Search
- Page Path
- HOME > Search
Original Articles
- Thyroid
- Active Surveillance for Low-Risk Papillary Thyroid Carcinoma as an Acceptable Management Option with Additional Benefits: A Comprehensive Systematic Review
- Jee Hee Yoon, Wonsuk Choi, Ji Yong Park, A Ram Hong, Hee Kyung Kim, Ho-Cheol Kang
- Endocrinol Metab. 2024;39(1):152-163. Published online January 22, 2024
- DOI: https://doi.org/10.3803/EnM.2023.1794
- 1,147 View
- 42 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
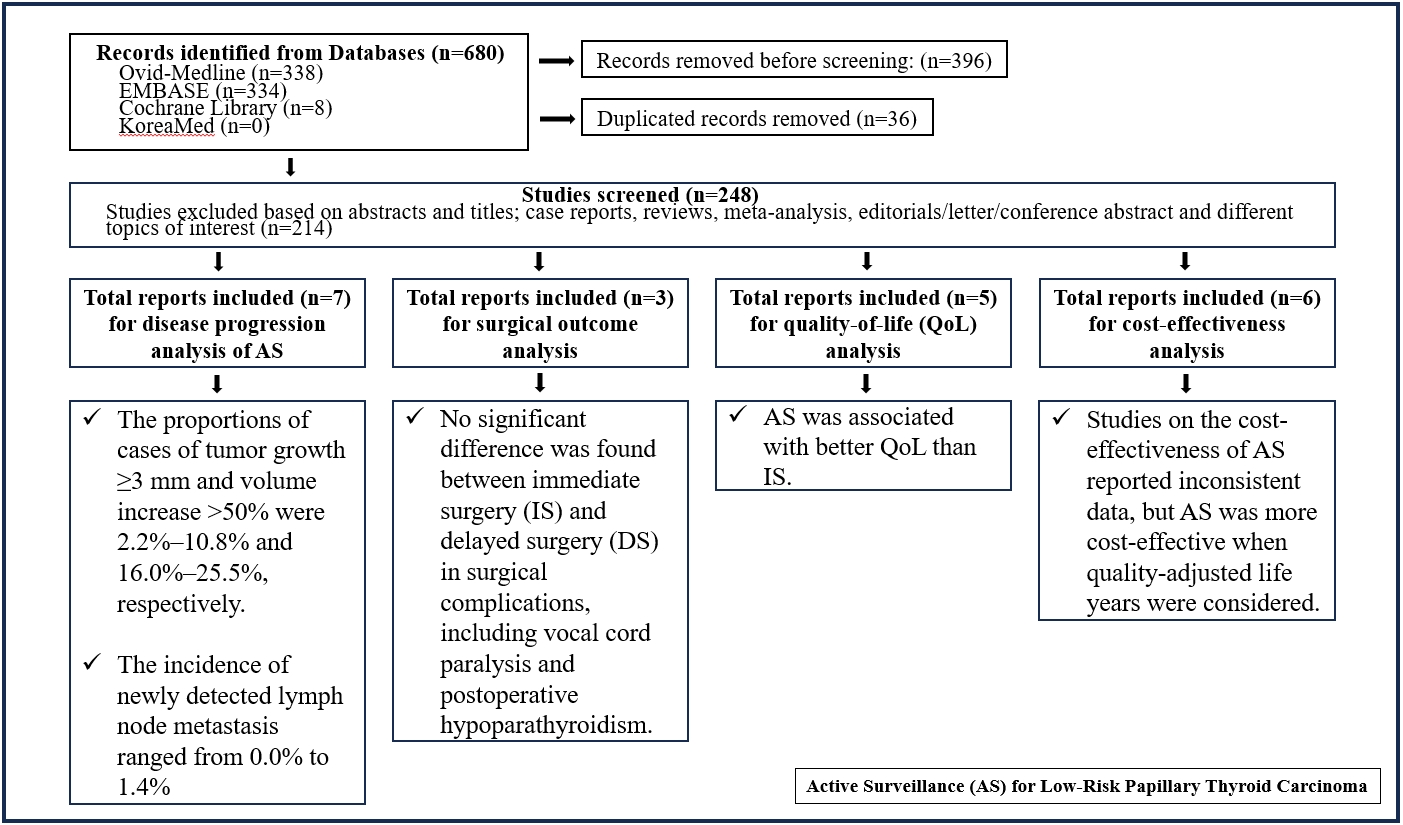
Active surveillance (AS) has been introduced as a management strategy for low-risk papillary thyroid carcinoma (PTC) due to its typically indolent nature. Despite this, the widespread adoption of AS has encountered several challenges. The aim of this systematic review was to evaluate the safety of AS related to disease progression and its benefits compared with immediate surgery (IS).
Methods
Studies related to AS in patients with low-risk PTC were searched through the Ovid MEDLINE, Embase, Cochrane Library, and KoreaMed databases. Studies on disease progression, surgical complication, quality of life (QoL), and cost-effectiveness were separately analyzed and narratively synthesized.
Results
In the evaluation of disease progression, the proportions of cases with tumor growth ≥3 mm and a volume increase >50% were 2.2%–10.8% and 16.0%–25.5%, respectively. Newly detected lymph node metastasis was identified in 0.0%–1.4% of patients. No significant difference was found between IS and delayed surgery in surgical complications, including vocal cord paralysis and postoperative hypoparathyroidism. AS was associated with better QoL than IS. Studies on the cost-effectiveness of AS reported inconsistent data, but AS was more cost-effective when quality-adjusted life years were considered.
Conclusion
AS is an acceptable management option for patients with low-risk PTC based on the low rate of disease progression and the absence of an increased mortality risk. AS has additional benefits, including improved QoL and greater QoL-based cost-effectiveness. -
Citations
Citations to this article as recorded by- It Is Time to Understand the Additional Benefits of Active Surveillance for Low-Risk Papillary Thyroid Carcinoma
Kyeong Jin Kim
Endocrinology and Metabolism.2024; 39(1): 95. CrossRef
- It Is Time to Understand the Additional Benefits of Active Surveillance for Low-Risk Papillary Thyroid Carcinoma

- Diabetes, obesity and metabolism
- Triglyceride-Glucose Index Predicts Future Atherosclerotic Cardiovascular Diseases: A 16-Year Follow-up in a Prospective, Community-Dwelling Cohort Study
- Joon Ho Moon, Yongkang Kim, Tae Jung Oh, Jae Hoon Moon, Soo Heon Kwak, Kyong Soo Park, Hak Chul Jang, Sung Hee Choi, Nam H. Cho
- Endocrinol Metab. 2023;38(4):406-417. Published online August 3, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1703
- 2,655 View
- 166 Download
- 3 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
While the triglyceride-glucose (TyG) index is a measure of insulin resistance, its association with cardiovascular disease (CVD) has not been well elucidated. We evaluated the TyG index for prediction of CVDs in a prospective large communitybased cohort.
Methods
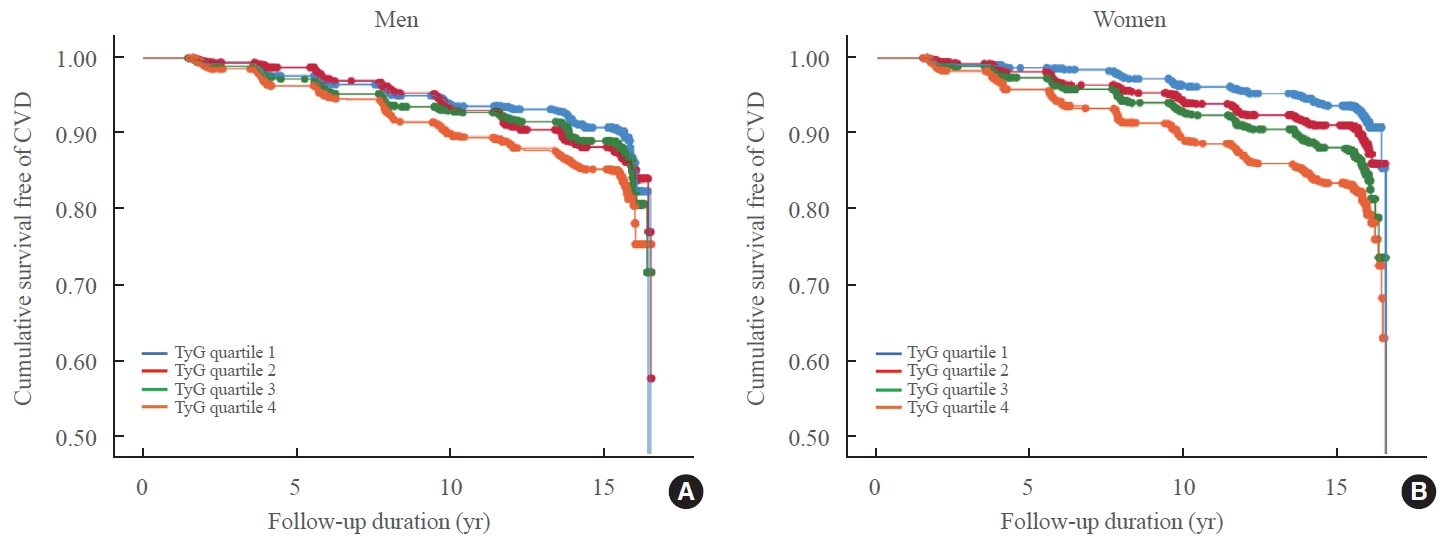
Individuals 40 to 70 years old were prospectively followed for a median 15.6 years. The TyG index was calculated as the Ln [fasting triglycerides (mg/dL)×fasting glucose (mg/dL)/2]. CVDs included any acute myocardial infarction, coronary artery disease or cerebrovascular disease. We used a Cox proportional hazards model to estimate CVD risks according to quartiles of the TyG index and plotted the receiver operating characteristics curve for the incident CVD.
Results
Among 8,511 subjects (age 51.9±8.8 years; 47.5% males), 931 (10.9%) had incident CVDs during the follow-up. After adjustment for age, sex, body mass index, diabetes mellitus, hypertension, total cholesterol, smoking, alcohol, exercise, and C-reactive protein, subjects in the highest TyG quartile had 36% increased risk of incident CVD compared with the lowest TyG quartile (hazard ratio, 1.36; 95% confidence interval, 1.10 to 1.68). Carotid plaque, assessed by ultrasonography was more frequent in subjects in the higher quartile of TyG index (P for trend=0.049 in men and P for trend <0.001 in women). The TyG index had a higher predictive power for CVDs than the homeostasis model assessment of insulin resistance (HOMA-IR) (area under the curve, 0.578 for TyG and 0.543 for HOMA-IR). Adding TyG index on diabetes or hypertension alone gave sounder predictability for CVDs.
Conclusion
The TyG index is independently associated with future CVDs in 16 years of follow-up in large, prospective Korean cohort. -
Citations
Citations to this article as recorded by- Construction and validation of a nomogram for predicting diabetes remission at 3 months after bariatric surgery in patients with obesity combined with type 2 diabetes mellitus
Kaisheng Yuan, Bing Wu, Ruiqi Zeng, Fuqing Zhou, Ruixiang Hu, Cunchuan Wang
Diabetes, Obesity and Metabolism.2024; 26(1): 169. CrossRef - Association between the triglyceride glucose index and chronic total coronary occlusion: A cross-sectional study from southwest China
Kaiyong Xiao, Huili Cao, Bin Yang, Zhe Xv, Lian Xiao, Jianping Wang, Shuiqing Ni, Hui Feng, Zhongwei He, Lei Xv, Juan Li, Dongmei Xv
Nutrition, Metabolism and Cardiovascular Diseases.2024; 34(4): 850. CrossRef - The association between TyG and all-cause/non-cardiovascular mortality in general patients with type 2 diabetes mellitus is modified by age: results from the cohort study of NHANES 1999–2018
Younan Yao, Bo Wang, Tian Geng, Jiyan Chen, Wan Chen, Liwen Li
Cardiovascular Diabetology.2024;[Epub] CrossRef - Triglyceride-glucose index predicts type 2 diabetes mellitus more effectively than oral glucose tolerance test-derived insulin sensitivity and secretion markers
Min Jin Lee, Ji Hyun Bae, Ah Reum Khang, Dongwon Yi, Mi Sook Yun, Yang Ho Kang
Diabetes Research and Clinical Practice.2024; 210: 111640. CrossRef - Evaluation of the novel three lipid indices for predicting five- and ten-year incidence of cardiovascular disease: findings from Kerman coronary artery disease risk factors study (KERCADRS)
Alireza Jafari, Hamid Najafipour, Mitra Shadkam, Sina Aminizadeh
Lipids in Health and Disease.2023;[Epub] CrossRef
- Construction and validation of a nomogram for predicting diabetes remission at 3 months after bariatric surgery in patients with obesity combined with type 2 diabetes mellitus

- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database) - Predicting the Risk of Insulin-Requiring Gestational Diabetes before Pregnancy: A Model Generated from a Nationwide Population-Based Cohort Study in Korea
- Seung-Hwan Lee, Jin Yu, Kyungdo Han, Seung Woo Lee, Sang Youn You, Hun-Sung Kim, Jae-Hyoung Cho, Kun-Ho Yoon, Mee Kyoung Kim
- Endocrinol Metab. 2023;38(1):129-138. Published online January 27, 2023
- DOI: https://doi.org/10.3803/EnM.2022.1609

- 2,130 View
- 156 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The severity of gestational diabetes mellitus (GDM) is associated with adverse pregnancy outcomes. We aimed to generate a risk model for predicting insulin-requiring GDM before pregnancy in Korean women.
Methods
A total of 417,210 women who received a health examination within 52 weeks before pregnancy and delivered between 2011 and 2015 were recruited from the Korean National Health Insurance database. The risk prediction model was created using a sample of 70% of the participants, while the remaining 30% were used for internal validation. Risk scores were assigned based on the hazard ratios for each risk factor in the multivariable Cox proportional hazards regression model. Six risk variables were selected, and a risk nomogram was created to estimate the risk of insulin-requiring GDM.
Results
A total of 2,891 (0.69%) women developed insulin-requiring GDM. Age, body mass index (BMI), current smoking, fasting blood glucose (FBG), total cholesterol, and γ-glutamyl transferase were significant risk factors for insulin-requiring GDM and were incorporated into the risk model. Among the variables, old age, high BMI, and high FBG level were the main contributors to an increased risk of insulin-requiring GDM. The concordance index of the risk model for predicting insulin-requiring GDM was 0.783 (95% confidence interval, 0.766 to 0.799). The validation cohort’s incidence rates for insulin-requiring GDM were consistent with the risk model’s predictions.
Conclusion
A novel risk engine was generated to predict insulin-requiring GDM among Korean women. This model may provide helpful information for identifying high-risk women and enhancing prepregnancy care. -
Citations
Citations to this article as recorded by- Establishment and validation of a nomogram to predict the neck contracture after skin grafting in burn patients: A multicentre cohort study
Rui Li, Yangyang Zheng, Xijuan Fan, Zilong Cao, Qiang Yue, Jincai Fan, Cheng Gan, Hu Jiao, Liqiang Liu
International Wound Journal.2023; 20(9): 3648. CrossRef - Predicting the Need for Insulin Treatment: A Risk-Based Approach to the Management of Women with Gestational Diabetes Mellitus
Anna S. Koefoed, H. David McIntyre, Kristen S. Gibbons, Charlotte W. Poulsen, Jens Fuglsang, Per G. Ovesen
Reproductive Medicine.2023; 4(3): 133. CrossRef - Prepregnancy Glucose Levels Within Normal Range and Its Impact on Obstetric Complications in Subsequent Pregnancy: A Population Cohort Study
Ho Yeon Kim, Ki Hoon Ahn, Geum Joon Cho, Soon-Cheol Hong, Min-Jeong Oh, Hai-Joong Kim
Journal of Korean Medical Science.2023;[Epub] CrossRef - Risk of Cause-Specific Mortality across Glucose Spectrum in Elderly People: A Nationwide Population-Based Cohort Study
Joonyub Lee, Hun-Sung Kim, Kee-Ho Song, Soon Jib Yoo, Kyungdo Han, Seung-Hwan Lee
Endocrinology and Metabolism.2023; 38(5): 525. CrossRef - The CHANGED Score—A New Tool for the Prediction of Insulin Dependency in Gestational Diabetes
Paul Rostin, Selina Balke, Dorota Sroka, Laura Fangmann, Petra Weid, Wolfgang Henrich, Josefine Theresia Königbauer
Journal of Clinical Medicine.2023; 12(22): 7169. CrossRef
- Establishment and validation of a nomogram to predict the neck contracture after skin grafting in burn patients: A multicentre cohort study

- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database) - Association among Current Smoking, Alcohol Consumption, Regular Exercise, and Lower Extremity Amputation in Patients with Diabetic Foot: Nationwide Population-Based Study
- Yoon Jae Lee, Kyung-Do Han, Jun Hyeok Kim
- Endocrinol Metab. 2022;37(5):770-780. Published online October 12, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1519
- 3,271 View
- 202 Download
- 2 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
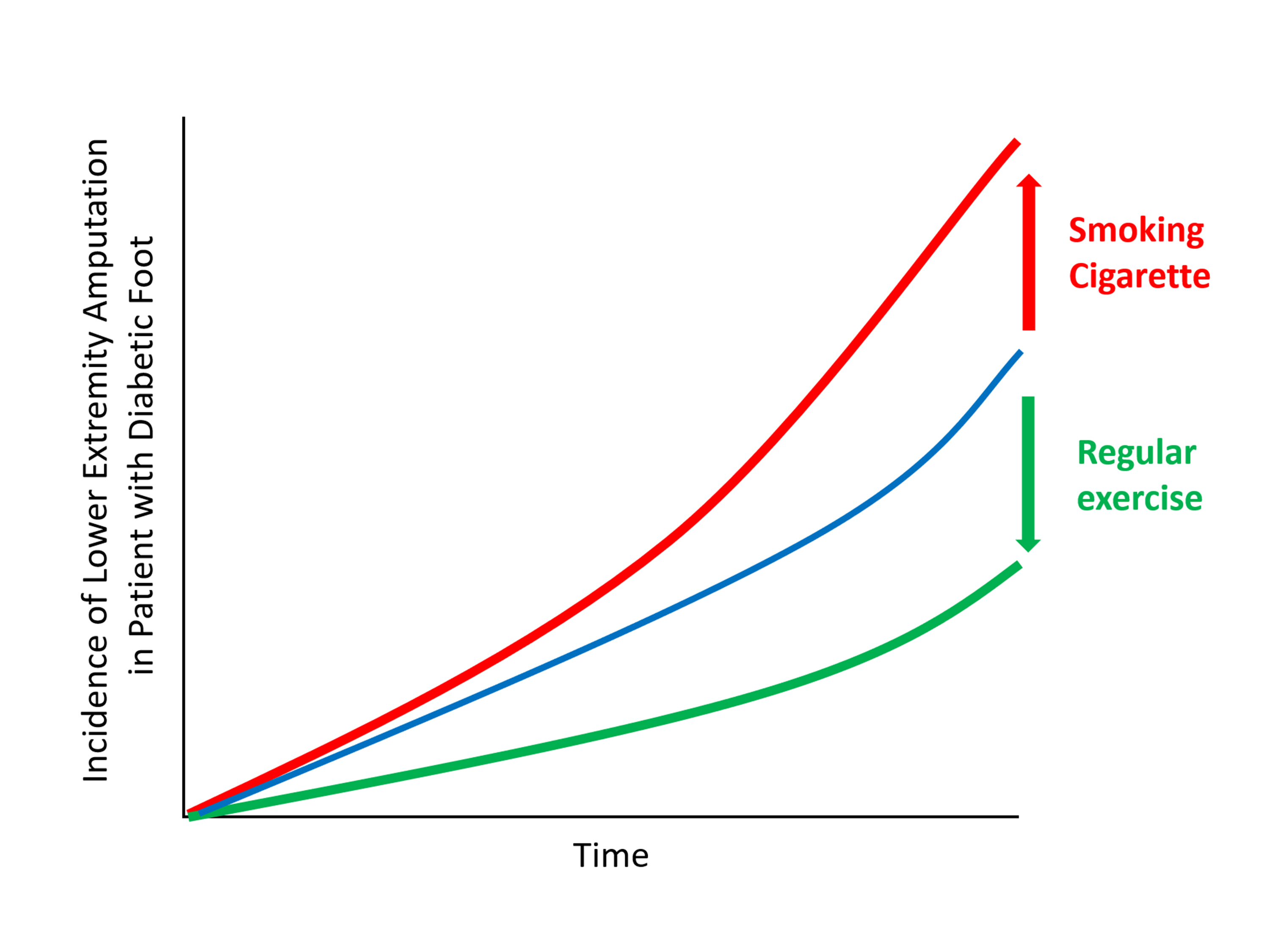
The present study investigates whether modifiable behavioral factors of current cigarette smoking, heavy alcohol consumption, and regular exercise are associated with risk of lower extremity amputation (LEA) in diabetic patients.
Methods
A total of 2,644,440 diabetic patients (aged ≥20 years) was analyzed using the database of the Korean National Health Insurance Service. Cox proportional hazard regression was used to assess adjusted hazard ratios (HRs) for the behavioral factors with risk of LEA under adjustment for potential confounders.
Results
The risk of LEA was significantly increased by current cigarette smoking and heavy alcohol consumption (HR, 1.436; 95% confidence interval [CI], 1.367 to 1.508 and HR, 1.082; 95% CI, 1.011 to 1.158) but significantly decreased with regular exercise (HR, 0.745; 95% CI, 0.706 to 0.786) after adjusting for age, sex, smoking, alcohol consumption, exercise, low income, hypertension, dyslipidemia, body mass index, using insulin or oral antidiabetic drugs, and diabetic duration. A synergistically increased risk of LEA was observed with larger number of risky behaviors.
Conclusion
Modification of behaviors of current smoking, heavy alcohol intake, and exercise prevents LEA and can improve physical, emotional, and social quality of life in diabetic patients. -
Citations
Citations to this article as recorded by- Adjuvant effect of antimicrobial photodynamic therapy (aPDT) in the treatment of diabetic foot ulcers: A case series
Rita de Cassia Ferreira, Rebeca Boltes Cecatto, Silvana Torres Perez, Raquel Agnelli Mesquita‐Ferrari, Sandra Kalil Bussadori, Cinthya Cosme Duran, Anna Carolina Tempestini Horliana, Kristianne Porta Santos Fernandes
Journal of Biophotonics.2024;[Epub] CrossRef - Factors associated with diabetic foot ulcers and lower limb amputations in type 1 and type 2 diabetes supported by real‐world data from the German/Austrian DPV registry
Alexander J. Eckert, Stefan Zimny, Marcus Altmeier, Ana Dugic, Anton Gillessen, Latife Bozkurt, Gabriele Götz, Wolfram Karges, Frank J. Wosch, Stephan Kress, Reinhard W. Holl
Journal of Diabetes.2024;[Epub] CrossRef - Investigating Diabetic Foot Pathophysiology and Amputation Prevention Strategies through Behavioral Modification
Jun Hyeok Kim
Journal of Wound Management and Research.2023; 19(3): 167. CrossRef
- Adjuvant effect of antimicrobial photodynamic therapy (aPDT) in the treatment of diabetic foot ulcers: A case series

- Calcium & Bone Metabolism
- Development of a Spine X-Ray-Based Fracture Prediction Model Using a Deep Learning Algorithm
- Sung Hye Kong, Jae-Won Lee, Byeong Uk Bae, Jin Kyeong Sung, Kyu Hwan Jung, Jung Hee Kim, Chan Soo Shin
- Endocrinol Metab. 2022;37(4):674-683. Published online August 5, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1461
- 3,869 View
- 211 Download
- 12 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Since image-based fracture prediction models using deep learning are lacking, we aimed to develop an X-ray-based fracture prediction model using deep learning with longitudinal data.
Methods
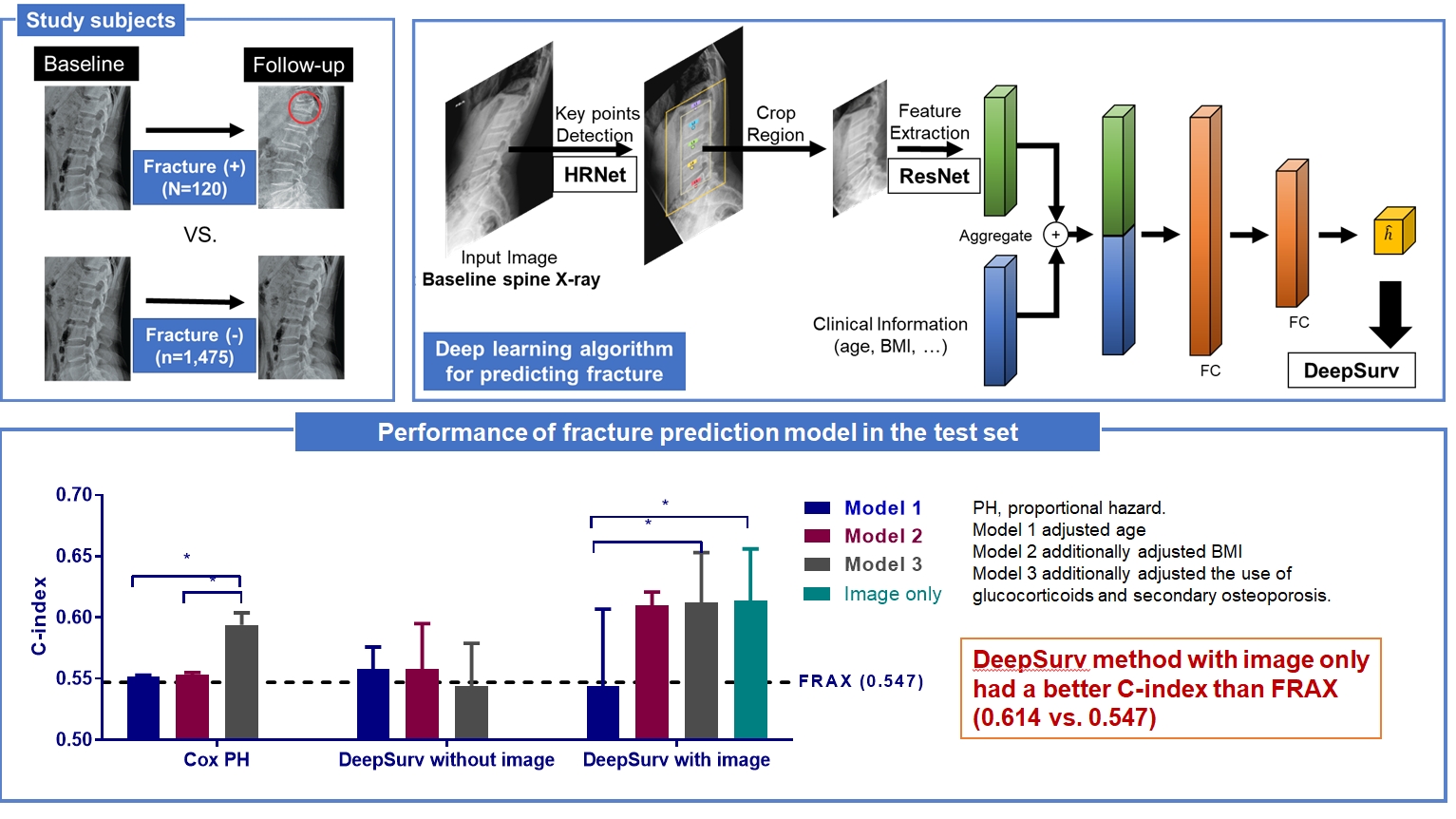
This study included 1,595 participants aged 50 to 75 years with at least two lumbosacral radiographs without baseline fractures from 2010 to 2015 at Seoul National University Hospital. Positive and negative cases were defined according to whether vertebral fractures developed during follow-up. The cases were divided into training (n=1,416) and test (n=179) sets. A convolutional neural network (CNN)-based prediction algorithm, DeepSurv, was trained with images and baseline clinical information (age, sex, body mass index, glucocorticoid use, and secondary osteoporosis). The concordance index (C-index) was used to compare performance between DeepSurv and the Fracture Risk Assessment Tool (FRAX) and Cox proportional hazard (CoxPH) models.
Results
Of the total participants, 1,188 (74.4%) were women, and the mean age was 60.5 years. During a mean follow-up period of 40.7 months, vertebral fractures occurred in 7.5% (120/1,595) of participants. In the test set, when DeepSurv learned with images and clinical features, it showed higher performance than FRAX and CoxPH in terms of C-index values (DeepSurv, 0.612; 95% confidence interval [CI], 0.571 to 0.653; FRAX, 0.547; CoxPH, 0.594; 95% CI, 0.552 to 0.555). Notably, the DeepSurv method without clinical features had a higher C-index (0.614; 95% CI, 0.572 to 0.656) than that of FRAX in women.
Conclusion
DeepSurv, a CNN-based prediction algorithm using baseline image and clinical information, outperformed the FRAX and CoxPH models in predicting osteoporotic fracture from spine radiographs in a longitudinal cohort. -
Citations
Citations to this article as recorded by- Automated detection of vertebral fractures from X-ray images: A novel machine learning model and survey of the field
Li-Wei Cheng, Hsin-Hung Chou, Yu-Xuan Cai, Kuo-Yuan Huang, Chin-Chiang Hsieh, Po-Lun Chu, I-Szu Cheng, Sun-Yuan Hsieh
Neurocomputing.2024; 566: 126946. CrossRef - Application of radiomics model based on lumbar computed tomography in diagnosis of elderly osteoporosis
Baisen Chen, Jiaming Cui, Chaochen Li, Pengjun Xu, Guanhua Xu, Jiawei Jiang, Pengfei Xue, Yuyu Sun, Zhiming Cui
Journal of Orthopaedic Research.2024;[Epub] CrossRef - Machine Learning and Deep Learning in Spinal Injury: A Narrative Review of Algorithms in Diagnosis and Prognosis
Satoshi Maki, Takeo Furuya, Masahiro Inoue, Yasuhiro Shiga, Kazuhide Inage, Yawara Eguchi, Sumihisa Orita, Seiji Ohtori
Journal of Clinical Medicine.2024; 13(3): 705. CrossRef - A CT-based Deep Learning Model for Predicting Subsequent Fracture Risk in Patients with Hip Fracture
Yisak Kim, Young-Gon Kim, Jung-Wee Park, Byung Woo Kim, Youmin Shin, Sung Hye Kong, Jung Hee Kim, Young-Kyun Lee, Sang Wan Kim, Chan Soo Shin
Radiology.2024;[Epub] CrossRef - A Novel QCT-Based Deep Transfer Learning Approach for Predicting Stiffness Tensor of Trabecular Bone Cubes
Pengwei Xiao, Tinghe Zhang, Yufei Huang, Xiaodu Wang
IRBM.2024; 45(2): 100831. CrossRef - Development and Validation of a Convolutional Neural Network Model to Predict a Pathologic Fracture in the Proximal Femur Using Abdomen and Pelvis CT Images of Patients With Advanced Cancer
Min Wook Joo, Taehoon Ko, Min Seob Kim, Yong-Suk Lee, Seung Han Shin, Yang-Guk Chung, Hong Kwon Lee
Clinical Orthopaedics & Related Research.2023; 481(11): 2247. CrossRef - Automated Opportunistic Trabecular Volumetric Bone Mineral Density Extraction Outperforms Manual Measurements for the Prediction of Vertebral Fractures in Routine CT
Sophia S. Goller, Jon F. Rischewski, Thomas Liebig, Jens Ricke, Sebastian Siller, Vanessa F. Schmidt, Robert Stahl, Julian Kulozik, Thomas Baum, Jan S. Kirschke, Sarah C. Foreman, Alexandra S. Gersing
Diagnostics.2023; 13(12): 2119. CrossRef - Machine learning‐based prediction of osteoporosis in postmenopausal women with clinical examined features: A quantitative clinical study
Kainat A. Ullah, Faisal Rehman, Muhammad Anwar, Muhammad Faheem, Naveed Riaz
Health Science Reports.2023;[Epub] CrossRef - Skeletal Fracture Detection with Deep Learning: A Comprehensive Review
Zhihao Su, Afzan Adam, Mohammad Faidzul Nasrudin, Masri Ayob, Gauthamen Punganan
Diagnostics.2023; 13(20): 3245. CrossRef - Deep learning system for automated detection of posterior ligamentous complex injury in patients with thoracolumbar fracture on MRI
Sang Won Jo, Eun Kyung Khil, Kyoung Yeon Lee, Il Choi, Yu Sung Yoon, Jang Gyu Cha, Jae Hyeok Lee, Hyunggi Kim, Sun Yeop Lee
Scientific Reports.2023;[Epub] CrossRef - Vertebra Segmentation Based Vertebral Compression Fracture Determination from Reconstructed Spine X-Ray Images
Srinivasa Rao Gadu, Chandra Sekhar Potala
International Journal of Electrical and Electronics Research.2023; 11(4): 1225. CrossRef - Computer Vision in Osteoporotic Vertebral Fracture Risk Prediction: A Systematic Review
Anthony K. Allam, Adrish Anand, Alex R. Flores, Alexander E. Ropper
Neurospine.2023; 20(4): 1112. CrossRef - A Meaningful Journey to Predict Fractures with Deep Learning
Jeonghoon Ha
Endocrinology and Metabolism.2022; 37(4): 617. CrossRef - New Horizons: Artificial Intelligence Tools for Managing Osteoporosis
Hans Peter Dimai
The Journal of Clinical Endocrinology & Metabolism.2022;[Epub] CrossRef
- Automated detection of vertebral fractures from X-ray images: A novel machine learning model and survey of the field

- Diabetes, Obesity and Metabolism
- The Presence of Clonal Hematopoiesis Is Negatively Associated with Diabetic Peripheral Neuropathy in Type 2 Diabetes
- Tae Jung Oh, Han Song, Youngil Koh, Sung Hee Choi
- Endocrinol Metab. 2022;37(2):243-248. Published online April 25, 2022
- DOI: https://doi.org/10.3803/EnM.2021.1337

- 3,339 View
- 123 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Clonal hematopoiesis of indeterminate potential (CHIP) has been reported to be associated with increased cardiovascular disease, aging and insulin resistance. Despite the debate of causal contribution of CHIP on metabolic diseases, we want to explore whether CHIP is related to diabetic peripheral neuropathy (DPN).
Methods
This study analyzed the prevalence of CHIP in patients with type 2 diabetes classified according to DPN status. Logistic regression analysis was used to evaluate the association between CHIP and DPN.
Results
CHIP was more prevalent in subjects without DPN than those with DPN (19.9% vs. 8.8%, respectively; P=0.013). Individuals having any CHIP, or DNA methyltransferase 3A (DNMT3A) CHIP were less likely to have any abnormality shown in DPN test; the adjusted odds ratio were 0.85 (95% confidence interval [CI], 0.73 to 1.00) and 0.70 (95% CI, 0.56 to 0.89), respectively. Interestingly, DNMT3A CHIP showed the negative association, but Tet methylcytosine dioxygenase 2 (TET2) CHIP showed the positive association with abnormal feet electrochemical skin conductance level.
Conclusion
On the contrary to expectations, CHIP was negatively associated with DPN. Functional linking between the mutation in hematopoietic cells and DPN, and the opposite role of DNMT3A and TET2 should be investigated. -
Citations
Citations to this article as recorded by- TET2 mutation as prototypic clonal hematopoiesis lesion
Luca Guarnera, Babal K. Jha
Seminars in Hematology.2024; 61(1): 51. CrossRef - Clonal hematopoiesis with DNMT3A mutation is associated with lower white matter hyperintensity volume
Woo‐Jin Lee, Keun‐Hwa Jung, Han Song, Heesun Lee, Hyo Eun Park, Youngil Koh, Su‐Yeon Choi, Kyung‐Il Park
CNS Neuroscience & Therapeutics.2023; 29(5): 1243. CrossRef
- TET2 mutation as prototypic clonal hematopoiesis lesion

- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database) - Cumulative Exposure to High γ-Glutamyl Transferase Level and Risk of Diabetes: A Nationwide Population-Based Study
- Ji-Yeon Park, Kyungdo Han, Hun-Sung Kim, Jae-Hyoung Cho, Kun-Ho Yoon, Mee Kyoung Kim, Seung-Hwan Lee
- Endocrinol Metab. 2022;37(2):272-280. Published online April 13, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1416

- 3,079 View
- 101 Download
- 5 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Elevated γ-glutamyl transferase (γ-GTP) level is associated with metabolic syndrome, impaired glucose tolerance, and insulin resistance, which are risk factors for type 2 diabetes. We aimed to investigate the association of cumulative exposure to high γ-GTP level with risk of diabetes.
Methods
Using nationally representative data from the Korean National Health Insurance system, 346,206 people who were free of diabetes and who underwent 5 consecutive health examinations from 2005 to 2009 were followed to the end of 2018. High γ-GTP level was defined as those in the highest quartile, and the number of exposures to high γ-GTP level ranged from 0 to 5. Hazard ratio (HR) and 95% confidence interval (CI) for diabetes were analyzed using the multivariable Cox proportional-hazards model.
Results
The mean follow-up duration was 9.2±1.0 years, during which 15,183 (4.4%) patients developed diabetes. There was a linear increase in the incidence rate and the risk of diabetes with cumulative exposure to high γ-GTP level. After adjusting for possible confounders, the HR of diabetes in subjects with five consecutive high γ-GTP levels were 2.60 (95% CI, 2.47 to 2.73) in men and 3.05 (95% CI, 2.73 to 3.41) in women compared with those who never had a high γ-GTP level. Similar results were observed in various subgroup and sensitivity analyses.
Conclusion
There was a linear relationship between cumulative exposure to high γ-GTP level and risk of diabetes. Monitoring and lowering γ-GTP level should be considered for prevention of diabetes in the general population. -
Citations
Citations to this article as recorded by- Validation of Estimated Small Dense Low-Density Lipoprotein Cholesterol Concentration in a Japanese General Population
Keisuke Endo, Ryo Kobayashi, Makito Tanaka, Marenao Tanaka, Yukinori Akiyama, Tatsuya Sato, Itaru Hosaka, Kei Nakata, Masayuki Koyama, Hirofumi Ohnishi, Satoshi Takahashi, Masato Furuhashi
Journal of Atherosclerosis and Thrombosis.2023;[Epub] CrossRef - Long-Term Cumulative Exposure to High γ-Glutamyl Transferase Levels and the Risk of Cardiovascular Disease: A Nationwide Population-Based Cohort Study
Han-Sang Baek, Bongseong Kim, Seung-Hwan Lee, Dong-Jun Lim, Hyuk-Sang Kwon, Sang-Ah Chang, Kyungdo Han, Jae-Seung Yun
Endocrinology and Metabolism.2023; 38(6): 770. CrossRef - Elevated gamma‐glutamyl transferase to high‐density lipoprotein cholesterol ratio has a non‐linear association with incident diabetes mellitus: A second analysis of a cohort study
Haofei Hu, Yong Han, Mijie Guan, Ling Wei, Qijun Wan, Yanhua Hu
Journal of Diabetes Investigation.2022; 13(12): 2027. CrossRef - Gamma-glutamyl transferase to high-density lipoprotein cholesterol ratio: A valuable predictor of type 2 diabetes mellitus incidence
Wangcheng Xie, Bin Liu, Yansong Tang, Tingsong Yang, Zhenshun Song
Frontiers in Endocrinology.2022;[Epub] CrossRef
- Validation of Estimated Small Dense Low-Density Lipoprotein Cholesterol Concentration in a Japanese General Population

- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database) - Frequency of Exposure to Impaired Fasting Glucose and Risk of Mortality and Cardiovascular Outcomes
- Seung-Hwan Lee, Kyungdo Han, Hyuk-Sang Kwon, Mee Kyoung Kim
- Endocrinol Metab. 2021;36(5):1007-1015. Published online October 21, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1218
- 3,825 View
- 126 Download
- 12 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Metabolic abnormalities, such as impaired fasting glucose (IFG), are dynamic phenomena; however, it is unclear whether the timing of IFG exposure and cumulative exposure to IFG are related to cardiovascular disease (CVD) and mortality risk.
Methods
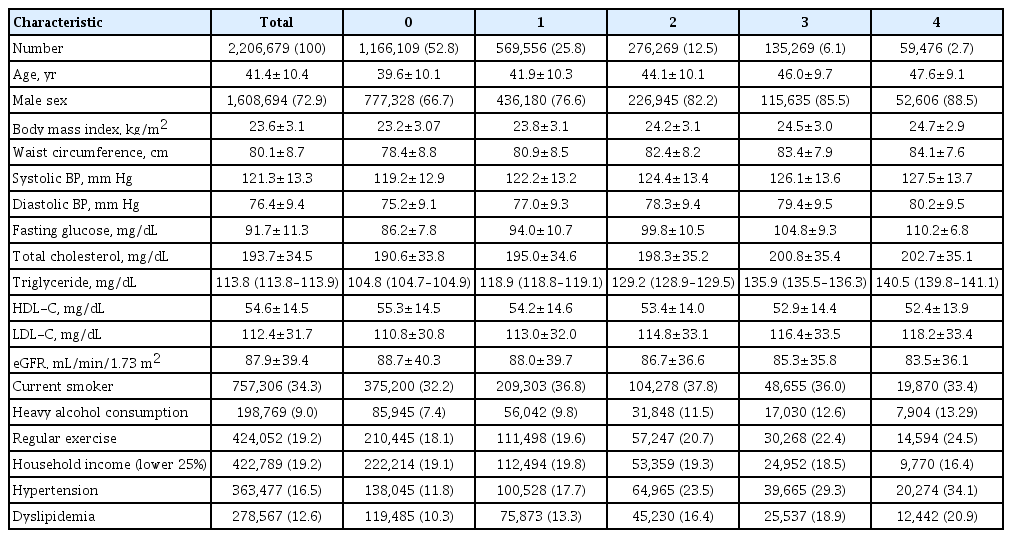
Data were extracted from a nationwide population-based cohort in South Korea for adults (n=2,206,679) who were free of diabetes and had 4 years of consecutive health examination data. Fasting blood glucose levels of 100 to 125 mg/dL were defined as IFG, and the number of IFG diagnoses for each adult in the 4-year period was tabulated as the IFG exposure score (range, 0 to 4). Adults with persistent IFG for the 4-year period received a score of 4.
Results
The median follow-up was 8.2 years. There were 24,820 deaths, 13,502 cases of stroke, and 13,057 cases of myocardial infarction (MI). IFG exposure scores of 1, 2, 3, and 4 were associated with all-cause mortality (multivariable-adjusted hazard ratio [aHR], 1.11; 95% confidence interval [CI], 1.08 to 1.15; aHR, 1.16; 95% CI, 1.12 to 1.20; aHR, 1.20; 95% CI, 1.15 to 1.25; aHR, 1.18; 95% CI, 1.11 to 1.25, respectively) compared with an IFG exposure score of 0. Adjusting for hypertension and dyslipidemia attenuated the slightly increased risk of MI or stroke associated with high IFG exposure scores, but significant associations for allcause mortality remained.
Conclusion
The intensity of IFG exposure was associated with an elevated risk of all-cause mortality, independent of cardiovascular risk factors. The association between IFG exposure and CVD risk was largely mediated by the coexistence of dyslipidemia and hypertension. -
Citations
Citations to this article as recorded by- A nationwide cohort study on diabetes severity and risk of Parkinson disease
Kyungdo Han, Bongsung Kim, Seung Hwan Lee, Mee Kyoung Kim
npj Parkinson's Disease.2023;[Epub] CrossRef - Diabetes severity is strongly associated with the risk of active tuberculosis in people with type 2 diabetes: a nationwide cohort study with a 6-year follow-up
Ji Young Kang, Kyungdo Han, Seung-Hwan Lee, Mee Kyoung Kim
Respiratory Research.2023;[Epub] CrossRef - Construction and Validation of a Model for Predicting Impaired Fasting Glucose Based on More Than 4000 General Population
Cuicui Wang, Xu Zhang, Chenwei Li, Na Li, Xueni Jia, Hui Zhao
International Journal of General Medicine.2023; Volume 16: 1415. CrossRef - Factors Affecting High Body Weight Variability
Kyungdo Han, Mee Kyoung Kim
Journal of Obesity & Metabolic Syndrome.2023; 32(2): 163. CrossRef - Exposure to perfluoroalkyl and polyfluoroalkyl substances and risk of stroke in adults: a meta-analysis
Min Cheol Chang, Seung Min Chung, Sang Gyu Kwak
Reviews on Environmental Health.2023;[Epub] CrossRef - Cumulative effect of impaired fasting glucose on the risk of dementia in middle-aged and elderly people: a nationwide cohort study
Jin Yu, Kyu-Na Lee, Hun-Sung Kim, Kyungdo Han, Seung-Hwan Lee
Scientific Reports.2023;[Epub] CrossRef - A Longitudinal Retrospective Observational Study on Obesity Indicators and the Risk of Impaired Fasting Glucose in Pre- and Postmenopausal Women
Myung Ji Nam, Hyunjin Kim, Yeon Joo Choi, Kyung-Hwan Cho, Seon Mee Kim, Yong-Kyun Roh, Kyungdo Han, Jin-Hyung Jung, Yong-Gyu Park, Joo-Hyun Park, Do-Hoon Kim
Journal of Clinical Medicine.2022; 11(10): 2795. CrossRef - Current Trends of Big Data Research Using the Korean National Health Information Database
Mee Kyoung Kim, Kyungdo Han, Seung-Hwan Lee
Diabetes & Metabolism Journal.2022; 46(4): 552. CrossRef - Lipid cutoffs for increased cardiovascular disease risk in non-diabetic young people
Mee Kyoung Kim, Kyungdo Han, Hun-Sung Kim, Kun-Ho Yoon, Seung-Hwan Lee
European Journal of Preventive Cardiology.2022; 29(14): 1866. CrossRef - Low-Density Lipoprotein Cholesterol Level, Statin Use and Myocardial Infarction Risk in Young Adults
Heekyoung Jeong, Kyungdo Han, Soon Jib Yoo, Mee Kyoung Kim
Journal of Lipid and Atherosclerosis.2022; 11(3): 288. CrossRef - Additive interaction of diabetes mellitus and chronic kidney disease in cancer patient mortality risk
Seohyun Kim, Gyuri Kim, Jae Hyeon Kim
Scientific Reports.2022;[Epub] CrossRef
- A nationwide cohort study on diabetes severity and risk of Parkinson disease

Review Articles
- Calcium & Bone Metabolism
- Review and Update of the Risk Factors and Prevention of Antiresorptive-Related Osteonecrosis of the Jaw
- Ha Young Kim
- Endocrinol Metab. 2021;36(5):917-927. Published online October 21, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1170
- 4,454 View
- 268 Download
- 8 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
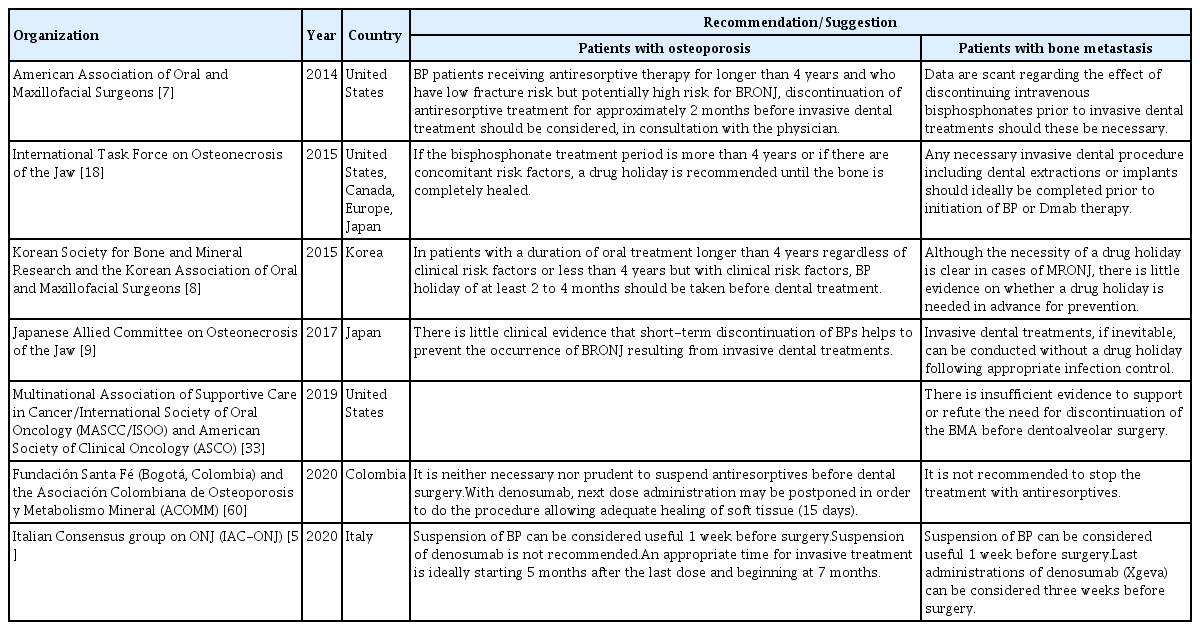
ePub - Antiresorptive-related osteonecrosis of the jaw (ARONJ) is a rare but serious adverse event of bisphosphonate or denosumab administration; it is associated with severe pain and a deteriorated quality of life. Since its first report in 2003, there have been many studies on its definition, epidemiology, pathophysiology, diagnosis, and treatment. Nevertheless, the epidemiology and mechanisms underlying this condition have not yet been fully delineated and several risk factors are known. Moreover, as there is no effective treatment currently available for osteonecrosis of the jaw, prevention is essential. Furthermore, close cooperation between prescribing physicians and dentists is important. The aim of this review was to provide up-to-date information regarding the risk factors and prevention of ARONJ from a physician’s perspective.
-
Citations
Citations to this article as recorded by- Risk factors for dental findings of the development of medication-related osteonecrosis of the jaw: Investigation of 3734 teeth in cancer patients receiving high dose antiresorptive agents
Mitsunobu Otsuru, Yoshinari Fujiki, Sakiko Soutome, Norio Nakamura, Taro Miyoshi, Tomofumi Naruse, Mizuho Ohnuma, Yuka Hotokezaka, Satoshi Rokutanda, Masahiro Umeda
Journal of Dental Sciences.2024; 19(1): 203. CrossRef - Editorial: Immunological processes in maxillofacial bone pathology
Matthias Tröltzsch
Frontiers in Immunology.2024;[Epub] CrossRef - Polysacharide of Agaricus blazei gel mitigates bone necrosis in model of the jaws related to bisphosphonate via Wnt signaling
Vanessa Costa de Sousa, Fátima Regina Nunes Sousa, Raquel Felipe Vasconcelos, Gisele Angelino Barreto, Conceição S. Martins, Nilson Romero Dias, Sislana Costa, Maria Jennifer Chaves Bernardino, George de Almeida Silva, Nadine Linhares, Delane Gondim, Mirn
Scientific Reports.2024;[Epub] CrossRef - When and how to stop denosumab therapy in a patient with osteoporosis
Eirena L. Goulden, Rachel K. Crowley
Clinical Endocrinology.2023; 98(5): 649. CrossRef - Clinical and Histopathological Aspects of MRONJ in Cancer Patients
George Adrian Ciobanu, Laurențiu Mogoantă, Adrian Camen, Mihaela Ionescu, Daniel Vlad, Ionela Elisabeta Staicu, Cristina Maria Munteanu, Mircea Ionuț Gheorghiță, Răzvan Mercuț, Elena Claudia Sin, Sanda Mihaela Popescu
Journal of Clinical Medicine.2023; 12(10): 3383. CrossRef - Bisphosphonates and osteonecrosis of the jaws: Clinical and forensic aspects
Diana Nogueira, Inês Morais Caldas, Ricardo Jorge Dinis-Oliveira
Archives of Oral Biology.2023; 155: 105792. CrossRef - Correlations between Immune Response and Etiopathogenic Factors of Medication-Related Osteonecrosis of the Jaw in Cancer Patients Treated with Zoledronic Acid
George Adrian Ciobanu, Laurențiu Mogoantă, Sanda Mihaela Popescu, Mihaela Ionescu, Cristina Maria Munteanu, Ionela Elisabeta Staicu, Răzvan Mercuț, Cristian Corneliu Georgescu, Monica Scrieciu, Daniel Vlad, Adrian Camen
International Journal of Molecular Sciences.2023; 24(18): 14345. CrossRef - Analysis of the Degree of Information of Dental Surgeons about Antiresorptive Drugs According to the Time Since Graduation in Dentistry
Flávia Godinho Costa Wanderley Rocha, Roberto Paulo Correia de Araújo
Pesquisa Brasileira em Odontopediatria e Clínica Integrada.2023;[Epub] CrossRef - Safety and Efficacy of Pamidronate in Neonatal Hypercalcemia Caused by Subcutaneous Fat Necrosis: A Case Report
Stefano Martinelli, Marco Pitea, Italo Francesco Gatelli, Tara Raouf, Graziano Barera, Ottavio Vitelli
Frontiers in Pediatrics.2022;[Epub] CrossRef - Zoledronic acid for osteoporosis and associated low-energy fractures
S. S. Rodionova, A. F. Kolondaev, A. N. Torgashin, I. A. Solomyannik
Meditsinskiy sovet = Medical Council.2022; (21): 163. CrossRef
- Risk factors for dental findings of the development of medication-related osteonecrosis of the jaw: Investigation of 3734 teeth in cancer patients receiving high dose antiresorptive agents

- Obesity and Metabolism
- An Update on Contraception in Polycystic Ovary Syndrome
- Seda Hanife Oguz, Bulent Okan Yildiz
- Endocrinol Metab. 2021;36(2):296-311. Published online April 15, 2021
- DOI: https://doi.org/10.3803/EnM.2021.958
- 11,859 View
- 752 Download
- 14 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
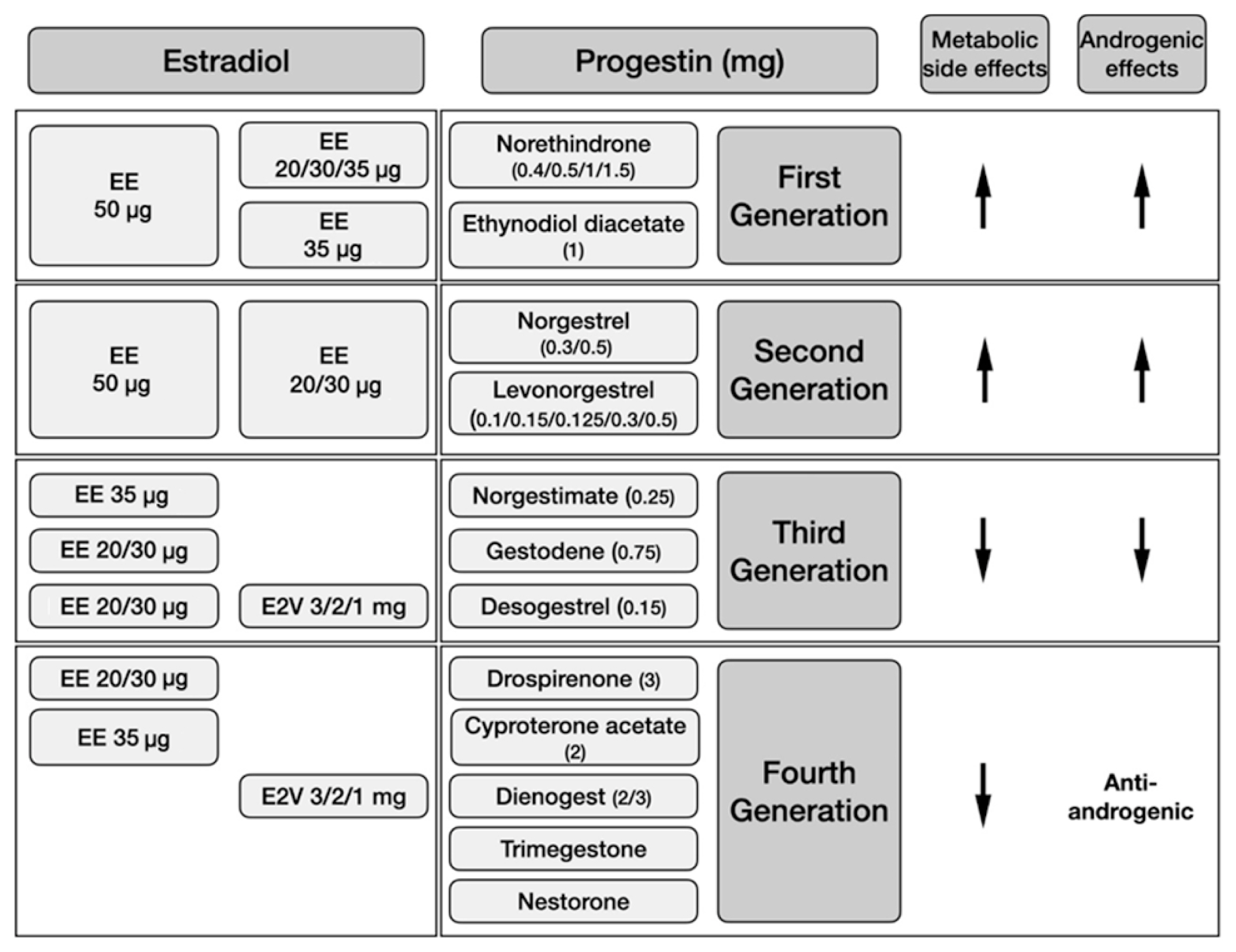
ePub - Polycystic ovary syndrome (PCOS) is a common endocrine disorder in reproductive-aged women, characterized by hyperandrogenism, oligo/anovulation, and polycystic ovarian morphology. Combined oral contraceptives (COCs), along with lifestyle modifications, represent the first-line medical treatment for the long-term management of PCOS. Containing low doses of estrogen and different types of progestin, COCs restore menstrual cyclicity, improve hyperandrogenism, and provide additional benefits such as reducing the risk of endometrial cancer. However, potential cardiometabolic risk associated with these agents has been a concern. COCs increase the risk of venous thromboembolism (VTE), related both to the dose of estrogen and the type of progestin involved. Arterial thrombotic events related to COC use occur much less frequently, and usually not a concern for young patients. All patients diagnosed with PCOS should be carefully evaluated for cardiometabolic risk factors at baseline, before initiating a COC. Age, smoking, obesity, glucose intolerance or diabetes, hypertension, dyslipidemia, thrombophilia, and family history of VTE should be recorded. Patients should be re-assessed at consecutive visits, more closely if any baseline cardiometabolic risk factor is present. Individual risk assessment is the key in order to avoid unfavorable outcomes related to COC use in women with PCOS.
-
Citations
Citations to this article as recorded by- Clinical management of androgen excess and defect in women
Elena Rosato, Francesca Sciarra, Marianna Minnetti, Anisa Degjoni, Mary Anna Venneri
Expert Review of Endocrinology & Metabolism.2024; 19(1): 21. CrossRef - Il rischio tromboembolico nella sindrome dell’ovaio policistico
Davide Ceccato, Francesca Dassie, Pietro Maffei, Roberto Mioni
L'Endocrinologo.2024; 25(2): 151. CrossRef - Systematic exploration of network pharmacology, in silico modeling and pharmacokinetic profiling for vitamin E in polycystic ovarian syndrome
Rukaiah Fatma Begum, Sumithra Mohan
Future Science OA.2024;[Epub] CrossRef - Current and emerging drug treatment strategies for polycystic ovary syndrome
Nafiye Helvaci, Bulent Okan Yildiz
Expert Opinion on Pharmacotherapy.2023; 24(1): 105. CrossRef - Weighted Gene Co-Expression Network Analysis (WGCNA) Discovered Novel Long Non-Coding RNAs for Polycystic Ovary Syndrome
Roozbeh Heidarzadehpilehrood, Maryam Pirhoushiaran, Malina Binti Osman, Habibah Abdul Hamid, King-Hwa Ling
Biomedicines.2023; 11(2): 518. CrossRef - The mechanism of Leonuri Herba in improving polycystic ovary syndrome was analyzed based on network pharmacology and molecular docking
Mali Wu, Hua Liu, Jie Zhang, Fangfang Dai, Yiping Gong, Yanxiang Cheng
Journal of Pharmacy & Pharmaceutical Sciences.2023;[Epub] CrossRef - Evaluation of the efficacy of an antioxidant combination for the modulation of metabolic, endocrine, and clinical parameters in patients with polycystic ovary syndrome
Carmen Pingarrón Santofímia, Silvia Poyo Torcal, Helena López Verdú, Alexandra Henríquez Linares, Virginia Calvente Aguilar, Pablo Terol Sánchez, María Sol Martínez García, Pilar Lafuente González
Gynecological Endocrinology.2023;[Epub] CrossRef - Contemporary Management of the Patient with Polycystic Ovary Syndrome
Nicolás Omar Francone, Tia Ramirez, Christina E. Boots
Obstetrics and Gynecology Clinics of North America.2023; 50(4): 695. CrossRef - Challenges in diagnosis and health care in polycystic ovary syndrome in Canada: a patient view to improve health care
Beate C. Sydora, Michaelann S. Wilke, Maggie McPherson, Sarah Chambers, Mahua Ghosh, Donna F. Vine
BMC Women's Health.2023;[Epub] CrossRef - Effect of Berberine Phytosome on reproductive, dermatologic, and metabolic characteristics in women with polycystic ovary syndrome: a controlled, randomized, multi-centric, open-label clinical trial
Francesco Di Pierro, Ruqqia Sultana, Amna Zia Eusaph, Saida Abrar, Mahroo Bugti, Fauzia Afridi, Umer Farooq, Somia Iqtadar, Fareeha Ghauri, Syeda Makhduma, Shazia Nourin, Ayesha Kanwal, Aasiya Bano, Ali Akbar Bugti, Shah Mureed, Ayesha Ghazal, Romana Irsh
Frontiers in Pharmacology.2023;[Epub] CrossRef - Investigation of taste function and eating behavior in women with polycystic ovary syndrome
Sila Cetik, Aylin Acikgoz, Bulent Okan Yildiz
Appetite.2022; 168: 105776. CrossRef - microRNAs and long non‐coding RNAs as biomarkers for polycystic ovary syndrome
Mona Tamaddon, Mostafa Azimzadeh, Seyed Mohammad Tavangar
Journal of Cellular and Molecular Medicine.2022; 26(3): 654. CrossRef - Effect of orlistat during individualized comprehensive life-style intervention on visceral fat in overweight or obese PCOS patients
Min Min, Xiangyan Ruan, Husheng Wang, Jiaojiao Cheng, Suiyu Luo, Zhongting Xu, Meng Li, Alfred Otto Mueck
Gynecological Endocrinology.2022; 38(8): 676. CrossRef - Effect of metformin and exenatide on pregnancy rate and pregnancy outcomes in overweight or obese infertility PCOS women: long-term follow-up of an RCT
Renyuan Li, Tingting Mai, Siyuan Zheng, Ying Zhang
Archives of Gynecology and Obstetrics.2022; 306(5): 1711. CrossRef - Oral contraceptives and stroke: Foes or friends
Varun Reddy, Megan Wurtz, Shahil H. Patel, Micheline McCarthy, Ami P. Raval
Frontiers in Neuroendocrinology.2022; 67: 101016. CrossRef - Clinical profiling of polycystic ovary syndrome patients in Kashmir population
Ahila Ashraf, Rajesh Singh, Shahnawaz Mir
Matrix Science Pharma.2022; 6(1): 23. CrossRef
- Clinical management of androgen excess and defect in women

Original Articles
- Clinical Study
- Development of a Non-Invasive Liver Fibrosis Score Based on Transient Elastography for Risk Stratification in Patients with Type 2 Diabetes
- Chi-Ho Lee, Wai-Kay Seto, Kelly Ieong, David T.W. Lui, Carol H.Y. Fong, Helen Y. Wan, Wing-Sun Chow, Yu-Cho Woo, Man-Fung Yuen, Karen S.L. Lam
- Endocrinol Metab. 2021;36(1):134-145. Published online February 24, 2021
- DOI: https://doi.org/10.3803/EnM.2020.887
- 4,486 View
- 131 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
In non-alcoholic fatty liver disease (NAFLD), transient elastography (TE) is an accurate non-invasive method to identify patients at risk of advanced fibrosis (AF). We developed a diabetes-specific, non-invasive liver fibrosis score based on TE to facilitate AF risk stratification, especially for use in diabetes clinics where TE is not readily available.
Methods
Seven hundred sixty-six adults with type 2 diabetes and NAFLD were recruited and randomly divided into a training set (n=534) for the development of diabetes fibrosis score (DFS), and a testing set (n=232) for internal validation. DFS identified patients with AF on TE, defined as liver stiffness (LS) ≥9.6 kPa, based on a clinical model comprising significant determinants of LS with the lowest Akaike information criteria. The performance of DFS was compared with conventional liver fibrosis scores (NFS, FIB-4, and APRI), using area under the receiver operating characteristic curve (AUROC), sensitivity, specificity, positive and negative predictive values (NPV).
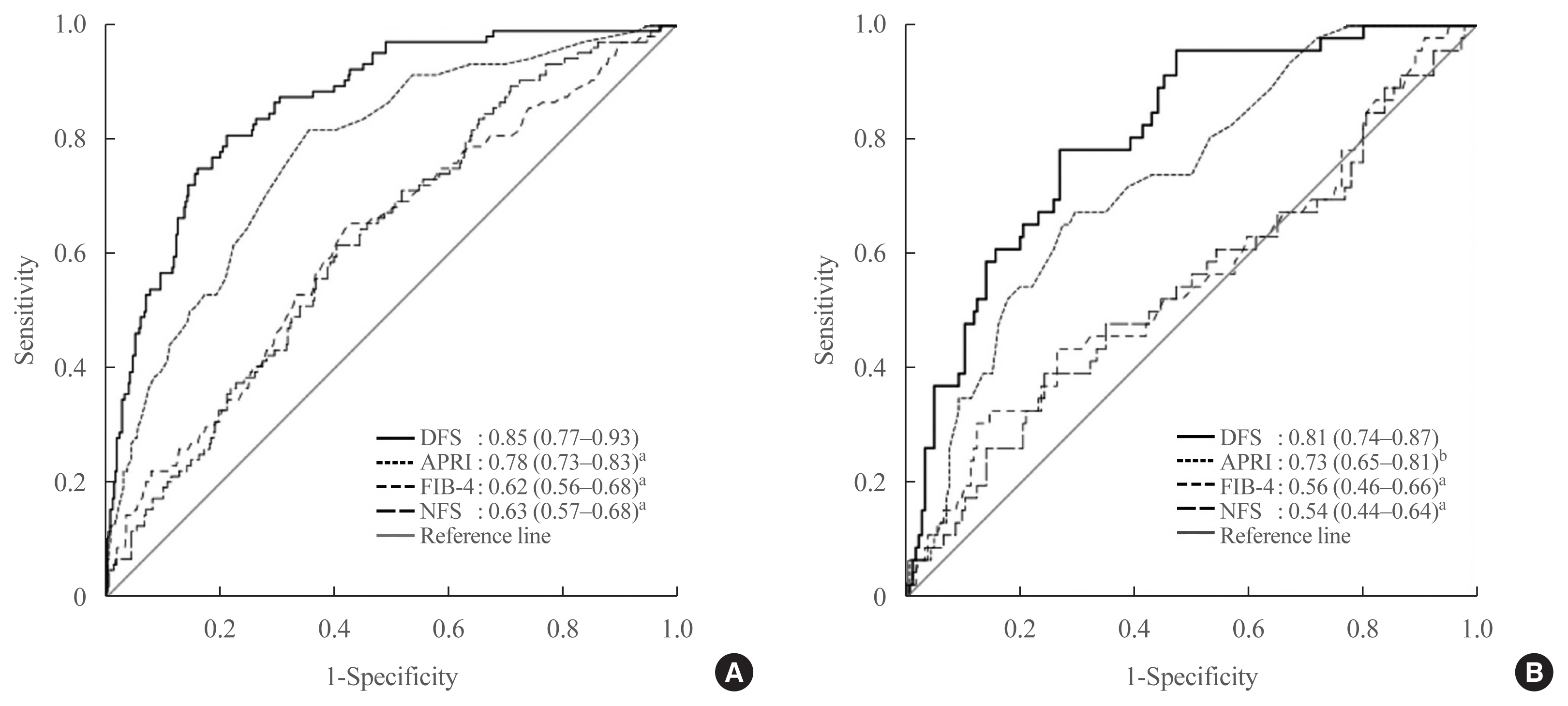
Results
DFS comprised body mass index, platelet, aspartate aminotransferase, high-density lipoprotein cholesterol, and albuminuria, five routine measurements in standard diabetes care. Derived low and high DFS cut-offs were 0.1 and 0.3, with 90% sensitivity and 90% specificity, respectively. Both cut-offs provided better NPVs of >90% than conventional fibrosis scores. The AUROC of DFS for AF on TE was also higher (P<0.01) than the conventional fibrosis scores, being 0.85 and 0.81 in the training and testing sets, respectively.
Conclusion
Compared to conventional fibrosis scores, DFS, with a high NPV, more accurately identified diabetes patients at-risk of AF, who need further evaluation by hepatologists. -
Citations
Citations to this article as recorded by- Implementation of a liver health check in people with type 2 diabetes
Kushala W M Abeysekera, Luca Valenti, Zobair Younossi, John F Dillon, Alina M Allen, Mazen Noureddin, Mary E Rinella, Frank Tacke, Sven Francque, Pere Ginès, Maja Thiele, Philip N Newsome, Indra Neil Guha, Mohammed Eslam, Jörn M Schattenberg, Saleh A Alqa
The Lancet Gastroenterology & Hepatology.2024; 9(1): 83. CrossRef - Sequential algorithm to stratify liver fibrosis risk in overweight/obese metabolic dysfunction-associated fatty liver disease
Chi-Ho Lee, David Tak-Wai Lui, Raymond Hang-Wun Li, Michele Mae-Ann Yuen, Carol Ho-Yi Fong, Ambrose Pak-Wah Leung, Justin Chiu-Man Chu, Loey Lung-Yi Mak, Tai-Hing Lam, Jean Woo, Yu-Cho Woo, Aimin Xu, Hung-Fat Tse, Kathryn Choon-Beng Tan, Bernard Man-Yung
Frontiers in Endocrinology.2023;[Epub] CrossRef - Non-Invasive Measurement of Hepatic Fibrosis by Transient Elastography: A Narrative Review
Luca Rinaldi, Chiara Giorgione, Andrea Mormone, Francesca Esposito, Michele Rinaldi, Massimiliano Berretta, Raffaele Marfella, Ciro Romano
Viruses.2023; 15(8): 1730. CrossRef - Metabolic dysfunction-associated fatty liver disease — How relevant is this to primary care physicians and diabetologists?
Chi-Ho Lee
Primary Care Diabetes.2022; 16(2): 245. CrossRef - Non‐alcoholic fatty liver disease and type 2 diabetes: An update
Chi‐H Lee, David TW Lui, Karen SL Lam
Journal of Diabetes Investigation.2022; 13(6): 930. CrossRef - Ultrasound-Based Hepatic Elastography in Non-Alcoholic Fatty Liver Disease: Focus on Patients with Type 2 Diabetes
Georgiana-Diana Cazac, Cristina-Mihaela Lăcătușu, Cătălina Mihai, Elena-Daniela Grigorescu, Alina Onofriescu, Bogdan-Mircea Mihai
Biomedicines.2022; 10(10): 2375. CrossRef
- Implementation of a liver health check in people with type 2 diabetes

- Clinical Study
- Predicting the Development of Myocardial Infarction in Middle-Aged Adults with Type 2 Diabetes: A Risk Model Generated from a Nationwide Population-Based Cohort Study in Korea
- Seung-Hwan Lee, Kyungdo Han, Hun-Sung Kim, Jae-Hyoung Cho, Kun-Ho Yoon, Mee Kyoung Kim
- Endocrinol Metab. 2020;35(3):636-646. Published online September 22, 2020
- DOI: https://doi.org/10.3803/EnM.2020.704
- 4,982 View
- 110 Download
- 10 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Most of the widely used prediction models for cardiovascular disease are known to overestimate the risk of this disease in Asians. We aimed to generate a risk model for predicting myocardial infarction (MI) in middle-aged Korean subjects with type 2 diabetes.
Methods
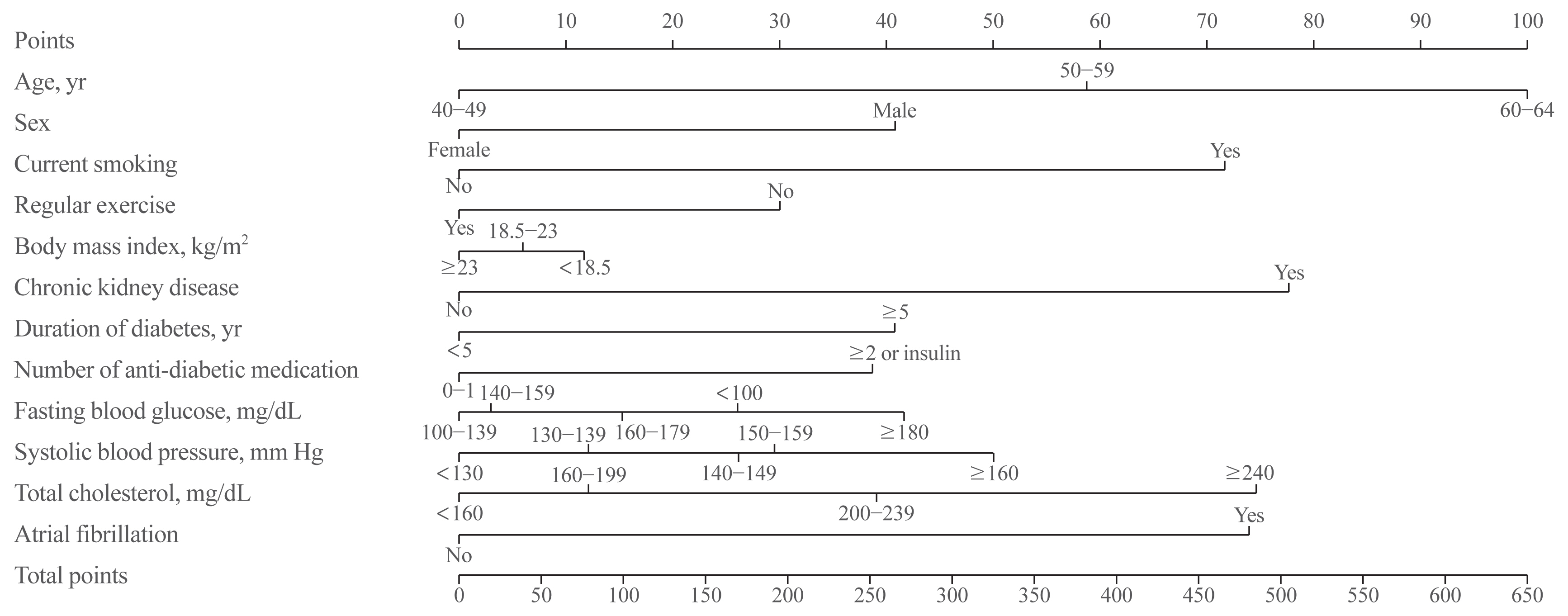
A total of 1,272,992 subjects with type 2 diabetes aged 40 to 64 who received health examinations from 2009 to 2012 were recruited from the Korean National Health Insurance database. Seventy percent of the subjects (n=891,095) were sampled to develop the risk prediction model, and the remaining 30% (n=381,897) were used for internal validation. A Cox proportional hazards regression model and Cox coefficients were used to derive a risk scoring system. Twelve risk variables were selected, and a risk nomogram was created to estimate the 5-year risk of MI.
Results
During 7.1 years of follow-up, 24,809 cases of MI (1.9%) were observed. Age, sex, smoking status, regular exercise, body mass index, chronic kidney disease, duration of diabetes, number of anti-diabetic medications, fasting blood glucose, systolic blood pressure, total cholesterol, and atrial fibrillation were significant risk factors for the development of MI and were incorporated into the risk model. The concordance index for MI prediction was 0.682 (95% confidence interval [CI], 0.678 to 0.686) in the development cohort and 0.669 (95% CI, 0.663 to 0.675) in the validation cohort.
Conclusion
A novel risk engine was generated for predicting the development of MI among middle-aged Korean adults with type 2 diabetes. This model may provide useful information for identifying high-risk patients and improving quality of care. -
Citations
Citations to this article as recorded by- A literature review of quality assessment and applicability to HTA of risk prediction models of coronary heart disease in patients with diabetes
Li Jiu, Junfeng Wang, Francisco Javier Somolinos-Simón, Jose Tapia-Galisteo, Gema García-Sáez, Mariaelena Hernando, Xinyu Li, Rick A. Vreman, Aukje K. Mantel-Teeuwisse, Wim G. Goettsch
Diabetes Research and Clinical Practice.2024; 209: 111574. CrossRef - Predicting the Risk of Insulin-Requiring Gestational Diabetes before Pregnancy: A Model Generated from a Nationwide Population-Based Cohort Study in Korea
Seung-Hwan Lee, Jin Yu, Kyungdo Han, Seung Woo Lee, Sang Youn You, Hun-Sung Kim, Jae-Hyoung Cho, Kun-Ho Yoon, Mee Kyoung Kim
Endocrinology and Metabolism.2023; 38(1): 129. CrossRef - Factors Affecting High Body Weight Variability
Kyungdo Han, Mee Kyoung Kim
Journal of Obesity & Metabolic Syndrome.2023; 32(2): 163. CrossRef - Coronary Artery Calcium Score as a Sensitive Indicator of Cardiovascular Disease in Patients with Type 2 Diabetes Mellitus: A Long-Term Cohort Study
Dae-Jeong Koo, Mi Yeon Lee, Sun Joon Moon, Hyemi Kwon, Sang Min Lee, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki Won Oh, Sung Rae Cho, Young-Hoon Jeong, Eun-Jung Rhee
Endocrinology and Metabolism.2023; 38(5): 568. CrossRef - Serum/plasma biomarkers and the progression of cardiometabolic multimorbidity: a systematic review and meta-analysis
Yichen Jin, Ziyuan Xu, Yuting Zhang, Yue Zhang, Danyang Wang, Yangyang Cheng, Yaguan Zhou, Muhammad Fawad, Xiaolin Xu
Frontiers in Public Health.2023;[Epub] CrossRef - Assessing the Validity of the Criteria for the Extreme Risk Category of Atherosclerotic Cardiovascular Disease: A Nationwide Population-Based Study
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
Journal of Lipid and Atherosclerosis.2022; 11(1): 73. CrossRef - Evaluating Triglyceride and Glucose Index as a Simple and Easy-to-Calculate Marker for All-Cause and Cardiovascular Mortality
Kyung-Soo Kim, Sangmo Hong, You-Cheol Hwang, Hong-Yup Ahn, Cheol-Young Park
Journal of General Internal Medicine.2022; 37(16): 4153. CrossRef - Effects of exercise initiation and smoking cessation after new-onset type 2 diabetes mellitus on risk of mortality and cardiovascular outcomes
Mee Kyoung Kim, Kyungdo Han, Bongsung Kim, Jinyoung Kim, Hyuk-Sang Kwon
Scientific Reports.2022;[Epub] CrossRef - Current Trends of Big Data Research Using the Korean National Health Information Database
Mee Kyoung Kim, Kyungdo Han, Seung-Hwan Lee
Diabetes & Metabolism Journal.2022; 46(4): 552. CrossRef - Lipid cutoffs for increased cardiovascular disease risk in non-diabetic young people
Mee Kyoung Kim, Kyungdo Han, Hun-Sung Kim, Kun-Ho Yoon, Seung-Hwan Lee
European Journal of Preventive Cardiology.2022; 29(14): 1866. CrossRef - Low-Density Lipoprotein Cholesterol Level, Statin Use and Myocardial Infarction Risk in Young Adults
Heekyoung Jeong, Kyungdo Han, Soon Jib Yoo, Mee Kyoung Kim
Journal of Lipid and Atherosclerosis.2022; 11(3): 288. CrossRef - Nonalcoholic fatty liver disease and the risk of insulin-requiring gestational diabetes
Sang Youn You, Kyungdo Han, Seung-Hawn Lee, Mee Kyoung Kim
Diabetology & Metabolic Syndrome.2021;[Epub] CrossRef
- A literature review of quality assessment and applicability to HTA of risk prediction models of coronary heart disease in patients with diabetes

- Clinical Study
- Achievement of LDL-C Targets Defined by ESC/EAS (2011) Guidelines in Risk-Stratified Korean Patients with Dyslipidemia Receiving Lipid-Modifying Treatments
- Ye Seul Yang, Seo Young Lee, Jung-Sun Kim, Kyung Mook Choi, Kang Wook Lee, Sang-Chol Lee, Jung Rae Cho, Seung-Jin Oh, Ji-Hyun Kim, Sung Hee Choi
- Endocrinol Metab. 2020;35(2):367-376. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.367
- 7,985 View
- 144 Download
- 8 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
This study assessed the proportion of risk-stratified Korean patients with dyslipidemia achieving their low-density lipoprotein cholesterol (LDL-C) targets as defined by the European Society of Cardiology/European Atherosclerosis Society (ESC/EAS) (2011) guidelines while receiving lipid-modifying treatments (LMTs).
Methods
In this multicenter, cross-sectional, observational study, we evaluated data from Korean patients aged ≥19 years who were receiving LMTs for ≥3 months and had an LDL-C value within the previous 12 months on the same LMT. Data were collected for demographics, cardiovascular (CV) risk factors, medical history, and healthcare consumption. Patients were risk-stratified according to the ESC Systematic COronary Risk Evaluation (SCORE) chart and LDL-C target achievement rate was assessed.
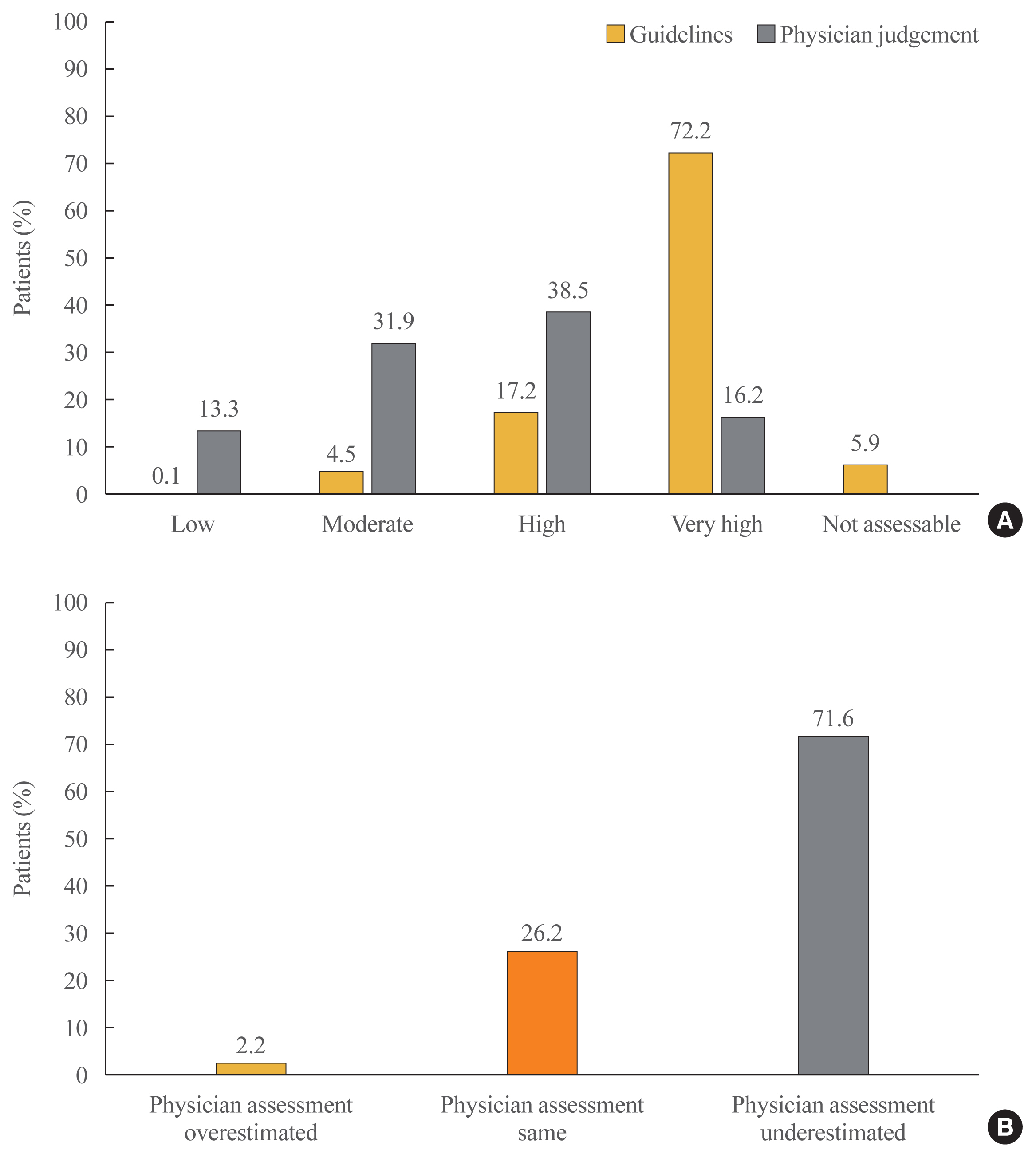
Results
Guideline-based risk-stratification of the 1,034 patients showed the majority (72.2%) to be in the very high-risk category. Investigators’ assessment of risk was underestimated in 71.6% compared to ESC/EAS guidelines. Overall LDL-C target achievement rate was 44.3%; target achievement was the highest (66.0%) in moderate-risk patients and the lowest (39.0%) in very high-risk patients. Overall 97.1% patients were receiving statin therapy, mostly as a single-agent (89.2%). High-intensity statins and the highest permissible dose of high-intensity statins had been prescribed to only 9.1% and 7.3% patients in the very high-risk group, respectively. Physician satisfaction with patients’ LDL-C levels was the primary reason for non-intensification of statin therapy.
Conclusion
Achievement of target LDL-C level is suboptimal in Korean patients with dyslipidemia, especially in those at very high-risk of CV events. Current practices in LMTs need to be improved based on precise CV risk evaluation posed by dyslipidemia. -
Citations
Citations to this article as recorded by- Lipid Management in Korean People With Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
Ye Seul Yang, Hack-Lyoung Kim, Sang-Hyun Kim, Min Kyong Moon
Journal of Lipid and Atherosclerosis.2023; 12(1): 12. CrossRef - Lipid Management in Korean People with Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
Ye Seul Yang, Hack-Lyoung Kim, Sang-Hyun Kim, Min Kyong Moon
Diabetes & Metabolism Journal.2023; 47(1): 1. CrossRef - Bempedoic Acid for Lipid Management in the Indian Population: An Expert Opinion
Jagdish Hiremath, J C Mohan, Prakash Hazra, JP S Sawhney, Ashwani Mehta, Sadanand Shetty, Abraham Oomman, Mahesh K Shah, Ganapathi Bantwal, Rajeev Agarwal, Rajiv Karnik, Peeyush Jain, Saumitra Ray, Sambit Das, Vibhuti Jadhao, Sachin Suryawanshi, Hanmant B
Cureus.2023;[Epub] CrossRef - Optimal implementation of the 2019 ESC/EAS dyslipidaemia guidelines in patients with and without atherosclerotic cardiovascular disease across Europe: a simulation based on the DA VINCI study
Julia Brandts, Sarah Bray, Guillermo Villa, Alberico L. Catapano, Neil R. Poulter, Antonio J. Vallejo-Vaz, Kausik K. Ray
The Lancet Regional Health - Europe.2023; 31: 100665. CrossRef - Management of Dyslipidemia in Patients with Diabetes Mellitus
Kyung Ae Lee
The Journal of Korean Diabetes.2023; 24(3): 111. CrossRef - Target Low-Density Lipoprotein-Cholesterol and Secondary Prevention for Patients with Acute Myocardial Infarction: A Korean Nationwide Cohort Study
Ju Hyeon Kim, Jung-Joon Cha, Subin Lim, Jungseok An, Mi-Na Kim, Soon Jun Hong, Hyung Joon Joo, Jae Hyoung Park, Cheol Woong Yu, Do-Sun Lim, Kyeongmin Byeon, Sang-Wook Kim, Eun-Seok Shin, Kwang Soo Cha, Jei Keon Chae, Youngkeun Ahn, Myung Ho Jeong, Tae Hoo
Journal of Clinical Medicine.2022; 11(9): 2650. CrossRef - Current Status of Low-Density Lipoprotein Cholesterol Target Achievement in Patients with Type 2 Diabetes Mellitus in Korea Compared with Recent Guidelines
Soo Jin Yun, In-Kyung Jeong, Jin-Hye Cha, Juneyoung Lee, Ho Chan Cho, Sung Hee Choi, SungWan Chun, Hyun Jeong Jeon, Ho-Cheol Kang, Sang Soo Kim, Seung-Hyun Ko, Gwanpyo Koh, Su Kyoung Kwon, Jae Hyuk Lee, Min Kyong Moon, Junghyun Noh, Cheol-Young Park, Sung
Diabetes & Metabolism Journal.2022; 46(3): 464. CrossRef - There is urgent need to treat atherosclerotic cardiovascular disease risk earlier, more intensively, and with greater precision: A review of current practice and recommendations for improved effectiveness
Michael E. Makover, Michael D. Shapiro, Peter P. Toth
American Journal of Preventive Cardiology.2022; 12: 100371. CrossRef - Non-achievement of the Low-Density Lipoprotein Cholesterol Goal in Older Patients with Type 2 Diabetes Mellitus and a Very High Cardiovascular Disease Risk: A Multicenter Study in Vietnam
Huan Thanh Nguyen, Khang Pham Trong Ha, An Huu Nguyen, Thu Thanh Nguyen, Hang My Lam
Annals of Geriatric Medicine and Research.2021; 25(4): 278. CrossRef
- Lipid Management in Korean People With Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement

- Clinical Study
- Low Predictive Value of FRAX Adjusted by Trabecular Bone Score for Osteoporotic Fractures in Korean Women: A Community-Based Cohort Study
- Hana Kim, Jung Hee Kim, Min Joo Kim, A Ram Hong, HyungJin Choi, EuJeong Ku, Ji Hyun Lee, Chan Soo Shin, Nam H. Cho
- Endocrinol Metab. 2020;35(2):359-366. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.359
- 5,930 View
- 132 Download
- 9 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The value of the Fracture Risk Assessment Tool (FRAX) and the trabecular bone score (TBS) for assessing osteoporotic fracture risk has not been fully elucidated in Koreans. We conducted this study to clarify the predictive value of FRAX adjusted by TBS for osteoporotic fractures in Korean women.
Methods
After screening 7,192 eligible subjects from the Ansung cohort, 1,165 women aged 45 to 76 years with available bone mineral density (BMD) and TBS data were enrolled in this study. We assessed their clinical risk factors for osteoporotic fractures and evaluated the predictive value of FRAX with or without BMD and TBS.
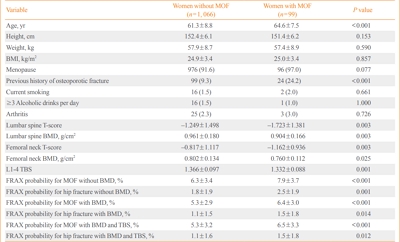
Results
During the mean follow-up period of 7.5 years, 99 (8.5%) women suffered major osteoporotic fractures (MOFs) and 28 (2.4%) experienced hip fractures. FRAX without BMD, BMD-adjusted FRAX, and TBS-adjusted FRAX were significantly associated with the risk of MOFs (hazard ratio [HR] per percent increase, 1.08; 95% confidence interval [CI], 1.03 to 1.14; HR, 1.09; 95% CI, 1.03 to 1.15; and HR, 1.07; 95% CI, 1.02 to 1.13, respectively). However, BMD-adjusted FRAX and TBS-adjusted FRAX did not predict MOFs better than FRAX without BMD based on the Harrell’s C statistic. FRAX probabilities showed limited value for predicting hip fractures. The cut-off values of FRAX without BMD, FRAX with BMD, and FRAX with BMD adjusted by TBS for predicting MOFs were 7.2%, 5.0%, and 6.7%, respectively.
Conclusion
FRAX with BMD and TBS adjustment did not show better predictive value for osteoporotic fractures in this study than FRAX without adjustment. Moreover, the cut-off values of FRAX probabilities for treatment might be lower in Korean women than in other countries. -
Citations
Citations to this article as recorded by- Update on the utility of trabecular bone score (TBS) in clinical practice for the management of osteoporosis: a systematic review by the Egyptian Academy of Bone and Muscle Health
Yasser El Miedany, Walaa Elwakil, Mohammed Hassan Abu-Zaid, Safaa Mahran
Egyptian Rheumatology and Rehabilitation.2024;[Epub] CrossRef - Comparison of predictive value of FRAX, trabecular bone score, and bone mineral density for vertebral fractures in systemic sclerosis: A cross-sectional study
Kyung-Ann Lee, Hyun-Joo Kim, Hyun-Sook Kim
Medicine.2023; 102(2): e32580. CrossRef - Screening for the primary prevention of fragility fractures among adults aged 40 years and older in primary care: systematic reviews of the effects and acceptability of screening and treatment, and the accuracy of risk prediction tools
Michelle Gates, Jennifer Pillay, Megan Nuspl, Aireen Wingert, Ben Vandermeer, Lisa Hartling
Systematic Reviews.2023;[Epub] CrossRef - Chronic airway disease as a major risk factor for fractures in osteopenic women: Nationwide cohort study
Sung Hye Kong, Ae Jeong Jo, Chan Mi Park, Kyun Ik Park, Ji Eun Yun, Jung Hee Kim
Frontiers in Endocrinology.2023;[Epub] CrossRef - Update on the clinical use of trabecular bone score (TBS) in the management of osteoporosis: results of an expert group meeting organized by the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Disease
Enisa Shevroja, Jean-Yves Reginster, Olivier Lamy, Nasser Al-Daghri, Manju Chandran, Anne-Laurence Demoux-Baiada, Lynn Kohlmeier, Marie-Paule Lecart, Daniel Messina, Bruno Muzzi Camargos, Juraj Payer, Sansin Tuzun, Nicola Veronese, Cyrus Cooper, Eugene V.
Osteoporosis International.2023; 34(9): 1501. CrossRef - Comparison of HU histogram analysis and BMD for proximal femoral fragility fracture assessment: a retrospective single-center case–control study
Sun-Young Park, Hong Il Ha, Injae Lee, Hyun Kyung Lim
European Radiology.2022; 32(3): 1448. CrossRef - Association of Trabecular Bone Score-Adjusted Fracture Risk Assessment Tool with Coronary Artery Calcification in Women
Tzyy-Ling Chuang, Yuh-Feng Wang, Malcolm Koo, Mei-Hua Chuang
Diagnostics.2022; 12(1): 178. CrossRef - Risk of osteoporotic fracture in women using the FRAX tool with and without bone mineral density score in patients followed at a tertiary outpatient clinic ‒ An observational study
Maria Helena Sampaio Favarato, Maria Flora de Almeida, Arnaldo Lichtenstein, Milton de Arruda Martins, Mario Ferreira Junior
Clinics.2022; 77: 100015. CrossRef - Comparison of Trabecular Bone Score–Adjusted Fracture Risk Assessment (TBS-FRAX) and FRAX Tools for Identification of High Fracture Risk among Taiwanese Adults Aged 50 to 90 Years with or without Prediabetes and Diabetes
Tzyy-Ling Chuang, Mei-Hua Chuang, Yuh-Feng Wang, Malcolm Koo
Medicina.2022; 58(12): 1766. CrossRef - Application of the Trabecular Bone Score in Clinical Practice
Sung Hye Kong, Namki Hong, Jin-Woo Kim, Deog Yoon Kim, Jung Hee Kim
Journal of Bone Metabolism.2021; 28(2): 101. CrossRef
- Update on the utility of trabecular bone score (TBS) in clinical practice for the management of osteoporosis: a systematic review by the Egyptian Academy of Bone and Muscle Health

Review Article
- Diabetes
- Recent Updates on Vascular Complications in Patients with Type 2 Diabetes Mellitus
- Chan-Hee Jung, Ji-Oh Mok
- Endocrinol Metab. 2020;35(2):260-271. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.260
- 7,577 View
- 282 Download
- 13 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
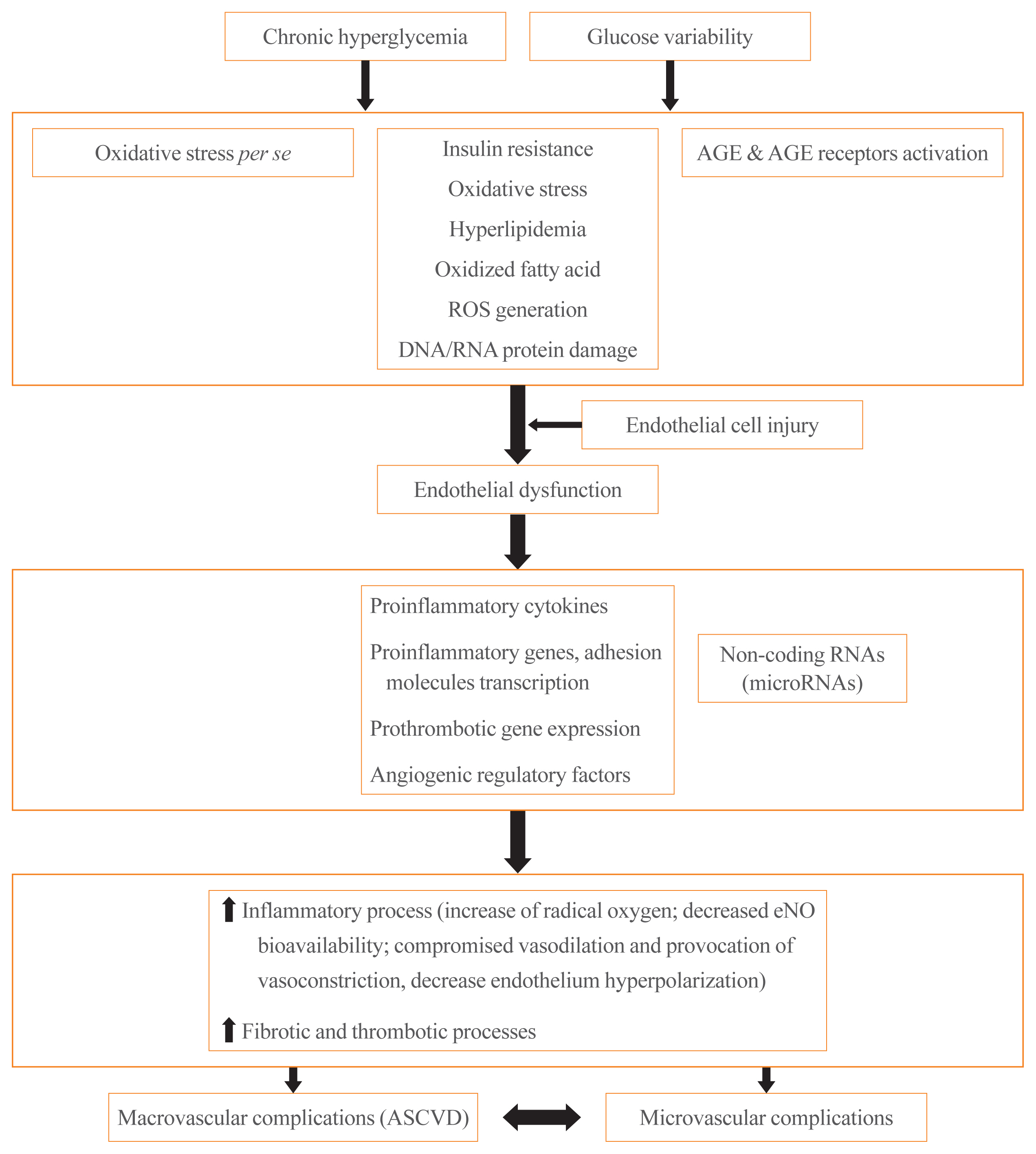
ePub - It is well known that patients with type 2 diabetes mellitus (T2DM) are at an increased risk of morbidity and mortality from atherosclerotic cardiovascular (CV) complications. Previously, the concept that diabetes mellitus (DM) is a “coronary artery disease (CAD) risk equivalent” was widely accepted, implying that all DM patients should receive intensive management. However, considerable evidence exist for wide heterogeneity in the risk of CV events among T2DM patients and the concept of a “CAD risk equivalent” has changed. Recent guidelines recommend further CV risk stratification in T2DM patients, with treatment tailored to the risk level. Although imaging modalities for atherosclerotic cardiovascular disease (ASCVD) have been used to improve risk prediction, there is currently no evidence that imaging-oriented therapy improves clinical outcomes. Therefore, controversy remains whether we should screen for CVD in asymptomatic T2DM. The coexistence of T2DM and heart failure (HF) is common. Based on recent CV outcome trials, sodium glucose cotransporter-2 inhibitors and glucagon like peptide-1 receptor agonists are recommended who have established ASCVD, indicators of high risk, or HF because of their demonstrated benefits for CVD. These circumstances have led to an increasing emphasis on ASCVD and HF in T2DM patients. In this review, we examine the literature published within the last 5 years on the risk assessment of CVD in asymptomatic T2DM patients. In particular, we review recent guidelines regarding screening for CVD and research focusing on the role of coronary artery calcium, coronary computed tomography angiography, and carotid intima-media thickness in asymptomatic T2DM patients.
-
Citations
Citations to this article as recorded by- Pathways of Coagulopathy and Inflammatory Response in SARS-CoV-2 Infection among Type 2 Diabetic Patients
Orsolya-Zsuzsa Akácsos-Szász, Sándor Pál, Kinga-Ilona Nyulas, Enikő Nemes-Nagy, Ana-Maria Fárr, Lóránd Dénes, Mónika Szilveszter, Erika-Gyöngyi Bán, Mariana Cornelia Tilinca, Zsuzsánna Simon-Szabó
International Journal of Molecular Sciences.2023; 24(5): 4319. CrossRef - Increased soluble endoglin levels in newly-diagnosed type 2 diabetic patients are associated with endothelial dysfunction
Xiaobing Dou, Xiujing Wang, Xiuhua Yu, Jiaqi Yao, Huiling Shen, Yao Xu, Bojing Zheng, Zhenying Zhang, Qingying Tan, Tianxiao Hu
Endocrine Journal.2023; 70(7): 711. CrossRef - Effects of hypertension on subcortical nucleus morphological alternations in patients with type 2 diabetes
Feng Cui, Zhi-Qiang Ouyang, Yi-Zhen Zeng, Bing-Bing Ling, Li Shi, Yun Zhu, He-Yi Gu, Wan-Lin Jiang, Ting Zhou, Xue-Jin Sun, Dan Han, Yi Lu
Frontiers in Endocrinology.2023;[Epub] CrossRef - Coronary Artery Calcium Score as a Sensitive Indicator of Cardiovascular Disease in Patients with Type 2 Diabetes Mellitus: A Long-Term Cohort Study
Dae-Jeong Koo, Mi Yeon Lee, Sun Joon Moon, Hyemi Kwon, Sang Min Lee, Se Eun Park, Cheol-Young Park, Won-Young Lee, Ki Won Oh, Sung Rae Cho, Young-Hoon Jeong, Eun-Jung Rhee
Endocrinology and Metabolism.2023; 38(5): 568. CrossRef - Exploring Endothelial Colony-Forming Cells to Better Understand the Pathophysiology of Disease: An Updated Review
Qiuwang Zhang, Anthony Cannavicci, Michael J. B. Kutryk, Giuseppe Mandraffino
Stem Cells International.2022; 2022: 1. CrossRef - Recent Insights into the Nutritional Antioxidant Therapy in Prevention and Treatment of Diabetic Vascular Complications: A Comprehensive Review
Narasimha M. Beeraka, Irina K. Tomilova, Galina A. Batrak, Maria V. Zhaburina, Vladimir N. Nikolenko, Mikhail Y. Sinelnikov, Liudmila M. Mikhaleva
Current Medicinal Chemistry.2022; 29(11): 1920. CrossRef - Topical Reappraisal of Molecular Pharmacological Approaches to Endothelial Dysfunction in Diabetes Mellitus Angiopathy
Constantin Munteanu, Mariana Rotariu, Marius-Alexandru Turnea, Aurelian Anghelescu, Irina Albadi, Gabriela Dogaru, Sînziana Calina Silișteanu, Elena Valentina Ionescu, Florentina Carmen Firan, Anca Mirela Ionescu, Carmen Oprea, Gelu Onose
Current Issues in Molecular Biology.2022; 44(8): 3378. CrossRef - Visfatin is negatively associated with coronary artery lesions in subjects with impaired fasting glucose
Fei Xu, Xiang Ning, Tong Zhao, Qinghua Lu, Huiqiang Chen
Open Medicine.2022; 17(1): 1405. CrossRef - Effects of dulaglutide on endothelial progenitor cells and arterial elasticity in patients with type 2 diabetes mellitus
Dandan Xie, Yutong Li, Murong Xu, Xiaotong Zhao, Mingwei Chen
Cardiovascular Diabetology.2022;[Epub] CrossRef - Serum netrin and VCAM-1 as biomarker for Egyptian patients with type IΙ diabetes mellitus
Maher M. Fadel, Faten R. Abdel Ghaffar, Shimaa K. Zwain, Hany M. Ibrahim, Eman AE. badr
Biochemistry and Biophysics Reports.2021; 27: 101045. CrossRef - Decoding the chemical composition and pharmacological mechanisms of Jiedu Tongluo Tiaogan Formula using high-performance liquid chromatography coupled with network pharmacology-based investigation
Qi Zhang, Chunli Piao, Wenqi Jin, De Jin, Han Wang, Cheng Tang, Xiaohua Zhao, Naiwen Zhang, Shengnan Gao, Fengmei Lian
Aging.2021; 13(21): 24290. CrossRef
- Pathways of Coagulopathy and Inflammatory Response in SARS-CoV-2 Infection among Type 2 Diabetic Patients


 KES
KES

 First
First Prev
Prev



