Search
- Page Path
- HOME > Search
- Adrenal gland
- A Contemporary Approach to the Diagnosis and Management of Adrenal Insufficiency
- Suranut Charoensri, Richard J. Auchus
- Endocrinol Metab. 2024;39(1):73-82. Published online January 22, 2024
- DOI: https://doi.org/10.3803/EnM.2024.1894
- 2,492 View
- 245 Download
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Adrenal insufficiency (AI) can be classified into three distinct categories based on its underlying causes: primary adrenal disorders, secondary deficiencies in adrenocorticotropin, or hypothalamic suppression from external factors, most commonly glucocorticoid medications used for anti-inflammatory therapy. The hallmark clinical features of AI include fatigue, appetite loss, unintentional weight loss, low blood pressure, and hyponatremia. Individuals with primary AI additionally manifest skin hyperpigmentation, hyperkalemia, and salt craving. The diagnosis of AI is frequently delayed due to the non-specific symptoms and signs early in the disease course, which poses a significant challenge to its early detection prior to an adrenal crisis. Despite the widespread availability of lifesaving glucocorticoid medications for decades, notable challenges persist, particularly in the domains of timely diagnosis while simultaneously avoiding misdiagnosis, patient education for averting adrenal crises, and the determination of optimal replacement therapies. This article reviews recent advancements in the contemporary diagnostic strategy and approaches to optimal treatment for AI.

- Miscellaneous
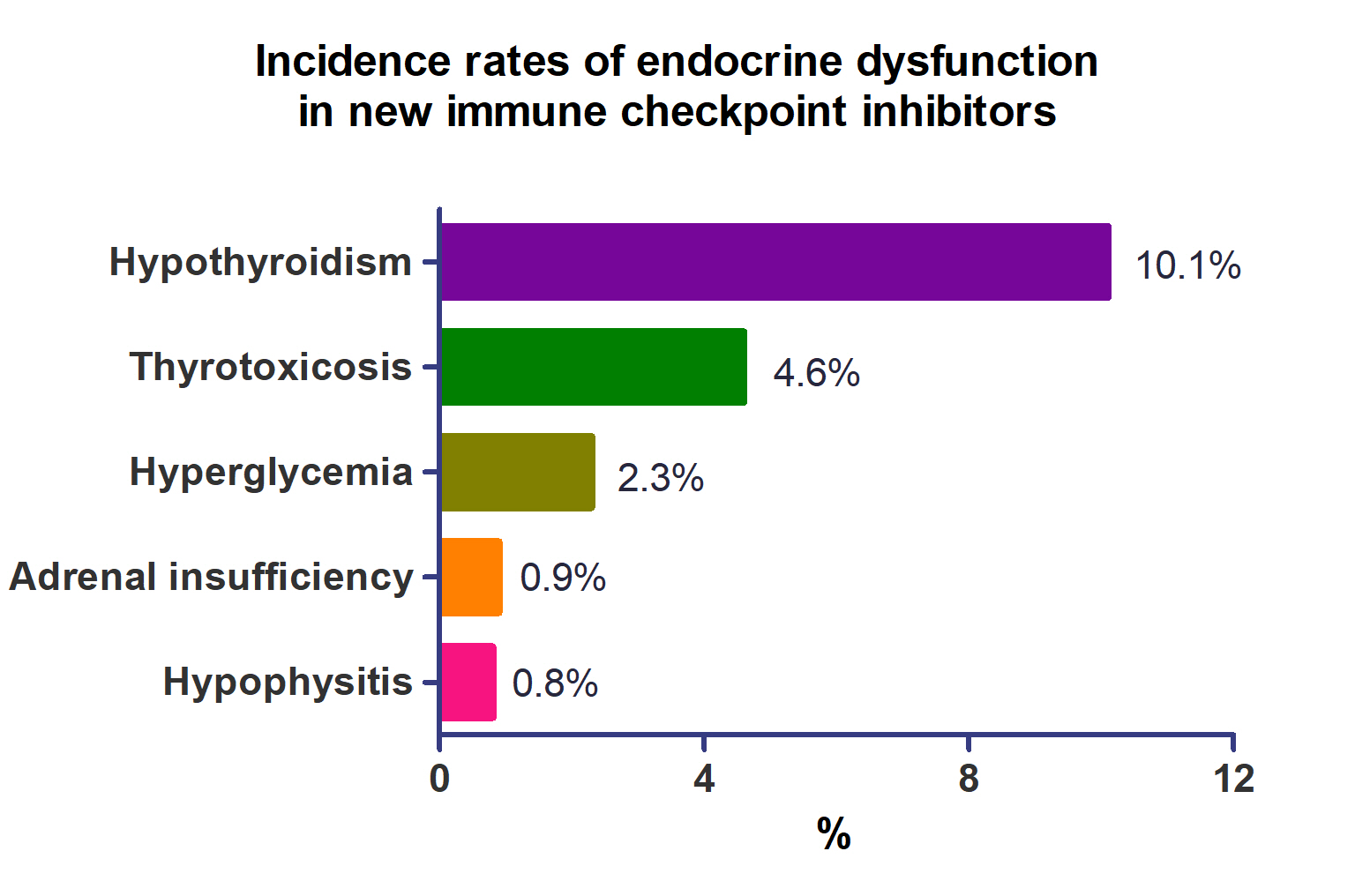
- Incidence of Endocrine-Related Dysfunction in Patients Treated with New Immune Checkpoint Inhibitors: A Meta-Analysis and Comprehensive Review
- Won Sang Yoo, Eu Jeong Ku, Eun Kyung Lee, Hwa Young Ahn
- Endocrinol Metab. 2023;38(6):750-759. Published online November 13, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1785
- 1,443 View
- 121 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
This study investigated the incidence of endocrine immune-related adverse events (irAEs) for recently developed immune checkpoint inhibitor (ICI) drugs.
Methods
We collected studies on newly developed ICI drugs using PubMed/Medline, Embase, and Cochrane Library from inception through January 31, 2023. Among ICI drugs, nivolumab, pembrolizumab, and ipilimumab were excluded from the new ICI drugs because many papers on endocrine-related side effects have already been published.
Results
A total of 44,595 patients from 177 studies were included in this analysis. The incidence of hypothyroidism was 10.1% (95% confidence interval [CI], 8.9% to 11.4%), thyrotoxicosis was 4.6% (95% CI, 3.8% to 5.7%), hypophysitis was 0.8% (95% CI, 0.5% to 1.1%), adrenal insufficiency was 0.9% (95% CI, 0.7% to 1.1%), and hyperglycemia was 2.3% (95% CI, 1.6% to 3.4%). Hypothyroidism and thyrotoxicosis occurred most frequently with programmed cell death protein-1 (PD-1) inhibitors (13.7% and 7.5%, respectively). The rate of endocrine side effects for the combination of a programmed death-ligand 1 inhibitor (durvalumab) and cytotoxic T lymphocyte-associated antigen 4 inhibitor (tremelimumab) was higher than that of monotherapy. In a meta-analysis, the combination of tremelimumab and durvalumab had a 9- to 10-fold higher risk of pituitary and adrenal-related side effects than durvalumab alone.
Conclusion
Newly developed PD-1 inhibitors had a high incidence of thyroid-related irAEs, and combined treatment with durvalumab and tremelimumab increased the risk of pituitary- and adrenal-related irAEs. Based on these facts, it is necessary to predict the endocrine side effects corresponding to each ICI drug, diagnose and treat them appropriately, and try to reduce the morbidity and mortality of patients.

- Adrenal Gland
- Clinical and Technical Aspects in Free Cortisol Measurement
- Man Ho Choi
- Endocrinol Metab. 2022;37(4):599-607. Published online August 19, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1549

- 4,688 View
- 290 Download
- 9 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Accurate measurement of cortisol is critical in adrenal insufficiency as it reduces the risk associated with misdiagnosis and supports the optimization of stress dose. Comprehensive assays have been developed to determine the levels of bioactive free cortisol and their clinical and analytical efficacies have been extensively discussed because the level of total cortisol is affected by changes in the structure or circulating levels of corticoid-binding globulin and albumin, which are the main reservoirs of cortisol in the human body. Antibody-based immunoassays are routinely used in clinical laboratories; however, the lack of molecular specificity in cortisol assessment limits their applicability to characterize adrenocortical function. Improved specificity and sensitivity can be achieved by mass spectrometry coupled with chromatographic separation methods, which is a cutting-edge technology to measure individual as well as a panel of steroids in a single analytical run. The purpose of this review is to introduce recent advances in free cortisol measurement from the perspectives of clinical specimens and issues associated with prospective analytical technologies.
-
Citations
Citations to this article as recorded by- Highly Responsive Bioassay for Quantification of Glucocorticoids
Mathias Flensted Poulsen, Martin Overgaard, Christian Brix Folsted Andersen, Andreas Lodberg
Analytical Chemistry.2024; 96(5): 2000. CrossRef - An LC-MS/MS Method for the Simultaneous Quantification of Insulin, Cortisol, Glucagon-like Peptide 1, Ghrelin, and Osteocalcin
Zhichao Zhang, Hareem Siddiqi, Yu-Ping Huang, Shannon McClorry, Peng Ji, Daniela Barile, Carolyn M. Slupsky
Separations.2024; 11(2): 41. CrossRef - Determination of cortisol cut-off limits and steroid dynamics in the ACTH stimulation test: a comparative analysis using Roche Elecsys Cortisol II immunoassay and LC-MS/MS
Sema Okutan, Nanna Thurmann Jørgensen, Lars Engers Pedersen, Stina Willemoes Borresen, Linda Hilsted, Lennart Friis Hansen, Ulla Feldt-Rasmussen, Marianne Klose
Endocrine.2024;[Epub] CrossRef - Advancements in Cortisol Detection: From Conventional Methods to Next-Generation Technologies for Enhanced Hormone Monitoring
Visesh Vignesh, Bernardo Castro-Dominguez, Tony D. James, Julie M. Gamble-Turner, Stafford Lightman, Nuno M. Reis
ACS Sensors.2024;[Epub] CrossRef - Comparative analysis of salivary cortisol measurements using different assay methods in relation to serum-free cortisol measurement
Anna Lee, Sooah Jang, Sanghoo Lee, Hyun-Kyung Park, In-Young Kim, Ryunsup Ahn, Jeong-Ho Seok, Kyoung-Ryul Lee
Practical Laboratory Medicine.2024; 40: e00393. CrossRef - A dilute and shoot method for urinary free cortisol analysis by LC-MS/MS
Ying Shen, Xia Luo, Qing Guan, Liming Cheng
Journal of Chromatography B.2024; 1239: 124127. CrossRef - Osteopathic Manipulation as a Method of Cortisol Modification: A Systematic Review
Dylan Thibaut, Valentine Santarlas, Joseph Hoppes, Alejandra Vásquez-Castillo, Alexa Morrow, Eddie Oviedo, James Toldi
Cureus.2023;[Epub] CrossRef - Pitfalls in the Diagnosis and Management of Hypercortisolism (Cushing Syndrome) in Humans; A Review of the Laboratory Medicine Perspective
Kade C. Flowers, Kate E. Shipman
Diagnostics.2023; 13(8): 1415. CrossRef - Electrochemical sensors for cortisol detection: Principles, designs, fabrication, and characterisation
Gopi Karuppaiah, Min-Ho Lee, Shekhar Bhansali, Pandiaraj Manickam
Biosensors and Bioelectronics.2023; 239: 115600. CrossRef - The role of the hypothalamic-pituitary-adrenal axis in depression across the female reproductive lifecycle: current knowledge and future directions
Liisa Hantsoo, Kathleen M. Jagodnik, Andrew M. Novick, Ritika Baweja, Teresa Lanza di Scalea, Aysegul Ozerdem, Erin C. McGlade, Diana I. Simeonova, Sharon Dekel, Sara L. Kornfield, Michelle Nazareth, Sandra J. Weiss
Frontiers in Endocrinology.2023;[Epub] CrossRef - РІВЕНЬ СТРЕСУ В ДІТЕЙ ШКІЛЬНОГО ВІКУ З COVID-19
Г. А. Павлишин, О. І. Панченко
Здобутки клінічної і експериментальної медицини.2023; (4): 119. CrossRef - Corticotropin-stimulated steroid profiles to predict shock development and mortality in sepsis: From the HYPRESS study
Josef Briegel, Patrick Möhnle, Didier Keh, Johanna M. Lindner, Anna C. Vetter, Holger Bogatsch, Dorothea Lange, Sandra Frank, Ludwig C. Hinske, Djillali Annane, Michael Vogeser, Michael Bauer, Thorsten Brenner, Patrick Meybohm, Markus Weigand, Matthias Gr
Critical Care.2022;[Epub] CrossRef
- Highly Responsive Bioassay for Quantification of Glucocorticoids

- Miscellaneous
- COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
- Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim, the Committee of Clinical Practice Guideline of the Korean Endocrine Society
- Endocrinol Metab. 2021;36(4):757-765. Published online August 17, 2021
- DOI: https://doi.org/10.3803/EnM.2021.404
- 10,360 View
- 419 Download
- 19 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Since the first outbreak of coronavirus disease 2019 (COVID-19), ongoing efforts have been made to discover an efficacious vaccine against COVID-19 to combat the pandemic. In most countries, both mRNA and DNA vaccines have been administered, and their side effects have also been reported. The clinical course of COVID-19 and the effects of vaccination against COVID-19 are both influenced by patients’ health status and involve a systemic physiological response. In view of the systemic function of endocrine hormones, endocrine disorders themselves and the therapeutics used to treat them can influence the outcomes of vaccination for COVID-19. However, there are very limited data to support the development of clinical guidelines for patients with specific medical backgrounds based on large clinical trials. In the current severe circumstances of the COVID-19 pandemic, position statements made by clinical specialists are essential to provide appropriate recommendations based on both medical evidence and clinical experiences. As endocrinologists, we would like to present the medical background of COVID-19 vaccination, as well as precautions to prevent the side effects of COVID-19 vaccination in patients with specific endocrine disorders, including adrenal insufficiency, diabetes mellitus, osteoporosis, autoimmune thyroid disease, hypogonadism, and pituitary disorders.
-
Citations
Citations to this article as recorded by- COVID-19 mRNA vaccine may trigger subacute thyroiditis
Mehmet Sözen, Ömercan Topaloğlu, Berrin Çetinarslan, Alev Selek, Zeynep Cantürk, Emre Gezer, Damla Köksalan, Taner Bayraktaroğlu
Human Vaccines & Immunotherapeutics.2024; 17(12): 5120. CrossRef - The role of co-morbidities in the development of an AEFI after COVID-19 vaccination in a large prospective cohort with patient-reported outcomes in the Netherlands
C. Ouaddouh, J.W. Duijster, T. Lieber, F.P.A.M. van Hunsel
Expert Opinion on Drug Safety.2024; 23(3): 323. CrossRef - Thyroid dysfunction in COVID-19
David Tak Wai Lui, Chi Ho Lee, Yu Cho Woo, Ivan Fan Ngai Hung, Karen Siu Ling Lam
Nature Reviews Endocrinology.2024;[Epub] CrossRef - Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
Hyeyeon Moon, Sunghwan Suh, Mi Kyoung Park
Journal of Korean Medical Science.2023;[Epub] CrossRef - Prior immunization status of COVID-19 patients and disease severity: A multicenter retrospective cohort study assessing the different types of immunity
Javaria Aslam, Faisal Shahzad Khan, Muhammad Talha Haris, Hewad Hewadmal, Maryam Khalid, Mohammad Y. Alshahrani, Qurrat-ul-ain Aslam, Irrum Aneela, Urooj Zafar
Vaccine.2023; 41(2): 598. CrossRef - Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
Endocrinology and Metabolism.2023; 38(2): 253. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Inactivated SARS-CoV-2 vaccination does not disturb the clinical course of Graves’ disease: An observational cohort study
Shichen Xu, Huixin Yu, Xian Cheng, Jing Wu, Jiandong Bao, Li Zhang
Vaccine.2023; 41(38): 5648. CrossRef - Adrenal Crisis Associated With COVID-19 Vaccination in Patients With Adrenal Insufficiency
Yukako Kurematsu, Takako Mohri, Sadanori Okada, Yutaka Takahashi
JCEM Case Reports.2023;[Epub] CrossRef - Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study
İbrahim Mert Erbaş, İrem Ceren Erbaş, Gözde Akın Kağızmanlı, Kübra Yüksek Acinikli, Özge Besci, Korcan Demir, Ece Böber, Nurşen Belet, Ayhan Abacı
Journal of Clinical Research in Pediatric Endocrinology.2023; 15(3): 248. CrossRef - Neue Aspekte der Glukokortikoidsubstitution bei Nebennierenrindeninsuffizienz
Tina Kienitz, Gesine Meyer
Der Internist.2022; 63(1): 12. CrossRef - Endocrine Follow-up During Post-Acute COVID-19: Practical Recommendations Based on Available Clinical Evidence
Rimesh Pal, Ameya Joshi, Sanjay K. Bhadada, Mainak Banerjee, Suresh Vaikkakara, Satinath Mukhopadhyay
Endocrine Practice.2022; 28(4): 425. CrossRef - Safety of Inactivated and mRNA COVID-19 Vaccination Among Patients Treated for Hypothyroidism: A Population-Based Cohort Study
Xi Xiong, Carlos King Ho Wong, Ivan Chi Ho Au, Francisco Tsz Tsun Lai, Xue Li, Eric Yuk Fai Wan, Celine Sze Ling Chui, Esther Wai Yin Chan, Franco Wing Tak Cheng, Kristy Tsz Kwan Lau, Chi Ho Lee, Yu Cho Woo, David Tak Wai Lui, Ian Chi Kei Wong
Thyroid.2022; 32(5): 505. CrossRef - The New Entity of Subacute Thyroiditis amid the COVID-19 Pandemic: From Infection to Vaccine
Mihaela Popescu, Adina Ghemigian, Corina Maria Vasile, Andrei Costache, Mara Carsote, Alice Elena Ghenea
Diagnostics.2022; 12(4): 960. CrossRef - Adrenal Crisis Secondary to COVID-19 Vaccination in a Patient With Hypopituitarism
Nikolina Markovic, Anila Faizan, Chirag Boradia, Sridhar Nambi
AACE Clinical Case Reports.2022; 8(4): 171. CrossRef - The Effect of Inactivated SARS-CoV-2 Vaccines on TRAB in Graves’ Disease
LingHong Huang, ZhengRong Jiang, JingXiong Zhou, YuPing Chen, HuiBin Huang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Osteoporosis in Patients With Respiratory Diseases
Yue Ma, Shui Qiu, Renyi Zhou
Frontiers in Physiology.2022;[Epub] CrossRef - Pilot Findings on SARS-CoV-2 Vaccine-Induced Pituitary Diseases: A Mini Review from Diagnosis to Pathophysiology
Ach Taieb, El Euch Mounira
Vaccines.2022; 10(12): 2004. CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - No need of glucocorticoid dose adjustment in patients with adrenal insufficiency before COVID-19 vaccine
Tania Pilli, Cristina Dalmiglio, Gilda Dalmazio, Alfonso Sagnella, Raffaella Forleo, Lucia Brilli, Fabio Maino, Cristina Ciuoli, Maria Grazia Castagna
European Journal of Endocrinology.2022; 187(1): K7. CrossRef - Diabetes and COVID-19 Vaccination
Hae Dong Choi, Jun Sung Moon
The Journal of Korean Diabetes.2021; 22(4): 221. CrossRef
- COVID-19 mRNA vaccine may trigger subacute thyroiditis

- Miscellaneous
- Clinical Characteristics, Management, and Potential Biomarkers of Endocrine Dysfunction Induced by Immune Checkpoint Inhibitors
- Shintaro Iwama, Tomoko Kobayashi, Hiroshi Arima
- Endocrinol Metab. 2021;36(2):312-321. Published online April 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1007

- 5,482 View
- 267 Download
- 15 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Immune-related adverse events (irAEs) affecting the endocrine glands are among the most frequent irAEs induced by immune checkpoint inhibitors (ICIs) and include hypopituitarism, primary adrenal insufficiency, thyrotoxicosis, hypothyroidism, hypoparathyroidism, and type 1 diabetes mellitus. Since the incidence and clinical features of endocrine irAEs vary according to the ICI used, it is important to understand the characteristics of these irAEs and to manage each one appropriately. Since some endocrine irAEs, including adrenal crisis and diabetic ketoacidosis, are potentially life-threatening, predicting the risk of endocrine irAEs before their onset is critical. Several autoantibodies have been detected in patients who develop endocrine irAEs, among which anti-thyroid antibodies may be predictive biomarkers of thyroid dysfunction. In this review, we describe the clinical features of each endocrine irAE induced by ICIs and discuss their potential biomarkers, including autoantibodies.
-
Citations
Citations to this article as recorded by- Clinical characteristics and potential biomarkers of thyroid and pituitary immune-related adverse events
Tomoko Kobayashi, Shintaro Iwama, Hiroshi Arima
Endocrine Journal.2024; 71(1): 23. CrossRef - A case of rapidly progressive insulin-dependent diabetes mellitus without islet autoantibodies developed over two years after the first dose of nivolumab
Kota Nishihama, Yuko Okano, Chisa Inoue, Kanako Maki, Kazuhito Eguchi, Soichiro Tanaka, Atsuro Takeshita, Mei Uemura, Taro Yasuma, Toshinari Suzuki, Esteban C. Gabazza, Yutaka Yano
Diabetology International.2024;[Epub] CrossRef - Endocrinopathies Associated With Immune Checkpoint Inhibitor Use
Anupam Kotwal, Randol Kennedy, Nupur Kikani, Sonali Thosani, Whitney Goldner, Afreen Shariff
Endocrine Practice.2024;[Epub] CrossRef - Recovery from insulin dependence in immune checkpoint inhibitor‐associated diabetes mellitus: A case report
Marie Okubo, Yuji Hataya, Kanta Fujimoto, Toshio Iwakura, Naoki Matsuoka
Journal of Diabetes Investigation.2023; 14(1): 147. CrossRef - Case Report: A Rising Cause of New-Onset Endocrinopathies After Immunotherapy
Charity Tan, Sarah Hendricks, Kristina Hernandez, Martha Benavides, Rupinderjit Samra
The Journal for Nurse Practitioners.2023; 19(5): 104582. CrossRef - Risk of Thyroid Dysfunction in PD-1 Blockade Is Stratified by the Pattern of TgAb and TPOAb Positivity at Baseline
Xin Zhou, Shintaro Iwama, Tomoko Kobayashi, Masahiko Ando, Hiroshi Arima
The Journal of Clinical Endocrinology & Metabolism.2023; 108(10): e1056. CrossRef - Severe thyrotoxicosis induced by tislelizumab: a case report and literature review
Liman Huo, Chao Wang, Haixia Ding, Xuelian Shi, Bin Shan, Ruoying Zhou, Ping Liang, Juan Hou
Frontiers in Oncology.2023;[Epub] CrossRef - Life-Threatening Endocrinological Immune-Related Adverse Events of Immune Checkpoint Inhibitor Therapy
Aleksandra Basek, Grzegorz K. Jakubiak, Grzegorz Cieślar, Agata Stanek
Cancers.2023; 15(24): 5786. CrossRef - Increased Risk of Thyroid Dysfunction by PD-1 and CTLA-4 Blockade in Patients Without Thyroid Autoantibodies at Baseline
Shintaro Iwama, Tomoko Kobayashi, Yoshinori Yasuda, Takayuki Okuji, Masaaki Ito, Masahiko Ando, Xin Zhou, Ayana Yamagami, Takeshi Onoue, Yohei Kawaguchi, Takashi Miyata, Mariko Sugiyama, Hiroshi Takagi, Daisuke Hagiwara, Hidetaka Suga, Ryoichi Banno, Tets
The Journal of Clinical Endocrinology & Metabolism.2022; 107(4): e1620. CrossRef - Biomarkers and risk factors for the early prediction of immune-related adverse events: a review
Ying Zhang, Xiaoling Zhang, Weiling Li, Yunyi Du, Wenqing Hu, Jun Zhao
Human Vaccines & Immunotherapeutics.2022;[Epub] CrossRef - Immune Checkpoint Inhibitors as a Threat to the Hypothalamus–Pituitary Axis: A Completed Puzzle
Agnese Barnabei, Andrea Corsello, Rosa Maria Paragliola, Giovanni Maria Iannantuono, Luca Falzone, Salvatore Maria Corsello, Francesco Torino
Cancers.2022; 14(4): 1057. CrossRef - Elevated TSH Level, TgAb, and Prior Use of Ramucirumab or TKIs as Risk Factors for Thyroid Dysfunction in PD-L1 Blockade
Tomoko Kobayashi, Shintaro Iwama, Ayana Yamagami, Yoshinori Yasuda, Takayuki Okuji, Masaaki Ito, Xin Zhou, Masahiko Ando, Takeshi Onoue, Takashi Miyata, Mariko Sugiyama, Daisuke Hagiwara, Hidetaka Suga, Ryoichi Banno, Tetsunari Hase, Masahiro Morise, Taka
The Journal of Clinical Endocrinology & Metabolism.2022; 107(10): e4115. CrossRef - Preconditioning of the immune system modulates the response of papillary thyroid cancer to immune checkpoint inhibitors
Fabiana Pani, Yoshinori Yasuda, Sylvie T Rousseau, Kevin C Bermea, Solmaz Roshanmehr, Rulin Wang, Srinivasan Yegnasubramanian, Patrizio Caturegli, Luigi Adamo
Journal for ImmunoTherapy of Cancer.2022; 10(12): e005538. CrossRef - Survival benefit of endocrine dysfunction following immune checkpoint inhibitors for nonthyroidal cancers
Anupam Kotwal, Mabel Ryder
Current Opinion in Endocrinology, Diabetes & Obesity.2021; 28(5): 517. CrossRef
- Clinical characteristics and potential biomarkers of thyroid and pituitary immune-related adverse events

- Clinical Study
- Stimulated Salivary Cortisol as a Noninvasive Diagnostic Tool for Adrenal Insufficiency
- Yoon Ji Kim, Jung Hee Kim, A Ram Hong, Kyeong Seon Park, Sang Wan Kim, Chan Soo Shin, Seong Yeon Kim
- Endocrinol Metab. 2020;35(3):628-635. Published online September 22, 2020
- DOI: https://doi.org/10.3803/EnM.2020.707

- 5,822 View
- 201 Download
- 12 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Salivary cortisol is routinely used as a diagnostic test for Cushing syndrome. The diagnostic use of salivary cortisol for adrenal insufficiency (AI), however, is less established. We aimed to investigate the utility of morning basal and adrenocorticotropic hormone-stimulated salivary cortisol in diagnosing AI in Korean adults.
Methods
We prospectively included 120 subjects (female, n=70) from Seoul National University Hospital. AI was defined as a stimulated serum cortisol level of <496.8 nmol/L during the short Synacthen test (SST). Serum and saliva samples were drawn between 8:00 AM and 10:00 AM. Salivary cortisol levels were measured using an enzyme immunoassay kit.
Results
Thirty-four patients were diagnosed with AI according to the SST results. Age, sex, body mass index, serum albumin levels, and serum creatinine levels did not significantly differ between the normal and AI groups. Basal and stimulated salivary cortisol levels were positively correlated with basal (r=0.538) and stimulated serum cortisol levels (r=0.750), respectively (all P<0.001). Receiver operating characteristic curve analysis yielded a cutoff level of morning basal salivary cortisol of 3.2 nmol/L (sensitivity, 84.9%; specificity, 73.5%; area under the curve [AUC]=0.822). The optimal cutoff value of stimulated salivary cortisol was 13.2 nmol/L (sensitivity, 90.7%; specificity, 94.1%; AUC=0.959). Subjects with a stimulated salivary cortisol level above 13.2 nmol/L but a stimulated serum cortisol level below 496.8 nmol/L (n=2) had lower serum albumin levels than those showing a concordant response.
Conclusion
The diagnostic performance of stimulated salivary cortisol measurements after the SST was comparable to serum cortisol measurements for diagnosing AI. -
Citations
Citations to this article as recorded by- Extensive expertise in endocrinology: adrenal crisis in assisted reproduction and pregnancy
Ulla Feldt-Rasmussen
European Journal of Endocrinology.2024; 190(1): R10. CrossRef - Turning Antibodies into Ratiometric Bioluminescent Sensors for Competition-Based Homogeneous Immunoassays
Eva A. van Aalen, Joep J. J. Lurvink, Leandra Vermeulen, Benice van Gerven, Yan Ni, Remco Arts, Maarten Merkx
ACS Sensors.2024; 9(3): 1401. CrossRef - A Contemporary Approach to the Diagnosis and Management of Adrenal Insufficiency
Suranut Charoensri, Richard J. Auchus
Endocrinology and Metabolism.2024; 39(1): 73. CrossRef - Diagnostic strategies in adrenal insufficiency
Vasiliki Siampanopoulou, Elisavet Tasouli, Anna Angelousi
Current Opinion in Endocrinology, Diabetes & Obesity.2023; 30(3): 141. CrossRef - The association between neuropeptide oxytocin and neuropsychiatric disorders after orthopedic surgery stress in older patients
Wanru Dong, Zengbo Ding, Xiao Wu, Ran Wan, Ying Liu, Liubao Pei, Weili Zhu
BMC Geriatrics.2023;[Epub] CrossRef - The Reliability of Salivary Cortisol Compared to Serum Cortisol for Diagnosing Adrenal Insufficiency with the Gold Standard ACTH Stimulation Test in Children
Silvia Ciancia, Sjoerd A. A. van den Berg, Erica L. T. van den Akker
Children.2023; 10(9): 1569. CrossRef - РІВЕНЬ СТРЕСУ В ДІТЕЙ ШКІЛЬНОГО ВІКУ З COVID-19
Г. А. Павлишин, О. І. Панченко
Здобутки клінічної і експериментальної медицини.2023; (4): 119. CrossRef - Secondary adrenal suppression related to high doses of inhaled corticosteroids in patients with severe asthma
Mariana Lobato, João Gaspar-Marques, Pedro Carreiro-Martins, Paula Leiria-Pinto
Annals of Allergy, Asthma & Immunology.2022; 128(4): 464. CrossRef - Clinical and Technical Aspects in Free Cortisol Measurement
Man Ho Choi
Endocrinology and Metabolism.2022; 37(4): 599. CrossRef - Continuous biomarker monitoring with single molecule resolution by measuring free particle motion
Alissa D. Buskermolen, Yu-Ting Lin, Laura van Smeden, Rik B. van Haaften, Junhong Yan, Khulan Sergelen, Arthur M. de Jong, Menno W. J. Prins
Nature Communications.2022;[Epub] CrossRef - Reversible Immunosensor for the Continuous Monitoring of Cortisol in Blood Plasma Sampled with Microdialysis
Laura van Smeden, Annet Saris, Khulan Sergelen, Arthur M. de Jong, Junhong Yan, Menno W. J. Prins
ACS Sensors.2022; 7(10): 3041. CrossRef - Adrenal insufficiency in HIV/AIDS: a review
Simon Mifsud, Zachary Gauci, Mark Gruppetta, Charles Mallia Azzopardi, Stephen Fava
Expert Review of Endocrinology & Metabolism.2021; 16(6): 351. CrossRef
- Extensive expertise in endocrinology: adrenal crisis in assisted reproduction and pregnancy

- Miscellaneous
- Encountering COVID-19 as Endocrinologists
- Eun-Jung Rhee, Jung Hee Kim, Sun Joon Moon, Won-Young Lee
- Endocrinol Metab. 2020;35(2):197-205. Published online June 23, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.197
- 13,293 View
- 277 Download
- 13 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - The world is entering an era of disaster and chaos due to coronavirus disease 2019 (COVID-19), which is caused by severe acute respiratory syndrome coronavirus 2. Since its first emergence in December 2019 in Wuhan, China, COVID-19 has swept through Asia and propagated throughout the world to Europe and North America. As of April 13, 1,773,084 people were infected and 111,652 people had died from COVID-19 globally, and new record levels of infection are being reported every day. Based on the data that have been amassed so far, the primary risk factors for a severe disease course or even mortality from COVID-19 are underlying diseases such as diabetes and hypertension. As the global prevalence of diabetes continues to increase, patients with endocrine diseases such as diabetes mellitus and those who are on long-term corticosteroid therapy due to adrenal insufficiency or hypopituitarism are at risk for a poor prognosis of COVID-19. As endocrinologists, we would like to briefly review the current knowledge about the relationship between COVID-19 and endocrine diseases and to discuss what we can do for the safety and health of our patients with endocrine diseases in this globally threatening situation.
-
Citations
Citations to this article as recorded by- Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study
İbrahim Mert Erbaş, İrem Ceren Erbaş, Gözde Akın Kağızmanlı, Kübra Yüksek Acinikli, Özge Besci, Korcan Demir, Ece Böber, Nurşen Belet, Ayhan Abacı
Journal of Clinical Research in Pediatric Endocrinology.2023; 15(3): 248. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - New-onset and relapsed Graves’ disease following COVID-19 vaccination: a comprehensive review of reported cases
Kan Chen, Yiyang Gao, Jing Li
European Journal of Medical Research.2023;[Epub] CrossRef - Assessment of Neuroendocrine Changes and Hypothalamo-Pituitary
Autoimmunity in Patients with COVID-19
Mustafa Sait Gonen, Annamaria De Bellis, Emre Durcan, Giuseppe Bellastella, Paolo Cirillo, Lorenzo Scappaticcio, Miriam Longo, Basak Ecem Bircan, Serdar Sahin, Cem Sulu, Hande Mefkure Ozkaya, Dildar Konukoglu, Fatma Ferda Kartufan, Fahrettin Kelestimur
Hormone and Metabolic Research.2022; 54(03): 153. CrossRef - COVID-19 and diabetes: Association intensify risk factors for morbidity and mortality
Prateek Sharma, Tapan Behl, Neelam Sharma, Sukhbir Singh, Ajmer Singh Grewal, Ali Albarrati, Mohammed Albratty, Abdulkarim M. Meraya, Simona Bungau
Biomedicine & Pharmacotherapy.2022; 151: 113089. CrossRef - The Relationship between COVID-19 and Hypothalamic–Pituitary–Adrenal Axis: A Large Spectrum from Glucocorticoid Insufficiency to Excess—The CAPISCO International Expert Panel
Mojca Jensterle, Rok Herman, Andrej Janež, Wael Al Mahmeed, Khalid Al-Rasadi, Kamila Al-Alawi, Maciej Banach, Yajnavalka Banerjee, Antonio Ceriello, Mustafa Cesur, Francesco Cosentino, Massimo Galia, Su-Yen Goh, Sanjay Kalra, Peter Kempler, Nader Lessan,
International Journal of Molecular Sciences.2022; 23(13): 7326. CrossRef - WhatsApp-Based virtual consultation in clinical practice during COVID times: A prospective institutional study
RamakanthBhargav Panchangam, Pradeep Puthenveetil, SunilKumar Kota, Sabaretnam Mayilvaganan
Annals of African Medicine.2022; 21(2): 132. CrossRef - Thyroid and COVID-19: a review on pathophysiological, clinical and organizational aspects
G. Lisco, A. De Tullio, E. Jirillo, V. A. Giagulli, G. De Pergola, E. Guastamacchia, V. Triggiani
Journal of Endocrinological Investigation.2021; 44(9): 1801. CrossRef - Effects of a DPP-4 Inhibitor and RAS Blockade on Clinical Outcomes of Patients with Diabetes and COVID-19
Sang Youl Rhee, Jeongwoo Lee, Hyewon Nam, Dae-Sung Kyoung, Dong Wook Shin, Dae Jung Kim
Diabetes & Metabolism Journal.2021; 45(2): 251. CrossRef - COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim
Endocrinology and Metabolism.2021; 36(4): 757. CrossRef - Collateral Damage of the COVID‐19 Pandemic on Nutritional Quality and Physical Activity: Perspective from South Korea
Soo Lim, Hyunjung Lim, Jean‐Pierre Després
Obesity.2020; 28(10): 1788. CrossRef - Diabetes mellitus and COVID-19 in the post-acute phase patients - possible links with physical and rehabilitation medicine and balneotherapy
Constantin Munteanu, Diana-Loreta PĂUN, Alina-Maria ȘUȚĂ, Simin Aysel FLORESCU, Gelu ONOSE, Mihail Hoteteu
Balneo Research Journal.2020; 11(Vol.11, no): 350. CrossRef - Managing Diabetes During the COVID-19 Pandemic
John Doupis, Konstantinos Avramidis
European Endocrinology.2020; 16(2): 85. CrossRef - Independent Impact of Diabetes on the Severity of Coronavirus Disease 2019 in 5,307 Patients in South Korea: A Nationwide Cohort Study
Sun Joon Moon, Eun-Jung Rhee, Jin-Hyung Jung, Kyung-Do Han, Sung-Rae Kim, Won-Young Lee, Kun-Ho Yoon
Diabetes & Metabolism Journal.2020; 44(5): 737. CrossRef - SARS-CoV-2 (COVID-19) and the Endocrine System
Michelle D Lundholm, Caroline Poku, Nicholas Emanuele, Mary Ann Emanuele, Norma Lopez
Journal of the Endocrine Society.2020;[Epub] CrossRef
- Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study

- Clinical Characteristics of Patients with Adrenal Insufficiency in a General Hospital
- Ye Yeon Lee, Nan Hee Cho, Jong Won Lee, Nam Kyung Kim, Hye Soon Kim, Mi-Kyung Kim
- Endocrinol Metab. 2017;32(1):83-89. Published online February 28, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.1.83
- 4,446 View
- 60 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Adrenal insufficiency (AI) is a life-threatening disorder caused by the deficiency of adrenal steroid hormones. This retrospective cross-sectional study investigated the characteristics of patients with AI in Korea.
Methods All consecutive patients with suspected AI who received care at a tertiary referral center in Korea in 2014 and underwent adrenocorticotropic hormone stimulation or insulin-tolerance testing were identified through a review of medical charts. Patients diagnosed with AI were enrolled. Their demographic, clinical, and treatment details were extracted.
Results Of 771 patients with suspected AI, 183 (23.7%) received a definitive diagnosis. The most common reason for testing was the presence of suspicious AI-related symptoms (30.0%), followed by a history of steroid medications (23.5%). Their mean age was 66.7 years, and females predominated (67.8%). The most common symptoms were general weakness, anorexia, arthralgia, and fever. Approximately half (53.6%) had a history of steroid use. Hydrocortisone was the most common treatment (71.6%), with most patients taking a 30 mg dose (44.2%). The most common dose frequency was twice a day (78.6%). Fourteen patients were treated for adrenal crisis (
n =10, 5.5%) or an intercurrent illness (n =4, 2.2%).Conclusion AI may have been caused by steroid medication use in many of the patients included in this study. The detection of AI can be improved by careful history-taking and being alert to the possibility that a patient has used steroids.
-
Citations
Citations to this article as recorded by- Risk of Mental Illnesses in Patients With Hypopituitarism: A Nationwide Population-Based Cohort Study
I-Hua Wei, Chih-Chia Huang
Psychiatry Investigation.2022; 19(6): 418. CrossRef - The Role of the Pharmacist in Optimizing Cancer Immunotherapy: A Retrospective Study of Nivolumab Adverse Events
Bradley D. Menz, Jacinta L. Johnson, Davina F. Gillard, William Chong, Michael B. Ward
Journal of Pharmacy Practice.2021; 34(3): 386. CrossRef - Clinical and biochemical factors to predict biochemical adrenal insufficiency in hospitalized patients with indeterminate cortisol levels: a retrospective study
Worapaka Manosroi, Natapong Kosachunhanan, Pichitchai Atthakomol
BMC Endocrine Disorders.2020;[Epub] CrossRef - Possible adrenal insufficiency among fatigue patients in a psychosomatic medical clinic
Sunao Matsubayashi, Nobuhiro Nakatake, Takeshi Hara
Endocrine Journal.2020; 67(1): 53. CrossRef - Encountering COVID-19 as Endocrinologists
Eun-Jung Rhee, Jung Hee Kim, Sun Joon Moon, Won-Young Lee
Endocrinology and Metabolism.2020; 35(2): 197. CrossRef - Glucocorticoid management of adrenal insufficiency in the United Kingdom: assessment using real-world data
Kamran Iqbal, Kate Halsby, Robert D Murray, Paul V Carroll, Robert Petermann
Endocrine Connections.2019; 8(1): 20. CrossRef
- Risk of Mental Illnesses in Patients With Hypopituitarism: A Nationwide Population-Based Cohort Study

- Clinical Study
- Recovery of Adrenal Function in Patients with Glucocorticoids Induced Secondary Adrenal Insufficiency
- Jong Ha Baek, Soo Kyoung Kim, Jung Hwa Jung, Jong Ryeal Hahm, Jaehoon Jung
- Endocrinol Metab. 2016;31(1):153-160. Published online March 16, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.1.153
- 4,927 View
- 81 Download
- 11 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The chronic use of glucocorticoids (GC) suppresses function of the hypothalamic-pituitary-adrenal axis and often results in secondary adrenal insufficiency (AI). The present study aimed to determine the recovery rate of adrenal function in patients with secondary AI within 1 to 2 years and to assess the factors predictive of adrenal function recovery.
Methods This was a retrospective observational study that enrolled patients diagnosed with GC-induced secondary AI between 2007 and 2013. AI was defined by peak serum cortisol levels <18 µg/dL during a standard-dose short synacthen test (SST). A follow-up SST was performed after 1 to 2 years, and responders were defined as those with adrenocorticotropic hormone (ACTH)-stimulated peak serum cortisol levels ≥18 µg/dL.
Results Of the total 34 patients diagnosed with GC-induced secondary AI at first, 20 patients (58.8%) recovered normal adrenal function by the time of the follow-up SST (median follow-up period, 16.5 months). Although the baseline serum ACTH and cortisol levels at the first SST did not differ between responders and non-responders, the incremental cortisol response during the first SST was higher in responders than that of non-responders (7.88 vs. 3.56,
P <0.01). Additionally, higher cortisol increments during the first SST were an independent predictive factor of the adrenal function recovery (odds ratio, 1.58; 95% confidence interval, 1.02 to 2.46;P <0.05).Conclusion In the present study, adrenal function recovery was achieved frequently in patients with GC-induced secondary AI within 1 to 2 years. Additionally, an incremental cortisol response at the first SST may be an important predictive factor of adrenal function recovery.
-
Citations
Citations to this article as recorded by- Secondary Adrenal Insufficiency: Recent Updates and New Directions for Diagnosis and Management
Lucinda M. Gruber, Irina Bancos
Endocrine Practice.2022; 28(1): 110. CrossRef - Oral corticosteroid elimination via a personalised reduction algorithm in adults with severe, eosinophilic asthma treated with benralizumab (PONENTE): a multicentre, open-label, single-arm study
Andrew Menzies-Gow, Mark Gurnell, Liam G Heaney, Jonathan Corren, Elisabeth H Bel, Jorge Maspero, Timothy Harrison, David J Jackson, David Price, Njira Lugogo, James Kreindler, Annie Burden, Alex de Giorgio-Miller, Kelly Padilla, Ubaldo J Martin, Esther G
The Lancet Respiratory Medicine.2022; 10(1): 47. CrossRef - Development and Resolution of Secondary Adrenal Insufficiency after an Intra-Articular Steroid Injection
Jia Wei Tan, Sachin K. Majumdar, Osamu Isozaki
Case Reports in Endocrinology.2022; 2022: 1. CrossRef - Long‐term corticosteroid use, adrenal insufficiency and the need for steroid‐sparing treatment in adult severe asthma
M. Gurnell, L. G. Heaney, D. Price, A. Menzies‐Gow
Journal of Internal Medicine.2021; 290(2): 240. CrossRef - Glucocorticoid Withdrawal—An Overview on When and How to Diagnose Adrenal Insufficiency in Clinical Practice
Katarzyna Pelewicz, Piotr Miśkiewicz
Diagnostics.2021; 11(4): 728. CrossRef - Morning Serum Cortisol as a Predictor for the HPA Axis Recovery in Cushing’s Disease
Q. Cui, D. Liu, B. Xiang, Q. Sun, L. Fan, M. He, Y. Wang, X. Zhu, H. Ye, Giorgio Borretta
International Journal of Endocrinology.2021; 2021: 1. CrossRef - Dexamethasone-related adrenal insufficiency in patients with brain and skull base tumours
H. Benghiat, P. Sanghera, D. Stange, P. Nightingale, A. Hartley, M.W O’Reilly, N. Nundall, H. Currie, M. Ali, G. Cruickshank, D. Spooner, A. Toogood
Supportive Care in Cancer.2018; 26(12): 4031. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - The unresolved riddle of glucocorticoid withdrawal
F. Guerrero Pérez, A. P. Marengo, C. Villabona Artero
Journal of Endocrinological Investigation.2017; 40(11): 1175. CrossRef - Lessons from iatrogenic Cushing syndrome in children
Betty P Messazos, Margaret R Zacharin
Journal of Paediatrics and Child Health.2016; 52(12): 1106. CrossRef
- Secondary Adrenal Insufficiency: Recent Updates and New Directions for Diagnosis and Management

- Adrenal gland
- Allgrove (Triple A) Syndrome: A Case Report from the Kashmir Valley
- Raiz Ahmad Misgar, Nazir Ahmad Pala, Mahroosa Ramzan, Arshad Iqbal Wani, Mir Iftikhar Bashir, Bashir Ahmad Laway
- Endocrinol Metab. 2015;30(4):604-606. Published online December 31, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.4.604
- 3,894 View
- 33 Download
- 10 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Allgrove (Triple A) syndrome is a rare autosomal recessive disorder characterized by cardinal features of adrenal insufficiency due to adrenocorticotropic hormone (ACTH) resistance, achalasia, and alacrimia. It is frequently associated with neurological manifestations like polyneuropathy. Since its first description by Allgrove in 1978, approximately 100 cases have been reported in the literature. Here we report an 18-year-old boy diagnosed as having Allgrove syndrome, with ACTH resistant adrenal insufficiency, achalasia, alacrimia, and severe motor polyneuropathy. Alacrimia was the earliest feature evident at the age of 8 years. He presented with achalasia and adrenal insufficiency at 12 and 18 years respectively and developed neurological symptoms in the form of severe muscle wasting at the age of 15 years. Patients with Allgrove syndrome usually manifest adrenal insufficiency and achalasia during first decade of life. Our patient manifested adrenal insufficiency and achalasia in the second decade and manifested neurological dysfunction before adrenal dysfunction.
-
Citations
Citations to this article as recorded by- Child Neurology: Allgrove Syndrome
Juhi Gupta, Sayoni Roy Chowdhury, Prashant Jauhari, Kaushik Ragunathan, Biswaroop Chakrabarty, Vandana Jain, Sheffali Gulati
Neurology.2024;[Epub] CrossRef - Don’t forget Allgrove syndrome in adult patients as a bulbar-ALS mimicker
Martina Vigano’, Vittorio Mantero, Paola Basilico, Fiammetta Pirro, Dario Ronchi, Alessio Di Fonzo, Andrea Salmaggi
Neurological Sciences.2023; 44(10): 3703. CrossRef - Triple A (Allgrove) syndrome due to AAAS gene mutation with a rare association of amyotrophy
Satyam Singh Jayant, Rahul Gupta, Kanhaiya Agrawal, Liza Das, Pinaki Dutta, Anil Bhansali
Hormones.2021; 20(1): 197. CrossRef - Allgrove syndrome with amyotrophy
Míriam Carvalho Soares, Otávio Gomes Lins, José Ronaldo Lima de Carvalho, Cláudia Cristina de Sá, Vanessa Van der Linden, Anna Paula Paranhos Miranda Covaleski
Practical Neurology.2021; : practneurol-2021-003192. CrossRef - Triple A syndrome (Allgrove syndrome) – A journey from clinical symptoms to a syndrome
Prakarti Yadav, Deepak Kumar, GopalK Bohra, MahendraK Garg
Journal of Family Medicine and Primary Care.2020; 9(5): 2531. CrossRef - Case report of a familial triple: a syndrome and review of the literature
Federica Gaiani, Pierpacifico Gismondi, Roberta Minelli, Giovanni Casadio, Nicola de’Angelis, Fabiola Fornaroli, Gian Luigi de’Angelis, Marco Manfredi
Medicine.2020; 99(22): e20474. CrossRef - Clinical and genetic characterisation of a series of patients with triple A syndrome
Erdal Kurnaz, Paolo Duminuco, Zehra Aycan, Şenay Savaş-Erdeve, Nursel Muratoğlu Şahin, Melişah Keskin, Elvan Bayramoğlu, Marco Bonomi, Semra Çetinkaya
European Journal of Pediatrics.2018; 177(3): 363. CrossRef - Clinical heterogeneity and molecular profile of triple A syndrome: a study of seven cases
Kanika Singh, Ratna Dua Puri, Pratibha Bhai, Archana Dayal Arya, Garima Chawla, Renu Saxena, Ishwar C. Verma
Journal of Pediatric Endocrinology and Metabolism.2018; 31(7): 799. CrossRef - Clinical and molecular report of c.1331 + 1G > A mutation of the AAAS gene in a Moroccan family with Allgrove syndrome: a case report
H. Berrani, T. Meskini, M. Zerkaoui, H. Merhni, S. Ettair, A. Sefiani, N. Mouane
BMC Pediatrics.2018;[Epub] CrossRef
- Child Neurology: Allgrove Syndrome

- A Case of Primary Adrenal Insufficiency in a Patient with Acquired Immunodeficiency Syndrome.
- Jae Ho Choi, Suk Chon, Yu Chul Hwang, Jun Seong Son, Seung Joon Oh, Kyu Jeung Ahn, Ho Yeon Chung, Jeong Taek Woo, Sung Woon Kim, Jin Woo Kim, Young Seol Kim, In Kyung Jeong
- Endocrinol Metab. 2011;26(3):253-257. Published online September 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.3.253
- 2,121 View
- 24 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - The adrenal gland is the most commonly involved endocrine organ in patients infected with the human immunodeficiency virus (HIV). Adrenal function abnormality is more common in HIV patients than in the general population. It is important to recognize the condition of adrenal insufficiency, as this adrenal disorder may prove fatal if left untreated. Herein, we report a case of primary adrenal insufficiency in a 37-year-old male patient with acquired immunodeficiency syndrome. The patient complained of fever, general weakness, and fatigue. Impaired adrenal function was noted in the rapid ACTH stimulation test. After steroid supplementation, the patient's symptoms were improved. Therefore, HIV care physicians should ascertain adrenal dysfunction in HIV patients when they complain of fever and general weakness.
-
Citations
Citations to this article as recorded by- A Case Report of Adrenal Insufficiency Treated with Korean Medicine
Young-ji Kim, Jung-yeon Kwon, Ho-yeon Go, Kyung-hwan Kong
The Journal of Internal Korean Medicine.2017; 38(5): 583. CrossRef
- A Case Report of Adrenal Insufficiency Treated with Korean Medicine

- A Case Report of Bilateral Adrenocortical Carcinoma Complicated by Adrenal Insufficiency.
- Min Joo Kim, Jung Hee Kim, Tae Young Kim, Sang Wan Kim
- Endocrinol Metab. 2011;26(3):243-247. Published online September 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.3.243
- 2,005 View
- 29 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Adrenocortical carcinoma is often functional and presents with signs and symptoms of adrenal steroid hormone excess. Adrenal insufficiency secondary to bilateral adrenocortical carcinoma is a particularly rare complication. We recently encountered a case of bilateral adrenocortical carcinoma complicated by adrenal insufficiency. A 52-year-old male was transferred to this hospital complaining of general weakness and weight loss. A bilateral adrenal mass was detected on abdomen CT. Plasma cortisol and aldosterone failed to rise during the rapid ACTH stimulation test. The CT-guided adrenal biopsy revealed findings consistent with adrenocortical carcinoma. Left hemiparesis was developed and brain metastasis was detected via brain MRI. Despite the application of gamma knife surgery and chemotherapy, the disease progressed and the patient died.
-
Citations
Citations to this article as recorded by- Bilateral Adrenocortical Carcinoma Presenting as Acute Adrenal Insufficiency
Anshita Aggarwal, Aprajita Verma, Aparajita Roy, Bindu Kulshreshtha
European Endocrinology.2020; 16(2): 172. CrossRef - A Case of Bilateral ACTH-independent Adrenal Adenomas with Cushing's Syndrome Treated by Ipsilateral Total and Contralateral Partial Laparoscopic Adrenalectomy
Seung Ah Park, Dong min Jung, Soon young Kim, Nan Young Choi, Tae-jun Kim, Yong kyun Kim, Seong kyun Na, Chul Sik Kim, Seong Jin Lee, Sung-Hee Ihm, Jun Goo Kang
The Korean Journal of Obesity.2013; 22(4): 254. CrossRef
- Bilateral Adrenocortical Carcinoma Presenting as Acute Adrenal Insufficiency

- No Significance of the Free Cortisol Index Compared to Total Cortisol in Critically Ill Patients.
- Kyung Won Kim, Sang Wan Kim, Hee Joung Kim, Chan Soo Shin, Sung Jae Park, Gil Joon Suh, Seong Yeon Kim
- Endocrinol Metab. 2011;26(2):120-125. Published online June 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.2.120
- 1,879 View
- 21 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Some patients exhibit an inadequate response of cortisol to stressful conditions; this state is known as critical illness-related corticosteroid insufficiency. These patients have low serum binding protein concentrations, thereby suggesting that total serum cortisol may not be reflective of circulating cortisol activity. As the free cortisol index (FCI = total cortisol/corticosteroid-binding globulin) has been correlated with serum free cortisol, we measured FCI in Korean patients for the first time. In this study, we attempted to determine whether FCI was superior to total cortisol in predicting 30-day mortality. METHODS: We recruited 65 critically ill patients with relatively high Acute Physiology, Age and Chronic Health Evaluation (APACHE III) scores. Fourteen patients with pituitary disease but normal pituitary function were recruited from outpatient clinics. Total cortisol and corticosteroid-binding globulin were measured in patients and controls during the short Synacthen test. RESULTS: The basal cortisol level and basal FCI level were higher in patients (n = 65) than in healthy controls (P < 0.001, respectively). We found that total cortisol was strongly correlated with FCI (P < 0.001) in critically ill patients; however, neither total cortisol nor FCI were associated with 30-day mortality among patients. Only severe clinical criteria (such as APACHE-III scores and low albumin) were associated with 30-day mortality. CONCLUSION: Our results do not suggest that FCI is more accurate than total cortisol in predicting clinical outcomes in critically ill patients. -
Citations
Citations to this article as recorded by- No Significance of the Free Cortisol Index Compared to Total Cortisol in Critically Ill Patients
Doo-Man Kim
Endocrinology and Metabolism.2011; 26(2): 118. CrossRef
- No Significance of the Free Cortisol Index Compared to Total Cortisol in Critically Ill Patients

- Primary Bilateral Adrenal Non-Hodgkin's Lymphoma Presented with Adrenal Insufficiency: A Case Report.
- Eun Young Lee, Kyoung Min Kim, Kwang Joon Kim, Songmi Noh, Jin Seok Kim, Woo Ik Yang, Sung Kil Lim
- Endocrinol Metab. 2011;26(1):101-105. Published online March 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.1.101
- 1,813 View
- 23 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Primary adrenal lymphoma is a very rare disease and it is known to have a poor prognosis. We report here on a case of primary adrenal insufficiency that was secondary to primary bilateral adrenal lymphoma. A 54-year old man was hospitalized because of easy fatigability, weight loss and consistent malaise for 6 months. The physical examination revealed hyperpigmentation on the anterior chest and hypotension. According these findings and symptoms, we did a rapid ACTH stimulation test with a clinical suspicion of adrenal insufficiency. He showed an inadequate adrenal response and so he was diagnosed with adrenal insufficiency. The abdominal CT images showed bilateral huge adrenal masses and increased uptake of the adrenal glands on PET. The pathologic diagnosis by ultrasound-guided gun biopsy of the right adrenal gland was diffuse large B cell lymphoma. The patient was administered combination chemotherapy with the R-CHOP regimen, and after 8-cycles of chemotherapy, he achieved complete remission of tumor according to the image studies and he recovered his adrenal function. Primary adrenal lymphoma, although a rare disease, should be considered in patients with bilateral enlargement of the adrenal glands and when the adrenal glands show increased uptake on a PET scan, and especially there is adrenal insufficiency.
-
Citations
Citations to this article as recorded by- Systemic vs. intrathecal central nervous system prophylaxis in primary adrenal/renal diffuse large b-cell Lymphoma: A multi-institution retrospective analysis and systematic review
John Xie, Albert Jang, Motohide Uemura, Shigeaki Nakazawa, Teresa Calimeri, Andres JM Ferreri, Shuang R. Chen, Janet L. Schmid, Theresa C. Brown, Francisco Socola, Hana Safah, Nakhle S. Saba
Leukemia Research Reports.2021; 16: 100263. CrossRef
- Systemic vs. intrathecal central nervous system prophylaxis in primary adrenal/renal diffuse large b-cell Lymphoma: A multi-institution retrospective analysis and systematic review

- A Case of Pituitary Macroadenoma Accompanied with CRH Deficiency.
- Yoo Jung Nahm, Jin Soo Kim, Keun Jong Cho, Uk Hyun Kil, Sung Yong Woo, Sung Rae Kim, Soon Jib Yoo, Sung Koo Kang, Ho Young Son
- J Korean Endocr Soc. 2006;21(2):153-157. Published online April 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.2.153
- 1,669 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - Pituitary tumor can be accompanied with various pituitary hormone abnormalities. Pituitary tumors can be divided into functioning or nonfunctioning tumors. A functioning pituitary tumor, via the oversecretion of pituitary hormones, causes diverse clinical features. A nonfunctioning pituitary tumor can be accompanied with pituitary dysfunction and this may be due to compression or destruction of normal pituitary tissue, suppression of the pituitary portal system or direct damage to the hypothalamus. Corticotropin-releasing hormone (CRH) deficiency, which is caused by defects in the synthesis or release of CRH, is a cause of secondary adrenocortical insufficiency. The clinical presentations are hypoglycemia, weight loss, anemia, weakness, nausea, vomiting and hyponatremia. Acquired CRH deficiency has also been suggested to occur based on a lack of adrenocorticotropic hormone (ACTH) response to insulin-induced hypoglycemia, but there is a normal ACTH response to exogenous CRH. We experienced a case of a woman with pituitary macroadenoma accompanied with CRH deficiency. We report here on this case with the review of the literature.


 KES
KES

 First
First Prev
Prev



