Search
- Page Path
- HOME > Search
- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database) - Cardiovascular Outcomes of Obesity According to Menopausal Status: A Nationwide Population-Based Study
- Bo Kyung Koo, Sang-Hyun Park, Kyungdo Han, Min Kyong Moon
- Endocrinol Metab. 2021;36(5):1029-1041. Published online October 21, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1197

- 3,688 View
- 117 Download
- 8 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
We estimated the effect of obesity on the incidence of cardiovascular disease (CVD) and mortality in women according to menopausal status.
Methods
Women aged 40 to 69 years under routine health check-ups provided by the National Health Insurance Service in 2009 were followed up till 2018 (n=2,208,559).
Results
In premenopausal women, a significant increment of mortality rate was found in underweight and obesity class II (hazard ratio [HR], 1.48; 95% confidence interval [CI], 1.31 to 1.67; and HR, 1.25; 95% CI, 1.12 to 1.39) compared to normal body mass index (BMI); overweight and obesity class I did not affect mortality rate. In postmenopausal women, obesity as well as overweight status reduced the risk of mortality compared to normal BMI (HR, 0.86; 95% CI, 0.83 to 0.88; and HR, 0.84; 95% CI, 0.82 to 0.86). By contrast, there was a linear association between CVD and BMI above the normal range irrespective of menopausal status, which was attenuated in diabetic women.
Conclusion
The current study replicated the J-shaped relationship between BMI and mortality, being more prominent in the postmenopausal group. The risk of CVD was linearly increased as BMI was increased above the normal range irrespective of menopausal status. -
Citations
Citations to this article as recorded by- Biosocial predictors and blood pressure goal attainment among postmenopausal women with hypertension
Geetha Kandasamy, Thangamani Subramani, Gigi Sam, Mona Almanasef, Tahani Almeleebia, Eman Shorog, Asma M. Alshahrani, Amjad Hmlan, Atheer Y. Al Suhaym, Kousalya Prabahar, Vinoth Prabhu Veeramani, Palanisamy Amirthalingam
Frontiers in Cardiovascular Medicine.2024;[Epub] CrossRef - A nationwide cohort study on diabetes severity and risk of Parkinson disease
Kyungdo Han, Bongsung Kim, Seung Hwan Lee, Mee Kyoung Kim
npj Parkinson's Disease.2023;[Epub] CrossRef - Cardiovascular Outcomes according to Comorbidities and Low-Density Lipoprotein Cholesterol in Korean People with Type 2 Diabetes Mellitus
Min Kyong Moon, Junghyun Noh, Eun-Jung Rhee, Sang Hyun Park, Hyeon Chang Kim, Byung Jin Kim, Hae Jin Kim, Seonghoon Choi, Jin Oh Na, Young Youl Hyun, Bum Joon Kim, Kyung-Do Han, In-Kyung Jeong
Diabetes & Metabolism Journal.2023; 47(1): 45. CrossRef - The effect of menopause on cardiovascular risk factors according to body mass index in middle-aged Korean women
Do Kyeong Song, Young Sun Hong, Yeon-Ah Sung, Hyejin Lee, Aysha Almas
PLOS ONE.2023; 18(3): e0283393. CrossRef - Low‐quality muscle mass rather than normal‐quality muscle mass determines fibrosis progression in biopsy‐proven NAFLD
Yun Kyu Lee, Bo Kyung Koo, Sae Kyung Joo, Dong Hyeon Lee, Heejoon Jang, Jee Won Chai, Myoung Seok Lee, Si Won Jang, Young Ho So, Jeong Hwan Park, Mee Soo Chang, Won Kim
Alimentary Pharmacology & Therapeutics.2023; 58(3): 322. CrossRef - Diabetes severity is strongly associated with the risk of active tuberculosis in people with type 2 diabetes: a nationwide cohort study with a 6-year follow-up
Ji Young Kang, Kyungdo Han, Seung-Hwan Lee, Mee Kyoung Kim
Respiratory Research.2023;[Epub] CrossRef - Effects of exercise initiation and smoking cessation after new-onset type 2 diabetes mellitus on risk of mortality and cardiovascular outcomes
Mee Kyoung Kim, Kyungdo Han, Bongsung Kim, Jinyoung Kim, Hyuk-Sang Kwon
Scientific Reports.2022;[Epub] CrossRef - Non-pharmacologic treatment for obesity
Bo Kyung Koo
Journal of the Korean Medical Association.2022; 65(7): 400. CrossRef
- Biosocial predictors and blood pressure goal attainment among postmenopausal women with hypertension

- Clinical Study
Big Data Articles (National Health Insurance Service Database) - Variabilities in Weight and Waist Circumference and Risk of Myocardial Infarction, Stroke, and Mortality: A Nationwide Cohort Study
- Da Hye Kim, Ga Eun Nam, Kyungdo Han, Yang-Hyun Kim, Kye-Yeung Park, Hwan-Sik Hwang, Byoungduck Han, Sung Jung Cho, Seung Jin Jung, Yeo-Joon Yoon, Yong Kyun Roh, Kyung Hwan Cho, Yong Gyu Park
- Endocrinol Metab. 2020;35(4):933-942. Published online December 23, 2020
- DOI: https://doi.org/10.3803/EnM.2020.871
- 5,565 View
- 110 Download
- 15 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Evidence regarding the association between variabilities in obesity measures and health outcomes is limited. We aimed to examine the association between variabilities in obesity measures and cardiovascular outcomes and all-cause mortality.
Methods
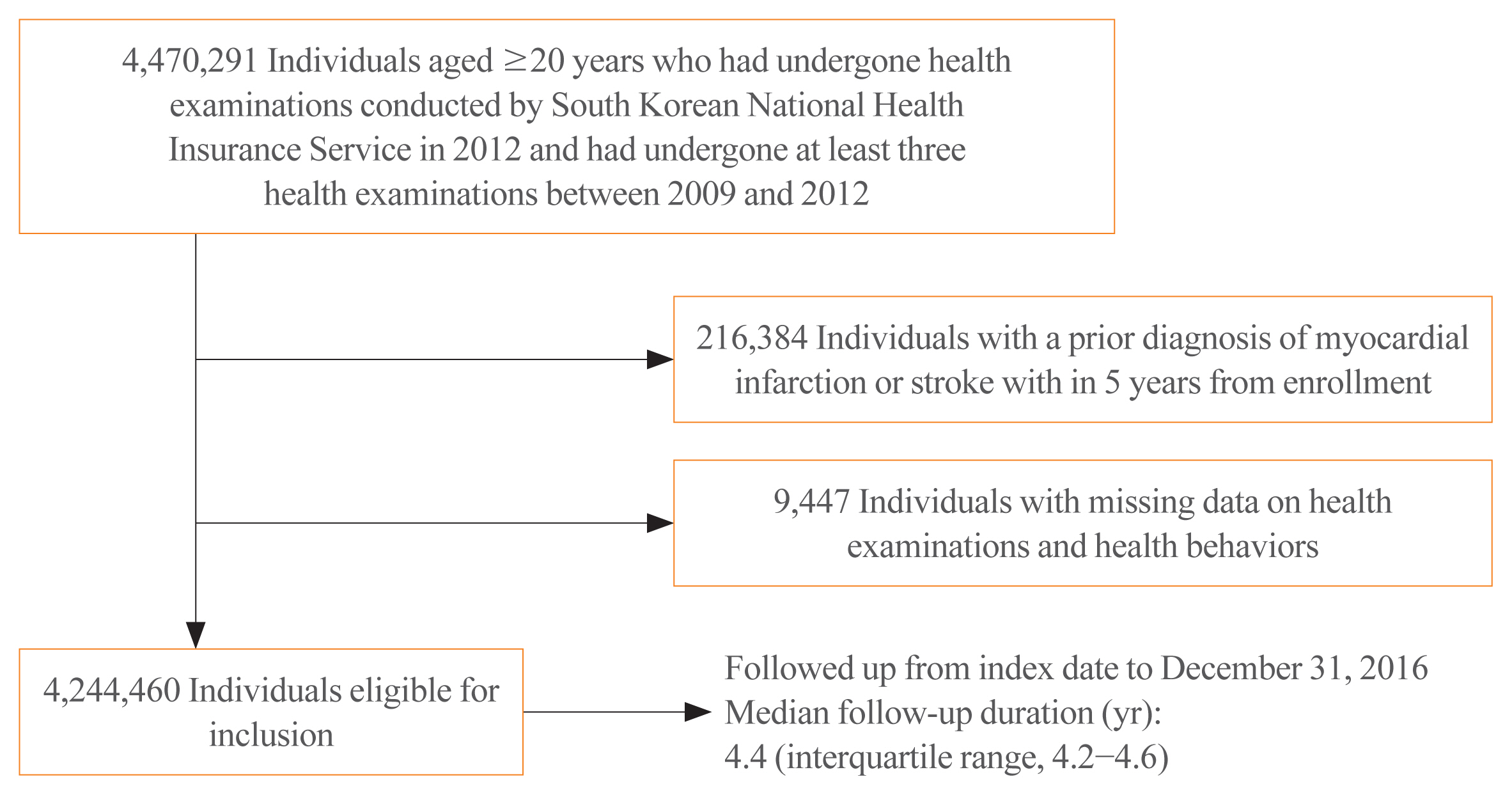
We identified 4,244,460 individuals who underwent health examination conducted by the Korean National Health Insurance Service during 2012, with ≥3 anthropometric measurements between 2009 and 2012. Variabilities in body weight (BW) and waist circumference (WC) were assessed using four indices including variability independent of the mean (VIM). We performed multivariable Cox proportional hazards regression analyses.
Results
During follow-up of 4.4 years, 16,095, 18,957, and 30,200 cases of myocardial infarction (MI), stroke, and all-cause mortality were recorded. Compared to individuals with the lowest quartiles, incrementally higher risks of study outcomes and those of stroke and all-cause mortality were observed among individuals in higher quartiles of VIM for BW and VIM for WC, respectively. The multivariable adjusted hazard ratios and 95% confidence intervals comparing the highest versus lowest quartile groups of VIM for BW were 1.17 (1.12 to 1.22) for MI, 1.20 (1.16 to 1.25) for stroke, and 1.66 (1.60 to 1.71) for all-cause mortality; 1.07 (1.03 to 1.12) for stroke and 1.29 (1.25 to 1.33) for all-cause mortality regarding VIM for WC. These associations were similar with respect to the other indices for variability.
Conclusion
This study revealed positive associations between variabilities in BW and WC and cardiovascular outcomes and allcause mortality. Our findings suggest that variabilities in obesity measures are associated with adverse health outcomes in the general population. -
Citations
Citations to this article as recorded by- Gender differences in midlife to later-life cumulative burden and variability of obesity measures and risk of all-cause and cause-specific mortality
Karim Kohansal, Siamak Afaghi, Davood Khalili, Danial Molavizadeh, Farzad Hadaegh
International Journal of Obesity.2024; 48(4): 495. CrossRef - Association of body mass index and blood pressure variability with 10-year mortality and renal disease progression in type 2 diabetes
Stephen Fava, Sascha Reiff
Acta Diabetologica.2024;[Epub] CrossRef - Weight variability and cardiovascular outcomes: a systematic review and meta-analysis
Robert J. Massey, Moneeza K. Siddiqui, Ewan R. Pearson, Adem Y. Dawed
Cardiovascular Diabetology.2023;[Epub] CrossRef - Family history, waist circumference and risk of ischemic stroke: A prospective cohort study among Chinese adults
Lei Liu, Xiaojia Xue, Hua Zhang, Xiaocao Tian, Yunhui Chen, Yu Guo, Pei Pei, Shaojie Wang, Haiping Duan, Ruqin Gao, Zengchang Pang, Zhengming Chen, Liming Li
Nutrition, Metabolism and Cardiovascular Diseases.2023; 33(4): 758. CrossRef - Big Data Research in the Field of Endocrine Diseases Using the Korean National Health Information Database
Sun Wook Cho, Jung Hee Kim, Han Seok Choi, Hwa Young Ahn, Mee Kyoung Kim, Eun Jung Rhee
Endocrinology and Metabolism.2023; 38(1): 10. CrossRef - Weight variability and diabetes complications
Francesco Prattichizzo, Chiara Frigé, Rosalba La Grotta, Antonio Ceriello
Diabetes Research and Clinical Practice.2023; 199: 110646. CrossRef - Research on obesity using the National Health Information Database: recent trends
Eun-Jung Rhee
Cardiovascular Prevention and Pharmacotherapy.2023; 5(2): 35. CrossRef - Weight cycling and risk of clinical adverse events in patients with heart failure with preserved ejection fraction: a post-hoc analysis of TOPCAT
Yi Tan, Hang Guo, Ning Zhang, Keyang Zheng, Guifang Liu
Frontiers in Endocrinology.2023;[Epub] CrossRef - Weight variability, physical functioning and incident disability in older adults
Katie J. McMenamin, Tamara B. Harris, Joshua F. Baker
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(4): 1648. CrossRef - Association between Variability of Metabolic Risk Factors and Cardiometabolic Outcomes
Min Jeong Park, Kyung Mook Choi
Diabetes & Metabolism Journal.2022; 46(1): 49. CrossRef - Effects of exercise initiation and smoking cessation after new-onset type 2 diabetes mellitus on risk of mortality and cardiovascular outcomes
Mee Kyoung Kim, Kyungdo Han, Bongsung Kim, Jinyoung Kim, Hyuk-Sang Kwon
Scientific Reports.2022;[Epub] CrossRef - Lipid cutoffs for increased cardiovascular disease risk in non-diabetic young people
Mee Kyoung Kim, Kyungdo Han, Hun-Sung Kim, Kun-Ho Yoon, Seung-Hwan Lee
European Journal of Preventive Cardiology.2022; 29(14): 1866. CrossRef - Body Mass Index Is Independently Associated with the Presence of Ischemia in Myocardial Perfusion Imaging
Chrissa Sioka, Paraskevi Zotou, Michail I. Papafaklis, Aris Bechlioulis, Konstantinos Sakellariou, Aidonis Rammos, Evangelia Gkika, Lampros Lakkas, Sotiria Alexiou, Pavlos Kekiopoulos, Katerina K. Naka, Christos Katsouras
Medicina.2022; 58(8): 987. CrossRef - Waist Circumference and Body Mass Index Variability and Incident Diabetic Microvascular Complications: A Post Hoc Analysis of ACCORD Trial
Daniel Nyarko Hukportie, Fu-Rong Li, Rui Zhou, Jia-Zhen Zheng, Xiao-Xiang Wu, Xian-Bo Wu
Diabetes & Metabolism Journal.2022; 46(5): 767. CrossRef - Nonalcoholic fatty liver disease and the risk of insulin-requiring gestational diabetes
Sang Youn You, Kyungdo Han, Seung-Hawn Lee, Mee Kyoung Kim
Diabetology & Metabolic Syndrome.2021;[Epub] CrossRef - Increased Risk of Nonalcoholic Fatty Liver Disease in Individuals with High Weight Variability
Inha Jung, Dae-Jeong Koo, Mi Yeon Lee, Sun Joon Moon, Hyemi Kwon, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
Endocrinology and Metabolism.2021; 36(4): 845. CrossRef
- Gender differences in midlife to later-life cumulative burden and variability of obesity measures and risk of all-cause and cause-specific mortality

- Clinical Study
- Relationships between Thigh and Waist Circumference, Hemoglobin Glycation Index, and Carotid Plaque in Patients with Type 2 Diabetes
- Myung Ki Yoon, Jun Goo Kang, Seong Jin Lee, Sung-Hee Ihm, Kap Bum Huh, Chul Sik Kim
- Endocrinol Metab. 2020;35(2):319-328. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.319
- 8,347 View
- 145 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
This study investigated the relationships of thigh and waist circumference with the hemoglobin glycation index (HGI) and carotid atherosclerosis in patients with type 2 diabetes.
Methods
This observational study included 3,075 Korean patients with type 2 diabetes, in whom anthropometric measurements and carotid ultrasonography were conducted. HGI was defined as the measured hemoglobin A1c (HbA1c) level minus the predicted HbA1c level, which was calculated using the linear relationship between HbA1c and fasting plasma glucose levels. Carotid atherosclerosis was defined as a clearly isolated focal plaque or focal wall thickening >50% of the surrounding intima-media thickness.
Results
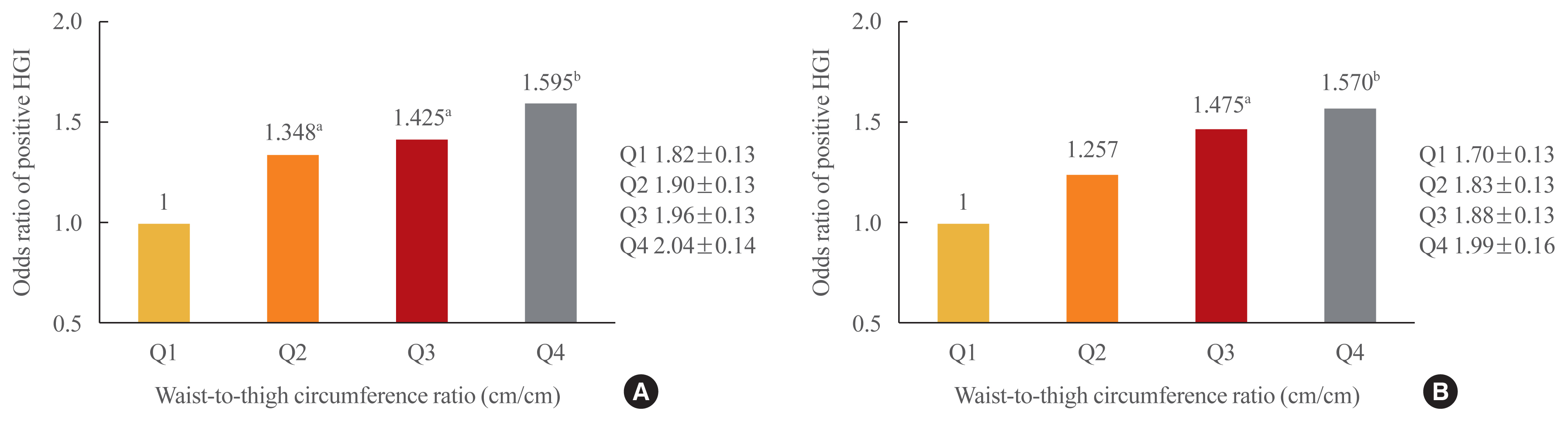
The frequency of a positive HGI decreased with increasing thigh circumference in men and increased with increasing waist circumference in women after adjusting for potential confounding variables. Thigh and waist circumference had a combined augmentative effect on the likelihood of positive HGI, which was dramatically higher in patients in higher waist-to-thigh ratio quartiles (adjusted odds ratios for the highest compared to the lowest quartile: 1.595 in men and 1.570 in women). Additionally, the larger the thigh circumference, the lower the risk of carotid atherosclerosis, although in women, this relationship lacked significance after adjustment for potential confounders.
Conclusion
HGI was associated with thigh circumference in men and waist circumference in women. In addition, the combination of low thigh circumference and high waist circumference was strongly associated with a higher HGI in Korean patients with type 2 diabetes. In particular, thigh circumference was associated with carotid atherosclerosis in men. However, further longitudinal studies are warranted. -
Citations
Citations to this article as recorded by- Association between hemoglobin glycation index and subclinical myocardial injury in the general population free from cardiovascular disease
Zhenwei Wang, Yihai Liu, Jing Xie, Nai-Feng Liu
Nutrition, Metabolism and Cardiovascular Diseases.2022; 32(2): 469. CrossRef - Association of Hemoglobin Glycation Index With Contrast-Induced Acute Kidney Injury in Patients Undergoing Coronary Angiography: A Retrospective Study
Zhezhe Chen, Duanbin Li, Maoning Lin, Hangpan Jiang, Tian Xu, Yu Shan, Guosheng Fu, Min Wang, Wenbin Zhang
Frontiers in Physiology.2022;[Epub] CrossRef - Associations of continuous glucose monitoring-assessed glucose variability with intima-media thickness and ultrasonic tissue characteristics of the carotid arteries: a cross-sectional analysis in patients with type 2 diabetes
Naohiro Taya, Naoto Katakami, Tomoya Mita, Yosuke Okada, Satomi Wakasugi, Hidenori Yoshii, Toshihiko Shiraiwa, Akihito Otsuka, Yutaka Umayahara, Kayoko Ryomoto, Masahiro Hatazaki, Tetsuyuki Yasuda, Tsunehiko Yamamoto, Masahiko Gosho, Iichiro Shimomura, Hi
Cardiovascular Diabetology.2021;[Epub] CrossRef
- Association between hemoglobin glycation index and subclinical myocardial injury in the general population free from cardiovascular disease

- Obesity and Metabolism
- Myths about Insulin Resistance: Tribute to Gerald Reaven
- Sun H. Kim, Fahim Abbasi
- Endocrinol Metab. 2019;34(1):47-52. Published online March 21, 2019
- DOI: https://doi.org/10.3803/EnM.2019.34.1.47
- 6,732 View
- 143 Download
- 3 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Gerald Reaven was often called the “father of insulin resistance.” On the 1-year anniversary of his death in 2018, we challenge three myths associated with insulin resistance: metformin improves insulin resistance; measurement of waist circumference predicts insulin resistance better than body mass index; and insulin resistance causes weight gain. In this review, we highlight Reaven's relevant research that helped to dispel these myths associated with insulin resistance.
-
Citations
Citations to this article as recorded by- Assessment of Antidiabetic and Anti-Inflammatory Activities of Carissa carandas Linn Extract: In Vitro and In Vivo Study
Manaschanok Lailerd, Thiri Wai Linn, Narissara Lailerd, Duangporn Amornlerdpison, Arisa Imsumran
Applied Sciences.2023; 13(11): 6454. CrossRef - Association of primary allostatic load mediators and metabolic syndrome (MetS): A systematic review
Francis Osei, Andrea Block, Pia-Maria Wippert
Frontiers in Endocrinology.2022;[Epub] CrossRef - Anthropometric indices and the risk of incident sudden cardiac death among adults with and without diabetes: over 15 years of follow-up in The Tehran Lipid and Glucose Study
Seyyed Saeed Moazzeni, Seyed Saeed Tamehri Zadeh, Samaneh Asgari, Fereidoun Azizi, Farzad Hadaegh
Diabetology & Metabolic Syndrome.2021;[Epub] CrossRef - Metabolic Syndrome or Insulin Resistance: Evolution, Controversies and Association With Cardiovascular Disease Risk
Arun K. Chopra
Indian Journal of Clinical Cardiology.2020; 1(2): 77. CrossRef
- Assessment of Antidiabetic and Anti-Inflammatory Activities of Carissa carandas Linn Extract: In Vitro and In Vivo Study

- Clinical Study
- Waist Circumference as a Marker of Obesity Is More Predictive of Coronary Artery Calcification than Body Mass Index in Apparently Healthy Korean Adults: The Kangbuk Samsung Health Study
- Jongsin Park, Eun Seo Lee, Da Young Lee, Jihyun Kim, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki-Won Oh, Sung-Woo Park, Eun-Jung Rhee
- Endocrinol Metab. 2016;31(4):559-566. Published online December 20, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.4.559
- 4,565 View
- 38 Download
- 33 Web of Science
- 30 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background We aimed to assess the risk for coronary artery calcification (CAC) according to groups subdivided by body mass index (BMI) and waist circumference (WC) in apparently healthy Korean adults.
Methods Thirty-three thousand four hundred and thirty-two participants (mean age, 42 years) in a health screening program were divided into three groups according to BMI: <23 kg/m2 (normal), 23 to 25 kg/m2 (overweight), and >25 kg/m2 (obese). In addition, the participants were divided into two groups according to WC. Coronary artery calcium score (CACS) was measured with multi-detector computed tomography in all participants. Presence of CAC was defined as CACS >0.
Results When logistic regression analysis was performed with the presence of CAC as the dependent variable, the risk for CAC increased as BMI increased after adjusting for confounding variables (1.102 [95% confidence interval (CI), 1.000 to 1.216]; 1.284 [95% CI, 1.169 to 1.410]; in the overweight and obese groups vs. the normal weight group). When the participants were divided into six groups according to BMI and WC, the subjects with BMI and WC in the obese range showed the highest risk for CAC (1.321 [95% CI, 1.194 to 1.461]) and those with BMI in the overweight range and WC in the obese range showed the second highest risk for CAC (1.235 [95% CI, 1.194 to 1.461]).
Conclusion Participants with obesity defined by both BMI and WC showed the highest risk for CAC. Those with BMIs in the overweight range but with WC in the obese range showed the second highest risk for CAC, suggesting that WC as a marker of obesity is more predictive of CAC than BMI.
-
Citations
Citations to this article as recorded by- Relationship Between Blood Group and
Obesity Reduction Through Diet Among
Adults of Urban Bihar
Vidya, Rahul Singh
Journal of Health Management.2024;[Epub] CrossRef - Association of Coronary Artery Calcium Density and Volume With Predicted Atherosclerotic Cardiovascular Disease Risk and Cardiometabolic Risk Factors in South Asians: The Mediators of Atherosclerosis in South Asians Living in America (MASALA) Study
Mahmoud Al Rifai, Alka M. Kanaya, Namratha R Kandula, Jaideep Patel, Mouaz H. Al-Mallah, Matthew Budoff, Miguel Cainzos-Achirica, Michael H. Criqui, Salim S. Virani
Current Problems in Cardiology.2023; 48(4): 101105. CrossRef - Body weight at age 20 and in midlife is more important than weight gain for coronary atherosclerosis: Results from SCAPIS
Göran Bergström, Annika Rosengren, Elin Bacsovics Brolin, John Brandberg, Kerstin Cederlund, Gunnar Engström, Jan E. Engvall, Maria J. Eriksson, Isabel Gonçalves, Emil Hagström, Stefan K. James, Tomas Jernberg, Mikael Lilja, Martin Magnusson, Anders Perss
Atherosclerosis.2023; 373: 46. CrossRef - Weight gain with age and coronary atherosclerosis: Only the tip of a deadly iceberg
Isabelle Lemieux, Jean-Pierre Després
Atherosclerosis.2023; 373: 55. CrossRef - Central obesity and its associated factors among cancer patients at the University of Gondar Comprehensive Specialized Hospital, Northwest Ethiopia
Meseret Derbew Molla, Haileab Fekadu Wolde, Ephrem Tafesse Teferi, Anteneh Ayelign Kibret
Frontiers in Oncology.2023;[Epub] CrossRef - Added value of waist circumference to body mass index for predicting fracture risk in obesity: a prospective study from the CARTaGENE cohort
Anne-Frédérique Turcotte, Sonia Jean, Suzanne N. Morin, Fabrice Mac-Way, Claudia Gagnon
Archives of Osteoporosis.2023;[Epub] CrossRef - Prevalence and significance of risk enhancing biomarkers in the United States population at intermediate risk for atherosclerotic disease
Gloria L. Vega, Jijia Wang, Scott M. Grundy
Journal of Clinical Lipidology.2022; 16(1): 66. CrossRef - Pericardial fat, thoracic peri-aortic adipose tissue, and systemic inflammatory marker in nonalcoholic fatty liver and abdominal obesity phenotype
Chun-Ho Yun, Jing-Rong Jhuang, Meng-Ting Tsou
Scientific Reports.2022;[Epub] CrossRef - Central Obesity and Associated Factors Among Urban Adults in Dire Dawa Administrative City, Eastern Ethiopia
Ephrem Israel, Kalkidan Hassen, Melese Markos, Kiber Wolde, Behailu Hawulte
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2022; Volume 15: 601. CrossRef - Gender-Based Association of Coronary Artery Calcification and Framingham Risk Score With Non-alcoholic Fatty Liver Disease and Abdominal Obesity in Taiwanese Adults, a Cross-Sectional Study
Meng-Ting Tsou, Jau-Yuan Chen
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Joint Associations of Obesity and Cardiorespiratory Fitness With Coronary Artery Calcium Composition
Sae Young Jae, Hyun Jeong Kim, Kyung Hyun Lee, Setor K. Kunutsor, Kevin S. Heffernan, Yoon-Ho Choi, Mira Kang
Journal of Cardiopulmonary Rehabilitation and Prevention.2022; 42(3): 202. CrossRef - Proposing new body mass index and waist circumference cut-offs based on cardiometabolic risks for a Central Asia population: A feasibility study
Aknur Kali, Arnur Gusmanov, Marat Aripov, Mei-Yen Chan
Frontiers in Endocrinology.2022;[Epub] CrossRef - New Model for Predicting the Presence of Coronary Artery Calcification
Samel Park, Min Hong, HwaMin Lee, Nam-jun Cho, Eun-Young Lee, Won-Young Lee, Eun-Jung Rhee, Hyo-Wook Gil
Journal of Clinical Medicine.2021; 10(3): 457. CrossRef - Obesity and Cardiovascular Disease: A Scientific Statement From the American Heart Association
Tiffany M. Powell-Wiley, Paul Poirier, Lora E. Burke, Jean-Pierre Després, Penny Gordon-Larsen, Carl J. Lavie, Scott A. Lear, Chiadi E. Ndumele, Ian J. Neeland, Prashanthan Sanders, Marie-Pierre St-Onge
Circulation.2021;[Epub] CrossRef - Association Between Obesity and Blood Pressure in Common Korean People
Nam Lyong Kang
Vascular Health and Risk Management.2021; Volume 17: 371. CrossRef - Prevalence of abdominal obesity and its association with cardiovascular risk among the adult population in Burkina Faso: findings from a nationwide cross-sectional study
Kadari Cisse, Sékou Samadoulougou, Mady Ouedraogo, Seni Kouanda, Fati Kirakoya-Samadoulougou
BMJ Open.2021; 11(7): e049496. CrossRef - Association between obesity and risk of fracture, bone mineral density and bone quality in adults: A systematic review and meta-analysis
Anne-Frédérique Turcotte, Sarah O’Connor, Suzanne N. Morin, Jenna C. Gibbs, Bettina M. Willie, Sonia Jean, Claudia Gagnon, Tuan Van Nguyen
PLOS ONE.2021; 16(6): e0252487. CrossRef - Association of Body Weight Variability with Adverse Cardiovascular Outcomes in Patients with Pre-Dialysis Chronic Kidney Disease
Sang Heon Suh, Tae Ryom Oh, Hong Sang Choi, Chang Seong Kim, Eun Hui Bae, Sue K. Park, Yong-Soo Kim, Yeong Hoon Kim, Kyu Hun Choi, Kook-Hwan Oh, Seong Kwon Ma, Soo Wan Kim
Nutrients.2021; 13(10): 3381. CrossRef - Associations among Obesity Degree, Glycemic Status, and Risk of Heart Failure in 9,720,220 Korean Adults
Eun-Jung Rhee, Hyemi Kwon, Se Eun Park, Kyung-Do Han, Yong-Gyu Park, Yang-Hyun Kim, Won-Young Lee
Diabetes & Metabolism Journal.2020; 44(4): 592. CrossRef - The effects of supplementation with L-arginine on anthropometric indices and body composition in overweight or obese subjects: A systematic review and meta-analysis
Mohammad Zeinali Khosroshahi, Omid Asbaghi, Sajjad Moradi, Mahnaz Rezaei kelishadi, Mojtaba Kaviani, Mahnaz Mardani, Cyrus Jalili
Journal of Functional Foods.2020; 71: 104022. CrossRef - Effect of Exercises and Diet Intervention in Pregnancy on Postpartum Weight Retention and Obesity Markers: Findings in Indian Women
Alka Pawalia, Sivachidambaram Kulandaivelan, Vikram Singh Yadav
Journal of Women's Health Physical Therapy.2020; 44(3): 123. CrossRef Magnitude of Central Obesity and its Associated Factors Among Adults in Urban Areas of Northwest Ethiopia
Meseret Derbew Molla, Haileab Fekadu Wolde, Asmamaw Atnafu
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2020; Volume 13: 4169. CrossRef- Is the coronary artery calcium score the first-line tool for investigating patients with severe hypercholesterolemia?
Sandra Kutkienė, Žaneta Petrulionienė, Aleksandras Laucevičius, Rimantė Čerkauskienė, Vytautas Kasiulevičius, Artūras Samuilis, Virginija Augaitienė, Aurelija Gedminaitė, Gintarė Bieliauskienė, Akvilė Šaulytė-Mikulskienė, Justina Staigytė, Emilija Petruli
Lipids in Health and Disease.2019;[Epub] CrossRef - Letter: Association of Z-Score of the Log-Transformed A Body Shape Index with Cardiovascular Disease in People Who Are Obese but Metabolically Healthy: The Korea National Health and Nutrition Examination Survey 2007-2010 (J Obes Metab Syndr 2018;27:158-65
Eun-Jung Rhee
Journal of Obesity & Metabolic Syndrome.2019; 28(2): 139. CrossRef - Lower Leg Fat Depots Are Associated with Albuminuria Independently of Obesity, Insulin Resistance, and Metabolic Syndrome (Korea National Health and Nutrition Examination Surveys 2008 to 2011)
Eugene Han, Nan Hee Cho, Mi Kyung Kim, Hye Soon Kim
Diabetes & Metabolism Journal.2019; 43(4): 461. CrossRef - Abdominal obesity increases metabolic risk factors in non-obese adults: a Hungarian cross-sectional study
Anita Lukács, Edina Horváth, Zsuzsanna Máté, Andrea Szabó, Katalin Virág, Magor Papp, János Sándor, Róza Ádány, Edit Paulik
BMC Public Health.2019;[Epub] CrossRef - Association between thyroid hormone levels, body composition and insulin resistance in euthyroid subjects with normal thyroid ultrasound: The Kangbuk Samsung Health Study
Hyemi Kwon, Jung‐Hwan Cho, Da Young Lee, Se Eun Park, Cheol‐Young Park, Won‐Young Lee, Ki‐Won Oh, Sung‐Woo Park, Eun‐Jung Rhee
Clinical Endocrinology.2018; 89(5): 649. CrossRef - Being Metabolically Healthy, the Most Responsible Factor for Vascular Health
Eun-Jung Rhee
Diabetes & Metabolism Journal.2018; 42(1): 19. CrossRef - Effects of lobeglitazone, a novel thiazolidinedione, on adipose tissue remodeling and brown and beige adipose tissue development in db/db mice
G Kim, Y-h Lee, M R Yun, J-Y Lee, E G Shin, B-W Lee, E S Kang, B-S Cha
International Journal of Obesity.2018; 42(3): 542. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef
- Relationship Between Blood Group and
Obesity Reduction Through Diet Among
Adults of Urban Bihar

- Clinical Study
- Association of Waist-Height Ratio with Diabetes Risk: A 4-Year Longitudinal Retrospective Study
- Yoon Jeong Son, Jihyun Kim, Hye-Jeong Park, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki-Won Oh, Sung-Woo Park, Eun-Jung Rhee
- Endocrinol Metab. 2016;31(1):127-133. Published online March 16, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.1.127
- 4,363 View
- 37 Download
- 26 Web of Science
- 24 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Waist-to-height ratio (WHtR) is an easy and inexpensive adiposity index that reflects central obesity. In this study, we examined the association of various baseline adiposity indices, including WHtR, with the development of diabetes over 4 years of follow-up in apparently healthy Korean individuals.
Methods A total of 2,900 nondiabetic participants (mean age, 44.3 years; 2,078 men) in a health screening program, who repeated the medical check-up in 2005 and 2009, were recruited. Subjects were divided into two groups according to development of diabetes after 4 years. The cut-off values of baseline body mass index (BMI), waist circumference (WC), and WHtR for the development of diabetes over 4 years were calculated. The sensitivity, specificity, and mean area under the receiver operator characteristic curve (AUROC) of each index were assessed. The odds ratio (OR) for diabetes development was analyzed for each of the three baseline adiposity indices.
Results During the follow-up period, 101 new cases (3.5%) of diabetes were diagnosed. The cut-off WHtR value for diabetes development was 0.51. Moreover, WHtR had the highest AUROC value for diabetes development among the three adiposity indices (0.716, 95% confidence interval [CI], 0.669 to 0.763; 0.702, 95% CI, 0.655 to 0.750 for WC; 0.700, 95% CI, 0.651 to 0.750 for BMI). After adjusting for confounding variables, the ORs of WHtR and WC for diabetes development were 1.95 (95% CI, 1.14 to 3.34) and 1.96 (95% CI, 1.10 to 3.49), respectively. No significant differences were observed between the two groups regarding BMI.
Conclusion Increased baseline WHtR and WC correlated with the development of diabetes after 4 years. WHtR might be a useful screening measurement to identify individuals at high risk for diabetes.
-
Citations
Citations to this article as recorded by- Comparison of waist circumference and waist‐to‐height ratio as predictors of clustering of cardiovascular risk factors among middle‐aged people in rural Khanh Hoa, Vietnam
Rachana Manandhar Shrestha, Thuy Thi Phuong Pham, Shohei Yamamoto, Chau Que Nguyen, Ami Fukunaga, Phan Cong Danh, Masahiko Hachiya, Huy Xuan Le, Hung Thai Do, Tetsuya Mizoue, Yosuke Inoue
American Journal of Human Biology.2024;[Epub] CrossRef - Novel anthropometric indices for predicting type 2 diabetes mellitus
Erfan Sadeghi, Alireza Khodadadiyan, Seyed Ali Hosseini, Sayed Mohsen Hosseini, Ashraf Aminorroaya, Massoud Amini, Sara Javadi
BMC Public Health.2024;[Epub] CrossRef - Body Composition and Cardiovascular Risk: A Study of Polish Military Flying Personnel
Agata Gaździńska, Stefan Gaździński, Paweł Jagielski, Paweł Kler
Metabolites.2023; 13(10): 1102. CrossRef - Cues of pregnancy decrease female physical attractiveness for males
Pavol Prokop, Martina Zvaríková, Milan Zvarík, Peter Fedor
Current Psychology.2022; 41(2): 697. CrossRef - Waist-to-height ratio has a stronger association with cardiovascular risks than waist circumference, waist-hip ratio and body mass index in type 2 diabetes
Jiang-Feng Ke, Jun-Wei Wang, Jun-Xi Lu, Zhi-Hui Zhang, Yun Liu, Lian-Xi Li
Diabetes Research and Clinical Practice.2022; 183: 109151. CrossRef - Diagnostic accuracy of anthropometric indices for discriminating elevated blood pressure in pediatric population: a systematic review and a meta-analysis
Jun-Min Tao, Wei Wei, Xiao-Yang Ma, Ying-Xiang Huo, Meng-Die Hu, Xiao-Feng Li, Xin Chen
BMC Pediatrics.2022;[Epub] CrossRef - The utilization of BMI in patients with high WHtR as to cardiovascular risk
Meliha Melin UYGUR
Journal of Health Sciences and Medicine.2022; 5(4): 1133. CrossRef - Assessment of obesity indices for prediction of hyperglycemia in adult population of Varanasi (Uttar Pradesh), India
Neha Rai, Hanjabam Barun Sharma, Renu Kumari, Jyotsna Kailashiya
Indian Journal of Physiology and Pharmacology.2021; 64: 195. CrossRef - Waist-to-height ratio and metabolic phenotype compared to the Matsuda index for the prediction of insulin resistance
Katharina Lechner, Benjamin Lechner, Alexander Crispin, Peter E. H. Schwarz, Helene von Bibra
Scientific Reports.2021;[Epub] CrossRef - Waist-to-Height Ratio (WHtR) in Predicting Coronary Artery Disease Compared to Body Mass Index and Waist Circumference in a Single Center from Saudi Arabia
Mostafa Q. Alshamiri, Faisal Mohd A Habbab, Saad Saeed AL-Qahtani, Khalil Abdullah Alghalayini, Omar Mohammed Al-Qattan, Fayez El-shaer, Anne Knowlton
Cardiology Research and Practice.2020; 2020: 1. CrossRef - A simple cut-off for waist-to-height ratio (0·5) can act as an indicator for cardiometabolic risk: recent data from adults in the Health Survey for England
Sigrid Gibson, Margaret Ashwell
British Journal of Nutrition.2020; 123(6): 681. CrossRef - Glucose Levels as a Mediator of the Detrimental Effect of Abdominal Obesity on Relative Handgrip Strength in Older Adults
Miguel Ángel Pérez-Sousa, Jesús del Pozo-Cruz, Carlos A. Cano-Gutiérrez, Atilio J. Ferrebuz, Carolina Sandoval-Cuellar, Mikel Izquierdo, Paula A. Hernández-Quiñonez, Robinson Ramírez-Vélez
Journal of Clinical Medicine.2020; 9(8): 2323. CrossRef Abnormal Glucose Metabolism and Associated Risk Factors Among Adults in Mekelle City, Ethiopia
Gebremedhin Gebreegziabiher, Tefera Belachew, Dessalegn Tamiru
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2020; Volume 13: 4017. CrossRefAnthropometric Indexes for Predicting High Blood Pressure in Vietnamese Adults: A Cross-Sectional Study
Quan Nguyen Minh, Minh Hoang Nguyen Vo
Integrated Blood Pressure Control.2020; Volume 13: 181. CrossRef- Relation between Baseline Height and New Diabetes Development: A Nationwide Population-Based Study
Eun-Jung Rhee, Jung-Hwan Cho, Hyemi Kwon, Se-Eun Park, Jin-Hyung Jung, Kyung-Do Han, Yong-Gyu Park, Yang-Hyun Kim, Won-Young Lee
Diabetes & Metabolism Journal.2019; 43(6): 794. CrossRef - Issues in Measuring and Interpreting Diet and Its Contribution to Obesity
Rachael M. Taylor, Rebecca L. Haslam, Tracy L. Burrows, Kerith R. Duncanson, Lee M. Ashton, Megan E. Rollo, Vanessa A. Shrewsbury, Tracy L. Schumacher, Clare E. Collins
Current Obesity Reports.2019; 8(2): 53. CrossRef - Assessment of the validity of multiple obesity indices compared with obesity-related co-morbidities
Jaeeun Myung, Kyung Yoon Jung, Tae Hyun Kim, Euna Han
Public Health Nutrition.2019; : 1. CrossRef - Profiles of body mass index and blood pressure among young adults categorised by waist-to-height ratio cut-offs in Shandong, China
Ying-xiu Zhang, Shu-rong Wang
Annals of Human Biology.2019; 46(5): 409. CrossRef - Air Pollution Has a Significant Negative Impact on Intentional Efforts to Lose Weight: A Global Scale Analysis
Morena Ustulin, So Young Park, Sang Ouk Chin, Suk Chon, Jeong-taek Woo, Sang Youl Rhee
Diabetes & Metabolism Journal.2018; 42(4): 320. CrossRef - Being Metabolically Healthy, the Most Responsible Factor for Vascular Health
Eun-Jung Rhee
Diabetes & Metabolism Journal.2018; 42(1): 19. CrossRef - Waist-to-height ratio index for predicting incidences of hypertension: the ARIRANG study
Jung Ran Choi, Sang Baek Koh, Eunhee Choi
BMC Public Health.2018;[Epub] CrossRef - Comparison of various anthropometric indices for the identification of a predictor of incident hypertension: the ARIRANG study
J. R. Choi, S. V. Ahn, J. Y. Kim, S. B. Koh, E. H. Choi, G. Y. Lee, Y. E. Jang
Journal of Human Hypertension.2018; 32(4): 294. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - THE ASSESMENT OF RELATION BETWEEN WAIST/HEIGHT RATIO AND TYPE 2 DIABETES RISK AMONG NURSING STUDENTS
Ceren Gezer
Journal of Food and Health Science.2017; : 141. CrossRef
- Comparison of waist circumference and waist‐to‐height ratio as predictors of clustering of cardiovascular risk factors among middle‐aged people in rural Khanh Hoa, Vietnam

- Obesity and Metabolism
- Increased Risk of Diabetes Development in Subjects with the Hypertriglyceridemic Waist Phenotype: A 4-Year Longitudinal Study
- Ki Joong Han, Shin Yeoung Lee, Nam Hee Kim, Hyun Beom Chae, Tae Hoon Lee, Choel Min Jang, Kyung Mo Yoo, Hae Jung Park, Min Kyung Lee, Won Seon Jeon, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki-Won Oh, Sung-Woo Park, Eun-Jung Rhee
- Endocrinol Metab. 2014;29(4):514-521. Published online December 29, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.4.514
- 4,547 View
- 30 Download
- 21 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The hypertriglyceridemic waist (HTGW) phenotype is a simple and inexpensive screening parameter to identify people at increased risk of cardiovascular disease. We evaluated whether the HTGW phenotype predicts diabetes in urban Korean adults.
Methods A total of 2,900 nondiabetic subjects (mean age 44.3 years), comprising 2,078 males (71.7%) and 822 females (28.3%) who underwent annual medical check-ups at our center between January 2005 and December 2009, were recruited. The subjects were divided into four groups according to baseline serum triglyceride (TG) level and waist circumference (WC): normal WC-normal TG (NWNT) level, normal WC-high TG level, enlarged WC-normal TG level, and enlarged WC-high TG (EWHT) level. High serum TG level was defined as ≥150 mg/dL and enlarged WC was defined as ≥90 cm for men and ≥85 cm for women. New cases of diabetes were determined according to questionnaires filled in by participants and the diagnostic criteria of the American Diabetes Association. Cox proportional hazards model analysis was used to assess the association of HTGW phenotype with the incidence of diabetes.
Results A total of 101 (3.5%) new diabetes cases were diagnosed during the study period. The EWHT group had a higher incidence of diabetes (8.3%) compared with the NWNT group (2.2%). The adjusted hazard ratio for diabetes for subjects with the EWHT phenotype at baseline was 4.113 (95% confidence interval [CI], 2.397 to 7.059) after adjustment for age, and 2.429 (95% CI, 1.370 to 4.307) after adjustment for age, sex, total cholesterol, systolic blood pressure, and alcohol drinking history. It was attenuated by inclusion of baseline fasting glucose level in the model.
Conclusion Subjects with the HTGW phenotype showed the highest risk of incident diabetes. This tool could be useful for identifying individuals at high risk of diabetes.
-
Citations
Citations to this article as recorded by- Triglyceridemic Waist Phenotypes as Risk Factors for Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis
Fiorella E. Zuzunaga-Montoya, Víctor Juan Vera-Ponce
International Journal of Statistics in Medical Research.2024; 13: 19. CrossRef - Association between hypertriglyceridemic-waist phenotype and circadian syndrome risk: a longitudinal cohort study
Li-Kun Hu, Yu-Hong Liu, Kun Yang, Ning Chen, Lin-Lin Ma, Yu-Xiang Yan
Hormones.2023; 22(3): 457. CrossRef - Caracterización del fenotipo de cintura hipertrigliceridémica en pacientes con diabetes mellitus tipo 2 en España: un estudio epidemiológico
I. Miñambres, J. Sánchez-Hernández, G. Cuixart, A. Sánchez-Pinto, J. Sarroca, A. Pérez
Revista Clínica Española.2021; 221(10): 576. CrossRef - Association of “hypertriglyceridemic waist” with increased 5-year risk of subclinical atherosclerosis in a multi-ethnic population: a prospective cohort study
Peyman Namdarimoghaddam, Adeleke Fowokan, Karin H. Humphries, G. B. John Mancini, Scott Lear
BMC Cardiovascular Disorders.2021;[Epub] CrossRef - Characterization of the hypertriglyceridemic waist phenotype in patients with type 2 diabetes mellitus in Spain: an epidemiological study
I. Miñambres, J. Sánchez-Hernandez, G. Cuixart, A. Sánchez-Pinto, J. Sarroca, A. Pérez
Revista Clínica Española (English Edition).2021; 221(10): 576. CrossRef - Association between Hypertriglyceridemic-Waist Phenotype and Risk of Type 2 Diabetes Mellitus in Middle-Aged and Older Chinese Population: A Longitudinal Cohort Study
Dezhong Chen, Ziyun Liang, Huimin Sun, Ciyong Lu, Weiqing Chen, Harry H. X. Wang, Vivian Yawei Guo
International Journal of Environmental Research and Public Health.2021; 18(18): 9618. CrossRef - Metabolic Syndrome, and Particularly the Hypertriglyceridemic-Waist Phenotype, Increases Breast Cancer Risk, and Adiponectin Is a Potential Mechanism: A Case–Control Study in Chinese Women
Yujuan Xiang, Wenzhong Zhou, Xuening Duan, Zhimin Fan, Shu Wang, Shuchen Liu, Liyuan Liu, Fei Wang, Lixiang Yu, Fei Zhou, Shuya Huang, Liang Li, Qiang Zhang, Qinye Fu, Zhongbing Ma, Dezong Gao, Shude Cui, Cuizhi Geng, Xuchen Cao, Zhenlin Yang, Xiang Wang,
Frontiers in Endocrinology.2020;[Epub] CrossRef - Hypertriglyceridemic Waist Phenotype and Lipid Accumulation Product: Two Comprehensive Obese Indicators of Waist Circumference and Triglyceride to Predict Type 2 Diabetes Mellitus in Chinese Population
Minrui Xu, Mingtao Huang, Deren Qiang, Jianxin Gu, Yong Li, Yingzi Pan, Xingjuan Yao, Wenchao Xu, Yuan Tao, Yihong Zhou, Hongxia Ma, Ulrike Rothe
Journal of Diabetes Research.2020; 2020: 1. CrossRef - Prevalence and relationship of hypertriglyceridaemic–waist phenotype and type 2 diabetes mellitus among a rural adult Chinese population
Yong-Cheng Ren, Yu Liu, Xi-Zhuo Sun, Bing-Yuan Wang, Yi Liu, Hu Ni, Yang Zhao, Dechen Liu, Xuejiao Liu, Dongdong Zhang, Feiyan Liu, Cheng Cheng, Leilei Liu, Xu Chen, Qionggui Zhou, Ming Zhang, Dongsheng Hu
Public Health Nutrition.2019; 22(8): 1361. CrossRef - Hypertriglyceridemic waist phenotype and abnormal glucose metabolism: a system review and meta-analysis
Chun-Ming Ma, Xiao-Li Liu, Na Lu, Rui Wang, Qiang Lu, Fu-Zai Yin
Endocrine.2019; 64(3): 469. CrossRef - Superior Role of Waist Circumference to Body-Mass Index in the Prediction of Cardiometabolic Risk in Dyslipidemic Patients
Ľ. Cibičková, K. Langová, H. Vaverková, J. Lukeš, N. Cibiček
Physiological Research.2019; : 931. CrossRef - Being Metabolically Healthy, the Most Responsible Factor for Vascular Health
Eun-Jung Rhee
Diabetes & Metabolism Journal.2018; 42(1): 19. CrossRef - Letter: Utility of the Visceral Adiposity Index and Hypertriglyceridemic Waist Phenotype for Predicting Incident Hypertension (Endocrinol Metab 2017;32:221-9, Mohsen Janghorbani et al.)
Eun-Jung Rhee
Endocrinology and Metabolism.2017; 32(3): 396. CrossRef - The Relationship between Hypertriglyceridemic Waist Phenotype and Early Diabetic Nephropathy in Type 2 Diabetes
Chun-Ming Ma, Rui Wang, Xiao-Li Liu, Na Lu, Qiang Lu, Fu-Zai Yin
Cardiorenal Medicine.2017; 7(4): 295. CrossRef - The Association of Hypertriglyceridemic Waist Phenotype with Chronic Kidney Disease and Its Sex Difference: A Cross-Sectional Study in an Urban Chinese Elderly Population
Jing Zeng, Miao Liu, Lei Wu, Jianhua Wang, Shanshan Yang, Yiyan Wang, Yao Yao, Bin Jiang, Yao He
International Journal of Environmental Research and Public Health.2016; 13(12): 1233. CrossRef - Prevalence of hypertriglyceridemic waist and association with risk of type 2 diabetes mellitus: a meta‐analysis
Yongcheng Ren, Xinping Luo, Chongjian Wang, Lei Yin, Chao Pang, Tianping Feng, Bingyuan Wang, Lu Zhang, Linlin Li, Xiangyu Yang, Hongyan Zhang, Jingzhi Zhao, Dongsheng Hu
Diabetes/Metabolism Research and Reviews.2016; 32(4): 405. CrossRef - Utility of hypertriglyceridemic waist phenotype for predicting incident type 2 diabetes: The Isfahan Diabetes Prevention Study
Mohsen Janghorbani, Masoud Amini
Journal of Diabetes Investigation.2016; 7(6): 860. CrossRef - βig-h3 Represses T-Cell Activation in Type 1 Diabetes
Maeva Patry, Romain Teinturier, Delphine Goehrig, Cornelia Zetu, Doriane Ripoche, In-San Kim, Philippe Bertolino, Ana Hennino
Diabetes.2015; 64(12): 4212. CrossRef - Hypertriglyceridemic Waist – a Simple Clinical Tool to Detect Cardiometabolic Risk: Comparison With Harmonized Definition of Metabolic Syndrome
H. VAVERKOVÁ, D. KARÁSEK, D. NOVOTNÝ, M. HALENKA, J. ORSÁG, L. SLAVÍK
Physiological Research.2015; : S385. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Changes in Metabolic Health Status Over Time and Risk of Developing Type 2 Diabetes
Seung-Hwan Lee, Hae Kyung Yang, Hee-Sung Ha, Jin-Hee Lee, Hyuk-Sang Kwon, Yong-Moon Park, Hyeon-Woo Yim, Moo-Il Kang, Won-Chul Lee, Ho-Young Son, Kun-Ho Yoon
Medicine.2015; 94(40): e1705. CrossRef
- Triglyceridemic Waist Phenotypes as Risk Factors for Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis

- Obesity and Metabolism
- Optimal Waist Circumference Cutoff Values for the Diagnosis of Abdominal Obesity in Korean Adults
- Yeong Sook Yoon, Sang Woo Oh
- Endocrinol Metab. 2014;29(4):418-426. Published online December 29, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.4.418
- 5,885 View
- 70 Download
- 65 Web of Science
- 71 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Abdominal obesity is associated closely with insulin resistance, diabetes, and cardiovascular disease. Waist circumference (WC) is a useful surrogate marker commonly used for abdominal adiposity. The determination of WC cutoff levels is important in the prevention and treatment of obesity, type 2 diabetes, and related cardiovascular diseases. Recent epidemiological evidence suggested that appropriate optimal cutoffs for Koreans ranged over 80 to 89.8 cm in males and 76.1 to 86.5 cm in females. We analyzed the data from two large cohorts using receiver operating characteristic curve analysis with the incidences of diabetes, hypertension, dyslipidemia, cerebrovascular disease, myocardial infarct, angina, coronary artery disease, and multiple metabolic risk factors as outcome variables. Optimal WC cutoff points for Koreans were 85 cm in males and 80 cm in females. However, considering the prevalence of abdominal obesity and the health costs for its prevention and management, 90 cm in males and 85 cm in females are probably more appropriate thresholds for abdominal obesity. These values may be modified once better research is performed through prospective studies using representative populations, common health outcomes, and proper analytical approaches.
-
Citations
Citations to this article as recorded by- The prevalence and factors associated with sarcopenia in Thai older adults: A systematic review and meta-analysis
Phatcharaphon Whaikid, Noppawan Piaseu
International Journal of Nursing Sciences.2024; 11(1): 31. CrossRef - Machine learning analysis for the association between breast feeding and metabolic syndrome in women
Jue Seong Lee, Eun-Saem Choi, Hwasun Lee, Serhim Son, Kwang-Sig Lee, Ki Hoon Ahn
Scientific Reports.2024;[Epub] CrossRef - Association between waist circumference change after smoking cessation and incidence of hypertension in Korean adults
H.J. Lee, J.W. Choi
Public Health.2024; 229: 73. CrossRef - Surrogate indices of insulin resistance using the Matsuda index as reference in adult men—a computational approach
Víctor Antonio Malagón-Soriano, Andres Julian Ledezma-Forero, Cristian Felipe Espinel-Pachon, Álvaro Javier Burgos-Cárdenas, Maria Fernanda Garces, Gustavo Eduardo Ortega-Ramírez, Roberto Franco-Vega, Jhon Jairo Peralta-Franco, Luis Miguel Maldonado-Acost
Frontiers in Endocrinology.2024;[Epub] CrossRef - Waist circumference and end‐stage renal disease based on glycaemic status: National Health Insurance Service data 2009–2018
Yun Kyung Cho, Ji Hye Huh, Shinje Moon, Yoon Jung Kim, Yang‐Hyun Kim, Kyung‐do Han, Jun Goo Kang, Seong Jin Lee, Sung‐Hee Ihm
Journal of Cachexia, Sarcopenia and Muscle.2023; 14(1): 585. CrossRef - Simple anthropometric measures to predict visceral adipose tissue area in middle-aged Indonesian men
Sahat Basana Romanti Ezer Matondang, Bennadi Adiandrian, Komang Shary Karismaputri, Cicilia Marcella, Joedo Prihartono, Dicky Levenus Tahapary, Yosuke Yamada
PLOS ONE.2023; 18(1): e0280033. CrossRef - Sleep Quality in Women with Premenstrual Syndrome Is Associated with Metabolic Syndrome-Related Variables
Hyejin Chun, Miae Doo
Healthcare.2023; 11(10): 1492. CrossRef - Gender, Age and Clinical Characteristics of Older Adults with High-Risk of Obstructive Sleep Apnea Assessed by the STOP-Bang Questionnaire
Gyu Lee Kim, Yun Jin Kim, Jeong Gyu Lee, Yu Hyeon Yi, Young Jin Tak, Seung Hun Lee, Young Jin Ra, Sang Yeoup Lee, Young Hye Cho, Eun Ju Park, Youngin Lee, Jung In Choi, Sae Rom Lee, Ryuk Jun Kwon, Soo Min Son
Korean Journal of Clinical Geriatrics.2023; 24(2): 72. CrossRef - Body Composition and Cardiovascular Risk: A Study of Polish Military Flying Personnel
Agata Gaździńska, Stefan Gaździński, Paweł Jagielski, Paweł Kler
Metabolites.2023; 13(10): 1102. CrossRef - Associated Factors with Changes of Metabolic Abnormalities among General Population in COVID-19 Pandemic
Eunjoo Kwon, Eun-Hee Nah, Suyoung Kim, Seon Cho, Hyeran Park
Korean Journal of Health Promotion.2023; 23(2): 55. CrossRef - Effects of Pharmacoacupuncture for Obesity: A Systematic Review and Meta-Analysis
Seyun Kim, Mi-Yeon Song, Won-Seok Chung, Hyungsuk Kim, Woo-Chul Shin, Junhyuk Kang, Joonwon Seo, Sangwoo Seo, Seung Ho Yu, Jung-Hyun Lim, Su-Hwan Ji, Jae-Heung Cho
Journal of Korean Medicine for Obesity Research.2023; 23(2): 112. CrossRef - Associations Between Elevated Growth Differentiation Factor-15 and Sarcopenia Among Community-dwelling Older Adults
Miji Kim, Jeremy D Walston, Chang Won Won, Anne B Newman
The Journals of Gerontology: Series A.2022; 77(4): 770. CrossRef - The association of obesity with thyroid carcinoma risk
Xiao‐Ni Ma, Cheng‐Xu Ma, Li‐Jie Hou, Song‐Bo Fu
Cancer Medicine.2022; 11(4): 1136. CrossRef - A Longitudinal Retrospective Observational Study on Obesity Indicators and the Risk of Impaired Fasting Glucose in Pre- and Postmenopausal Women
Myung Ji Nam, Hyunjin Kim, Yeon Joo Choi, Kyung-Hwan Cho, Seon Mee Kim, Yong-Kyun Roh, Kyungdo Han, Jin-Hyung Jung, Yong-Gyu Park, Joo-Hyun Park, Do-Hoon Kim
Journal of Clinical Medicine.2022; 11(10): 2795. CrossRef - Association of Metabolic Health and Central Obesity with the Risk of Thyroid Cancer: Data from the Korean Genome and Epidemiology Study
Dung N. Nguyen, Jin Hee Kim, Mi Kyung Kim
Cancer Epidemiology, Biomarkers & Prevention.2022; 31(3): 543. CrossRef - Interaction of polygenic variants specific for abdominal obesity risk with energy metabolism in large Korean cohorts
Sunmin Park
Nutrition Bulletin.2022; 47(3): 307. CrossRef - Effects of Oral Health Behavior and Mental Health on Metabolic Syndrome in Korean Adults
Jin-Ah Jung, Hye-Won Cheon, Sang-Eun Moon, Sun-Hwa Hong
Journal of Dental Hygiene Science.2022; 22(2): 90. CrossRef - Relation of Dietary n-3 and n-6 Fatty Acid Intakes to Metabolic Syndrome in Middle-Aged People Depending on the Level of HbA1c: A Review of National Health and Nutrition Survey Data from 2014 to 2016
Seo-Woo Park, Do-Yeong Kim, Gyeong-Tae Bak, Dae-Sung Hyun, Sung-Kyung Kim
Medicina.2022; 58(8): 1017. CrossRef - Synergistic Interaction between Hyperuricemia and Abdominal Obesity as a Risk Factor for Metabolic Syndrome Components in Korean Population
Min Jin Lee, Ah Reum Khang, Yang Ho Kang, Mi Sook Yun, Dongwon Yi
Diabetes & Metabolism Journal.2022; 46(5): 756. CrossRef - Risk of Carotid Atherosclerosis in Subjects with Prediabetes Overlapping Metabolic Syndrome
Seol A Jang, Kyoung Min Kim, Seok Won Park, Chul Sik Kim
Metabolic Syndrome and Related Disorders.2022; 20(10): 599. CrossRef - Association of high body mass index, waist circumference, and body fat percentage with sarcopenia in older women
Myung Chul Yoo, Chang Won Won, Yunsoo Soh
BMC Geriatrics.2022;[Epub] CrossRef - Relationship between low skeletal muscle mass, sarcopenic obesity and left ventricular diastolic dysfunction in Korean adults
Jee Hee Yoo, Sung Woon Park, Ji Eun Jun, Sang‐Man Jin, Kyu Yeon Hur, Moon‐Kyu Lee, Mira Kang, Gyuri Kim, Jae Hyeon Kim
Diabetes/Metabolism Research and Reviews.2021;[Epub] CrossRef - Association of Early-Life Mental Health With Biomarkers in Midlife and Premature Mortality
George B. Ploubidis, G. David Batty, Praveetha Patalay, David Bann, Alissa Goodman
JAMA Psychiatry.2021; 78(1): 38. CrossRef - A clinical evaluation of noninvasive and contactless radiofrequency technique in the treatment of abdominal fat
Jie Qin, Meng‐er Guo, Xue‐gang Xu, Chao Zhang, Cheng‐qian Yu, Yuan‐hong Li, Hong‐duo Chen
Journal of Cosmetic Dermatology.2021; 20(9): 2765. CrossRef - Exercise training and burdock root (Arctium lappa L.) extract independently improve abdominal obesity and sex hormones in elderly women with metabolic syndrome
Min-Seong Ha, Jang Soo Yook, Minchul Lee, Kazuya Suwabe, Woo-Min Jeong, Jae-Jun Kwak, Hideaki Soya
Scientific Reports.2021;[Epub] CrossRef - Effect of body mass index and abdominal obesity on mortality after percutaneous coronary intervention: a nationwide, population-based study
Woo-Hyuk Song, Eun Hui Bae, Jeong Cheon Ahn, Tae Ryom Oh, Yong-Hyun Kim, Jin Seok Kim, Sun-Won Kim, Soo Wan Kim, Kyung-Do Han, Sang-Yup Lim
The Korean Journal of Internal Medicine.2021; 36(Suppl 1): S90. CrossRef - Individual and Synergistic Relationships of Low Muscle Mass and Low Muscle Function with Depressive Symptoms in Korean Older Adults
Youngyun Jin, Seamon Kang, Hyunsik Kang
International Journal of Environmental Research and Public Health.2021; 18(19): 10129. CrossRef - Association between Metabolic Syndrome and the Number of Remaining Teeth in Postmenopausal Women: A Cross-Sectional Analysis Using the Korean National Health and Nutritional Examination Survey
Jeong-In Kim, Choong-Ho Choi, Ki-Ho Chung
Journal of Clinical Medicine.2021; 10(20): 4759. CrossRef - No Association between Metabolic Syndrome and Periodontitis in Korean Postmenopausal Women
Jeong-In Kim, Choong-Ho Choi, Ki-Ho Chung
International Journal of Environmental Research and Public Health.2021; 18(21): 11110. CrossRef - Relative Lean Body Mass and Waist Circumference for the Identification of Metabolic Syndrome in the Korean General Population
Eunjoo Kwon, Eun-Hee Nah, Suyoung Kim, Seon Cho
International Journal of Environmental Research and Public Health.2021; 18(24): 13186. CrossRef - SVM-based waist circumference estimation using Kinect
Dasom Seo, Euncheol Kang, Yu-mi Kim, Sun-Young Kim, Il-Seok Oh, Min-Gul Kim
Computer Methods and Programs in Biomedicine.2020; 191: 105418. CrossRef - Effects of abdominal obesity on the association between air pollution and kidney function
Su-Min Jeong, Jin-Ho Park, Hyun-Jin Kim, Hyuktae Kwon, Seo Eun Hwang
International Journal of Obesity.2020; 44(7): 1568. CrossRef - Effect of sarcopenic obesity on deterioration of physical function in the elderly
Hyun Ho Kong, Chang Won Won, Won Kim
Archives of Gerontology and Geriatrics.2020; 89: 104065. CrossRef - Effects of low skeletal muscle mass and sarcopenic obesity on albuminuria: a 7-year longitudinal study
Jee Hee Yoo, Gyuri Kim, Sung Woon Park, Min Sun Choi, Jiyeon Ahn, Sang-Man Jin, Kyu Yeon Hur, Moon-Kyu Lee, Mira Kang, Jae Hyeon Kim
Scientific Reports.2020;[Epub] CrossRef A Novel Indicator of Children’s Lipid Accumulation Product Associated with Impaired Fasting Glucose in Chinese Children and Adolescents
Yongting Yuan, Hong Xie, Lili Sun, Bangxuan Wang, Li Zhang, Hui Han, Rongying Yao, Yehuan Sun, Lianguo Fu
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2020; Volume 13: 1653. CrossRef- The Association between the Ratio of Energy Intake to Basal Metabolic Rate and Physical Activity to Sarcopenia: Using the Korea National Health and Nutrition Examination Surveys (2008–2011)
Yu Jin Cho, Mi Hee Cho, Bomi Han, Minji Park, Seolah Bak, Minseon Park
Korean Journal of Family Medicine.2020; 41(3): 167. CrossRef - Waist circumference as a vital sign in clinical practice: a Consensus Statement from the IAS and ICCR Working Group on Visceral Obesity
Robert Ross, Ian J. Neeland, Shizuya Yamashita, Iris Shai, Jaap Seidell, Paolo Magni, Raul D. Santos, Benoit Arsenault, Ada Cuevas, Frank B. Hu, Bruce A. Griffin, Alberto Zambon, Philip Barter, Jean-Charles Fruchart, Robert H. Eckel, Yuji Matsuzawa, Jean-
Nature Reviews Endocrinology.2020; 16(3): 177. CrossRef - Lung function as a predictor of incident type 2 diabetes in community-dwelling adults: A longitudinal finding over 12 years from the Korean Genome and Epidemiology Study
J.H. Lee, H.S. Lee, Y.J. Lee
Diabetes & Metabolism.2020; 46(5): 392. CrossRef - Sex- and age-specific effects of energy intake and physical activity on sarcopenia
Yu Jin Cho, Youn-Hee Lim, Jae Moon Yun, Hyung-Jin Yoon, Minseon Park
Scientific Reports.2020;[Epub] CrossRef - Protective effect of smoking cessation on subsequent myocardial infarction and ischemic stroke independent of weight gain: A nationwide cohort study
Jung-Hwan Cho, Hye-Mi Kwon, Se-Eun Park, Jin-Hyung Jung, Kyung-Do Han, Yong-Gyu Park, Yang-Hyun Kim, Eun-Jung Rhee, Won-Young Lee, Michael Cummings
PLOS ONE.2020; 15(7): e0235276. CrossRef - Optimal Cutoff Values for Anthropometric Adiposity Measures of Sri Lankan Adult Women
Nirmala Rathnayake, Gayani Alwis, Janaka Lenora, Sarath Lekamwasam
Journal of Obesity.2020; 2020: 1. CrossRef Differences in the Association Among the Vitamin D Concentration, Dietary Macronutrient Consumption, and Metabolic Syndrome Depending on Pre- and Postmenopausal Status in Korean Women: A Cross-Sectional Study
Hyejin Chun, Gi Dae Kim, Miae Doo
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2020; Volume 13: 3601. CrossRef- Patterns of change in cardiovascular risks of Korean male workers: a 10-year cohort analysis using the National Health Insurance Service–National Sample Cohort (NHIS-NSC) 2.0 database
Hosihn Ryu, Jiyeon Jung, Jihyun Moon
BMJ Open.2020; 10(11): e038446. CrossRef - Predictive Performance of Glycated Hemoglobin for Incident Diabetes Compared with Glucose Tolerance Test According to Central Obesity
Suji Yoo, Jaehoon Jung, Hosu Kim, Kyoung Young Kim, Soo Kyoung Kim, Jungwha Jung, Jong Ryeal Hahm, Jong Ha Baek
Endocrinology and Metabolism.2020; 35(4): 873. CrossRef - Metabolic Syndrome and Risk of Lung Cancer: An Analysis of Korean National Health Insurance Corporation Database
Sooim Sin, Chang-Hoon Lee, Sun Mi Choi, Kyung-Do Han, Jinwoo Lee
The Journal of Clinical Endocrinology & Metabolism.2020; 105(11): e4102. CrossRef - Association of body mass index with bladder cancer risk in men depends on abdominal obesity
Jin Bong Choi, Jung Ho Kim, Sung-Hoo Hong, Kyung-Do Han, U-Syn Ha
World Journal of Urology.2019; 37(11): 2393. CrossRef - Lower Leg Fat Depots Are Associated with Albuminuria Independently of Obesity, Insulin Resistance, and Metabolic Syndrome (Korea National Health and Nutrition Examination Surveys 2008 to 2011)
Eugene Han, Nan Hee Cho, Mi Kyung Kim, Hye Soon Kim
Diabetes & Metabolism Journal.2019; 43(4): 461. CrossRef - The Risk of Myocardial Infarction and Ischemic Stroke According to Waist Circumference in 21,749,261 Korean Adults: A Nationwide Population-Based Study
Jung-Hwan Cho, Eun-Jung Rhee, Se-Eun Park, Hyemi Kwon, Jin-Hyung Jung, Kyung-Do Han, Yong-Gyu Park, Hye Soon Park, Yang-Hyun Kim, Soon-Jib Yoo, Won-Young Lee
Diabetes & Metabolism Journal.2019; 43(2): 206. CrossRef - Association between Serum Gamma-Glutamyltransferase and Prevalence of Metabolic Syndrome Using Data from the Korean Genome and Epidemiology Study
Mi Young Lee, Dae Sung Hyon, Ji Hye Huh, Hae Kyung Kim, Sul Ki Han, Jang Young Kim, Sang Baek Koh
Endocrinology and Metabolism.2019; 34(4): 390. CrossRef - The Association between Obesity Phenotypes and Early Renal Function Decline in Adults without Hypertension, Dyslipidemia, and Diabetes
Jung In Choi, Young Hye Cho, Sang Yeoup Lee, Dong Wook Jeong, Jeong Gyu Lee, Yu Hyeon Yi, Young Jin Tak, Seung Hun Lee, Hye Rim Hwang, Eun Ju Park
Korean Journal of Family Medicine.2019; 40(3): 176. CrossRef - Sex differences in the association between asthma incidence and modifiable risk factors in Korean middle-aged and older adults: NHIS-HEALS 10-year cohort
Susan Park, Sun-Young Jung, Jin-Won Kwon
BMC Pulmonary Medicine.2019;[Epub] CrossRef - Plasma sphingomyelins increase in pre-diabetic Korean men with abdominal obesity
Seung-Soon Im, Hyeon Young Park, Jong Cheol Shon, In-Sung Chung, Ho Chan Cho, Kwang-Hyeon Liu, Dae-Kyu Song, Kyoung Heon Kim
PLOS ONE.2019; 14(3): e0213285. CrossRef - Estimating the Cutoff Points of Time-Dependent Risk Factors by Using Joint Modeling of Longitudinal and Time-to-Event Data: A 14-Year Follow-up Study—Tehran Lipid and Glucose Study
Nezhat Shakeri, Fereidoun Azizi
Asia Pacific Journal of Public Health.2019; 31(8): 728. CrossRef - Metabolic Obesity Phenotypes and Thyroid Cancer Risk: A Cohort Study
Hyemi Kwon, Yoosoo Chang, Ara Cho, Jiin Ahn, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki-Won Oh, Sung-Woo Park, Hocheol Shin, Seungho Ryu, Eun-Jung Rhee
Thyroid.2019; 29(3): 349. CrossRef - Trends and Cut-Point Changes in Obesity Parameters by Age Groups Considering Metabolic Syndrome
Hyung Jun Park, Young Ho Hong, Yun Jung Cho, Ji Eun Lee, Jae Moon Yun, Hyuktae Kwon, Sang Hyuck Kim
Journal of Korean Medical Science.2018;[Epub] CrossRef - Difference in prostate cancer incidence around sixty years: effects of age and metabolic diseases
Jin Bong Choi, Jung Ho Kim, Sung‐Hoo Hong, Kyung‐Do Han, U‐Syn Ha
Cancer Medicine.2018; 7(6): 2736. CrossRef - The Association of Low Back Pain with Obesity and Abdominal Obesity among Koreans Aged 50 Years or More
Eun Young Choi
Korean Journal of Health Promotion.2018; 18(3): 119. CrossRef - Association between oral health and colorectal adenoma in a screening population
Donghyoun Lee, Kyung Uk Jung, Hyung Ook Kim, Hungdai Kim, Ho-Kyung Chun
Medicine.2018; 97(37): e12244. CrossRef - An association of metabolic syndrome and chronic kidney disease from a 10-year prospective cohort study
Ji Hye Huh, Dhananjay Yadav, Jae Seok Kim, Jung-Woo Son, Eunhee Choi, Seong Hwan Kim, Chol Shin, Ki-Chul Sung, Jang Young Kim
Metabolism.2017; 67: 54. CrossRef - Anatomic fat depots and cardiovascular risk: a focus on the leg fat using nationwide surveys (KNHANES 2008–2011)
Eugene Han, Yong-ho Lee, Byung-Wan Lee, Eun Seok Kang, In-Kyu Lee, Bong-Soo Cha
Cardiovascular Diabetology.2017;[Epub] CrossRef - Association between Body Weight Changes and Menstrual Irregularity: The Korea National Health and Nutrition Examination Survey 2010 to 2012
Kyung Min Ko, Kyungdo Han, Youn Jee Chung, Kun-Ho Yoon, Yong Gyu Park, Seung-Hwan Lee
Endocrinology and Metabolism.2017; 32(2): 248. CrossRef - Low muscle mass and risk of type 2 diabetes in middle-aged and older adults: findings from the KoGES
Jang Won Son, Seong Su Lee, Sung Rae Kim, Soon Jib Yoo, Bong Yun Cha, Ho Young Son, Nam H. Cho
Diabetologia.2017; 60(5): 865. CrossRef - Safety and efficacy of a non-contact radiofrequency device for body contouring in Asians
Dong Hye Suh, Chang Min Kim, Sang Jun Lee, Hyunjoo Kim, Suk Keu Yeom, Hwa Jung Ryu
Journal of Cosmetic and Laser Therapy.2017; 19(2): 89. CrossRef - Arterial stiffness and its association with clustering of metabolic syndrome risk factors
Wanda R. P. Lopes-Vicente, Sara Rodrigues, Felipe X. Cepeda, Camila Paixão Jordão, Valéria Costa-Hong, Akothirene C. B. Dutra-Marques, Jefferson C. Carvalho, Maria Janieire N. N. Alves, Luiz A. Bortolotto, Ivani C. Trombetta
Diabetology & Metabolic Syndrome.2017;[Epub] CrossRef - Associations of sitting time and occupation with metabolic syndrome in South Korean adults: a cross-sectional study
Jin Young Nam, Juyoung Kim, Kyung Hee Cho, Young Choi, Jaewoo Choi, Jaeyong Shin, Eun-Cheol Park
BMC Public Health.2016;[Epub] CrossRef - Associations of Obesity and Dyslipidemia with Intake of Sodium, Fat, and Sugar among Koreans: a Qualitative Systematic Review
Yoon Jung Kang, Hye Won Wang, Se Young Cheon, Hwa Jung Lee, Kyung Mi Hwang, Hae Seong Yoon
Clinical Nutrition Research.2016; 5(4): 290. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Ambient Temperature and Prevalence of Obesity: A Nationwide Population-Based Study in Korea
Hae Kyung Yang, Kyungdo Han, Jae-Hyoung Cho, Kun-Ho Yoon, Bong-Yun Cha, Seung-Hwan Lee, David Meyre
PLOS ONE.2015; 10(11): e0141724. CrossRef - Acupoint Catgut Embedding for Obesity: Systematic Review and Meta-Analysis
Taipin Guo, Yulan Ren, Jun Kou, Jing Shi, Sun Tianxiao, Fanrong Liang
Evidence-Based Complementary and Alternative Medicine.2015; 2015: 1. CrossRef - Elderly men over 65 years of age with late-onset hypogonadism benefit as much from testosterone treatment as do younger men
Farid Saad, Aksam Yassin, Ahmad Haider, Gheorghe Doros, Louis Gooren
Korean Journal of Urology.2015; 56(4): 310. CrossRef - Administration of Hwang-Ryun-Haedok-tang, a Herbal Complex, for Patients With Abdominal Obesity: A Case Series
Seungwon Kwon, WooSang Jung, A Ri Byun, SangKwan Moon, KiHo Cho, KyoungHo Shin
EXPLORE.2015; 11(5): 401. CrossRef
- The prevalence and factors associated with sarcopenia in Thai older adults: A systematic review and meta-analysis

- Obesity and Metabolism
- The Impact of Different Anthropometric Measures on Sustained Normotension, White Coat Hypertension, Masked Hypertension, and Sustained Hypertension in Patients with Type 2 Diabetes
- Baris Afsar
- Endocrinol Metab. 2013;28(3):199-206. Published online September 13, 2013
- DOI: https://doi.org/10.3803/EnM.2013.28.3.199
- 3,079 View
- 44 Download
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Many studies have aimed to determine whether body mass index (BMI), waist circumference (WC), or waist to hip ratio (WHR) best predicts hypertension in diabetic patients, with conflicting results. However, no study has examined the specific relationship between these anthropometric parameters with sustained normotension (SNT), white coat hypertension (WCHT), masked hypertension (MHT), and sustained hypertension (SHT) based on office and ambulatory blood pressure (BP) measurements in these patients.
Methods Patients with newly diagnosed type 2 diabetes underwent the following procedures: history taking, measurements of anthropometric parameters, office and ambulatory BP measurements, physical examination, laboratory analysis, and random and 24-hour urine analysis.
Results In total, there were 65 dippers and 37 nondipper patients. None of the anthropometric parameters were different between the dippers and the nondippers. There were 25 patients with SNT, 32 with WCHT, seven with MHT, and 38 with SHT. A comparison of anthropometric parameters between these four groups of patients showed that WC (
P =0.016) and WHR (P =0.015) were different among all groups. According to regression analysis, only BMI was independently related with MHT (odds ratio [OR], 1.373,P =0.022), whereas only WC has been associated with SHT (OR, 1.321,P =0.041).Conclusion Among anthropometric parameters, only WC and WHR were different in SNT, WCHT, MHT, and SHT in newly diagnosed patients with type 2 diabetes.
-
Citations
Citations to this article as recorded by- Masked arterial hypertension: what is known and what expected to be learned?
A.Yu. Gorshkov, A.A. Fedorovich, O.M. Drapkina
Profilakticheskaya meditsina.2020; 23(6): 143. CrossRef - Association of the conicity index with diabetes and hypertension in Brazilian women
Mirelli Dantas Andrade, Maria Camila Pruper de Freitas, Alyne Mayumi Sakumoto, Caroline Pappiani, Samantha Caesar de Andrade, Viviane Laudelino Vieira, Nágila Raquel Teixeira Damasceno
Archives of Endocrinology and Metabolism.2016; 60(5): 436. CrossRef - Brief Review of Articles in 'Endocrinology and Metabolism' in 2013
Won-Young Lee
Endocrinology and Metabolism.2014; 29(3): 251. CrossRef
- Masked arterial hypertension: what is known and what expected to be learned?

- Relationship with Serum Adiponectin Concentrations and Obesity in Korean Children.
- Hyoun Ah Kim, Hyoung Suk Lee, Chul Sik Kim, Chul Woo Ahn, Yoon Sok Chung, Kwan Woo Lee, Kap Bum Huh, Dae Jung Kim
- J Korean Endocr Soc. 2003;18(5):473-480. Published online October 1, 2003
- 1,162 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Adiponectin is an adipocytokine that is highly specific to adipose tissue. In contrast to other adipocytokine, the adiponectin levels are decreased in obesity and/or type 2 diabetes. There are few studies regarding the correlation between the adiponectin concentration and obesity in children. Thus, whether the serum adiponectin concentrations are associated with adiposity in children was investigated. METHODS: One hundred and sixty four subjects were selected from the participants in an ongoing study on the relationship between birth weight and insulin resistance in children. The current weights, heights, body fat percentages, waist circumferences, blood pressures, lipid profiles and insulin resistance, by the HOMA method, were measured in all the subjects. The serum adiponectin concentrations were determined by a validated sandwich ELISA, using a human adiponectin-specific antibody. RESULTS: The serum adiponectin concentration was negatively correlated with the body mass index, waist circumference, systolic blood pressure, insulin resistance by HOMA and serum triglycerides, and positively correlated with the serum HDL cholesterol level. The serum adiponectin concentrations in the boys were significantly lower than in the girls. In a multiple regression analysis, the serum adiponectin concentration was strongly associated with waist circumference and gender. CONCLUSION: It is concluded that there was an inverse relationship between the serum adiponectin concentration and abdominal adiposity in children. However, further studies on independent gender differences on adiponectin are needed.


 KES
KES

 First
First Prev
Prev



