Hee Kim, Sang Wan Kim, Dohyun Han, Chan Soo Shin
- Endocrinol Metab. 2024;39(2):375-386. Published online March 21, 2024
- DOI: https://doi.org/10.3803/EnM.2023.1827

- 404 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Parathyroid adenoma (PA) is a common endocrine disease linked to multiple complications, but the pathophysiology of the disease remains incompletely understood. The study aimed to identify the key regulator proteins and pathways of PA according to functionality and volume through quantitative proteomic analyses.
Methods
We conducted a retrospective study of 15 formalin-fixed, paraffin-embedded PA samples from tertiary hospitals in South Korea. Proteins were extracted, digested, and the resulting peptides were analyzed using liquid chromatography-tandem mass spectrometry. Pearson correlation analysis was employed to identify proteins significantly correlated with clinical variables. Canonical pathways and transcription factors were analyzed using Ingenuity Pathway Analysis.
Results
The median age of the participants was 52 years, and 60.0% were female. Among the 8,153 protein groups analyzed, 496 showed significant positive correlations with adenoma volume, while 431 proteins were significantly correlated with parathyroid hormone (PTH) levels. The proteins SLC12A9, LGALS3, and CARM1 were positively correlated with adenoma volume, while HSP90AB2P, HLA-DRA, and SCD5 showed negative correlations. DCPS, IRF2BPL, and FAM98A were the main proteins that exhibited positive correlations with PTH levels, and SLITRK4, LAP3, and AP4E1 had negative correlations. Canonical pathway analysis demonstrated that the RAN and sirtuin signaling pathways were positively correlated with both PTH levels and adenoma volume, while epithelial adherence junction pathways had negative correlations.
Conclusion
Our study identified pivotal proteins and pathways associated with PA, offering potential therapeutic targets. These findings accentuate the importance of proteomics in understanding disease pathophysiology and the need for further research.

- Hypothalamus and pituitary gland
- Clinical Characteristics, Diagnosis, and Treatment of Thyroid Stimulating Hormone-Secreting Pituitary Neuroendocrine Tumor (TSH PitNET): A Single-Center Experience
- Jung Heo, Yeon-Lim Suh, Se Hoon Kim, Doo-Sik Kong, Do-Hyun Nam, Won-Jae Lee, Sung Tae Kim, Sang Duk Hong, Sujin Ryu, You-Bin Lee, Gyuri Kim, Sang-Man Jin, Jae Hyeon Kim, Kyu Yeon Hur
- Endocrinol Metab. 2024;39(2):387-396. Published online February 5, 2024
- DOI: https://doi.org/10.3803/EnM.2023.1877

- 843 View
- 35 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Thyroid-stimulating hormone (TSH)-secreting pituitary neuroendocrine tumor (TSH PitNET) is a rare subtype of PitNET. We investigated the comprehensive characteristics and outcomes of TSH PitNET cases from a single medical center. Also, we compared diagnostic methods to determine which showed superior sensitivity.
Methods
A total of 17 patients diagnosed with TSH PitNET after surgery between 2002 and 2022 in Samsung Medical Center was retrospectively reviewed. Data on comprehensive characteristics and treatment outcomes were collected. The sensitivities of diagnostic methods were compared.
Results
Seven were male (41%), and the median age at diagnosis was 42 years (range, 21 to 65); the median follow-up duration was 37.4 months. The most common (59%) initial presentation was hyperthyroidism-related symptoms. Hormonal co-secretion was present in four (23%) patients. Elevated serum alpha-subunit (α-SU) showed the greatest diagnostic sensitivity (91%), followed by blunted response at thyrotropin-releasing hormone (TRH) stimulation (80%) and elevated sex hormone binding globulin (63%). Fourteen (82%) patients had macroadenoma, and a specimen of one patient with heavy calcification was negative for TSH. Among 15 patients who were followed up for more than 6 months, 10 (67%) achieved hormonal and structural remission within 6 months postoperatively. A case of growth hormone (GH)/TSH/prolactin (PRL) co-secreting mixed gangliocytoma-pituitary adenoma (MGPA) was discovered.
Conclusion
The majority of the TSH PitNET cases was macroadenoma, and 23% showed hormone co-secretion. A rare case of GH/TSH/PRL co-secreting MGPA was discovered. Serum α-SU and TRH stimulation tests showed great diagnostic sensitivity. Careful consideration is needed in diagnosing TSH PitNET. Achieving remission requires complete tumor resection. In case of nonremission, radiotherapy or medical therapy can improve the long-term remission rate.

- Adrenal Gland
- Clinical and Molecular Characteristics of PRKACA L206R Mutant Cortisol-Producing Adenomas in Korean Patients
- Insoon Jang, Su-jin Kim, Ra-Young Song, Kwangsoo Kim, Seongmin Choi, Jang-Seok Lee, Min-Kyeong Gwon, Moon Woo Seong, Kyu Eun Lee, Jung Hee Kim
- Endocrinol Metab. 2021;36(6):1287-1297. Published online December 2, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1217

- 3,890 View
- 127 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
An activating mutation (c.617A>C/p.Lys206Arg, L206R) in protein kinase cAMP-activated catalytic subunit alpha (PRKACA) has been reported in 35% to 65% of cases of cortisol-producing adenomas (CPAs). We aimed to compare the clinical characteristics and transcriptome analysis between PRKACA L206R mutants and wild-type CPAs in Korea.
Methods
We included 57 subjects with CPAs who underwent adrenalectomy at Seoul National University Hospital. Sanger sequencing for PRKACA was conducted in 57 CPA tumor tissues. RNA sequencing was performed in 13 fresh-frozen tumor tissues.
Results
The prevalence of the PRKACA L206R mutation was 51% (29/57). The mean age of the study subjects was 42±12 years, and 87.7% (50/57) of the patients were female. Subjects with PRKACA L206R mutant CPAs showed smaller adenoma size (3.3±0.7 cm vs. 3.8±1.2 cm, P=0.059) and lower dehydroepiandrosterone sulfate levels (218±180 ng/mL vs. 1,511±3,307 ng/mL, P=0.001) than those with PRKACA wild-type CPAs. Transcriptome profiling identified 244 differentially expressed genes (DEGs) between PRKACA L206R mutant (n=8) and wild-type CPAs (n=5), including five upregulated and 239 downregulated genes in PRKACA L206R mutant CPAs (|fold change| ≥2, P<0.05). Among the upstream regulators of DEGs, CTNNB1 was the most significant transcription regulator. In several pathway analyses, the Wnt signaling pathway was downregulated and the steroid biosynthesis pathway was upregulated in PRKACA mutants. Protein-protein interaction analysis also showed that PRKACA downregulates Wnt signaling and upregulates steroid biosynthesis.
Conclusion
The PRKACA L206R mutation in CPAs causes high hormonal activity with a limited proliferative capacity, as supported by transcriptome profiling.

Review Articles
- Adrenal Gland
- Adrenal Venous Sampling for Subtype Diagnosis of Primary Hyperaldosteronism
- Mitsuhide Naruse, Akiyo Tanabe, Koichi Yamamoto, Hiromi Rakugi, Mitsuhiro Kometani, Takashi Yoneda, Hiroki Kobayashi, Masanori Abe, Youichi Ohno, Nobuya Inagaki, Shoichiro Izawa, Masakatsu Sone
- Endocrinol Metab. 2021;36(5):965-973. Published online October 21, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1192
- 5,025 View
- 228 Download
- 7 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
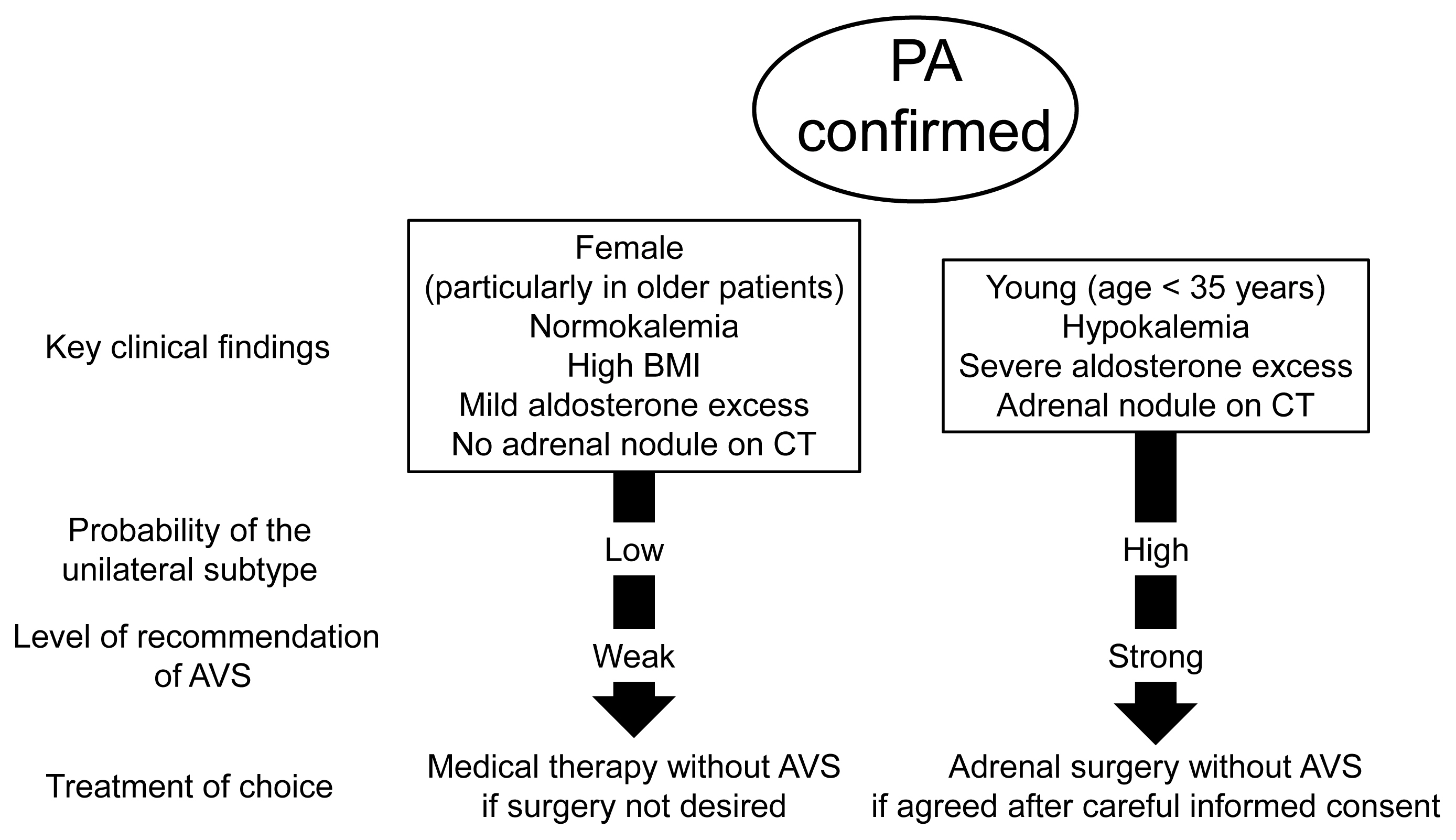
ePub - Adrenal venous sampling (AVS) is the key procedure for lateralization of primary hyperaldosteronism (PA) before surgery. Identification of the adrenal veins using computed tomography (CT) and intraoperative cortisol assay facilitates the success of catheterization. Although administration of adrenocorticotropic hormone (ACTH) has benefits such as improving the success rate, some unilateral cases could be falsely diagnosed as bilateral. Selectivity index of 5 with ACTH stimulation to assess the selectivity of catheterization and lateralization index (LI) >4 with ACTH stimulation for unilateral diagnosis is used in many centers. Co-secretion of cortisol from the tumor potentially affects the lateralization by the LI. Patients aged <35 years with hypokalemia, marked aldosterone excess, and unilateral adrenal nodule on CT have a higher probability of unilateral disease. Patients with normokalemia, mild aldosterone excess, and no adrenal tumor on CT have a higher probability of bilateral disease. Although no methods have 100% specificity for subtype diagnosis that would allow bypassing AVS, prediction of the subtype should be considered when recommending AVS to patients. Methodological standardization and strict indication improve diagnostic quality of AVS. Development of non-invasive imaging and biochemical markers will drive a paradigm shift in the clinical practice of PA.
-
Citations
Citations to this article as recorded by- A controlled trial of percutaneous adrenal arterial embolization for hypertension in patients with idiopathic hyperaldosteronism
Yaqiong Zhou, Xinquan Wang, Jixin Hou, Jindong Wan, Yi Yang, Sen Liu, Tao Luo, Qiting Liu, Qiang Xue, Peijian Wang
Hypertension Research.2024; 47(2): 311. CrossRef - Screening and diagnosis of primary aldosteronism. Consensus document of all the Spanish Societies involved in the management of primary aldosteronism
Marta Araujo-Castro, Jorge Gabriel Ruiz-Sánchez, Paola Parra Ramírez, Patricia Martín Rojas-Marcos, Almudena Aguilera-Saborido, Jorge Francisco Gómez Cerezo, Nieves López Lazareno, María Eugenia Torregrosa Quesada, Jorge Gorrin Ramos, Josep Oriola, Esteba
Endocrine.2024;[Epub] CrossRef - Diagnostic accuracy of using multiple cytokines to predict aldosterone-producing adenoma
Fei Qin, Hong Wen, Xiaoge Zhong, Yajin Pan, Xiaomei Lai, Tingting Yang, Jing Huang, Jie Yu, Jianling Li
Scientific Reports.2023;[Epub] CrossRef - A clinical assessment of portable point-of-care testing for quick cortisol assay during adrenal vein sampling
Ko Aiga, Mitsuhiro Kometani, Shigehiro Karashima, Seigo Konishi, Takuya Higashitani, Daisuke Aono, Xurong Mai, Mikiya Usukura, Takahiro Asano, Ayako Wakayama, Yuko Noda, Wataru Koda, Tetsuya Minami, Satoshi Kobayashi, Toshinori Murayama, Takashi Yoneda
Scientific Reports.2023;[Epub] CrossRef - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - Correlation of Histopathologic Subtypes of Primary Aldosteronism with Clinical Phenotypes and Postsurgical Outcomes
Chang Ho Ahn, You-Bin Lee, Jae Hyeon Kim, Young Lyun Oh, Jung Hee Kim, Kyeong Cheon Jung
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef - The Entity of Connshing Syndrome: Primary Aldosteronism with Autonomous Cortisol Secretion
Mara Carsote
Diagnostics.2022; 12(11): 2772. CrossRef
- A controlled trial of percutaneous adrenal arterial embolization for hypertension in patients with idiopathic hyperaldosteronism

- Adrenal gland
- The Genotype-Based Morphology of Aldosterone-Producing Adrenocortical Disorders and Their Association with Aging
- Xin Gao, Yuto Yamazaki, Yuta Tezuka, Kei Omata, Yoshikiyo Ono, Ryo Morimoto, Yasuhiro Nakamura, Fumitoshi Satoh, Hironobu Sasano
- Endocrinol Metab. 2021;36(1):12-21. Published online February 24, 2021
- DOI: https://doi.org/10.3803/EnM.2021.101
- 4,786 View
- 194 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
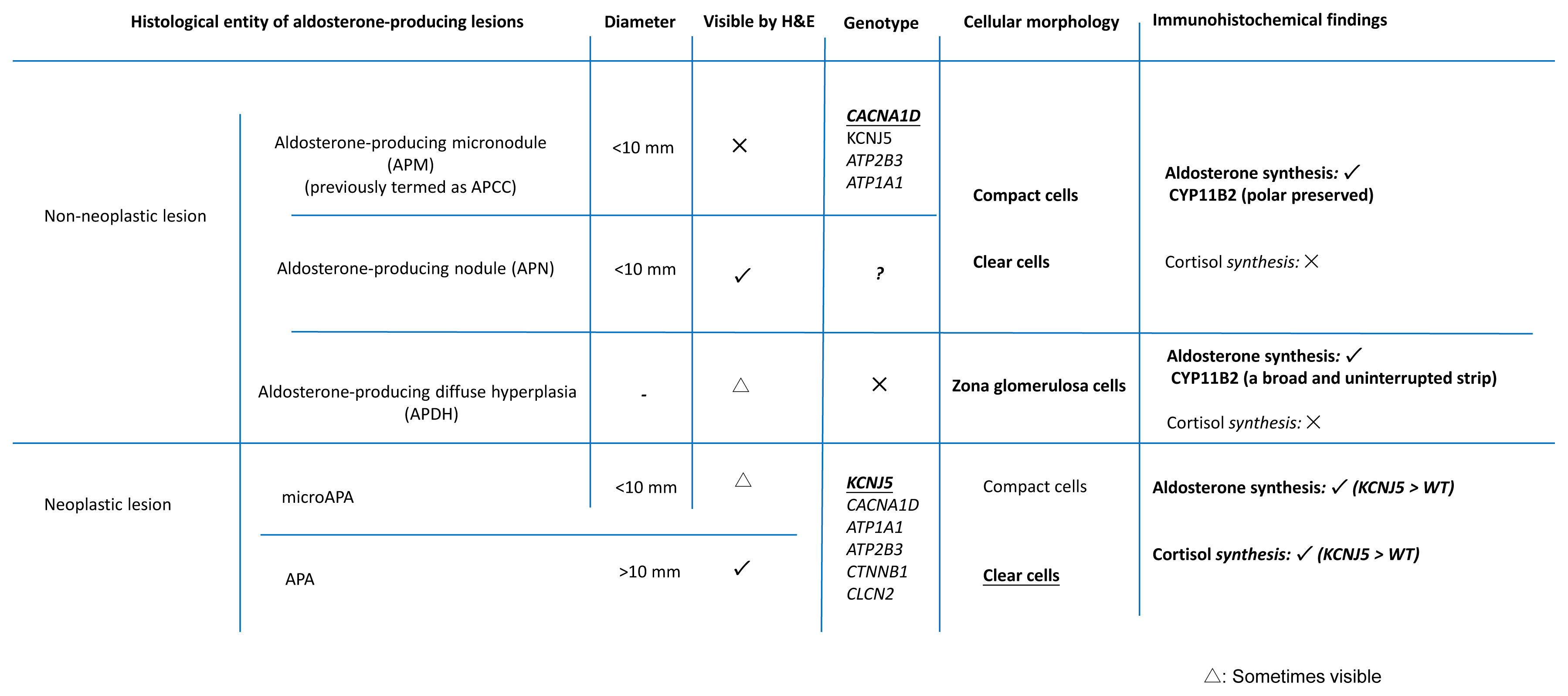
ePub - Primary aldosteronism (PA) is the most common cause of secondary hypertension, and is associated with an increased incidence of cardiovascular events. PA itself is clinically classified into the following two types: unilateral PA, mostly composed of aldosteroneproducing adenoma (APA); and bilateral hyperaldosteronism, consisting of multiple aldosterone-producing micronodules (APMs) and aldosterone-producing diffuse hyperplasia. Histopathologically, those disorders above are all composed of compact and clear cells. The cellular morphology in the above-mentioned aldosterone-producing disorders has been recently reported to be closely correlated with patterns of somatic mutations of ion channels including KCNJ5, CACNA1D, ATP1A1, ATP2B3, and others. In addition, in non-pathological adrenal glands, APMs are frequently detected regardless of the status of the renin-angiotensin-aldosterone system (RAAS). Aldosterone-producing nodules have been also proposed as non-neoplastic nodules that can be identified by hematoxylin and eosin staining. These non-neoplastic CYP11B2-positive nodules could represent possible precursors of APAs possibly due to the presence of somatic mutations. On the other hand, aging itself also plays a pivotal role in the development of aldosterone-producing lesions. For instance, the number of APMs was also reported to increase with aging. Therefore, recent studies indicated the novel classification of PA into normotensive PA (RAAS-independent APM) and clinically overt PA.
-
Citations
Citations to this article as recorded by- Subtype-specific Body Composition and Metabolic Risk in Patients With Primary Aldosteronism
Seung Shin Park, Chang Ho Ahn, Sang Wan Kim, Ji Won Yoon, Jung Hee Kim
The Journal of Clinical Endocrinology & Metabolism.2024; 109(2): e788. CrossRef - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - Correlation of Histopathologic Subtypes of Primary Aldosteronism with Clinical Phenotypes and Postsurgical Outcomes
Chang Ho Ahn, You-Bin Lee, Jae Hyeon Kim, Young Lyun Oh, Jung Hee Kim, Kyeong Cheon Jung
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef - Expression of CYP11B1 and CYP11B2 in adrenal adenoma correlates with clinical characteristics of primary aldosteronism
Chang Ho Ahn, Hee Young Na, So Yeon Park, Hyeong Won Yu, Su‐Jin Kim, June Young Choi, Kyu Eun Lee, Sang Wan Kim, Kyeong Cheon Jung, Jung Hee Kim
Clinical Endocrinology.2022; 96(1): 30. CrossRef - Pathology of Aldosterone Biosynthesis and its Action
Xin Gao, Yuto Yamazaki, Yuta Tezuka, Kei Omata, Yoshikiyo Ono, Ryo Morimoto, Yasuhiro Nakamura, Takashi Suzuki, Fumitoshi Satoh, Hironobu Sasano
The Tohoku Journal of Experimental Medicine.2021; 254(1): 1. CrossRef - Cellular Senescence in Adrenocortical Biology and Its Disorders
Xin Gao, Faping Li, Bin Liu, Yuxiong Wang, Yishu Wang, Honglan Zhou
Cells.2021; 10(12): 3474. CrossRef
- Subtype-specific Body Composition and Metabolic Risk in Patients With Primary Aldosteronism

Original Article
- Clinical Study
- Long-Term Results of Thermal Ablation of Benign Thyroid Nodules: A Systematic Review and Meta-Analysis
- Se Jin Cho, Jung Hwan Baek, Sae Rom Chung, Young Jun Choi, Jeong Hyun Lee
- Endocrinol Metab. 2020;35(2):339-350. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.339
- 10,859 View
- 306 Download
- 39 Web of Science
- 45 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Ultrasound-guided thermal ablations have become one of the main options for treating benign thyroid nodules. To determine efficacy of thermal ablation of benign thyroid nodules, we performed a meta-analysis of studies with long-term follow-up of more than 3 years.
Methods
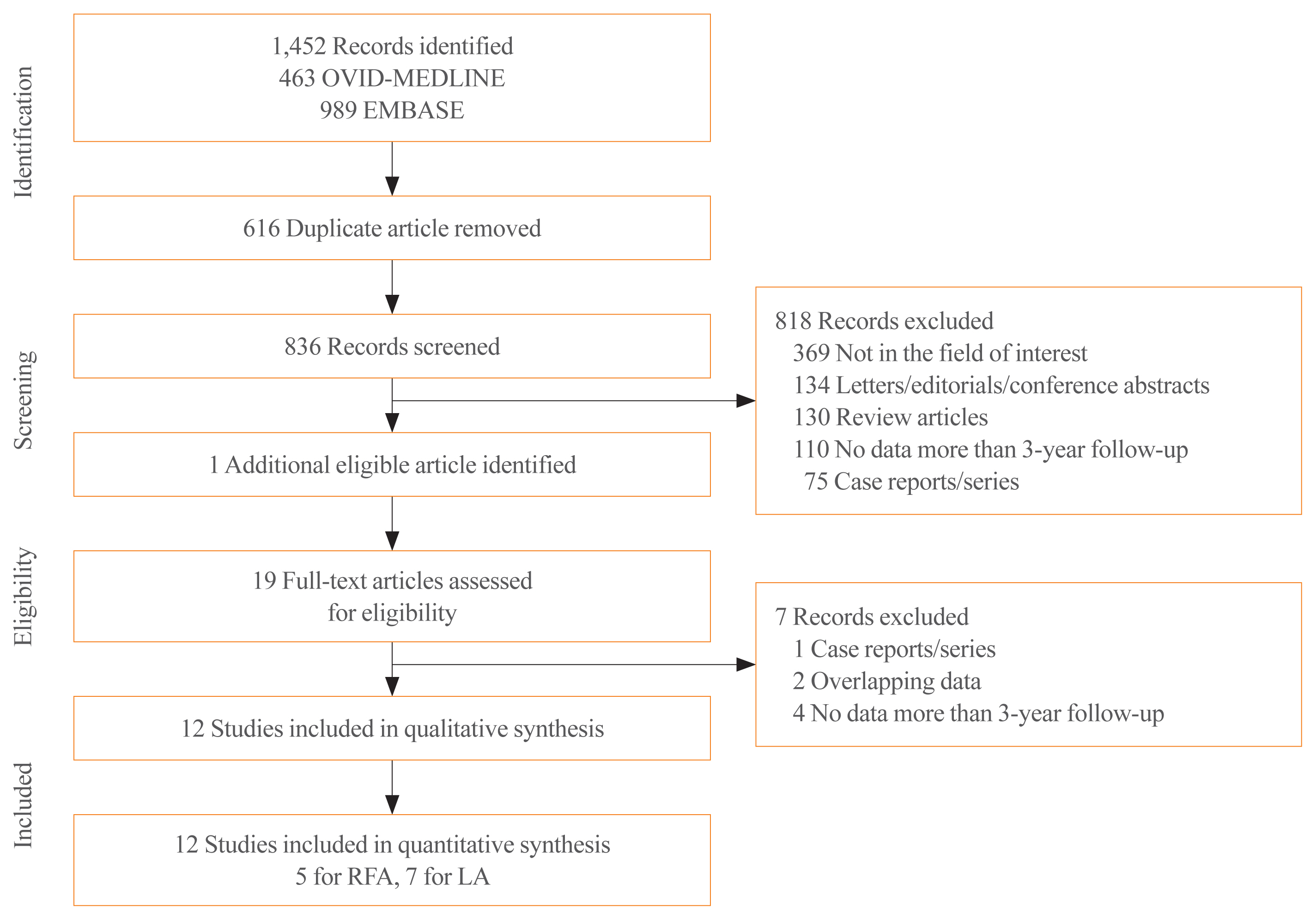
Databases were searched for studies published up to August 25, 2019, reporting patients with benign thyroid nodules treated with thermal ablation and with follow-up data of more than 3 years. Data extraction and quality assessment were performed according to PRISMA guidelines. The analysis yielded serial volume reduction rates (VRRs) of ablated nodules for up to 3 years or more, and adverse effect of ablation during follow-up. Radiofrequency ablation (RFA) and laser ablation (LA) were compared in a subgroup analysis.
Results
The pooled VRRs for ablated nodules showed rapid volume reduction before 12 months, a plateau from 12 to 36 months, and more volume reduction appearing after 36 months, demonstrating long-term maintenance of treatment efficacy. Thermal ablation had an acceptable complication rate of 3.8%. Moreover, patients undergoing nodule ablation showed no unexpected delayed complications during the follow-up period. In the subgroup analysis, RFA was shown to be superior to LA in terms of the pooled VRR and the number of patients who underwent delayed surgery.
Conclusion
Thermal ablations are safe and effective methods for treating benign thyroid nodules, as shown by a long follow-up analysis of more than 3 years. In addition, RFA showed superior VRRs compared with LA for the treatment of benign thyroid nodules, with less regrowth and less delayed surgery. -
Citations
Citations to this article as recorded by- Five-year follow-up results of thermal ablation for benign thyroid nodules: Systematic review and meta-analysis
Xidong Xu, Ying Peng, Guoxin Han
American Journal of Otolaryngology.2024; 45(1): 104025. CrossRef - Radiofrequency Ablation for Benign Nodules and for Cancer, Too?
Jonathon O. Russell, Kaitlyn M. Frazier
Otolaryngologic Clinics of North America.2024; 57(1): 83. CrossRef - An anthropomorphic thyroid phantom for ultrasound‐guided radiofrequency ablation of nodules
Tim Boers, Wyger Brink, Leonardo Bianchi, Paola Saccomandi, Johan van Hespen, Germen Wennemars, Sicco Braak, Michel Versluis, Srirang Manohar
Medical Physics.2024; 51(2): 826. CrossRef - The safety and efficacy of radiofrequency ablation in benign pediatric thyroid disease in the US: An initial case series
Grace S. Kim, Hilary Seeley, Julia Noel, Iram Ahmad, Kara Meister
Laryngoscope Investigative Otolaryngology.2024;[Epub] CrossRef - Radioiodine versus radiofrequency ablation to treat autonomously functioning thyroid nodules: a systematic review and comparative meta-analysis
Luca Giovanella, Maria Luisa Garo, Alfredo Campenní, Petra Petranović Ovčariček
European Journal of Nuclear Medicine and Molecular Imaging.2024;[Epub] CrossRef - Novel and Advanced Ultrasound Techniques for Thyroid Thermal Ablation
Wai-Kin Chan, Jui-Hung Sun, Miaw-Jene Liou, Chia-Jung Hsu, Yu-Ling Lu, Wei-Yu Chou, Yan-Rong Li, Feng-Hsuan Liu
Endocrinology and Metabolism.2024; 39(1): 40. CrossRef - Sublethal thermal stress promotes migration and invasion of thyroid cancer cells
Chi-Yu Kuo, Chung-Hsin Tsai, Jun Kui Wu, Shih-Ping Cheng, Yi-Hsien Hsieh
PLOS ONE.2024; 19(2): e0298903. CrossRef - The Role of Radiofrequency Ablation in Benign and Malignant Thyroid Nodules
Meghal Shah, Catherine McManus
Surgical Clinics of North America.2024;[Epub] CrossRef - Comparison of ultrasound-guided microwave ablation, laser ablation, and radiofrequency ablation for the treatment of elderly patients with benign thyroid nodules: A meta-analysis
Ying Qian, Zheng Li, Chunyun Fan, Yong Huang
Experimental Gerontology.2024; 191: 112425. CrossRef - Ultrasound imaging in thyroid nodule diagnosis, therapy, and follow‐up: Current status and future trends
Tim Boers, Sicco J. Braak, Nicole E. T. Rikken, Michel Versluis, Srirang Manohar
Journal of Clinical Ultrasound.2023; 51(6): 1087. CrossRef - Ultrasound (US)-Guided Ablation of Thyroid Nodules
Byung Seup Kim
Journal of Surgical Ultrasound.2023; 10(1): 14. CrossRef - Ultrasound-Guided Radiofrequency Ablation versus Thyroidectomy for the Treatment of Benign Thyroid Nodules in Elderly Patients: A Propensity-Matched Cohort Study
L. Yan, X.Y. Li, Y. Li, Y. Luo
American Journal of Neuroradiology.2023; 44(6): 693. CrossRef - Minimally Invasive Ablative Treatments for Benign Thyroid Nodules: Current Evidence and Future Directions
Enrico Papini, Laszlo Hegedüs
Thyroid®.2023; 33(8): 890. CrossRef - Influence factors and nomogram for volume reduction rate in benign thyroid nodule after thermal ablation
Shiliang Cao, Lijia Wang, Ying Wei, Zhenlong Zhao, Jie Wu, Mingan Yu
International Journal of Hyperthermia.2023;[Epub] CrossRef - Choice in Ablative Therapies for Thyroid Nodules
Q Lina Hu, Jennifer H Kuo
Journal of the Endocrine Society.2023;[Epub] CrossRef - 2022 Taiwan clinical multicenter expert consensus and recommendations for thyroid radiofrequency ablation
Wei-Che Lin, Wen-Chieh Chen, Pei-Wen Wang, Yi-Chia Chan, Yen-Hsiang Chang, Harn-Shen Chen, Szu-Tah Chen, Wei-Chih Chen, Kai-Lun Cheng, Shun-Yu Chi, Pi-Ling Chiang, Chen-Kai Chou, Feng-Fu Chou, Shun-Chen Huang, Feng-Hsuan Liu, Sheng-Dean Luo, Fen-Yu Tseng,
Ultrasonography.2023; 42(3): 357. CrossRef - Comparison of the Efficiency of Radiofrequency and Microwave Ablation Methods in the Treatment of Benign Thyroid Nodules
Mahi N. Cerit, Cem Yücel, Ethem T. Cerit, Mehmet M. Yalçın, Halit N. Şendur, Suna Ö. Oktar
Academic Radiology.2023; 30(10): 2172. CrossRef - Radiofrequency ablation for autonomously functioning nodules as treatment for hyperthyroidism: subgroup analysis of toxic adenoma and multinodular goitre and predictors for treatment success
M. M. D. van der Meeren, F. B. M. Joosten, S. H. P. P. Roerink, L. N. Deden, W. J. G. Oyen
European Journal of Nuclear Medicine and Molecular Imaging.2023; 50(12): 3675. CrossRef - Massive Hemorrhage and Mortality Following Thyroid Radiofrequency Ablation
Seulki Song, Jin Pyeong Kim
Ear, Nose & Throat Journal.2023;[Epub] CrossRef - Clinical Approach for Thyroid Radiofrequency Ablation
Jung Suk Sim
Journal of the Korean Society of Radiology.2023; 84(5): 1017. CrossRef - General Principles for the Safe Performance, Training, and Adoption of Ablation Techniques for Benign Thyroid Nodules: An American Thyroid Association Statement
Catherine F. Sinclair, Jung Hwan Baek, Kathleen E. Hands, Steven P. Hodak, Timothy C. Huber, Iram Hussain, Brian Hung-Hin Lang, Julia E. Noel, Maria Papaleontiou, Kepal N. Patel, Gilles Russ, Jonathon Russell, Stefano Spiezia, Jennifer H. Kuo
Thyroid®.2023; 33(10): 1150. CrossRef - A comprehensive review of interventional ablation techniques for the management of thyroid nodules and metastatic lymph nodes
Jennifer H. Kuo, Catherine F. Sinclair, Brian Lang, Stefano Spiezia, Mingan Yu, Eun Ju Ha, Dong Gyu Na, Chiara Offi, Kepal N. Patel, Jung Hwan Baek
Surgery.2022; 171(4): 920. CrossRef - Radiofrequency ablation and related ultrasound‐guided ablation technologies for treatment of benign and malignant thyroid disease: An international multidisciplinary consensus statement of the American Head and Neck Society Endocrine Surgery Section with
Lisa A. Orloff, Julia E. Noel, Brendan C. Stack, Marika D. Russell, Peter Angelos, Jung Hwan Baek, Kevin T. Brumund, Feng‐Yu Chiang, Mary Beth Cunnane, Louise Davies, Andrea Frasoldati, Anne Y. Feng, Laszlo Hegedüs, Ayaka J. Iwata, Emad Kandil, Jennifer K
Head & Neck.2022; 44(3): 633. CrossRef - Assessment of thyroid-specific quality of life in patients with benign symptomatic thyroid nodules treated with radiofrequency or ethanol ablation: a prospective multicenter study
So Yeong Jeong, Eun Ju Ha, Jung Hwan Baek, Tae Yong Kim, Yu-Mi Lee, Jeong Hyun Lee, Jeonghun Lee
Ultrasonography.2022; 41(1): 204. CrossRef - Thyroid Nodule Radiofrequency Ablation: Complications and Clinical Follow Up
James Y. Lim, Jennifer H. Kuo
Techniques in Vascular and Interventional Radiology.2022; 25(2): 100824. CrossRef - Radiofrequency Ablation of Solid, Non-Functional Thyroid Nodules
Michael Douek
Techniques in Vascular and Interventional Radiology.2022; 25(2): 100821. CrossRef - Efficacy and Safety of Thermal Ablation for Treating Lymph Node Metastasis From Papillary Thyroid Carcinoma: A Systematic Review and Meta-Analysis
Zheng Ding, Juan Chen, Zhiguang Chen, Xiaoke Zeng, Pengchao Zheng, Xuemei Wang, Xinwu Cui, Liang Sang
Frontiers in Oncology.2022;[Epub] CrossRef - Intraoperative Neuromonitoring: Evaluating the Role of Continuous IONM and IONM Techniques for Emerging Surgical and Percutaneous Procedures
Catherine McManus, Jennifer Hong Kuo
Frontiers in Endocrinology.2022;[Epub] CrossRef - Thermal Ablation for the Management of Papillary Thyroid Microcarcinoma in the Era of Active Surveillance and Hemithyroidectomy
Sae Rom Chung, Jung Hwan Baek, Young Jun Choi, Jeong Hyun Lee
Current Oncology Reports.2022; 24(8): 1045. CrossRef - enhanced anarchic society optimization technique for the classification of ultrasound thyroid images using ILBP
D. Anitha, S. Sathya Priya
International journal of health sciences.2022; : 4713. CrossRef - Image-Guided Percutaneous Ablation for Primary and Metastatic Tumors
Arian Mansur, Tushar Garg, Apurva Shrigiriwar, Vahid Etezadi, Christos Georgiades, Peiman Habibollahi, Timothy C. Huber, Juan C. Camacho, Sherif G. Nour, Alan Alper Sag, John David Prologo, Nariman Nezami
Diagnostics.2022; 12(6): 1300. CrossRef - Efficacy and safety of ultrasound-guided microwave ablation versus surgical resection for Bethesda category IV thyroid nodules: A retrospective comparative study
Jingjing Yang, Ya Zhang, Xingjia Li, Yueting Zhao, Xue Han, Guofang Chen, Xiaoqiu Chu, Ruiping Li, Jianhua Wang, Fei Huang, Chao Liu, Shuhang Xu
Frontiers in Endocrinology.2022;[Epub] CrossRef - Long-term follow-up of the radiofrequency ablation of benign thyroid nodules: the value of additional treatment
Hyun Jin Kim, Jung Hwan Baek, Woojin Cho, Jung Suk Sim
Ultrasonography.2022; 41(4): 661. CrossRef - Das „heiße“ Schilddrüsenkarzinom mit einem kritischen Blick auf die Thermoablation
Joachim Jähne, Andreas Niesen, Joachim Bernhardts, Marija Hillemans
Der Chirurg.2021; 92(1): 34. CrossRef - Current Practice of Percutaneous Ablation Technologies for Thyroid Nodules 2020
Haris Muhammad, Jonathon O. Russell, Prasanna Santhanam, Aniqa Tehreem, Ralph P. Tufano
Current Otorhinolaryngology Reports.2021; 9(1): 52. CrossRef - RFA and benign thyroid nodules: Review of the current literature
Haris Muhammad, Prasanna Santhanam, Jonathon O. Russell, Jennifer H. Kuo
Laryngoscope Investigative Otolaryngology.2021; 6(1): 155. CrossRef - Thermal Treatment Options for Benign Thyroid Nodules—The Role of Radio-Frequency Ablation and Laser Therapy
Erivelto Volpi
Clinical Thyroidology.2021; 33(1): 17. CrossRef - Comparative efficacy of different ultrasound-guided ablation for the treatment of benign thyroid nodules: Systematic review and network meta-analysis of randomized controlled trials
Linye He, Wanjun Zhao, Zijing Xia, Anping Su, Zhihui Li, Jingqiang Zhu, Ivan D. Florez
PLOS ONE.2021; 16(1): e0243864. CrossRef - Unresolved Clinical Issues in Thermal Ablation of Benign Thyroid Nodules: Regrowth at Long-Term Follow-Up
Jung Suk Sim, Jung Hwan Baek
Korean Journal of Radiology.2021; 22(8): 1436. CrossRef - Current Status and Challenges of US-Guided Radiofrequency Ablation of Thyroid Nodules in the Long Term: A Systematic Review
Stella Bernardi, Andrea Palermo, Rosario Francesco Grasso, Bruno Fabris, Fulvio Stacul, Roberto Cesareo
Cancers.2021; 13(11): 2746. CrossRef - Update of Radiofrequency Ablation for Treating Benign and Malignant Thyroid Nodules. The Future Is Now
Ralph P. Tufano, Pia Pace-Asciak, Jonathon O. Russell, Carlos Suárez, Gregory W. Randolph, Fernando López, Ashok R. Shaha, Antti Mäkitie, Juan P. Rodrigo, Luiz Paulo Kowalski, Mark Zafereo, Peter Angelos, Alfio Ferlito
Frontiers in Endocrinology.2021;[Epub] CrossRef - Factors Associated with the Efficacy of Radiofrequency Ablation in the Treatment of Benign Thyroid Nodules
Huynh Q Khanh, Nguyen L Vuong, Tran Q Tien
World Journal of Endocrine Surgery.2021; 12(3): 117. CrossRef - Long-Term Outcomes of Thermal Ablation for Benign Thyroid Nodules: The Issue of Regrowth
Jung Suk Sim, Jung Hwan Baek, Rosaria Meccariello
International Journal of Endocrinology.2021; 2021: 1. CrossRef - Matrix 3D ultrasound-assisted thyroid nodule volume estimation and radiofrequency ablation: a phantom study
T. Boers, S. J. Braak, M. Versluis, S. Manohar
European Radiology Experimental.2021;[Epub] CrossRef - Learning curve analysis of radiofrequency ablation for benign thyroid nodules
Chi-Yu Kuo, Chien-Liang Liu, Chung-Hsin Tsai, Shih-Ping Cheng
International Journal of Hyperthermia.2021; 38(1): 1536. CrossRef
- Five-year follow-up results of thermal ablation for benign thyroid nodules: Systematic review and meta-analysis

Case Reports
- A Case of Adrenocortical Adenoma Associated with Incidental Pheochromocytoma.
- Sung Jun Hong, Young Sik Choi, Yo Han Park, Byung Cheol Yoon, Young Hwan Bae, Seon Ja Park, Ja Young Koo
- J Korean Endocr Soc. 1996;11(4):531-537. Published online November 7, 2019
- 1,183 View
- 44 Download
-
 Abstract
Abstract
 PDF
PDF - The coexistence of adrenal cortical tumor and pheochromocytoma was extremely rare. A total of 25 reported cases showing evidence of hyperfuction of the adrenal cortex and pheochromocytoma were noted in the literature. Of those twenty cases were coexistence of pheochromocytoma and adrenocortical hyperplasia and only five cases were coincident pheochromocytoma and adreno-cortical adenoma. Recently, we experienced a case of adrenocortical adenoma associated with incidental pheochrmocytoma. A 55-year-old woman complained of progressive weight gain and epigastric discomfort. Hormonal and radiologic studies revealed Cushings syndrome with a left adrenal tumor. Adrenalectomy was performed and the gland actually had two nodules on its surface, one pheochromocytoma and the other cortical adenoma. This patient was the first case of pheochromocytoma with adrenocortical adenoma in Korea. We report the case with a review of literature.

- A Case of Giant Adrenal Adenoma Presenting Primary Aldosteronism.
- Ji Hyun Lee, Bong Soo Cha, Moon Suk Nam, Young Duk Song, Sung Kil Lim, Hyun Chul Lee, Kap Bum Huh, Hyung Chan Suh, Young Hwa Choi, Jae Min Park, Jung Soo Park, Soon Won Hong, Dong Hwan Shin
- J Korean Endocr Soc. 1996;11(3):348-354. Published online November 7, 2019
- 1,290 View
- 25 Download
-
 Abstract
Abstract
 PDF
PDF - Primary aldosteronism is a syndrome chracterized by hypokalemic alkalosis and hypertension. Small sized adrenal cortical adenomas have been the major cause of this syndrome in most of the patients. However, if the adrenal mass is larger than 6cm in diameter and with irregular consistency, malignancy is more favored. We experienced a patient who had a giant adrenal adenoma with primary aldosteronism. A 24-year-old female presented with hypertension, hypokalemia, low plasma renin, and high plasrna aldosterone levels, was found to have a 6×5.5×5 cm sized left adrenal tumor by MRI. Her clinical laboratory feature did not revealed any evidence of Cushing's syndrome or pheochromocytoma. Preoperatively adrenal carcinoma presenting pure adrenal aldosteronism was suspected due to large size and heterogenous signal character of the adrenal mass in radiologic study. At operation well encapsulated, round giant adrenal tumor weighing 65gm(4.5×4×4 cm) was removed. There was no evidence of metastasis with return of adrenal function to normal after surgery. Benign adrenal adenoma was confirmed by the gross morphology and the histologic features.

- A Case of Mediastinal parathyroid adenoma localized by technetium-99m sestamibi scanning.
- Bong Yun Cha, Kwang Woo Lee, Ho Young Son, Sung Koo Kang, Ki Ho Song, Sung Hee Lee, Won Hee Han, Hyung Sun Sohn
- J Korean Endocr Soc. 1996;11(2):227-232. Published online November 7, 2019
- 1,019 View
- 22 Download
-
 Abstract
Abstract
 PDF
PDF - We present a patient with primary hyperparathyroidism in whom preoperative Tc-99m sestarnibi scanning cleary demonstrated mediastinal parathyroid adenoma. After resectian of tumor through median sternotomy, he was restored to the normocalcemia. This case suggests that Tc-99m sestamibi scanning may be a useful method in the preoperative localization of mediastinal parathyroid adenoma.

- A Case of Pituitary Feedback Adenoma Caused by Primary Hypothyroidism.
- Soon Jib Yoo, Sang A Chang, Yoo Bae Ahn, Hyun Sik Son, Kun Ho Yoon, Moo Il Kang, Bong Yun Cha, Kwang Woo Lee, Ho Young Son, Sung Koo Kang, Myung Hee Chung
- J Korean Endocr Soc. 1996;11(2):199-206. Published online November 7, 2019
- 1,154 View
- 29 Download
-
 Abstract
Abstract
 PDF
PDF - A 14-year-old girl presented with severe headache and grand mal seizure. A magnetic resonance imaging(MRI) of brain showed a pituitary mass(1.0X1.5X1.3cm) incidentally during seizure evaluation. On physical examination, nodular goiter was detected on her anterior neck. The hormone study showed markdly increased basal thyroid stimulating hormone(TSH) level compared to thyroid hormone level, hyperprolactinemia and decreased basal growth hormone level. TSH and prolactin showed exaggerated response to thyrotropin releasing hormone(TRH) and the growth hormone showed delayed and blunted response to insulin-induced hypoglycemia. With the results of thyroid autoantibody and thyroid scan, the diagnosis of Hashimoto's thyroiditis was possible. Thyroid hormone and anticonvulsant drug were started with close observation of clinical status under the impression of pituitary feedback adenoma caused by hypothyroidism. After 3 months replacement therapy of levothyroxine sodium, she achieved euthyroid state with disappearance of headache and nodular goiter. After continuous replacement therapy for 9 months more, the pituitary mass was successfully regressed on follow up MRI with normalization of basal prolactin level. Grand mal seizure was developed after withholding anticonvulsant drug even though continuous admmistration of thyroid hormone. Because of similarity among pituitary adenoma discovered incidentally, careful hormonal study and high index of suspicion should be maintained to achieve correct diagnosis in order to avoid unnecessary pituitary surgery in these patients.

- A Case of True Precocious Puberty Associated with Pituitary Microadenoma Treated with LHRH Agonist.
- In Kyu Lee, Soon Woo Kim, Heung Sik Kim, Chin Moo Kang
- J Korean Endocr Soc. 1994;9(3):244-250. Published online November 6, 2019
- 1,194 View
- 49 Download
-
 Abstract
Abstract
 PDF
PDF - Recently Brain CT and MRI have greatly contributed to the discovery of intracranial tumors including cysts which cause precocious puberty. Among many precocious pubetry patients that had previously been diagnosed as idopathic, a number of cases turn out the true precocious puberty caused by intracranial lesion.Authors experienced a case of true precocious puberty in a seven year old female whose vaginal bleeding appeared at age of five and she also had breast enlargement on admission. Pituitary microadenoma was found on her brain MRI and the microadenoma turned to be nonfunctional on hormonal tests.Following three does of decapety1-CR(LHRH Agonist), the vaginal bleeding was ceased and the deceleration of breast enlargement was noted. Her growth velocity was also affected but the further observation for final height would be warranted.

Original Articles
- A Clinical Observation of Endocrine Adrenal Tumors.
- Hye Young Park, Tae Suk Kim, Soo Jin Lee, Dong Gu Choi, Moon Ho Kang
- J Korean Endocr Soc. 1994;9(3):228-238. Published online November 6, 2019
- 1,082 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - Endocrine adrenal tumors are uncommon but clinically significant because they can be managed successfully by surgical therapy. During pregnancy, adrenal tumors can be a cause of death for both mother and baby, unless they diagnoses antenatally and managed properly. To investigate clinical characteristics of endocrine adrenal tumors, we analyzed 26 cases of adrenal tumor diagnosed and managed in Chung Ang Gil Hospital including cases associated with pregnancy and also a rare case of paraganglioma in liver. 1) There were 7 cases of Cushing's syndrome among which two cases were due to Cushing's disease and five cases were due to adrenal adenoma. Six cases were managed successfully by appropriate surgery. Another one case was associated with pregnancy but the patient expired due to sudden development of pulmonary edema and hypotension during preoperative preparation.2) Among 9 cases of primary aldosteronism, 8 cases were aldosterone-producing adenoma(APA) and 1 case was idiopathic hyperaldosteronism(IHA). In differential diagnosis between APA and IHA, diagnostic accuracy of postural study and adrenal CT was 86%, 78% respectively. In each one case of APA and IHA, adrenal venous aldosterone sampling was used for the differential diagnosis. Six cases of APA were managed by appropriate surgery. One patient with APA who refuses surgery and one patient with IHA were placed on spironolactone with good response.3) Among 10 cases of pheochromocytoma, seven cases were from adrenal gland and three cases were paragangliomas including one case originating from liver and two cases from abdominal ganglia. One patient with pheochromocytoma was diagnosed in 1st trimester of pregnancy and she was successfully treated by surgery.We observed 26 cases of endocrine adrenal tumors which were successfully managed except one case. We think that it is important to pay attention to adrenal tumor for early diagnosis particulary when associated with pregnancy. Paraganglioma in liver, although very rare, should be included in the differential diagnosis of space occupying lesion in liver.

- Endocrinological and Morphological Characteristics of Clinically Nonfunctioning Pituitary Adenoma.
- Jae Wha Jo, Moon Suk Nam, Hyun Chul Lee, Tae Seung Kim, Kyu Chang Lee, Hyun Joo Jung
- J Korean Endocr Soc. 1994;9(3):200-212. Published online November 6, 2019
- 1,136 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - Forth-nine patients with clinically nonfunctioning pituitary adenomas were evaluated clinically, endocrinologically and morphologically in this study.The results obtained were as follows.1) The mean age was 47.1 years(range 23 to 76 years), and 22 were male(44.9%) and 27(55.1%) female.2) The major clinical manifestations of male patients were visual disturbance(72.7%), headache(54.5%), loss of libido(45.5%), but those of female visual disturbance(59.6%), headache(48.1%), amenorrhea(48.1%), loss of body hair(25.9%), and galactorrhea(22.2%).3) All were macroadenomas evaluated by CT scan, and in the male patients 16(72.7%) were grade III and 6(27.3%) grade IV by Hardy classification, and in the female patients 6(22.2%) were grade II, 12(44.4%) grade III, and 9(33.3%) grade IV.4) The elevation of serum prolactin were observed 7(31.8%) out of male, and 24(88.9%) of female.5) Combined stimulation test revealed that GH insufficiency was 89.6%, ACTH 58.9%, LH 58.7%, FSH 51.1 %, and TSH 50.0% and hormone insufficiency more than 4 pituitary hormone was 54.2%.6) Prolactin response to TRH decreased in 12(70.6%) of 17 patients with normal basal prolactin, and 19(76.0%) of 25 with elevated prolactin.7) Immunohistochemistry revealed that null cell adenoma was 57.1%, gonadotrope adenoma 26.5%, plurihormonal adenoma 8.0%, silent corticotrope adenoma 4.0%, thyrotrope adenoma(2.0%), and lactotrope adenoma(2.0%).8) The ultrastructural characteristics examined by electron-microscopy were similar despite of immunohistochemical differences.In summary, the prevalance of clinically nonfunctioning pituitary adenoma was middle aged men and women, and their main symptoms were visual disturbance and headache. Hyperprolactinemia and pituitary hormone insufficiency more than 4 hormone were observed commonly. Most of them were null cell adenoma and gonadotrope adenoma examined by immunohistochemistry. Further study using modern techniques: cell culture, subunit-immunostaining. And Northern blot analysis of mRNA for pituitary hormone or subunit, will be needed to clarify null cell adenomas.

Case Report
- A Case of Thyrotropin - Secreting Pituitary Adenoma.
- Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee, Chang Soon Koh, Woon Bae Kim, Hye Young Park, Jin Sung Kim
- J Korean Endocr Soc. 1994;10(2):153-160. Published online November 6, 2019
- 1,242 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - thyrotropin-secreting(TSH) pituitary adenoma is extremely rare condition causing hyperthyroidism by uncontrolled secretion of thyrotropin. Among total pituitary adenomas, less than 1 percent are thyrotropin-secreting type, and only about 150 cases have been reported till now. However, increasing numbers of cases are being found due to the availability of ultra-sensitive TSH assay. We report here a patient with thyrotropin-secreting pituitay adenoma secreting TSH with production of lutenizing hormone(LH), follicle stimulating hormone(FSH), growth hormone(GH), prolactin(PRL) and free alpha-subunit.A 21-years old man visited thyroid clinic because of palpitation and dyspnea on exertion. He had diffuse goiter and features of mild thyrotoxicosis, and his thyroid function test showed increased T3, T4 and normal TSH. Serum free alpha-subunit concentration was 7420.5pg/ml(24.7mIU/ml) and the molar ratio of free alpha-subunit to TSH was 15.9. Basal pituitary hormone levels except TSH and the response to combined pituitary stimulation test were normal. A large sellar mass extending into frontal lobe was found on sellar MRI, so it was removed surgically leaving residual tumor mass due to the extensive nature of tumor. In immunohistochemical study the tumor tissue was stained with antibodies to TSH, LH, FSH, GH and PRL. His hyperthyroidism and goiter disappeared after partial removal of tumor. Somatostatin analogue(octreotide acetate) were given continuously via subcutaneous route(150 ug/day) using infusion pump to reduce the size of residual tumor. After 4 months of octreotide infusion, the size of tumor decreased slightly, and he is under treatment without any side effect.

Review Article
- 10 Years Prospective Study for the Surgical Total Removal of Pituitary Tumor; Preliminary Report - 2, 5 Years Follow Up.
- Eun Jig Lee, Sung Kil Lim, Kap Bum Huh, Sun Ho Kim, Dong Ik Kim, Byung Hee Lee, Ju Heon Yoon, Su Yeon Choi, Joong Uhn Choi, Sang Seop Chung, Kyu Chang Lee
- J Korean Endocr Soc. 1994;10(2):85-94. Published online November 6, 2019
- 967 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - The goal of the pituitary tumor surgery is restoration of the normal endocrine function and releaving the pressure effects of the tumor mass on the adjacent neural structures. The authors had proceeded with the 10 years prospective follow-up study for the endocrine function and recurrence of pituitary tumor in the patients who received the complete total resection of tumor mass by the means of total capsulectomy.The authors will discuss the preliminary result of 2.5 years follow-up of this study.


 KES
KES

 First
First Prev
Prev



