Search
- Page Path
- HOME > Search
- Thyroid
- Thyroid Hormone Reference Intervals among Healthy Individuals In Lanzhou, China
- Yan Lu, Wen-Xia Zhang, De-Hong Li, Lian-Hua Wei, Yu-Jun Zhang, Fu-Na Shi, Shen Zhou
- Endocrinol Metab. 2023;38(3):347-356. Published online June 14, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1638
- 2,064 View
- 121 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The common reference intervals (RIs) for thyroid hormones currently used in China are provided by equipment manufacturers. This study aimed to establish thyroid hormone RIs in the population of Lanzhou, a city in the subplateau region of northwest China, and compare them with previous reports and manufacturer-provided values.
Methods
In total, 3,123 individuals (1,680 men, 1,443 women) from Lanzhou, an iodine-adequate area of China, perceived as healthy were selected. The Abbott Architect analyzer was used to determine the serum concentration of thyroid hormones. The 95% RI was estimated using the 2.5th and 97.5th percentiles as the lower and upper reference limits, respectively.
Results
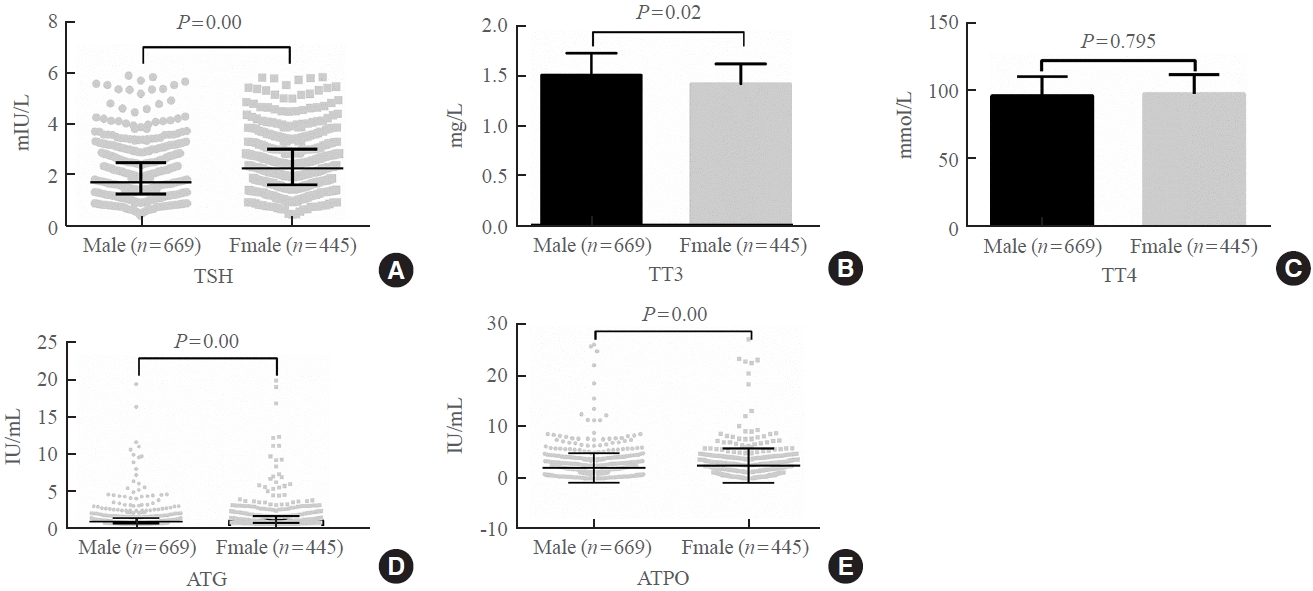
The serum levels of thyroid-stimulating hormone (TSH), total triiodothyronine (TT3), antithyroglobulin (ATG) antibody, and antithyroid peroxidase (ATPO) antibody levels were significantly correlated with sex (P<0.05). TSH, total thyroxine (TT4), and ATPO levels were significantly correlated with age (P<0.05). The serum levels of TSH, ATG, and ATPO in men were significantly lower than in women; in contrast, the serum TT3 level was significantly higher in men than in women (P<0.05). Serum TSH, TT3, TT4, and ATG levels differed across age groups (P<0.05), but no such variation was observed for ATG levels (P>0.05). The established RIs of TSH, ATG, and ATPO in this study differed between sexes (P<0.05). The thyroid hormone RIs established herein were inconsistent with the manufacturer-provided values.
Conclusion
The RIs of thyroid hormones in the healthy population of Lanzhou were inconsistent with those in the manufacturer’s manual. Validated sex-specific values are required for diagnosing thyroid diseases. -
Citations
Citations to this article as recorded by- Burden of non-alcoholic fatty liver disease in subclinical hypothyroidism
Mahmood Dhahir Al-Mendalawi
Journal of Clinical and Scientific Research.2024; 13(1): 68. CrossRef
- Burden of non-alcoholic fatty liver disease in subclinical hypothyroidism

- Thyroid
- Best Achievements in Translational and Basic Thyroidology in 2020
- Sun Wook Cho, Young Joo Park
- Endocrinol Metab. 2021;36(1):36-40. Published online February 24, 2021
- DOI: https://doi.org/10.3803/EnM.2021.104
- 3,296 View
- 138 Download
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - This review discusses articles published in 2020 that presented noteworthy achievements in translational and basic thyroidology. Previously unresolved questions about thyroid hormone receptor actions and signaling mechanisms were answered using various novel in vitro and in vivo models. Using high resolution cryo-electron microscopy, the fine functional structure of thyroglobulin was demonstrated, and new insights into the pathogenesis of thyroid disease were achieved, with a focus on research into thyroid-disrupting chemicals and the gut microbiome. Novel therapeutic approaches were tried in the field of advanced thyroid cancer treatments.

- The Effect of Methimazole on the Thyroglobulin Synthesis in Cultured Porcine Thyroid Cells.
- Eun Jig Lee, Hyun Chul Lee, Kap Bum Huh, Kyung Rae Kim, Sung Kil Lim, Kyung Mi Lee
- J Korean Endocr Soc. 1994;9(4):332-336. Published online November 6, 2019
- 1,148 View
- 25 Download
-
 Abstract
Abstract
 PDF
PDF - The thioureylene drugs, propylthiouracil and methylmercaptoimidazol(MMI), exert their antithyroid effect primarily through inhibition of thyroid peroxidase-catalyzed iodination of thyroglobulin. Recently the interest about the effect to the thyroglobulin synthesis of these drugs have been increasing. So we studied the MMI effect to the thyroglobulin synthesis in cultured porcine thyroid cells. Porcine thyroid cells were isolated by sequential trypsinization in the presence of EGTA, seeded at high density(1X10^6 cells/cm^2) and cultured. One week later, MMI was added in different concentrations(0, 0.2, 1, 5mM) with TSH only or with 4H(b-TSH, Insulin, Transferrin, Hydrocortisone) or without hormone. Medias were collected after 24 hours and compared the amount of thyroglobulin secreted. And also pulse-labeling were performed with S^35 cysteine/methionine(1-2uCi/well) for 30, 60, 90min at the same conditions.There was no significant change in the amount of the secreted thyroglobulin by MMI, and there was no significant change in the pulse-labeled interacellular thyroglobulin by MMI. And also there was no significant change in the secretion of TSH-stimulated thyroglobulin by MMI. So we conclude that MMI has no effect on the thyroglobulin synthesis in cultured porcine thyroid cells and also MMI has no effect on the TSH-stimulated thyroglobulin synthesis in cultured porcine thyroid cell.

- The Effect of Iodine on the thyroglobulin Synthesis in Cultured Porcine Thyroid Cells.
- Eun Jig Lee, Hyun Chul Lee, Kap Bum Huh, Kyung Rae Kim, Sung Kil Lim, Kyung Mi Lee
- J Korean Endocr Soc. 1994;9(4):318-324. Published online November 6, 2019
- 1,140 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - The amount of thyroglobulin synthesized from thyroid cells and stored in colloid space in very important in thyroid hormone synthesis. The thyroglobulin synthesis is mainly regulated by TSH secreted from the pituitary gland. But recently there were some reports about the possibility that iodine regulated the thyroid protein synthesis. So our studied were conducted to determined whether iodine could have inhibitory effect on thyroglobulin synthesis and methimazole could abolish the inhibitory effect of idoine.Porcine thyroid cells were isolated by sequential trypsinization in the presence of EGTA, seeded at high density(1X10^6 cells/cm^2) and cultured. One week later, Nal was added in different concentrations(10^-7, 10^-6, 10^-5, 10^-4M). 24hour medias were collected and checked the amount of thyroglobulin secreted. And also pulse-labeling were performed with[^35S] cysteine/methionine(1-2 uCi/well) for 1 hour at the same conditions. We used 3mM methimazole and 10^-4M NaI to observe the blocking effect of methimazol in iodine.The extracellular thyroglobulin secretion was significantly decreased by iodine in dose dependent manner(82.4%, 80.7%, 76.8% and 73.1% of control). And also intracellular thyroglobulin synthesis was significantly decreased by iodide in dose dependent manner(100.5%, 83.4%, 82.3% and 79.4% of control). The inhibitory effect of iodide was abolished by methimazole(74.7% to 101.3% of control). These data indicate that high iodide inhibit the thyroglobulin synthesis and secretion from the thyroid cells, and furthermore autoregulation by iodide may include thyroglobulin synthesis. And also this effect is dependent on the generation of an organic form of iodine because methimazole abolish the inhibitory effect of iodide.

- Changes in Thyrotropin Receptor Blocking Antibody after Antithyroid drug Administration to Patients with Atrophic Autoimmune Thyroiditis (Primary Myxedema).
- Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee, Jae Hoon Chung, Chang Soon Koh, Chan Soo Shin, Won Bae Kim
- J Korean Endocr Soc. 1994;10(3):229-241. Published online November 6, 2019
- 1,071 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - It is well Known that antithyroid drug treatment of Graves' disease suppresses excessive thyroid hormone synthesis and causes a parallel decrease in serum thyroid autoantibody levels including thyroid stimulating antibodies(TSAb) in most patients suggesting the immunosuppressive or immunomodulating effects of antithyroid drugs. In the context of view that thyrotropin receptor blocking antibody may play an important pathogenetic role at least in some patients with primary myxedema(chronic atrophic autoimmune thyroiditis), antithyroid drug treatment in these patients might be beneficial to disease course. To evaluate the effect of antithyroid drug on the thyrotropin receptor blocking antibody levels, we serially measured thyrotropin-binding inhibitor immunoglobulins(TBII) and thyroid stimulation blocking antibodies(TSBAb) using FRTL-5 cells, antimicrosomal- and antithyroglobulin antibody activities in 7 patients with primary myedema who have blocking TSH receptor antibodies during 6 months of methimazole(MMI, 40mg/day) administration. TBII and TSBAb activities did not change after MMI, but one of them showed stepwise decrease and disappearance of TBII and TSBAb activities. Antimicrosomal- and antithyroglobulin antibody activities decreased significantly after 3 months of MMI administration in those patients. These results suggest a minimal effect of antithyroid drug treatment on the level of thyrotropin receptor blocking antibodies. Persistence of thyrotropin receptor blocking antibodies despite of the decrease in antimicrosomal and antithyroglobulin antibodies might suggest that blocking TSH receptor antibodies of primary myxedema is produced mainly in extrathyroidal tissue in contrast to the thyroid stimulating antibodies of Graves' disease. One patient, whose blocking antibody have disappeared after MMI treatment, is under observation to see if she will remain in remission of hypothyroidism.

- The Effect of Tumor Necrosis Factor - α on the Thyroglobulin Synthesis and TSH Action in Cultured Porcine Thyroid Cells.
- Jae Wha Jo, Eun Jig Lee, Moon Suk Nam, Su Youn Nam, Young Duk Song, Sung Kil Lim, Hyun Chul Lee, Kap Bum Huh, Kyung Rae Kim
- J Korean Endocr Soc. 1994;10(3):220-228. Published online November 6, 2019
- 1,037 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - Abnormal thyroid function is seen in a wide variety of patients with acute and chronic nonthyroidal-illness, consisting of reduction in both thyroid function and peripheral T_4 to T_3 conversion including decreased serum thyroxin(T_4), decreased triiodothyronine and normal or slightly increased serum TSH. Recently increasing awareness of the role of tumor necrosis factor-alpha(TNF-alpha) in systemic illness led us to consider a possible contribution of TNF-alpha to thyroid dysfunction in this setting. So we hypothesized that TNF-alpha might affect the function of the thyroid gland. We, therefore, explored the effects of TNF-alpha on the cultured porcine thyroid cells in TSH-stimulated and TSH-nonstimulated conditions. Primarily cultured porcine thyroid cells were incubated with various concentrations(-500pg/ml) of recombinant buman TNF-alpha and bTSH(1mu/ml), with measurement of secreted thyroglobulin(Tg) and cyclic AMP(c-AMP) as the end points of stimulation, and produced intracellular Tg by pulse-labelling. TNF-alpha significantly inhibited TSH-stimulated intracellular Tg synthesis and extracellar Tg secretion at 200 and 500pg/ml concentration. TNF-alpha didn't affect c-AMP production at any concentration tested. So we conclude that increased in serum TNF-alpha may be responsible for reduced thyroid function in patients with acute and chronic nonthyroidal-illness.

- Endocrine Research
- Comparison of Thyroglobulin Measurements Using Three Different Immunoassay Kits: A BRAMHS Tg-Plus RIA Kit, a BRAMHS hTg Sensitive Kryptor Kit, and a Beckman Coulter ACCESS Immunoassay Kit
- Mijin Kim, Min Ji Jeon, Won Gu Kim, Jong Jin Lee, Jin-Sook Ryu, Eun-Jung Cho, Dae-Hyun Ko, Woochang Lee, Sail Chun, Won-Ki Min, Tae Yong Kim, Young Kee Shong, Won Bae Kim
- Endocrinol Metab. 2016;31(3):462-468. Published online August 2, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.3.462
- 5,103 View
- 49 Download
- 8 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Second-generation thyroglobulin immunometric assays (Tg-IMAs) have been developed with improved sensitivity. Our aim was to compare the diagnostic value of Tg-IMA measurements using a Kryptor (BRAHMS AG) kit (Tg-K) and an ACCESS (Beckman Coulter) kit (Tg-A) with that of the first-generation Tg measurement using a Tg-plus (BRAHMS AG) kit (Tg+).
Methods We enrolled 82 differentiated thyroid cancer patients who underwent total thyroidectomy with radioactive iodine remnant ablation and who underwent diagnostic whole body scan using recombinant human thyroid stimulating hormone (rhTSH). The Tg+, Tg-K, and Tg-A were measured before rhTSH administration during levothyroxine treatment (suppressed Tg) from the same sample. Serum Tg+ was measured after rhTSH stimulation (stimulated Tg).
Results Suppressed Tg+ was more significantly correlated with suppressed Tg-K (
R 2=0.919,P <0.001) than with suppressed Tg-A (R 2=0.536,P <0.001). The optimal cut-off values of suppressed Tg+, Tg-K, and Tg-A for predicting stimulated Tg+ of 1 ng/mL were 0.3, 0.2, and 0.2 ng/mL, respectively. The sensitivity, specificity, and accuracy of suppressed Tg+ were 67%, 100%, and 90%, respectively; those of suppressed Tg-K were 83%, 90%, and 88%; those of suppressed Tg-A were 96%, 82%, and 87%, respectively. The positive predictive and negative predictive values of Tg+ were 100% and 87%, respectively; those of Tg-K were 79% and 92%; and those of Tg-A were 73% and 98%.Conclusion We could not clearly demonstrate which kit had better diagnostic performance after comparison of first-generation Tg measurements with Tg-IMA measurements. Also, there were kit-to-kit variations between Tg-IMA kits. Suppressed Tg measured by Tg-IMA was insufficient to completely substitute for a stimulated Tg measurement.
-
Citations
Citations to this article as recorded by- Comparison of the diagnostic performances of US-guided fine needle aspiration cytology and thyroglobulin measurement for lymph node metastases in patients with differentiated thyroid carcinoma: a meta-analysis
Rong-Bin Liu, Da-Lei Zhou, Bo-Heng Xu, Xin-Hua Yang, Qing Liu, Xiao Zhang, Tao Tang, Zu-Lu Ye, Yue Li
European Radiology.2021; 31(5): 2903. CrossRef - Preoperative Serum Thyroglobulin and Its Correlation with the Burden and Extent of Differentiated Thyroid Cancer
Hosu Kim, So Young Park, Jun-Ho Choe, Jee Soo Kim, Soo Yeon Hahn, Sun Wook Kim, Jae Hoon Chung, Jaehoon Jung, Tae Hyuk Kim
Cancers.2020; 12(3): 625. CrossRef - Estimating the Growth Rate of Lung Metastases in Differentiated Thyroid Carcinoma: Response Evaluation Criteria in Solid Tumors or Doubling Time?
Eyun Song, Jonghwa Ahn, Min Ji Jeon, Sang Min Lee, Jeong Hyun Lee, Tae Yong Kim, Jung Hwan Baek, Won Bae Kim, Young Kee Shong, Won Gu Kim
Thyroid.2020; 30(3): 418. CrossRef - Impact of delayed radioiodine therapy in intermediate‐/high‐risk papillary thyroid carcinoma
Mijin Kim, Minkyu Han, Min Ji Jeon, Won Gu Kim, In Joo Kim, Jin‐Sook Ryu, Won Bae Kim, Young Kee Shong, Tae Yong Kim, Bo Hyun Kim
Clinical Endocrinology.2019; 91(3): 449. CrossRef - Tertiary Care Experience of Sorafenib in the Treatment of Progressive Radioiodine-Refractory Differentiated Thyroid Carcinoma: A Korean Multicenter Study
Mijin Kim, Tae Hyuk Kim, Dong Yeob Shin, Dong Jun Lim, Eui Young Kim, Won Bae Kim, Jae Hoon Chung, Young Kee Shong, Bo Hyun Kim, Won Gu Kim
Thyroid.2018; 28(3): 340. CrossRef - A Follow-Up Strategy for Patients with an Excellent Response to Initial Therapy for Differentiated Thyroid Carcinoma: Less Is Better
Min Ji Jeon, Mijin Kim, Suyeon Park, Hye-Seon Oh, Tae Yong Kim, Won Bae Kim, Young Kee Shong, Won Gu Kim
Thyroid.2018; 28(2): 187. CrossRef - Preoperative serum thyroglobulin predicts initial distant metastasis in patients with differentiated thyroid cancer
Hosu Kim, Young Nam Kim, Hye In Kim, So Young Park, Jun-Ho Choe, Jung-Han Kim, Jee Soo Kim, Jae Hoon Chung, Tae Hyuk Kim, Sun Wook Kim
Scientific Reports.2017;[Epub] CrossRef
- Comparison of the diagnostic performances of US-guided fine needle aspiration cytology and thyroglobulin measurement for lymph node metastases in patients with differentiated thyroid carcinoma: a meta-analysis

- A Case of Incidental Struma Ovarii Confounded with the Metastasis of Papillary Thyroid Cancer.
- Young Hee Jung, Sung Min Jung, Jong Min Lee, Yi Sun Jang, In Suk Lee, Jong Ok Kim, Hye Soo Kim
- Endocrinol Metab. 2012;27(3):227-231. Published online September 19, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.3.227
- 1,764 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - A focal radioactive iodine uptake in the pelvis of a patient with differentiated thyroid cancer needs differential diagnosis besides bone metastasis. Struma ovarii is a rare monodermal ovarian teratoma composed predominantly of mature thyroid tissue; 5-10% of these tumors are malignant. As diagnosis and surgery of thyroid cancer have increased recently, incidental cases of struma ovarii, after radioactive iodine treatment, were occasionally reported. Rare cases of ovary metastasis of thyroid cancer were also reported. We report a case of benign struma ovarii incidentally found in a patient with papillary thyroid cancer. The patient showed a sustained high level of thyroglobulin and focal radioactive iodine uptake in the right pelvis, confused with distant metastasis, after total thyroidectomy and radioactive iodine treatment.

- Effects of alpha-lipoic Acid on Differentiation of Thyroid Cancer Cells.
- Won Gu Kim, Doo Hee Han, Hyun Jeung Choi, Eui Young Kim, Tae Yong Kim, Young Kee Shong, Won Bae Kim
- J Korean Endocr Soc. 2010;25(1):28-36. Published online March 1, 2010
- DOI: https://doi.org/10.3803/jkes.2010.25.1.28
- 2,095 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Induction of re-differentiation is necessary for the proper treatment of patients with recurrent or metastatic differentiated thyroid cancer (DTC) because cancer cells show de-differentiation in about 30% of these patients. In this study, we evaluated the expression of thyroid specific genes after treatment with various agents to induce re-differentiation in the follicular thyroid cancer cell line FTC-133. METHODS: FTC-133 cells were treated with U0126, LY294002, trichostatin A, retinoic acid (RA), 5'-azacytidine and alpha-lipoic acid (ALA). We evaluated mRNA expression of thyroid specific genes, thyroglobulin (Tg), sodium iodine symporter (NIS), PAX-8 and TTF-1 by reverse transcriptase polymerase chain reaction (PCR). Quantified expression of Tg mRNA was also evaluated by real-time PCR. RESULTS: The expression of Tg mRNA increased after 48 h of treatment with 0.1 uM RA and the expression of Tg mRNA and TTF-1 mRNA increased after 48-72 h of treatment with ALA (10~100 uM). There was no change in thyroid specific gene expression by the other agents. Increased expression of Tg mRNA was confirmed by real-time PCR (1.3 times by 10 uM ALA and 3.6 times by 100 uM ALA). There was no basal NIS mRNA expression in FTC-133 cells and none of the tested agents induced expression of NIS mRNA. There was no change in phosphorylation of AMPK1-alpha after ALA treatment of FTC-133 cells. CONCLUSION: ALA increases mRNA expression of Tg and TTF-1 of FTC-133 thyroid cancer cells and these effects are not mediated by activation of AMP kinase. The finding that ALA could be a potential re-differentiation inducing agent in thyroid cancer cells is novel. Further studies are needed to elucidate the mechanism of induction of re-differentiation. Furthermore, the effect of ALA on NIS expression and on iodine uptake should be evaluated using diverse thyroid cancer cell lines.

- Change in Thyroid Autoantibodies According to the Clinical Course of Painless Thyroiditis Excluding Postpartum Thyroiditis.
- Ihn Suk Lee, Young Suk Jo, Bon Jeong Ku, Minho Shong, Young Kun Kim, Heung kyu Ro
- J Korean Endocr Soc. 2008;23(4):245-252. Published online August 1, 2008
- DOI: https://doi.org/10.3803/jkes.2008.23.4.245
- 2,020 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Painless thyroiditis is characterized by painless, destructive inflammation of the thyroid gland. Although thyroid autoantibodies are frequently detected in patients suffering from this condition, the clinical significance of these antibodies is not well understood. Therefore, this study was conducted to investigate the relationship between thyroid function and thyroid autoantibodies in painless thyroiditis according to clinical course. METHODS: Patients proven to have painless thyroiditis were retrospectively included in this study. We analyzed their clinical features, thyroid function and titers of thyroid autoantibodies according to clinical course, which was divided into three phases; thyrotoxic, hypothyroid and recovery. RESULTS: Of the 21 patients included in this study, 2 were male and 19 were female. During the thyrotoxic phase, the mean free T4 concentration was 4.03 (2~6.8) ng/mL and the mean concentration of thyroid stimulating hormone (TSH) was 0.02 (0.01~0.07) U/mL. In addition, the titer of antithyroglobulin antibody and antithyroid peroxidase antibody was 298 (4.8~995) U/mL and 3318 (0.1~25280) U/mL, respectively during this phase. During the hypothyroid phase, the mean TSH was 16.3 (4.3-49.5) U/mL and was found to be positively correlated with the level of free T4 observed during the thyrotoxic phase (r = 0.523, P = 0.031). During the recovery phase, the titer of antithyroglobulin antibody was significantly reduced to 180 (38~487) U/mL when compared with the titer taken during the thyrotoxic phase (P = 0.016). Additionally, during the hypothyroid phase, patients found to have antithyroid peroxidase antibody had a higher titer of TSH than those that did not (23.9 (6.5~49.5) vs. 11.2 (5.3~18.2) U/mL, P = 0.004). CONCLUSION: The titer of free T4 and the presence of antithyroid peroxidase observed during the thyrotoxic phase were related to the titer of TSH during hypothyroid phase. Additionally, the titer of antithyroglobulin antibody was significantly reduced during the recovery phase.

- Influence of Anti-thyroglobulin Antibody on the Measurement of Thyroglobulin using the Immunoradiometric Assay.
- Byeong Cheol Ahn, Jin Ho Bae, Shin Young Jeong, Ho Yong Park, Jung Guk Kim, Sung Woo Ha, Jaetae Lee, Bo Wan Kim, Kyu Bo Lee
- J Korean Endocr Soc. 2004;19(1):42-47. Published online February 1, 2004
- 1,290 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Serum thyroglobulin(Tg) is a valuable and sensitive tool needed in the follow-up of patients with differentiated thyroid cancer(DTC), but antithyroglobulin antibody(Anti-Tg), common in patients with DTC, can interfere with the assay for Tg. In this study, we evaluated the influence of Anti-Tg on the measurement of Tg using the immunoradiometric assay(IRMA). METHODS: In using ELSA-hTg in vivo test(CIS international, Schering, France), a solid phase two-site IRMA was used to measure Tg(23.5ng/mL, 62.5ng/mL) under the absence or presence of three concentrations of Anti-Tg(25U/mL, 50U/mL, 100U/mL). We also performed Tg measurement using patients serum that was mixed with patients serum containing high Anti-Tg. ANOVA and Scheffe tests were performed to evaluate the effect of Anti-Tg on Tg IRMA, and an inverse regression was made to calculate the level of Tg from measured Tg and used Anti-Tg levels and also to assess the degree of effect of anti-Tg on Tg IRMA. RESULTS: In measuring Tg using the standard solution, the presence of Anti-Tg resulted in a falsely suppressed Tg value. The IRMAs for 23.5ng/mL of the standard Tg solution resulted in 24.5+/-.1 ng/mL under no Anti-Tg, 11.8+/-.4ng/mL under 25U/mL of Anti-Tg, 7.7+/-.1ng/mL under 50U/mL of Anti-Tg, and 4.5+/-.4ng/mL under 100U/mL of Anti-Tg. IRMAs 62.5ng/mL of the standard Tg solution resulted in 65.9+/-.7ng/mL under no Anti-Tg, 36.3+/-.2ng/mL under 25U/mL of Anti-Tg, 23.7+/-.7ng/mL under 50U/mL of Anti-Tg, and 14.0+/-.0ng/mL under 100U/mL of Anti-Tg. (ANOVA test, p=0.000). The degree of suppression of the measured Tg value was positively correlated with the Anti-Tg level (Quadratic model regression, Sig T=0.000). The presence of Anti-Tg also resulted in a falsely suppressed Tg value for the Tg measurement using patient's serum. CONCLUSION: The presence of Anti-Tg could consist of the use of Tg as a tumor, therefore Anti-Tg should be measured in all patients diagnosed with DTC. The interpretation of the Tg level must be performed with extreme caution in patients with Anti-Tg.

- Serum Thyroglobulin Levels Predicting Recurrence and Distant Metastasis after Surgery in Patients with Differentiated Thyroid Cancer.
- Kyoung Soo Kim, Jin Sook Ryu, Suck Joon Hong, Won Bae Kim, Young Kee Shong
- J Korean Endocr Soc. 2003;18(2):153-165. Published online April 1, 2003
- 1,660 View
- 48 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Reports on serum thyroglobulin(Tg) levels being used to predict recurrence or distant metastasis during the follow-up of patients with differentiated thyroid cancer(DTC) has been inconsistent. In addition, there have been few reports that attempt to define the cut-off value of Tg for recurrence or distant metastasis obtained by a receiver operating characteristic(ROC) curve. As well, there are differences in opinions on what the value should be on the first serum Tg level measured just before radioactive iodine(RAI) ablation(Tg-RAI), during thyroxine administration (Tg-on), and after thyroxine withdrawal(Tg-off) during the follow-up. Reports on the positive predictive values(PPVs) and negative predictive values(NPVs) of these Tg values are rare. METHODS: A total of 205 patients(42 males, 163 females) with DTC were studied. All patients had undergone total or near-total thyroidectomy. After surgery and RAI ablation, annual thyroxine withdrawal 131I-whole body scan(WBS) with Tg measurements was performed. The mean duration of follow-up was 5.0 (1.4~7.4) years. The most sensitive and specific Tg values(cut-off values) for tumor recurrence and/or distant metastasis were selected by using ROC curves. We also calculated the PPVs and NPVs for recurrence and/or distant metastasis using two-by-two tables. RESULTS: Cut-off values of Tg-RAI, Tg-on, and Tg-off for recurrence were 11.8, 1.4, and 3.3ng/mL, respectively. For these values, the sensitivities were 85.4, 82.2, and 93.3%, with the specificitiesat 89.2, 92.4, and 88.0%. PPVs were 71.9, 77.1, and 77.0% while NPVs were 95.0, 94,4, and 97.8%. The cut-off values for distant metastasis were 27.4, 2.5, and 7.9ng/mL, respectively. For these cut-off values, the sensitivities were 86.7, 87.5, and 92.3%, with the specificities being 86.2, 90.8, and 80.2%. PPVs were 34.2, 46.7, and 25.0% and NPVs were 98.7, 98.8, and 99.3%. CONCLUSION: All three serum Tg levels were sensitive and specific markers for recurrence and distant metastasis. Their PPVs were low in contrast to the high NPVs. In comparison with Tg-on, Tg-off showed higher sensitivity and NPV as well as lower specificity and PPV. Therefore, in the case of higher Tg-on during the follow-up period, efforts to find recurrence and distant metastasis,such as 131I-WBS, should be done. In addition, regular measurement of Tg-off or Tg after stimulation with recombinant human TSH is recommended as a screening test.

- Molecular Diagnosis of Recurrent Thyroid Cancer by Reverse Transcription-Polymerase Chain Reaction of Thyroglobulin Messenger Ribonucleic Acid in Peripheral Blood.
- Sung Il Kwon, Ki Ryong Park, Hyun Young Kim, Chae Hee Shin, Young Chan Lim, Young Sik Choi, Yo Han Park, Kang Dae Lee, Hee Kyung Chang, Jae Hwa Lee, Ha Yong Yum
- J Korean Endocr Soc. 2002;17(4):501-513. Published online August 1, 2002
- 1,091 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Differentiated thyroid cancer is the most common endocrine malignancy. Despite advances in the treatment of thyroid cancer, disease recurrence and metastasis may occur in as many as 20% of patients, and so continues to pose major problems in its clinical management. Serum thyroglobulin (Tg) measurements, by immunoassay, are used to detect residual or recurrent thyroid cancer following thyroid ablation. However, the usefulness of immunoassay is limited by both the requirement for thyroid hormone withdrawal, to attain optimal test sensitivity, and interference by the antithyroglobulin antibody (Anti-Tg Ab). Recent studies have reported the clinical usefulness of reverse transcription-polymerase chain reaction (RT-PCR) detection of Tg mRNA in the peripheral blood of patients with differentiated thyroid carcinomas. We performed this study to evaluate the usefulness RT-PCR of Tg mRNA in peripheral blood of patients with thyroid carcinoma following a total thyroidectomy and radioiodine ablation therapy. METHODS: Forty cases that underwent a total thyroidectomy and radioiodine ablation therapy were included in this study. Of the 40 patients, 35 were papillary carcinomas and 5 were follicular carcinomas. Ten normal control subjects were also studied. Tg mRNA was extracted. Then RT-PCR, and nested RT-PCR, were run with specific Tg primers. Concurrently, DNA sequencing of the isolates was carried out to prove the isolates were identical to the nucleotide sequence of the Tg. RESULTS: The Tg was detected in 4 of 19 patients, with either a residual thyroid bed, or metastasis, on a 131I whole body scan and in 1 of 21 patients with a negative radioiodine scan. Surprisingly, the Tg mRNA was detected in all the patients and normal controls. CONCLUSION: From our results we can not recommend Tg mRNA, detected by RT-PCR in peripheral blood, as a tumor marker superior to that of the Tg serum level. We consider an intensive re-evaluation of the method is required before considering its clinical applications.

- Clinical Applications of 18-FDG PET in Recurred Differentiated Thyroid Cancer with Negative 131I Whole Body Scintigraphy: A Comparative Analysis with 99mTc-MIBI Scintigraphy.
- Jong Chul Won, Sung Jin Lee, Tae Yun Lee, Il Seong Nam-Goong, Sy Yeol Lee, Ha Young Kim, Jung Hee Han, Jin Sook Ryu, Dae Hyuk Moon, Il Min Ahn
- J Korean Endocr Soc. 2001;16(4-5):481-493. Published online October 1, 2001
- 936 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
In patients with differentiated thyroid cancer treated by surgery and radioactive iodine ablation, serum thyroglobulin(Tg) and 131I whole body scan(WBS) are recognized as being the best cooperative indicators for detection of recurrence or metastasis. However, in some cases, 131I WBS shows no specific lesions despite elevated serum Tg. Therefore, 18-Fluorine-fluorodeoxyglucose (FDG) positron emission tomography(PET) has emerged as a useful method for the detection of 131I WBS negative thyroid cancers. The aims of the present study are to evaluate the clinical usefulness of this technique in detection and to compare the results with 99mTc-MIBI scintigraphy(MIBI) in cases of final results being confirmed by histologic diagnosis and other imaging methods. METHODS: We conducted a retrospective analysis amon 131I WBS negative recurred papillary thyroid carcinoma patients(male: female ratio=9:22, median age=42 yr). FDG PET was performed in 28 patients and MIBI 28 patients, 25 of whom were common to both groups. All patients had histologically proven recurrence/metastasis and negative 131I WBS results but persistently elevated serum Tg levels. In each case overall clinical evaluations were performed including histology, cytology, thyroglobulin level, other imaging methods, posttherapy 131I WBS and subsequent clinical course, to allow comparison with the results of FDG PET. RESULTS: In 19 cases of patients with negative 131I WBS, proven recurrence/metastasis lesions were detected in FDG PET. Compared with MIBI, FDG PET was found to be superior in 8 cases(including 2 patients with distant metastases). No FDG-negative/MIBI-positive tumor was observed. One FDG PET negative and MIBI negative case was proven 3 months later to be metastatic cervical lymph nodes, Sensitivities were 94.7% in the FDG PET group and 52.6% in MIBI. Diagnostic accuracy of FDG PET was superior to that of MIBI(93% vs. 62%, respectively, p=0.003). CONCLUSION: Our results confirmed the clinical usefulness of FDG PET for detection of 131I negative differentiated thyroid cancers and suggested the value of FDG PET as an initial diagnostic step, rather than MIBI, in these cases.

- The Changes of Expression of Thyroid Specific Antigens in Aging.
- Young Joo Park, Eun Shin Park, Tae Yong Kim, Sang Wan Kim, Hyeong Kyu Park, Do Joon Park, Won Bae Kim, Chan Soo Shin, Kyoung Soo Park, Seong Yeon Kim, Sang Chul Park, Hong Kyu Lee, Bo Youn Cho
- J Korean Endocr Soc. 2001;16(4-5):457-466. Published online October 1, 2001
- 1,023 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
With the prevalence of serum antithyroglobulin(anti-TG) and antithyroperoxidase(anti-TPO) autoantibodies increasing with age, it has been suggested that changes of thyroid autoimmunity with aging are associated with endemic iodine intake. To understand the mechanism of aging-related increases of thyroid autoimmune response, we investigated the expression of thyroid specific autoantigens of aged phenotype, and compared them with those of young phenotype both in vivo and in vitro. METHODS: Sprague-Dawley rats were sacrificed at 5, 10 and 16 weeks(young), and at 23 months(aged). Their FRTL-5 thyroid cells were harvested at cell passages less than 10(fresh) or more than 30 (aged). The expression of thyroid autoantigens, sodium-iodide symporter(NIS), TSH receptor (TSHR), TG and TPO, were examined by northern blot analysis. To evaluate the effects of iodide, 1mM of NaI was added to the medium for 24 hours, and following incubation the expressions of MHC class I and class II were also examined. RESULTS: The expressions of TPO were markedly increased in the aged rats, and those of TG were moderately. However, NIS and TSHR showed no differences in their expression levels between aged rats and young rats. In vitro, there were no differences in the expressions of TG or TPO, nor of NIS or TSHR, between aged cells and fresh cells. Neither did Iodide exhibit any influence on the expression of MHC molecules in aged cells or fresh cells. CONCLUSION: The expression levels of TPO and TG were increased in aged rats, which may partially explain the mechanism of increasing thyroid autoimmunity with age.


 KES
KES

 First
First Prev
Prev



